Frontline of Healthcare

Резюме
- A recent Bain survey shows that 25% of US clinicians are considering switching careers, primarily due to burnout.
- Clinicians care most about factors like the quality of patient care, a manageable workload, and flexibility—yet many aren’t satisfied with their employers on these dimensions.
- To retain their workforce, providers can consider near- and long-term actions that mitigate burnout, spark engagement, and foster a supportive culture.
US clinicians have been bearing the brunt of a brutal environment over the past two years. As clinical acuity and medical uncertainty rose with the pandemic, providers’ financial health steadily slipped, and labor challenges mounted. Now, around a third of US clinicians are considering switching employers, according to Bain’s recent Frontline of Healthcare survey. On top of that, a quarter are considering switching careers altogether (see Figure 1).
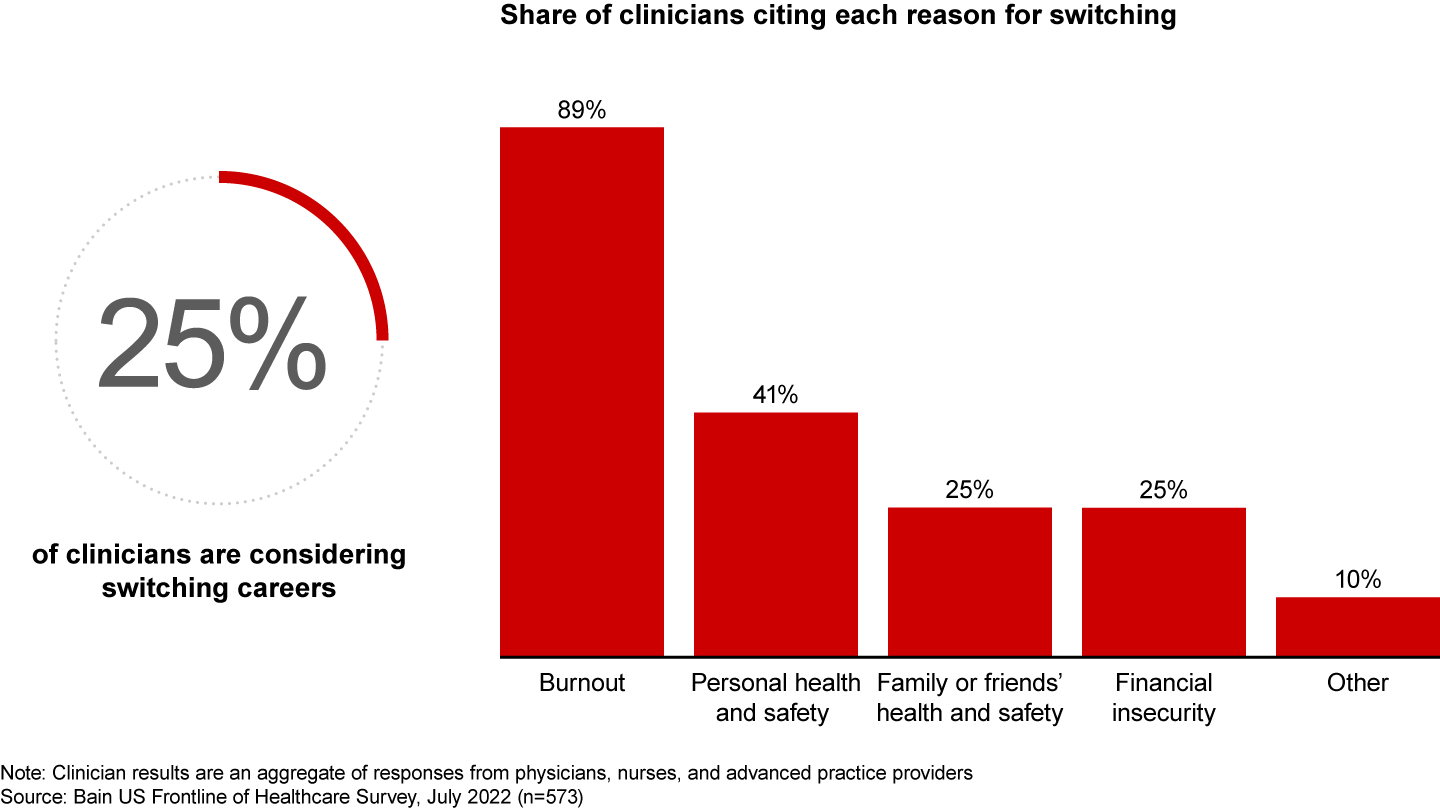

Of those considering leaving the field entirely, 89% cite burnout as the main cause. Additionally, around 40% of all clinicians surveyed say they don’t have the resources they need to operate at full potential. They report a lack of effective processes and workflows, supplies, and equipment. And 59% don’t believe their teams are adequately staffed.
In these conditions, burnout is pervasive: Based on our survey, 63% of clinicians feel worn out at the end of the workday, 51% feel they don’t have time and energy for family and friends during leisure time, and 38% feel exhausted in the morning at the thought of another day at work. It’s no wonder that around half of physicians, advanced practice providers (APPs), and nurses say their mental health has declined since the start of the pandemic.
Many of these stories are well known, but the data paints an even more vivid picture. The effects of burnout should not be underestimated. Our survey shows that the Net Promoter ScoreSM from US physicians—a measure of their likelihood to recommend their employer—has tumbled from 36 points in 2020 to 19 points today. Clinicians at management-led practices—for instance, those operated by a hospital, health system, parent company, or private equity fund—are considerably worse off, giving a Net Promoter Score of 6 points, compared with 40 points for those at physician-led practices. Nurses are also extremely dissatisfied, giving a Net Promoter Score of 11 points.
Amid skyrocketing turnover rates, the potential resignation of a quarter of the workforce would further exacerbate the tight labor market, which is already on track to be short 38,000 to 124,000 physicians by 2034, according to the AAMC. Turnover is highest among hospital-based staff, increasing 6.4 percentage points in the past year alone, according to NSI’s National Health Care Retention & RN Staffing Report. The staff RN turnover rate has reached 27%, exceeding the turnover rate for hospital staff overall (26%) for the first time.
What can employers do to improve frontline well-being, satisfaction, and retention?
The message from clinicians is clear: better compensation, support to deliver high-quality patient care, a more manageable workload, flexible work arrangements, and more clinically focused job responsibilities. These are the five most important criteria for clinicians across all roles (see Figure 2). And yet, nearly 40% of clinicians aren’t satisfied with their employers across most of these dimensions.
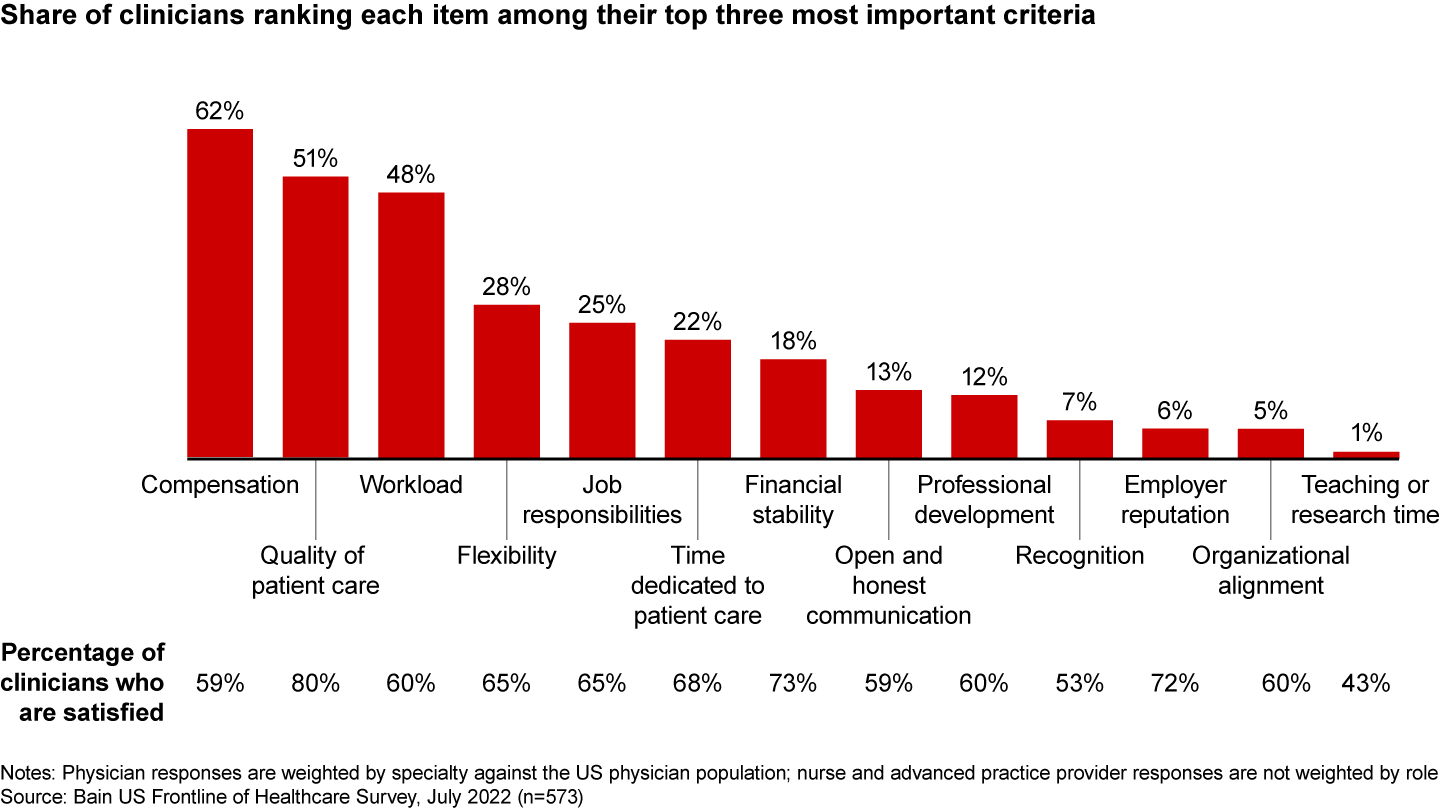

Given rising inflation and labor shortages, providers will need to ensure they are offering fair and adequate compensation to attract and retain talent. In addition, several other near- and long-term fixes can mitigate clinician burnout, spark employee engagement, and foster a more supportive work culture.
Mitigate clinician burnout
Near term: Routinely assess and address clinician well-being. Leading employers are measuring clinician well-being and providing access to mental health support at the individual and group level. Although numerous state, federal, and professional resources exist, there’s still much that can be done in-house.
Ochsner Health, for example, has stood up an Office of Professional Well-Being. It also developed a four-pronged approach to mental health, including measuring and benchmarking overall staff wellness, deploying webinars around personal and professional well-being, asking leaders to destigmatize mental health discussions by sharing their own stories, and creating a resource group for women to discuss the unique stressors they face.
Other organizations, including Rutgers Biomedical and Health Sciences, Hartford HealthCare, and the University of Michigan Medical School, have established a chief wellness officer (CWO) role. The CWO identifies causes of worker anxiety, partakes in operational decision making, guides organizational response in times of crisis, and deploys support resources around workers’ well-being.
Long term: Invest in technology and people to ease administrative burdens. From scribes to coders to ancillary support services, the right technology and personnel can help reduce the draining administrative tasks that steal focus from clinicians’ most valuable work. Tools with automated referrals or scheduling, intelligent workforce management, and intelligent workflow management can also increase the day-to-day predictability of the job, greatly improving employees’ sense of work-life balance in a demanding environment.
However, around 50% to 70% of clinicians say they’ve still never used these high-potential technologies. Most clinicians expressed that they would like to use them, if they could.
Several available tools promise to reduce clinicians’ manual tasks and remove obstacles to productivity. For instance, Pega’s AI-based tools help providers automate workflow management tasks, including patient correspondence and data writing or retrieval, to cut down on errors and labor. Similarly, CareAlign, a clinician-designed, collaborative workflow tool, touts that more than 75% of its users have boosted efficiency, saved time, and prevented clinical errors.
Long term: Redesign the clinical operating model. Rapidly evolving care models, fast-paced technology development, and changing patient preferences have made it difficult for clinicians to work at the top of their licenses. In fact, more than 30% of clinicians report that they don’t work at the top of their license for most of their workday—compromising their productivity and contributing to fatigue.
Some providers are implementing multidisciplinary care teams (MDCTs) in both inpatient and outpatient settings to help alleviate clinicians’ workload. These providers are upending the clinical operating model by assembling formal teams with varied roles and skill sets based on the setting and the needs of the patient population. For example, a team could be comprised of physicians, APPs, RNs, pharmacists, health coaches, and social workers.
Bellin Health customizes its multidisciplinary teams for specific types of care. For example, nurses, IT, admin support, physical therapists, specialist physicians, and others may come together on an acute lower back pain team. Team members support physicians by completing forms, scheduling appointments, preparing prescription orders, and more. By fully rolling out this model, Bellin Health improved overall clinician satisfaction, delivered more timely care, and even decreased costs and increased revenue per patient.
MDCTs can be a real game changer—and clinicians are the first to agree. Around 70% believe that working in an MDCT would not only allow them to work at the top of their license but also to deliver high-quality patient care and improve the patient experience and satisfaction. Similarly, more than 70% of patients who received care from an MDCT report greater quality and convenience of care.
Spark employee engagement
Near term: Engage clinicians in decision making. Clinicians who feel they have a voice in their organization are far more satisfied at work. In fact, those who say they are sufficiently engaged in making important strategic and operational decisions give their employer a Net Promoter Score of 47 points, compared with negative 64 points for those who don’t. Still, around a third of clinicians don’t feel they are involved in any strategic decision making today. And only around 40% say their employers have feedback systems to give them a voice.
Good engagement can take many forms. Providers can set up an anonymous employee survey, host a town hall, initiate a global request for feedback, or embed clinician representatives in the decision-making bodies throughout the organization. Simply giving clinicians a platform to voice their opinions can help them feel more involved in decision-making processes and engaged in their organizations.
Long term: Elevate employee voices with feedback systems. Engaged employees are invaluable: Inspired and satisfied employees are three times more productive and 50% less likely to leave.
What’s more, highly engaged employees are crucial to delivering the differentiated customer experience that healthcare providers need to attract and retain patients in today’s highly competitive market. Bain research shows there’s a virtuous cycle between employee satisfaction and customer advocacy. Enthusiastic, loyal employees provide better experiences for customers, approach the job with a productive energy, and come up with creative service improvements. In fact, a higher employee Net Promoter Score (eNPS) is strongly correlated with a higher customer Net Promoter Score.
Leading companies are going beyond mere metric tracking to set up a true employee Net Promoter System®. These providers establish a closed feedback loop that allows them to respond to employee feedback quickly and escalate systemic issues. By ensuring issues and opportunities are routed to the right place, prioritized, and resolved, the system promotes continuous improvement of the employee experience, heightening morale and generating greater patient advocacy.
Foster a supportive work culture
Near term: Build a culture of recognition. Around 55% of clinicians who aren’t considering switching careers feel that practicing medicine is a calling. They report the positive impact they make throughout their careers as the biggest reason for staying.
Championing these moments of impact—from early recognition of a patient’s clinical change, to helping a patient better manage a chronic condition, to investing time to train future clinicians—on a regular basis can bolster the organization’s culture. Recognition can go a long way in making clinicians feel valued for their efforts and work—as they should. It can feel just as rewarding as financial incentives, making it a low-cost, high-ROI way to boost employee satisfaction and retention. Yet providers don’t celebrate their employees often or well enough: Only about half of clinicians are satisfied with the recognition they are receiving today.
Long term: Champion support and inclusion. Building a distinctive culture of support is as powerful as it is difficult. It’s crucial to strengthening an organization’s talent strategy and delivering value. Yet today, more than 30% of clinicians say they don’t feel included in their organizations. And almost 60% feel they don’t get the coaching and mentorship they need.
Building a diverse and inclusive culture isn’t easy, but it’s the right investment to make. Nearly half of clinicians cite an inclusive work environment as being “very important” when choosing an employer. And across industries, companies with both diverse and inclusive teams are five times more likely to innovate than organizations with low diversity and no inclusion.
We’ve seen several best practices accelerate providers’ DEI journeys. Leading companies invest heavily in DEI data infrastructure, routinely collecting data and personal stories to understand the company’s current state and track progress. In addition, they put marginalized voices at the center of their approach, to ensure they have a robust understanding of the organization’s starting point and to guide their actions going forward.
Strong coaching and mentorship are also directly correlated to employee satisfaction and well-being. A study by the Mayo Clinic found that each 1-point increase in a supervisor’s leadership score was associated with a 7% decrease in the odds of employee burnout and an 11% increase in the likelihood of employee satisfaction. Supervisors with high leadership scores hold career development conversations, provide coaching and feedback, go out of their way to recognize good work, and encourage direct reports to share ideas.
Providers have long focused on delivering high-quality care for their patients. Now, the imperative is clear: They need to ensure this high-quality care extends to their clinicians and employees. Those that take near- and long-term actions today will not only be better positioned to retain their current workforce but also to attract the next generation of top talent.
The authors would like to thank Monica Pinto Basto and Brittany Rodriguez for their contributions.