Brief
We are on a collision course between the way we pay healthcare providers and the types of health insurance that employers and individuals want to buy. Providers and health plans are adopting global risk models—including full capitation, shared savings and accountable care organizations (ACOs)—which pass the financial risk of managing a population to the providers. To manage this risk, providers seek to strengthen the gatekeeper role for each patient, ideally reinforced by a more restrictive health maintenance organization (HMO) product.
At the same time, employers are increasingly opting for high-deductible, tiered networks or other products that are designed to shift financial risk to patients by making them think about what medical care they consume and where. The patient incentives embedded in these plans can take control away from the physician by motivating patients to seek lower-cost care outside their networks. The incentives in typical preferred provider organizations (PPOs) have a neutral impact on a primary care physician’s (PCP) ability to guide patients and keep them in their network. But the very point of consumer directed health plans (CDHP)—steep incentives, coupled with cost and quality data on providers—is to turn patients into active shoppers who do not passively defer to their PCPs (see Figure 1).
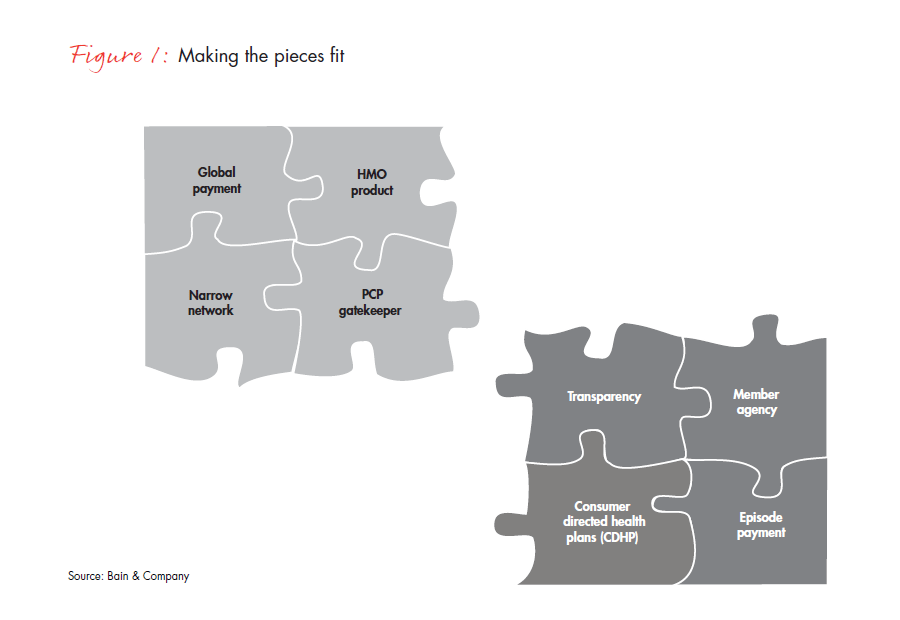
Payment methods that promote tighter care management within specific networks can clash with plan incentives that encourage patients to push back on those restrictions. The solution for health plans is to match their payment strategy to the market. In markets with high HMO penetration, with providers well set up to manage population health and patients accustomed to more restrictive networks, global risk arrangements may make sense. In markets where high-deductible plans and/or traditional PPOs are dominant and primary care is fragmented, a different approach to payment—one based on episodes of care—may be more effective.
Before designing a payment reform strategy, there are a number of key decisions managers of a plan must make about target members, products and spending goals. These key design elements are critical to the development of an effective payment reform strategy (see below, “Making the pieces fit: Key design elements”).
Applying a global risk model in Massachusetts
The case example of Blue Cross Blue Shield of Massachusetts (BCBSMA) provides an instructive example of a health plan that engineered a payment reform strategy reflecting its local market. In 2009, BCBSMA launched the alternative quality contract (AQC) as part of its payment reform strategy. The AQC is a capitated payment model, whereby BCBSMA establishes specific budgets (cost targets) that participating providers must meet to manage the members in their care. A global budget model is a good choice for BCBSMA given the prevalence of HMOs and the degree of provider consolidation and integration in its market. By negotiating a global budget, they have been able to address the costs associated with the entire continuum of care. Moreover, this approach addresses one of the most challenging causes of high cost: utilization of academic medical centers. BCBSMA hopes to use the AQC to make physicians more economically sensitive and thoughtful about where they refer their patients.
Eastern Massachusetts is one of the largest HMO markets in the country. That dominance has allowed BCBSMA to focus the AQC initially on HMO members. Beginning with members that providers have the most capacity to manage and influence has allowed them to develop the infrastructure and the confidence to be successful. BCBSMA is currently considering how to apply this model to PPO members because they are not required to select a PCP.
Early results are encouraging. The 2009 cohort of providers participating in the AQC experienced 2.8% lower costs over the first two years than the control group being paid fee-for-service. Over the same time period as costs were being reduced, quality actually improved for the contracted groups. Perhaps more important, the sub-group of providers within the 2009 cohort that were new to capitation (and therefore starting from a higher base of utilization) experienced an average reduction of $60.75 per quarter—an 8.2% savings relative to the control group. Half of the 8.2% savings came from lower utilization and half from lower prices due to shifts to lower-cost sites of care.
In our experience, global payments can be the right strategy if implemented in the right markets and for the right providers. While not all providers will be successful taking on the challenge of managing populations—because it will likely take longer and be more difficult than most anticipate—there are clearly a number of success stories to share. The early adopters of capitation (e.g., Kaiser Permanente, Group Health Cooperative, Geisinger Health System, many of the Pioneer ACOs and BCBSMA’s AQC providers) all demonstrate the tantalizing potential of aligning a provider’s incentives with cost and quality goals.
An alternative path to controlling costs
Markets with high penetration of CDHPs are a prime example of areas where global payment models may not work effectively. In such an environment, a global payment model would be a poor payment choice, since the plans are designed to make patients into choosy consumers, potentially sending them out of network for lower-cost services. In these plan designs, patients are expected to find the best price, while their physicians are being paid fee-for-service with little incentive to help or to manage their care.
Consumer-directed plans have been around since the late ’90s but have begun to grow rapidly in the last few years. The main reason for growth is that they reduce the increase in costs more effectively than other plan designs, but employers are also wary of additional taxes on rich benefit designs that will be imposed by the Affordable Care Act in 2018. In 2012, 22% of employers of all sizes offered CDHPs, a growth rate of 19% over 2011. Surveys indicate about 40% of all employers will offer such plans in five years (see Figure 2), and as many as 68% of large employers (those with more than 500 employees). A recent study showed that CDHPs with strong employee engagement report medical inflation rates 4% lower than plans with lower deductibles. Moreover, the data suggests that savings come from lower utilization of high-cost items such as hospital stays and prescription drugs, while patients continue to see their primary care physicians for routine and preventive care as often as ever. Clearly, putting patients in charge of their own buying decisions is a powerful tool for cost control.
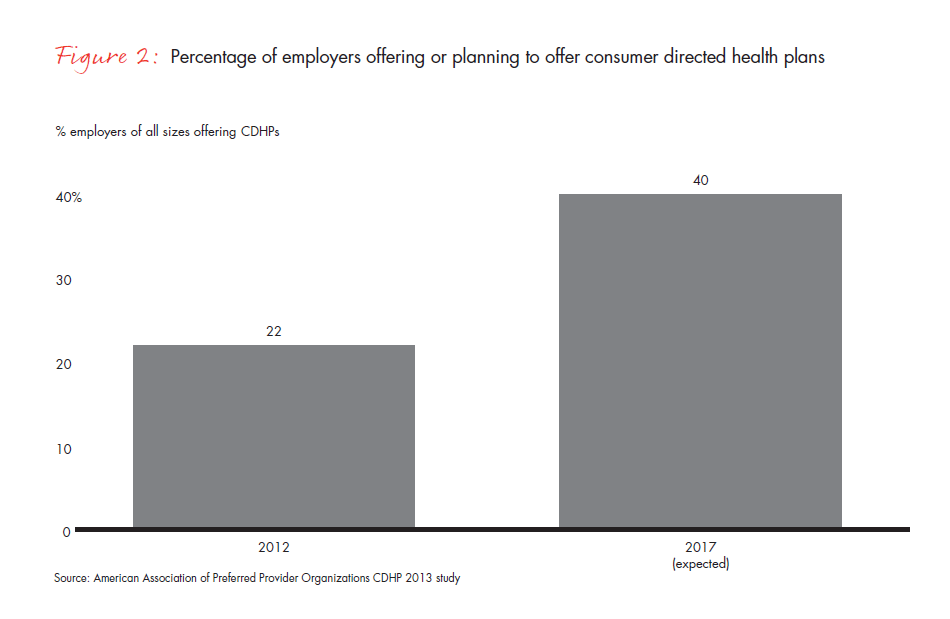
Evidence shows that to be effective, however, these financial incentives need to be coupled with user-friendly data on the cost and quality of various providers. But these comparison tools tend to profile what we call “piece parts” of medicine. They include everything from diagnostic tests to emergency-room visits, presenting a problem for patients who don’t want to shop for every small procedure, especially when it is urgent or complex. A piecemeal approach presents a problem for the healthcare system too, as it works against an integrated approach. Indeed, it dis-integrates care.
While some plans are aggregating claims data so that they can show the likely cost of an entire episode of care, few are broadly contracting with providers on an episode basis. Many plans continue to pay providers fee-for-service and hope that the threat of losing market share will be sufficient to force change. Change could come more quickly if providers also had more immediate financial incentives to re-engineer care.
The way forward
While we are advocates of global payment models, we believe that in many markets with a strong presence of CDHPs, an alternative and more powerful model will be the episode-of-care approach. Episode-based payments offer a fixed payment for certain procedures like hip or heart surgery, but they have been slow to catch on, partly due to the operational complexity of calculating these payments. Hopefully, the Centers for Medicare and Medicaid Services’ Bundled Payment for Care Improvement project, which has attracted significant interest, will offer a methodology (and incentives) that can be emulated by commercial plans. Episode-based payments may also help resolve the tension between providers and patients by giving providers the incentive to engineer their episodes for the highest quality at the lowest cost, and patients the opportunity to evaluate total cost and quality in a simpler way.
Health plans everywhere are working to design incentives that will change provider behavior. And employers everywhere are on a separate journey to create powerful patient incentives to make employees healthier and more prudent about their healthcare spending. At this stage, each constituency is pulling hardest on the lever that makes it most successful. ACOs tend toward total risk models as opposed to fee-for-service, and employers tend toward CDHPs rather than HMOs or other gatekeeper models. The problem is that these incentives create a tension that can work at cross-purposes. Moreover, these discussions can take on the tone of political debates, pitting patient incentive advocates (Vouchers! High deductible plans! Transparency!) vs. provider incentive advocates (ACOs! Medical homes!). Plans and providers do not need an either-or world. In the transition to value-based care, they can and must manage both. Payment reform models need to be designed with this in mind and vary by market and segment to promote positive behavior changes for both providers and patients.
Making the pieces fit: Key design elements
- Which member groups should we focus on? Medicare, commercial and dual-eligible populations all have their own dynamics.
- What insurance products do these members buy and are the products consistent with a specific payment approach? HMOs with a built-in gatekeeper are more conducive to global risk arrangements. PPOs with a loose network permit more freedom of choice and lend themselves better to episode bundling.
- What areas of spending, specific to the population, should we address in order for payment reform to succeed? Healthcare communities often exhibit unique market features that can escalate costs, such as utilization of high-cost academic medical centers for routine care or overutilization of specialists.
- What is the right kind of network? What does the market demand in terms of choice, and should we be selective about how we delegate risk to providers? Not all providers are ready for new payment models. A reform strategy must not get too far ahead of the provider community but still address enough members and providers to be meaningful.
Dale Stafford is a partner with Bain & Company based in the firm’s Washington, DC, office. Phyllis Yale is a Senior Advisor with Bain and based in Boston. She is a member of the Board of Directors of Blue Cross Blue Shield of Massachusetts.

