Brief
It seems that everyone in the healthcare community is talking about “integrated care.” But because the term covers such a wide range of concepts, it is difficult to define it, let alone understand its implications for manufacturers. For those with memories of “managed care” and “disease management” in the 1990s—concepts that did not transform the fee-for-service, inflationary model of healthcare delivery—integrated care may sound like just another fad trending on Twitter. Not surprisingly, many pharmaceutical and medical technology executives remain skeptical: Will the adoption of integrated care approaches yield improvements in healthcare productivity? And, if so, will it really require changes to the core business model of manufacturers?
While healthy skepticism seems appropriate, we see untapped value in managing patients more effectively across “points of care,” and we believe that trend will continue given the broader market forces. We also believe that the emergence of integrated systems will significantly impact many manufacturers’ operating models, affecting everything from clinical trial design to go-to-market models.
The more important issue is whether the move to integrated care will require manufacturers to evolve their business models, perhaps by migrating from a products only to a more solutions-oriented company. Before making that choice, executives need a clear perspective on three key questions:
- Are there significant unmet needs for care integration in the disease states where you play?
- Do you have distinctive assets and competencies to contribute?
- Is there a viable business model to capture the value you create?
Before addressing these questions, however, it may be helpful to review the forces underling the emergence of integrated care models and some general implications for the traditional pharma and medtech operating models. For practicality, this review focuses on the US market, but the concepts and approaches are globally relevant.
Forces underlying the emergence of integrated care models
At its most basic level, integrated care creates value by changing the behavior of patients and healthcare providers in ways that improve clinical outcomes, reduce cost and provide a better experience for all. Over the past decade, market conditions have evolved in ways that have enabled integrated care models to emerge:
- Structural changes in healthcare delivery, including consolidation of physician practices, a shift toward physician employment and the emergence of integrated delivery networks (IDNs) with aligned incentives across payers and providers;
- Increased digitization of healthcare, allowing easier and higher-quality data collection, improved analytics and easier information sharing among all players;
- Greater consumer engagement, driving demand for a more seamless care experience and increasing the legitimacy of the patient/caregiver in treatment choices and ongoing care.
These factors could enable a step-change in productivity and quality that the existing system is currently too fragmented to achieve.
For the moment, providers are leading the charge. Hospitals have been snapping up primary and specialty care practices to ensure a steady referral flow and create a network that improves efficiency and effectiveness. In 2008, there were 53 publicly announced physician group mergers and acquisitions. Three years later that number had roughly doubled to 108, although it slowed down in 2012, according to The Health Care Services Acquisition Report by Irving Levin Associates, 2013.
For physicians—still the primary customers for pharma and medtech companies—life in these larger entities brings a different economic reality. Bain’s 2013 survey of US physicians found that between half and two-thirds believe that they will be participating in pay-for-performance, capitation or bundled payment initiatives in the next two years, a percentage considerably higher than what we see today (see Figure 1). Changes in incentives are also translating into changes in attitudes: A similar Bain survey in 2011 showed that physicians increasingly understand and accept their role in cost management. In short, providers are aligning with payers—economically and attitudinally.
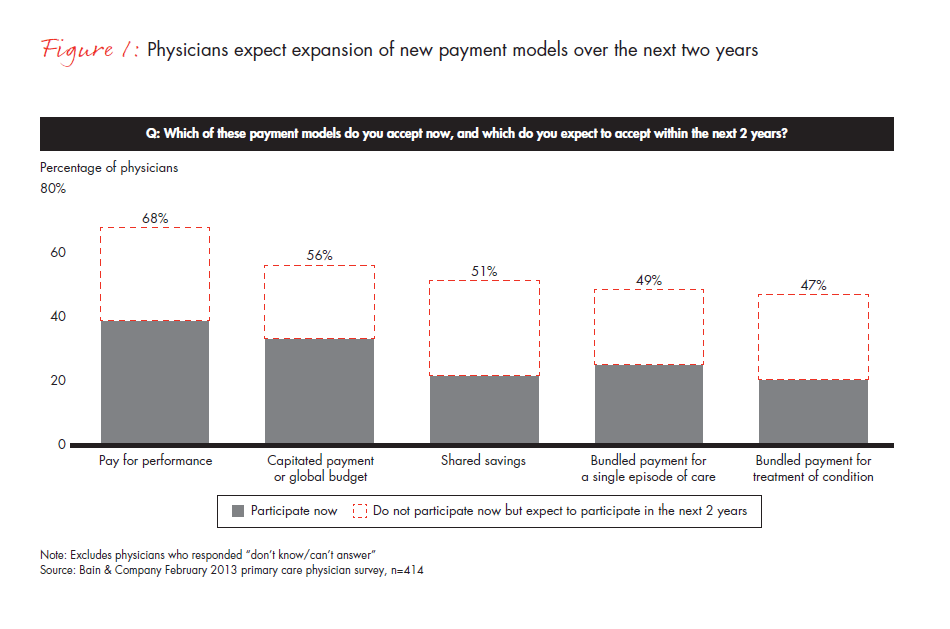
In this environment there is a lot of experimentation going on, with payers buying providers and providers disintermediating payers. Even pharmacy groups like Walgreens are entering the fray by forming accountable care organizations with leading physician groups. Not all of these moves will be successful, in part because of the significant execution challenges, but the players are learning and adjusting in real time. Emerging from the noise are outlines of new care models that offer manufacturers a potential entry point.
Evolving models of integrated care
The most promising models are coalescing around patient-based “units of integration,” in other words, a coherent set of clinical and economic activities focused on a particular medical procedure or patient type. Combining previously disparate but related activities creates a new market with services that can be measured, priced and sold—sometimes directly to employers. The two models described below differ in objectives and scope, but both aim to deliver less fragmented care at lower cost (see Figure 2).
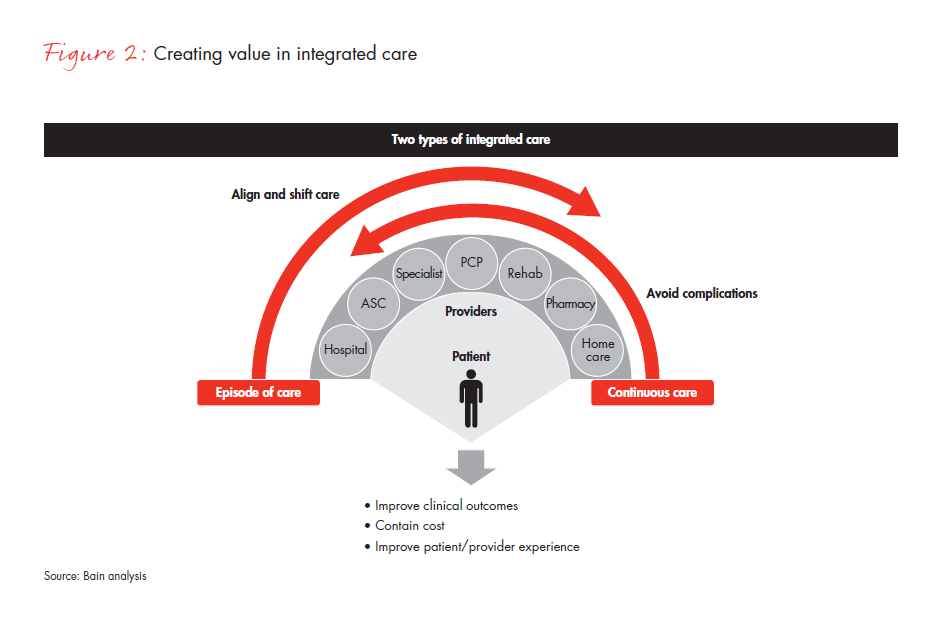
Episode of care. The narrowest approach seeks to integrate all activities around a procedure or medical event, an episode of care, such as a joint replacement or transplant operation. This approach creates value by integrating pre- and post-procedure activities (such as rehabilitative home care) into a holistic program that produces superior outcomes and patient experience. By treating the procedure as one rather than many events, such models can maintain high-quality standards while reducing cost and shifting care to more convenient centers. Bundled payment initiatives and readmission penalties by public and private payers accelerate the adoption of these approaches by using financial incentives to link activities and increase the focus on outcomes.
One example of an episode of care approach is the coronary artery bypass grafts (CABG) program developed by the physician-led Cleveland Clinic. This program provides an entire suite of treatment services—hospital, specialty care, labs and imaging, rehabilitation services, protocol design and claims management. For instance, the clinic offers Lowe’s, the retail chain, a bundled payment structure in the form of a flat fee covering all activities— from admission through a specific number of post-operative days—for all Lowe’s employees requiring the procedure. In one case alone, the partnership between the clinic and Lowe’s saved $62,000. The clinic has since expanded the program to customers like Kohl’s, Rich’s, Boeing and Walmart. The clinic also expects to gain share from payer profit pools and increase its revenues by expanding its patient base into other geographies (see Figure 3).
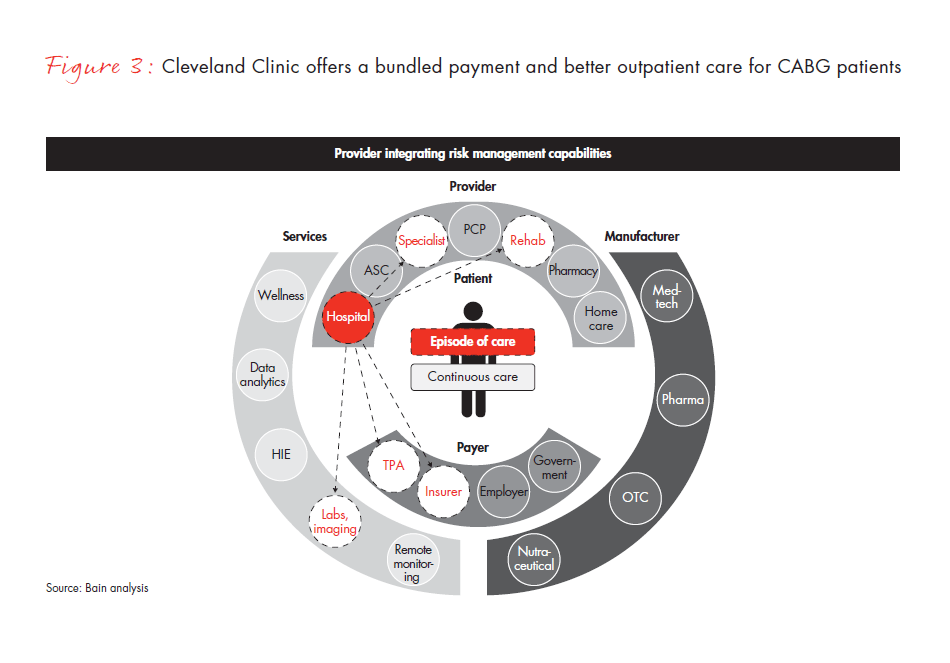
Continuous care. The second approach focuses on avoiding high-cost events in the first place through a patient-centric continuous care model. This model focuses more on chronic conditions and creates value by connecting the various patient points of care (such as a home, doctor’s offi ce or clinic) to reduce waste, improve clinical outcomes and enhance patient and physician experience. It is generally targeted at entire populations under a capitated reimbursement scheme. This is a big prize, given the potential for care improvement in populations such as the elderly or those with diseases like diabetes, where treatment adherence and disease monitoring play a significant role in outcomes. This is also an area where players in other sectors, such as technology and telecommunications, see an opening to enter the healthcare market.
The health insurance giant Humana illustrates a continuous care approach in its Humana Cares program (see Figure 4), which provides integrated care for patients with complex and chronic conditions. Using big data analytics, more than 200,000 participants had been selected and enrolled by the end of 2012. Patients in Humana Cares typically have their care coordinated over the telephone by a registered nurse employed by Humana. The program includes health education and coaching, monitoring of adherence to medication and coordination of other acute and chronic care for a population of primarily Medicare Advantage enrollees. Initiated in 2009, this approach resulted in 26% fewer hospital readmissions and a 13% decline in emergency room visits by early 2012.
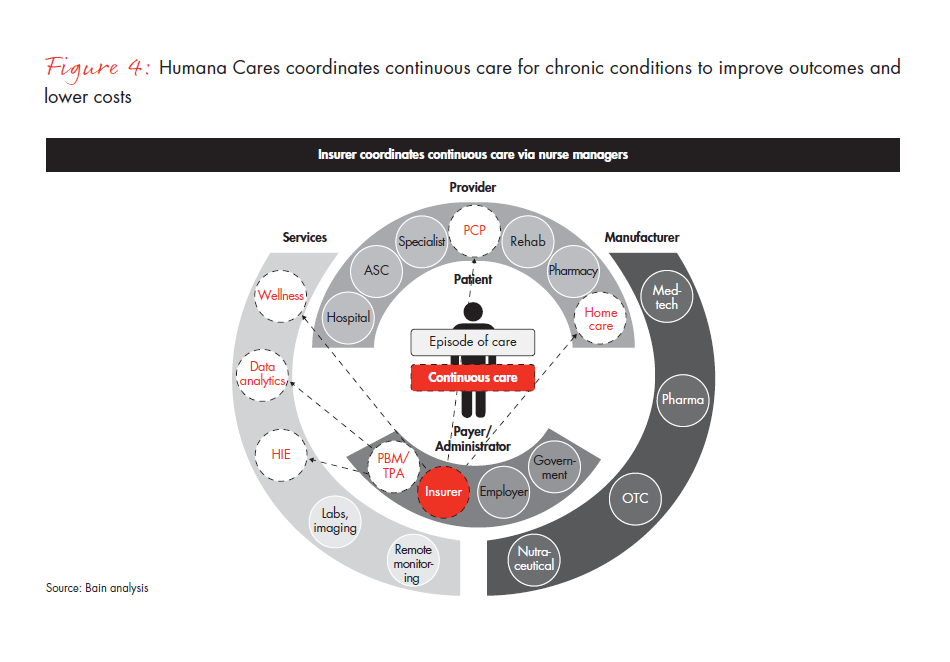
The above models may sound intuitive and easy to grasp, but implementation is a challenge. Aligning incentives across the various silos, finding credible partners to complete the offering, evaluating financial risk, pricing the products accurately and changing organizational behavior are all very difficult, and many providers and payers are only beginning the journey. The question for manufacturers is how and when to respond, if at all.
Implications for pharmaceutical and medical technology companies
There is a real debate within the leadership of many pharma and medtech companies about the implications of these trends on their businesses. The debate is especially intense since it is occurring when manufacturers’ profit pools are shrinking and the traditional engagement model with customers is under pressure in developed markets (see the Bain Brief, “Healthcare 2020”).
At a minimum, companies will need to rethink how they develop and market their products. Historically, the focus has been on generating a “point sale” with physicians in a fee-for-service reimbursement model. Going forward, it will become more of a “systems sell” to networks in a bundled or capitated reimbursement model. Put differently, manufacturers used to sell into a profit center but will increasingly be selling into a cost center. That requires a shift from selling inputs such as clinical efficacy, safety and unit pricing to selling outputs like real-world outcomes and total care costs. Manufacturers have some experience with that kind of dialogue with payers for market access, but what is new is the need to have similar conversations with providers to drive usage. It calls for enhanced capabilities in account management and health economics, along with improved dialogue between marketing and development. It also requires customized approaches to serve larger provider networks with their own proprietary databases, protocols and performance metrics.
The larger question is whether a company should evolve its business model and take a more active role in advancing care integration, thereby gaining a seat at the table alongside its customers. These discussions often start by considering what role a company can credibly play and whether there are any distinct resources to contribute.
In our experience, firms often overlook a number of hidden assets, including:
- Deep knowledge of specific disease states or conditions and the scientific capabilities to advance the state of knowledge;
- Global perspective on medical best practices and capabilities in economic and health outcomes modeling to assess different approaches;
- Promotional infrastructure and capabilities to influence and change physician and patient behavior;
- Financial resources and a comfort with making investment decisions in situations of relative uncertainty.
Our research shows that physicians do welcome pharma and medtech involvement in integrated care, particularly in areas such as adherence and wellness programs, evidence-based protocols, remote monitoring, analytics and telemedicine (see Figure 5).
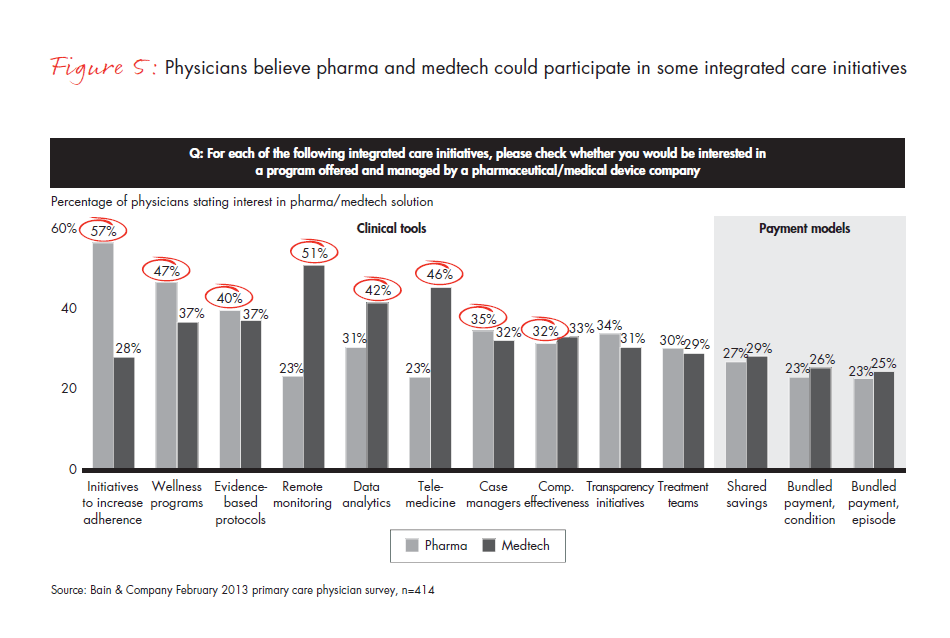
Seizing the opportunity for a partnership role in the continuous care of diabetic patients, the pharma company Sanofi made a decision to build a full suite of services around its market-leading insulin product, Lantus, for Type 1 and Type 11 diabetics. In addition to the core product, Sanofi is creating wellness programs, improving diabetes education, integrating insulin dosing and glucose monitoring devices, enabling remote monitoring and working with both primary care providers and patients to improve adherence. The goal is ambitious: to gain market acceptance by reducing HbA1c results by 10% while increasing patient satisfaction. Sanofi hopes to realize a new revenue stream in testing devices and gain a greater share of the insulin market for Lantus. The medtech company Medtronic is exploring similar models in a variety of disease states through its recent acquisition of Cardiocom.
How will you answer the key questions?
While integrated care offers the promise of new profit pools—potentially redefining what it means to be a pharma or medtech company—we would urge caution. Before considering a wholesale or even partial revision of your business model, you need to be comfortable with your answer to the questions we introduced earlier:
1. Are there significant unmet needs for care integration in the disease states where you play?
The medical conditions most fertile for integrated solutions are those that require frequent and ongoing attention, are managed across multiple locations and where patient behavior has a significant impact on outcomes. There also have to be “pain points” and missed opportunities in the care continuum that contribute to suboptimal care, excess cost or inconvenience for patients and providers.
In the recent 2013 Bain survey, primary care physicians were very positive about the value that integrated care solutions could provide for a number of chronic diseases, but they were especially supportive of those with heavy patient or caregiver involvement, such as diabetes, heart conditions and asthma (see Figure 6).
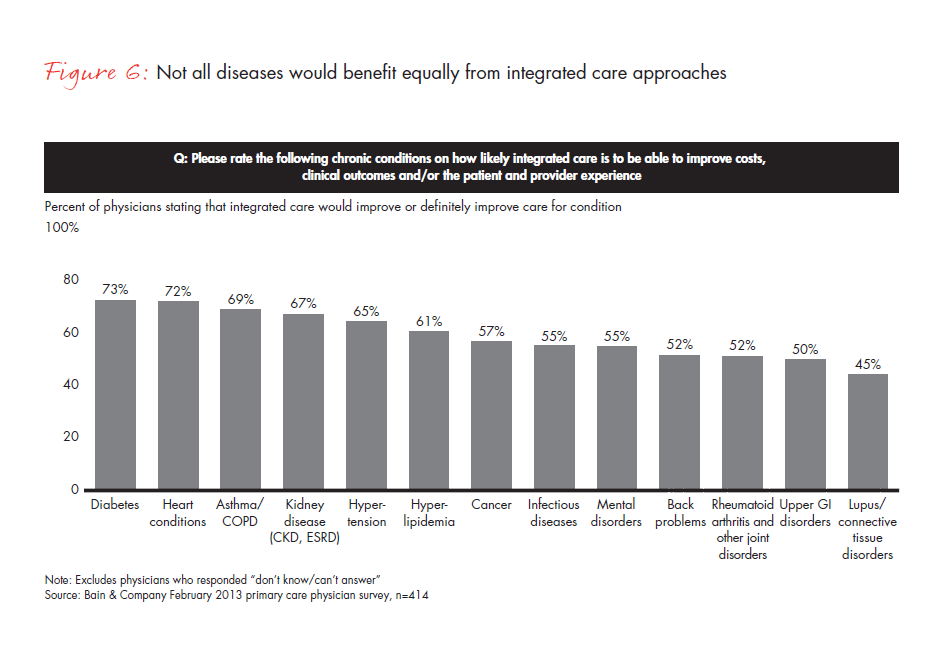
The first step in assessing your portfolio is to take a broad view of your target disease area and develop a rigorous understanding of the end-to-end patient, physician and payer experience. Analyses would include patient flows and key sources of “leakage,” cost mapping and real-world clinical outcomes, including key differences by market segment. With that perspective, you can assess areas for improvement and the degree of difficulty in achieving the required behavior change. Some of this data already exists at an aggregate level for payer negotiations, but the focus here is real-world data and may require partnerships with willing provider institutions to demonstrate credibility.
2. Do you have distinctive assets and competencies? Are you well positioned to fill the need in the market?
Armed with a robust understanding of the highest-yield levers of change for a given patient population, the question remains whether your firm is well suited to promote those changes. Here are a few factors to consider:
- First, since integrated solutions seek to connect different constituencies—patient with physician, primary care with specialist—there is an enormous network effect, with the potential for value creation rising disproportionately with market presence. As a result, incumbents with high market share in a core product are in a stronger position to promote a new, integrated standard of care.
- Second, while there are certainly leading firms in many disease areas, few have dominant positions across all of the required components of an integrated solution. Our research suggests providers and payers are worried about potential conflicts of interest and want to maintain the option to make best-in-class choices across the treatment continuum. Pharma and medtech companies will need to decide which components are critical to their offering and use the full range of business development options to gain access to those assets—from mergers and acquisitions to partnerships of varying forms.
- Finally, there is a significant managerial challenge in moving from a product-based orientation to a solutions-based one. An integrated offering may include markedly different technologies with very different regulatory contexts. To be successful, companies need the internal flexibility to manage across businesses with different development cycles, financial metrics and capital allocation hurdles.
3. Is there a viable business model to capture value?
This may be the most difficult question to answer. Payers and providers can capture the value of integrated models by lowering their cost base and improving their market position. For manufacturers, the task is more difficult.
It is often challenging for manufacturers to define the value of an integrated offering beyond the sum of the constituent products and services. Usage protocols are largely in the public domain and the data supporting the underlying analytics are usually generated by the patient or providers themselves and not always available to the manufacturer.
Manufacturers may have also contributed to the problem by positioning their products as giveaways, paid for by increased share or reduced price erosion of their core product. Where firms have attempted more ambitious solutions, such as risk-sharing structures, the difficulty in finding workable models and the administrative burden for payers and providers have limited adoption.
As the analytics improve and provider networks become more sophisticated about their own strengths and limitations, partnerships can and will emerge, likely with manufacturers playing a role as “care extenders.” These solutions will likely be tailored and priced for each customer in true B2B fashion, and value will be captured by manufacturers through lower commercial costs (such as by sharply reducing sales reps) as well as traditional product and service revenues, potentially with a shared risk component.
As for consumers, so far they have shown a reluctance to make significant out-of-pocket expenditures in areas such as disease monitoring and adherence. It may be a lack of appropriate financial incentives, an assumption that if a given innovation were medically important it would be reimbursed, or simply that closer management of chronic conditions does not offer immediate rewards. Exceptions occur with consumer-oriented conditions such as dermatology or when a motivated caregiver is involved, such as parents of Type 1 diabetics or adults with elderly parents. Outside of these markets, however, the greatest value of consumers in integrated care may be in creating demand for manufacturers’ offering with payers and providers.
Ultimately, companies may have to look beyond traditional measures of profitability to determine the success of their integrated care approach. It will take some shareholder education, but factors like customer loyalty, income sustainability, averted cost pressure, lower commercialization costs, better customer insights and improved image are all persuasive elements in a company’s valuation.
Where does this leave you as you evaluate the integrated care marketplace? The pharma and medtech industries have had a very successful run over the past century doing what they do best—developing innovative products that improve patient quality of life and broader public health. Many will no doubt continue to be successful in the face of supply- and demand-side pressures by revamping their innovation and commercial models. Nonetheless, the changes under way in the broader healthcare system are unlikely to leave the current business models of manufacturers untouched. For certain disease conditions and with more innovative customers, we do expect to see the emergence of more integrated models for the supply of drugs and devices.
The key questions are how to know when your business is ripe for these types of solutions, what the solution might be that yields competitive advantage and how to effect the internal transformation required to deliver the results.
Michael Retterath is a partner with Bain & Company based in New York. Tamara Olsen is a Bain partner based in Boston. George Eliades is a Bain partner based in San Francisco. All are leaders in the firm’s Global Healthcare practice.
The authors wish to acknowledge the work of Ben Siegal and Ryan Hess.





