Brief
It’s 3 AM. Alan awakes from a deep sleep and sits upright in his bed. Since his heart attack and surgery the year before, he has been hyperaware of changes in his heart rate, and he is feeling discomfort in his chest. Alan attaches to his smartphone a digital tool that his payer, CareCo, gave him after his discharge. The Smartheart device produces an ECG in a few seconds and uploads it to an on-call nurse at CareCo.1 Understanding that it is the middle of the night, she sends a text message to Alan’s phone. “Alan, I see you have sent me an ECG reading. Are you ok?” Alan texts back, “I’m not sure. I am feeling heaviness in my chest.” The nurse monitors Alan’s vitals for a few minutes and asks him a few questions. She sees that the ECG is normal but suggests that she set up an appointment with Alan’s internist, Dr. Lisa Hodgkins, for the next day. The nurse uses the ZocDoc app to set up the appointment and lets Alan know about the timing.2 She also advises Alan to wear his IneedMD, an at-home monitoring device that will send readings to her every half hour for the remainder of the night.3
In the morning, using videoconferencing on his laptop, Alan talks to Dr. Hodgkins, who conferences in a cardiologist in another office. Based on the ECGs Alan has been sending them for a few weeks and the database on patients like Alan, the doctors confidently adjust his medication to a lower-cost but equally effective generic drug. Dr. Hodgkins uses her tablet to send the prescription to Alan’s pharmacy. Within an hour, Alan has a new prescription with a “GlowCap,” which will send him a message on his smartphone or sound an alarm if he fails to take his medication at the right time. It also alerts his physician via a report if he misses any doses.4 Because of this digital technology, Alan avoids an ER visit in the middle of the night and a long stressful drive to his physician the next day.
This is not a true story, but it is also not science fiction. All of these digital tools are either available right now or will be soon—SHL Telemedicine’s Smartheart device, the IneedMD monitoring glove, the videoconferencing tool, the physician’s tablet, the ZocDoc tool for online scheduling, the electronic health record (EHR) and the GlowCap. Because of the proliferation of digital tools flooding the marketplace, it is easy to conclude that the digital revolution in healthcare has taken off and is gaining altitude. The promise of these tools is that their prudent use can help flatten healthcare spending and potentially even hold it at 18% of GDP by 2020. But that will not happen without considerable effort, expense and commitment (see Figure 1).
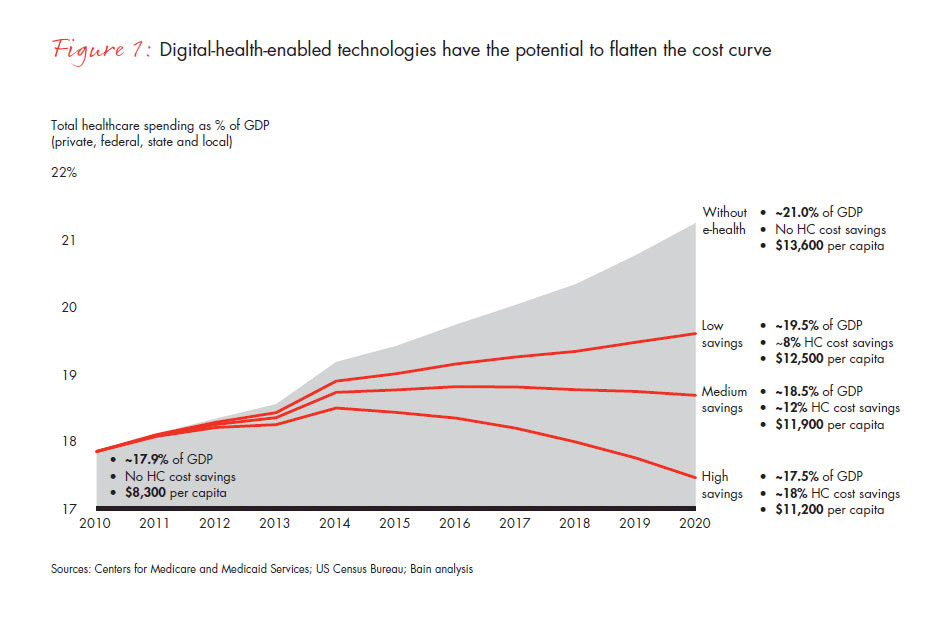
All stakeholders have something to gain—and lose— by embracing digital technology. If we assume that digital tools can be a disruption to traditional practice, it is not a big leap to conclude that such technology has the potential to change the setting of where and how care is delivered, how data will be collected and used, how care may be managed against well-defined standards of care, how drugs and devices will be evaluated by payers, and how patients themselves may use the new integrated information to choose providers and treatments. The advent of digital health can provide the information and connectivity to enable all those stakeholders to address these challenges in a more creative way.
In the next decade, digital health will facilitate three fundamental shifts in healthcare: bending the cost curve, increasing the speed and value of innovation, and enhancing outcomes and quality of care. Much like the digital transformation of the financial services industry decades ago, there will be winners and losers in the new digital age. Some companies will catch the wave soon enough to reap significant savings; others will wait and be left behind. Even without being an early adopter, you can take action now to ensure that you not only survive but thrive (see Figure 2).
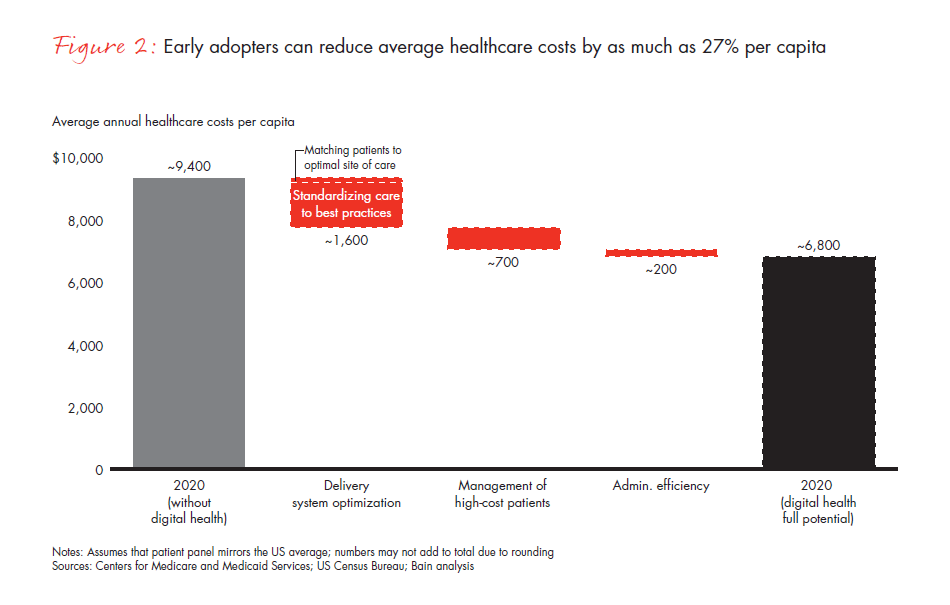
Bending the cost curve
Let’s start with a hypothetical payer, CareCo, that sees the wave of innovation and does not want to be left behind. The company has conducted a digital health diagnostic to determine its priorities and benchmark itself against its competitors. CareCo realizes that digital technology can fundamentally change the delivery of healthcare and focuses on four major opportunities to increase the efficiency of its integrated payer business:
- Improving its administrative efficiency (potential savings of ~$200 per member per year, or PMPY)
- Managing high-cost patients more effectively (~$700 PMPY)
- Linking patients to high-quality providers (~$1400 PMPY)
- Matching patients to optimal sites of care (~$200 PMPY)
Improving administrative efficiency
CareCo already uses a variety of tools to reduce administrative costs: Automatic scheduling allows patients to schedule appointments via email or online, kiosks streamline on-site patient check-ins and e-billing facilitates online claims filing and bill pay. Patients can view their tests and email their physician via an online portal. Staff who previously spent time on back-office filing are free to work on direct patient care. CareCo provides incentives for its extensive provider network to use electronic health and electronic medical records (EHR and EMR). A recent study showed that while only 25% of physicians are “on target” to meet the federal standards for using these records, 66% of the survey respondents use some form of EHR system to manage clinical information.5
In addition, the data-rich environment enables CareCo to better understand outcomes and identify subsets of patients that respond to specific therapies. This information creates value not only for the payer, but also for manufacturers designing new drugs and products for specific populations.
We estimate that digital health technologies like these can reduce administrative costs by up to 10%, for an overall reduction in PMPY costs of $200.6
Managing high-cost patients more effectively
Patients like Alan, who start out with an acute-care episode like a heart attack, become chronic-care patients as they manage their disease over time. Analysts estimate that 1% of patients drive 30% of healthcare costs.7 For this reason alone, CareCo has provided Alan and his physician with a variety of tools to maintain his health and keep him out of the hospital. And even simpler device-free tools have allowed integrated systems, like the Henry Ford Health System in Detroit, to reduce expected hospital readmissions for heart failure patients by 36%.8 Henry Ford uses Tel-Assurance, a care coordination tool that can be either phone- or Web-based, which has been readily accepted by its diverse patient population. These high-cost patients become extremely attractive targets for the kinds of monitoring tools that medical technology and pharmaceutical companies have started to introduce, and they create an opportunity for suppliers to go beyond a specific pill or device and create a more comprehensive approach to treatment.
Digital health can also help providers and payers identify high-risk patients who have not yet experienced an acute-care episode by using predictive modeling9 and data from patients’ EHR to pinpoint those who need extra reminders to take their medication, and engaging them in ways to monitor their own progress and health.
Implementing digital health to manage high-cost patients can generate PMPY savings of approximately $700 or around 7%.10
Linking patients to high-quality providers
We know that physicians and hospitals differ dramatically in their quality and cost, and the highest-cost providers are not always the highest quality.11 Even the most basic of procedures can vary dramatically in cost. The state of Maine publishes the average cost of 30 common medical procedures online. Data show that Anthem Blue Cross Blue Shield HMO members can pay anywhere from $537 to $3,151 for a colonoscopy, depending on whether the procedure is done in a doctor’s office, a freestanding surgicenter or an outpatient surgery unit attached to an acute-care hospital.12 One of the reasons for the variation in price is the lack of transparent and accessible information for patients or employers about these variations. But price variation also reflects a widely held but erroneous belief that hospitals always provide a higher quality of care for even the most basic procedures. As digital technology begins to standardize care and technology in all settings of care, and as long as quality is equivalent, the price of care will drive utilization to the lower-cost settings.
CareCo shares data on quality with all its network physicians via the clinical decision support (CDS) systems, which it has distributed to standardize care based on evidence-based protocols. At Virginia Mason Medical Center in Seattle, for example, the implementation of robust CDS systems has decreased the use of advanced imaging by nearly a quarter without compromising outcomes.13 And CDS systems can reduce adverse drug events from drug interactions by 50%.14
Increased scrutiny of the effectiveness of expensive procedures will also create an opportunity for medical technology companies. In an environment where “smarter” devices can transmit every heartbeat from a patient’s remote device to a central place for monitoring and evaluation, the availability of more accurate, real-time data will enable providers to deliver better quality care. On the other hand, the same real-time data may cause providers and institutions to evaluate the effectiveness of a procedure or device more rigorously than before. For example, knee arthroscopy is one of the top 10 outpatient procedures today, with more than 650,000 surgeries performed every year. Recent studies show that by applying CDS systems and other tools, up to 44% of those surgeries could be deemed unnecessary.15 In a price-competitive environment, medical technology companies face a significant challenge to differentiate their products in a number of ways. One option is to create “appropriate use” guidelines that enable surgeons to justify the use of the device and the company to hold price, while affirming the importance of evidence-based decision making. The burden of proof will remain with the manufacturer to demonstrate value and benefit.
Implementing digital health to link patients to low-cost, high-quality providers and eliminate unnecessary procedures can generate PMPY savings of approximately $1,400 or about 15%.16
Matching patients to optimal sites of care. Digital health initiatives will help to funnel patients to the most appropriate, cost-effective sites of care, reducing both hospital costs and in-office physician appointment costs.
Avoided hospital visits will generate the largest savings. We estimate that around 20% of total ER visits are for conditions that could be treated at a doctor’s office or walk-in retail clinic at a fraction of the cost of the emergency room, for annual PMPY savings of about $100.17 Many such complications could have been avoided had the patient’s vital signs been continuously monitored while the patient was recovering at home. In cases like Alan’s, the value of remote monitoring tools that track a patient’s vitals can be worth about $40 in PMPY savings.18
In the primary care setting, we estimate PMPY savings of approximately $30 by replacing routine in-office visits with video chat and instant messaging.19 A pharmaceutical company developed an iPhone application that can test a patient’s vision and send a picture of the patient’s eye to the doctor to check for signs of infection.20 This saves both the patient and the doctor time and enables patients who use drugs that require monitoring to be examined remotely. Tools like this engage patients in the management of their own care and make it easier for doctors to track and monitor the progress of each patient, demonstrating their value and encouraging patient compliance.
CareCo’s digital health journey does not happen overnight, but the reward is substantial: By aggressively implementing digital health and using it to drive care coordination and cost savings, CareCo reduces PMPY costs by some $2,500, for overall savings of 25% compared with companies that have no digital health initiatives in place.
Bending the cost curve is only one of the transformational changes that will come from the digital revolution. Digital technology can also allow manufacturers, payers and providers to deliver on their promise to increase the speed and quality of their research.
Increasing the speed and value of innovation
Of the many challenges facing manufacturers, the most significant are the cost and pace of innovation. A recent Forbes article suggests that the cost of an average drug developed by a major pharmaceutical company is not around $1 billion as usually cited, but closer to $4 billion and can be as high as $11 billion.21 At a time when the pressure to innovate is high, the new digital world offers manufacturers a variety of opportunities to conduct research and development in a different way. Processes such as “crowdsourcing,” where a company reaches out to new and broader communities for ideas for solutions, can speed up and enhance the research process. Eli Lilly was one of the first to use crowdsourcing via the Web to broaden its research reach,22 and Harvard Medical School has used InnoCentive’s crowd-sourcing capability to solve scientific problems around Type 1 diabetes.23 Collaborative data sharing, such as Sage Bionetworks, which is creating large repositories of data for research purposes, is another way to accelerate the pace of innovation.24 The digital revolution is already creating better data to drive more evidence-based decision making on the front end of innovation.
Imagine a global pharmaceutical company called PharmaCo that is focusing on next-generation drugs for heart disease. The company is running a Phase III trial for a new drug for heart disease and decides digital tools can improve the process. PharmaCo uses a well-defined screen to recruit Dr. Johnson as an investigator through Sermo.25 He begins the search for subjects by posting a message describing the trial on a specially designated area of the healthcare social network PatientsLikeMe.26 His assistant scans profiles on the website to identify especially promising potential subjects and sends them individual messages describing the new study. The company next contacts the payer, CareCo, to mine its database and reach out to Dr. Hodgkins and Alan, her patient. Web-based recruitment can result in a nearly two-thirds reduction in recruitment time compared with traditional office-based methods and can allow the drug company to save 60% of marketing spending.27 Within two to three months, the company has filled the trial and is ready to begin treatment.
Once the trial is under way, Dr. Johnson receives daily reports on the trial’s progress, compiled and sent to him by a virtual clinical research associate (CRA)—a customized computer program that parses and prioritizes data from patients’ self-reports and costs a fraction of a traditional CRA. It utilizes real-time patient feedback and analyzes adverse events and patient dropouts. It also identifies subjects who are higher risks for either and alerts Dr. Johnson to these cases so that he can intervene where appropriate. As a result, he reduces the dropout rate by 30% so that more than 80% of all subjects complete the trial.28
Dr. Johnson keeps in close touch with Alan’s physician, Dr. Hodgkins, who in turn keeps Alan informed about all aspects of the trial, without either of them having to travel to the site. Alan’s data are integrated with the data of the other patients, and the trial proceeds swiftly and smoothly. Fully integrated, the digital tools can shorten trial timelines by a third and reduce costs by nearly 15%.
These tools also are an asset for in-line products, creating more accurate outcomes data through real-time monitoring, better patient satisfaction through new forms of patient engagement and gaming that drive adherence, and new methods to integrate sites of care for patients with chronic disease. The companies that are first to introduce these tools will have a distinct competitive advantage.
Enhancing outcomes and quality of care
Beyond reducing costs and increasing the speed of innovative products to market, digital technology can improve outcomes and quality of care for patients in a number of significant ways. “Patient engagement” as a term of art is both overused and underutilized, but there is little doubt that providing a patient with high-quality care is enhanced by the adoption of new digital tools by the patient, as well as the suppliers, payers and providers who serve them.
For Alan, rapid treatment of his heart symptoms improves his quality of life by reducing the need for an unnecessary ER visit. The daily burden of managing his complex health regimen will be eased by digital health tools that can automate many of the tasks—such as recording his heart rate on a minute-by-minute basis or tracking his prescription adherence—activities that he would either have to do manually or not at all. Adherence is a key to good outcomes, and simple medication reminders have been shown to increase adherence to medications from 50% up to 96%.29
When acute episodes do occur, digital health can enable better outcomes through higher-quality treatment. Armed with real-time data analysis from remote monitoring tools, health professionals can respond to acute events rapidly, which improves outcomes. Every 30-minute decrease in time-to-treatment reduces mortality risk by 7.5%.30
Decreases in mortality and reductions in adverse drug events and surgical complications are all possible with more engaged patients, better information and providers who willingly embrace digital technology (see Figure 3). But as we noted in the introduction, there are real barriers to adoption that we cannot ignore.
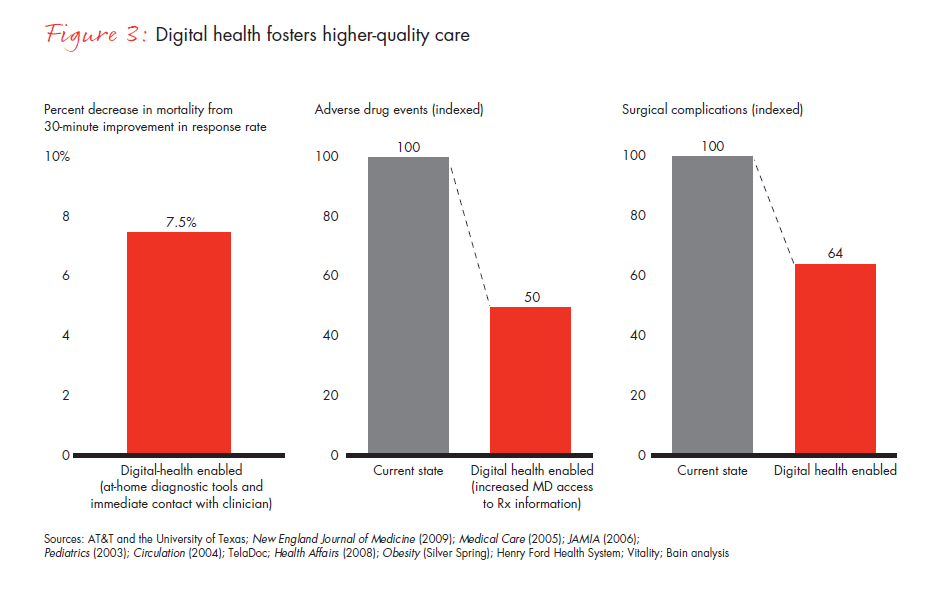
Barriers to adoption—they are real and they are daunting
The adoption of new and exciting digital tools in healthcare must be accompanied by a sober and practical assessment of the barriers to adoption. There are three basic types of barriers: participant adoption barriers, organizational barriers, and policy and regulatory barriers.
As a sector, healthcare does not have a track record of proactively adopting new technology, and in fact, has low levels of investment in IT compared with other data-driven industries such as financial services.
Concerns over the cost of IT systems and the need to secure extremely sensitive patient health data partially explain these low levels of investment. However, new technologies are becoming both less expensive and more secure than legacy IT. For example, Bain analysis suggests that by 2014, cloud technology will have reduced costs by 30% to 40% compared with legacy IT.31 And security concerns may fade as highly secure cloud-based systems are developed and tested, as is currently happening in other sensitive industries.
We believe there will be two waves of adoption of digital health by providers. The first wave has already begun. Some providers are already using mobile technologies such as tablets and smartphones. In fact, in 2012, penetration of smartphones is estimated at 81% among physicians vs. only 48% in the general population.32 The availability of broadband and the integration of tablets into many medical schools’ curricula will only accelerate. These tools require little up-front investment and are easy to use.
The second wave of adoption will require substantial external incentives. The early adopter effects are greater here, as these systems require substantial investment and interoperability to achieve their full potential. For example, EHR adoption was low before billions of dollars in federal stimulus funding and the prospect of reimbursement penalties created significant financial incentives for adoption.33
In the short term, the healthcare industry is likely to adopt only the “quick wins”—the easy-to-use, convenient technologies that do not require significant business model changes—and thus they will realize only 20% of the total potential value of digital health. In order to capture the remaining 80% of digital health’s potential value, companies will need to implement some quick wins and then use the incremental margins to increase IT spending by up to 5% of revenue (see Figure 4).

Organizational barriers will also pose challenges. Virtually every healthcare company is doing something related to digital technology, e.g., establishing a website, providing customers with information online, providing opportunities for online ordering and scheduling or social networking. These efforts are likely to be scattered across the organization, with each department or product team squeezing out a nod to digital technology from a piece of the marketing budget. The digital approach becomes fragmented and underpowered and fails to capture the full potential of a more integrated approach. What each organization needs is a more centralized approach, one that has its own budget, is separate from the IT department, is coordinated across the organization and has senior executive endorsement.
The remaining barriers to adoption relate to public policy about reimbursement and regulation and are much more difficult for an individual company to address and resolve.
The two largest areas of digital health value creation— reduced acute episodes through care coordination for patients with chronic conditions and matching patients with low-cost, high-quality providers—may require more significant reimbursement reform to be widely adopted.
- Care coordination may require a more rapid implementation of bundled payments that reward providers for investing in the primary care of chronic-care patients to avoid acute episodes. While this type of payment is one of the elements of health reform, it is not yet widespread and may take a decade to fully implement.
- Matching patients with low-cost, high-quality providers will depend on comparable quality data and will require increased competitive pressure before payers willingly make changes to their networks, policies and product design. Change will not come without integrated and more accessible data about provider performance—data that are not easily available today.
Finally, regulatory barriers continue to loom large in the minds of payers and providers considering these new technologies. However, as the need to slow the growth of healthcare costs becomes more and more critical, we believe that regulators will clear the regulatory roadblocks and approve technologies that can help to bend the cost curve. While the security and privacy of patient data will remain of paramount concern to patients, we believe that regulators will continue to provide more clarity in regards to HIPAA34 privacy and security regulations and will show more flexibility on legislative issues such as “standing authorization” to enable data to be shared when it can improve a patient’s care.
Who will be the winners and losers in the digital transformation? (See Figure 5)
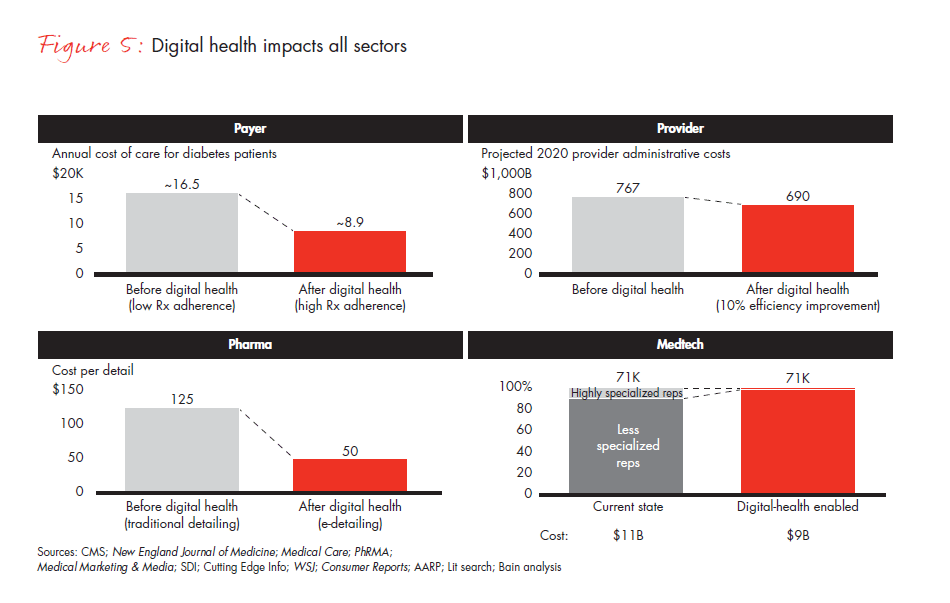
Patients
There are early signs that many patients rapidly adopt the new digital tools when they are available. Patients may not realize the extent to which the quality of care differs from provider to provider, but the digital revolution will certainly speed up their access to integrated data, quality providers, more tools to manage their own health and communities to help them manage their disease state through gaming, social media or other innovative forms of engagement. How quickly will these new tools become commonplace? How will it effect the way patients take responsibility for their health?
Physicians and other providers
If digital health can reduce the time physicians and other providers spend on administrative tasks, they will be clear winners. Easy access to one another’s expertise and patient information can elevate the practice of medicine from an art to more of a science—and even make it more fun for the practitioners. The new standardization will, however, cause a certain loss of autonomy for physicians. As physicians aggregate into larger practices, they will lose some of their professional decision- making power over individual treatment decisions.
Will the benefits of greater access to patients and more information outweigh the loss of autonomy?
Brick-and-mortar providers
In almost every scenario, the use of evidence facilitated by digital technology will reduce the need for hospital beds and put pressure on community hospitals and academic medical centers (AMCs) to do more with less. Hospitals will experience tremendous competitive pressure to adopt the latest health information technology (HIT), and the cost of HIT will only drive down their already small margins. We believe AMCs will be at an initial advantage, with greater margins to invest in those new technologies. But as community hospitals catch up, digital health will begin to level the playing field between the state-of-the-art facilities at AMCs and the community hospitals through adoption of standards of care. Will digital health accelerate the ability of community hospitals to capitalize on their low-cost position to gain share?
Payers
The line between payer and provider is becoming increasingly blurred. In light of market trends, payers will have to fundamentally shift their business model, and digital health will be a critical component of getting there. Will payers play a small role and cede much of care management to providers? Or in a future that requires IT infrastructure to enable treatment, are payers in the best position to become the IT provider that powers the whole system? Will payers maintain their transactional role? Or can they play a broader role in care management?
Pharmaceutical companies
The digital revolution has the potential to turn the world upside down for pharmaceutical companies. With easier access to data, all products will be reviewed more carefully and thoroughly by public and private payers. In the past, data about patients came mainly from clinical trials. With the advent of tools that can transmit individual patient data quickly and accurately, the challenge will be to speed the process of research and development so that these companies can create better drugs on a faster timeline. When companies do create a better product, digital technology will enable a more rapid commercialization of the product. But success for pharmaceutical companies will depend on their ability to demonstrate real clinical as well as economic benefit to those who are paying the bill. Can pharmaceutical companies get ahead of the curve of digital adoption and maintain a seat at the table?
Medical device companies
The adoption of digital health will be an opportunity and serious challenge for the medical device industry as well. To the extent that the digital revolution speeds the creation of smarter devices that provide real clinical and economic benefit, there will be many business opportunities—better tools for patient monitoring and tools to keep patients out of hospitals and emergency rooms. However, like pharmaceutical companies, medical device companies will have even more pressure to prove the value of their products because the data will tell payers if a product is worth it. Medical device companies will have to create more compelling outcomes-based research, as well as lower costs to maintain sales in an environment in which procedure volume is likely to decline. There will be advantages in inventory tracking and reduction in salesforce through digital tools, as well as better access to information for patients and providers. But overall, digital health will likely begin a move toward standardization, not differentiation, of devices. More and more decision making is already shifting to institutional procurement and away from the prior decision makers—physicians. How can medical device companies use digital health to continue to differentiate their products and compete in the new digital arena?
Is it all worth it?
Healthcare is at a tipping point, and part of the transformation of healthcare will be digital health. Like the financial services industry, these new tools will provide better access, quality and innovation at a lower cost of service. Once these tools are in place, customers will demand them. Can you imagine choosing a bank without automated tellers or the ability to monitor and pay your bills online? Investing in these technologies is compelling, regardless of your sector, and we believe those who take advantage of these tools will be the biggest winners.
Chuck Farkas is a partner with Bain & Company and a leader in the firm’s Healthcare practice. Tim van Biesen is a partner with Bain & Company and leads Bain’s Healthcare practice in the Americas. This report was prepared by Chuck Farkas, Tim Van Biesen and Sonali Madia Patel. The authors would like to thank Reynold Strossen, Trae Wallace, Kristin Heintz and Erin Yu for their research.
How IT transformed banking
Beginning with the introduction of the ATM in 1967, financial services companies have invested in transformative IT systems, which have revolutionized the industry’s cost structure, products and consumer experience. IT has drastically reduced costs, from $4.00 per interaction conducted in person in a branch to $0.08 per interaction through a smartphone app. IT has also enabled innovation, such as the E*TRADE Internet trading platforms; consumer engagement, as seen with the success of www.mint.com’s financial management tools; and quality, observed through the real-time availability of accurate information on financial markets worldwide.
To fund these investments, the financial services industry significantly increased its spending on IT. In the early 1990s, before the Internet revolution, financial services spent roughly 3% of revenue on IT, according to a Gartner report. In the mid-1990s, as the industry invested in the first generation of Internet systems, its IT spending increased to 10% of revenue. By 2000, spending had stabilized at a “maintenance” level of roughly 6% to 8% of revenue. Healthcare spends only 3% of revenue on IT today, and to achieve the same gains in cost reduction, innovation, consumer engagement and quality as financial services, it may need to increase spending to a similar degree.
A day in the life of the...
Digital health won’t just transform the back office. It will change the daily lives of people throughout the healthcare system—from doctors, nurses and clinical investigators to patients, including both the seriously ill and the very healthy.
To hear Bain & Company partners discuss how digital health will transform the day in the life of each of these stakeholders, go to: www.bain.com/digitalhealth
Physician
A host of digital technologies, many of them tablet based and Internet enabled, will make doctor-patient interactions more efficient and aid doctors with surgical preparation, pharma details and even their own continuing medical education.
Operating room nurse
From setting up for surgery to tracking equipment and approving medical devices, surgical ward nurses can rely on many new technologies to reduce costs and improve patient care.
Community health worker
The emerging markets healthcare sector is a natural fit for mobile platforms, as large mobile usage and high smartphone penetration promise to bring better quality care to poor and remote areas.
Clinical investigator
Technology can improve drug trial participation rates, monitor compliance and reduce costly drop-outs, while speeding regulatory decisions and new trial launches.
Acute care patient
Digital health technologies can detect emergencies, transmit data from patients on their way to the emergency room, minimize costly transfers and allow patients to be discharged earlier by monitoring them remotely for post-treatment complications.
Chronic care patient
Remote monitoring, social media and even gaming can improve medication adherence and speed intervention for patients with conditions that can quickly become dangerous and expensive if not controlled.
Healthy patient
Digital health isn’t only for the sick. Exercise monitors, calorie trackers, fitness-oriented social networks and other digital technologies can help the healthy stay that way.
1 Brian Dolan, “FDA clears Smartheart mobile ECG device,” MobiHealthNews, April 17, 2012, accessed April 19, 2012, http://mobihealthnews.com/17031/fda-clears-smartheart-mobile-ecg-device/.
2 ZocDoc is an online scheduling tool. Accessed March 28, 2012, http://www.zocdoc.com/.
3 IneedMD is a glove that sends ECG information to a physician or remote location, accessed March 28, 2012, http://medgadget.com/2010/09/self_administered_12_lead_ecg_glove_for_athome_monitoring.html.
4 “How GlowCaps work,” accessed March 28, 2012, http://www.vitality.net/glowcaps_howglowcapswork.html.
5 California HealthCare Foundation, “Study finds physicians slow to transition to electronic records,” iHealthBeat, February 22, 2012, accessed March 28, 2012, http://www.ihealthbeat.org/articles/2012/2/22/study-finds-physicians-slow-to-transition-to-electronic-records.aspx#.
6 Interview with Darshan Mahajan, president of the State Medical Board of Ohio, December 2011; Bain analysis.
7 Peter Crooks, “Managing High-Risk, High-Cost Patients: The Southern California Kaiser Permanente Experience in the Medicare ESRD Demonstration Project,” The Permanente Journal, Kaiser Permanente, Spring 2005/Vol. 9, No. 2, accessed April 11, 2012, http://xnet.kp.org/permanentejournal/spring05/highrisk.html.
8 Bernie Monegain, “Henry Ford reduces hospital admissions with remote monitoring,” Healthcare IT News, September 9, 2009, accessed March 28, 2012, http://www.healthcareitnews.com/news/henry-ford-reduces-hospital-admissions-remote-monitoring.
9 Companies like OptumHealth have developed programs such as eSync that combine “medical claims and pharmacy data, lab results, self-reported data and behavioral and segmentation information” to predict a population’s medical needs and conditions before they occur and calculate the value from interventions such as increasing Rx adherence to evidence-based medicine, accessed March 28, 2012, http://www.optumhealth.com/content/attachments/110107_Value%20Driver%20White%20Paper.pdf.
10 Interview with Bain team and following sources, accessed March 28, 2012, http://www.cms.gov/reports/downloads/mccall_mgh_cmhcb_final_2010.pdf; http://xnet.kp.org/permanentejournal/spring05/highrisk.html; https://www.cms.gov/NationalHealthExpendData/downloads/proj2010.pdf.
11 David C. Goodman, Elliott S. Fisher, Chiang-Hua Chang, “Hospitalization: A Dartmouth Atlas Report on Post-Acute Care for Medicare Beneficiaries,” The Dartmouth Institute for Health Policy and Clinical Practice, September 28, 2011, http://www.dartmouthatlas.org/downloads/reports/Post_discharge_events_092811.pdf.
12 Andrew Conte and Luis Fabregas, “Costs can vary widely for same medical procedures,” Pittsburgh Tribune Review, September 25, 2011, accessed March 28, 2012, http://www.pittsburghlive.com/x/pittsburghtrib/news/s_758618.html.
13 CC Blackmore, RS Mecklenburg, GS Kaplan, “Effectiveness of clinical decision support in controlling inappropriate imaging,” Journal of the American College of Radiology 8:1 (January 2011): 19–25, http://www.jacr.org/article/S1546-1440(10)00389-3/abstract, accessed March 28, 2012, http://www.ncbi.nlm.nih.gov/pubmed/21211760.
14 Bain interviews.
15 Vonda J. Sines, “Unnecessary Surgery: The Four Most Common Unwarranted Operations,” accessed April 9, 2012, http://voices.yahoo.com/unnecessary-surgery-four-most-common-unwarranted-428454.html?cat=5; J. Bruce Moseley, et al., “A Controlled Trial of Arthroscopic Surgery for Osteoarthritis of the Knee,” The New England Journal of Medicine 347:2 (July 11, 2002): 81–88.
16 Bain analysis.
17 National Hospital Ambulatory Medical Care Survey: 2008 Emergency Department Summary Tables, accessed April 24, 2012, http://www.cdc.gov/nchs/data/ahcd/nhamcs_emergency/nhamcsed2008.pdf; Sadeq Chowdhury and Steven Maclin, “Statistical Brief #318: Expenses and Characteristics of Physician Visits in Different Ambulatory Care Settings, 2008,” March 2011, accessed April 24, 2012, http://meps.ahrq.gov/mepsweb/data_files/publications/st318/stat318.pdf.
18 James E. Mansfield Jr., Dennis Callahan, “Benefits of over-the-counter heartburn medication to consumers and the healthcare system,” NielsenHealth, December 7, 2008; National Ambulatory Medical Care Survey, Centers for Disease Control and Prevention’s National Center for Health Statistics, 2008; www.teladoc.com.
19 Expert interview; ibid James E. Mansfield and Dennis Callahan, “Benefits of over-the-counter heartburn medication to consumers and the healthcare system,” NielsenHealth, December 7, 2008, accessed April 24, 2012, http://www.chpa-info.org/media/resources/r_5333.pdf; Health Care and Business: Using new technologies to reduce costs, improve access and increase employee satisfaction, Teladoc, accessed April 24, 2012, http://www.teladoc.com/pdfs/Telehealth-Special-Report.pdf.
20 The “EyeSnapi” application was invented by Palo Alto ophthalmologist Harvey Fishman, Ph.D., http://abclocal.go.com/kgo/story?section=news/health&id=8110799.
21 Matthew Herper, “The Truly Staggering Cost of Inventing New Drugs,” Forbes, February 10, 2012, accessed April 24, 2012, http://www.forbes.com/sites/matthewherper/2012/02/10/the-truly-staggering-cost-of-inventing-new-drugs/.
22 Charles Babcock, “Eli Lily Uses Web to Broaden Drug Research Reach,” Crowdsourcing.com, September 14, 2011, accessed April 24, 2012, http://www.crowdsourcing.org/document/eli-lilly-uses-web-to-broaden-drug-research-reach/6615.
23 Eliot Van Buskirk, “Harvard-Based Crowdsource Project Seeks New Diabetes Answers—and Questions,” Wired, February 3, 2010, accessed April 9, 2012, http://www.wired.com/epicenter/2010/02/crowdsourcing-rewires-harvard-medical-researchers-brain/.
24 Sage Bionetworks is a new medical research organization that works through partnerships with other research organizations to gather data and provide training in research methodology, accessed March 28, 2012, http://sagebase.org/info/faqs.php.
25 Sermo is an online resource for physicians to engage in discussions about clinical issues, accessed March 28, 2012, http://www.sermo.com/.
26 PatientsLikeMe is an online resource for patients to share experiences and gather data about their treatment, accessed March 28, 2012, http://www.patientslikeme.com/.
27 Patient Safety Institute and First Consulting Group, “Economic Value of an Electronic Health Information Exchange (EHIX) Network,” May 2007, accessed April 9, 2012, http://www.ptsafety.org/resources/PSI_Pharma_Value_White_Paper.pdf.
28 Ibid.
29 GlowCaps presentation, accessed April 24, 2012, http://www.vitality.net/docs/pharma_presentation.pdf.
30 Giuseppe De Luca, Harry Suryapranata, Jan Paul Ottervanger and Elliott M. Antman, “Time Delay to Treatment and Mortality in Primary Angioplasty for Acute Myocardial Infarction,” American Heart Association, accessed April 24, 2012, http://circ.ahajournals.org/content/109/10/1223.
31 Bain Research, “Cloud Computing POV: Complete Integrated Materials,” (updated January 2012).
32 Manhattan Research, “Physicians and Mobile: Profiling Advanced Smartphone Users,” 2010, 4; Mark Walsh, “Nielsen: Smartphone Penetration Reaches 48%,” Online Media Daily, February 21, 2012, accessed April 9, 2012, http://www.mediapost.com/publications/article/168085/nielsen-smartphone-penetration-reaches-48.html.
33 Edward Fotsch, “Health IT and Rapid Adoption of Electronic Health Records in the US,” PDR Network, April 2011, accessed April 9, 2012, http://www.gs1.org/docs/healthcare/news_events/060411/26_Fotsch_EHR.pdf.
34 HIPAA is the Health Insurance Portability and Accountability Act of 1996, accessed April 24, 2012, http://www.hhs.gov/ocr/privacy/hipaa/understanding/summary/index.html.




