Brief

Резюме
- The volume of procedures at ambulatory surgery centers is forecast to grow by 6% to 7% a year through 2021.
- Orthopedic, spine and cardio procedures will increase the fastest through the mid-2020s.
- Medtech companies’ traditional commercial model is too costly and complex for ambulatory surgery centers.
- Surgeons at ambulatory surgery centers have a greater propensity than those in hospitals to switch to a competing device manufacturer if offered a discount.
Ambulatory surgery centers (ASCs) are transforming healthcare delivery as well as the market for medical devices and equipment. By focusing on routine, lower-risk procedures in a more convenient setting, ASCs can offer surgical procedures at rates 35% to 50% lower than hospitals. That’s saving the US healthcare system an estimated $40 billion a year and fueling ASC growth. In 2018, 5,700 ASCs operating in the US performed 23 million procedures and generated $35 billion in revenue.
The steady growth of ASCs creates new challenges and opportunities for medtech companies. Most leadership teams have been focused on acute care hospitals as their primary customers given their historical dominance of most surgical procedures; as a result, they have not devoted much strategic energy and attention to ASCs as an important customer channel.
Now it’s becoming urgent. ASCs performed more than half of all outpatient surgeries in 2017, up from 32% in 2005, and their influence is set to increase. Bain research shows procedures performed at ASCs will grow by an average 6% to 7% a year through 2021, up from 4% to 5% over the past three years (see Figure 1). Orthopedic, spine and cardio procedures will grow the fastest. That shift will increase price pressure on medical devices and products because ASCs have lower reimbursement rates and ASC-based physicians are more price sensitive than their hospital-based peers are. Selling to ASCs, which are smaller, lower volume and more geographically dispersed, drives up the costs of sales and distribution and adds complexity to medtech companies’ business models.
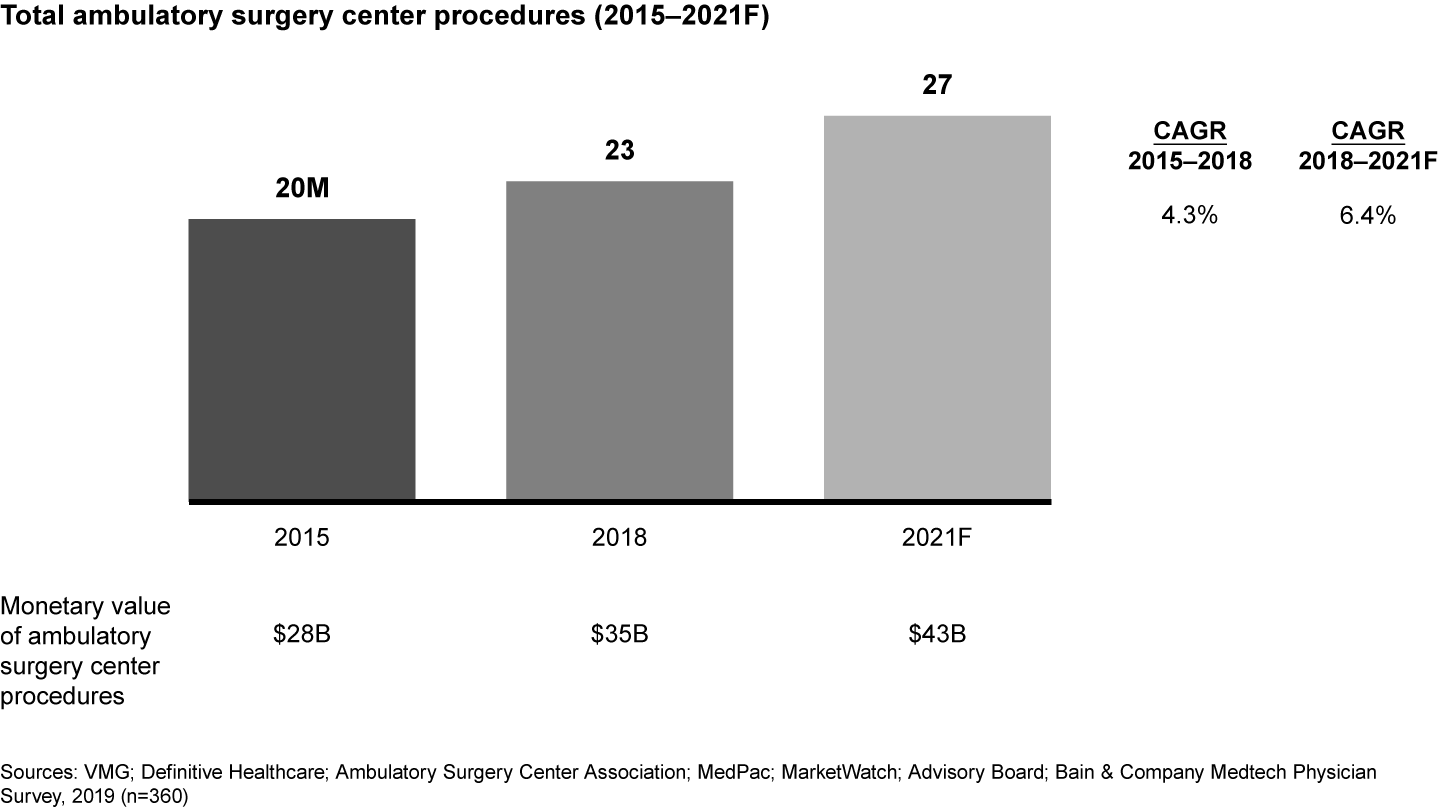

A handful of medtech leadership teams are forging strategies to capture that new business. To compete effectively for a share of the outpatient surgery market, the leaders in this fast-growing sector are turning necessity into a virtue by developing lower-cost service models and simplifying their product offerings. They also are providing ASCs with a wider range of customized services and offering partnerships that address ASC needs. Such services include support for administration, scheduling, operating room utilization and staffing.
The growing volume of procedures handled by ASCs affects the broader healthcare industry as well. Hospitals and payers are rethinking their business models as highly profitable surgical procedures shift to outpatient centers. Many hospital networks are responding to this trend by acquiring ASCs to recapture a slice of the lost business—around 25% of ASCs now have hospitals as shareholders—while others are acquiring physician groups to control referral patterns. Payers continue to support the shift to lower-cost healthcare settings, and some are becoming ASC operators. In 2017, Optum acquired Surgical Care Affiliates, significantly expanding its own ambulatory surgery business.
Accelerated growth
Broad industry trends are fueling the growth of ASCs, the first of which was founded in 1970. A steady rise in healthcare spending has put fierce pressure on costs and margins throughout the industry, encouraging the shift to outpatient care. Payers are helping steer procedures to ASCs by lowering provider reimbursements for hospitals and reducing patient copayment for procedures performed at outpatient centers.
ASCs hold strong allure for physicians as well. A recent Bain survey showed that nearly 60% of physicians who are not affiliated with an ASC are interested in practicing at one. As advantages, they cite the potential to own equity in the center, the increased control over their own surgery schedules and the reduced bureaucracy when compared with traditional hospitals.
Over the next three years, growth in the volume of procedures performed in ASCs will accelerate, propelled by cost pressure, Medicare approval to reimburse a growing number of procedures for ASCs, the rise of results-based care models, and physician and patient preference for outpatient surgery centers.
Our analysis shows single-specialty centers focused on orthopedics, cardiology and spinal surgery will see the fastest growth in volume of procedures through the mid-2020s. These centers also are likely to have a higher average reimbursement per procedure. Let’s take a closer look at the ASC growth dynamic in each of these specialties (see Figure 2).
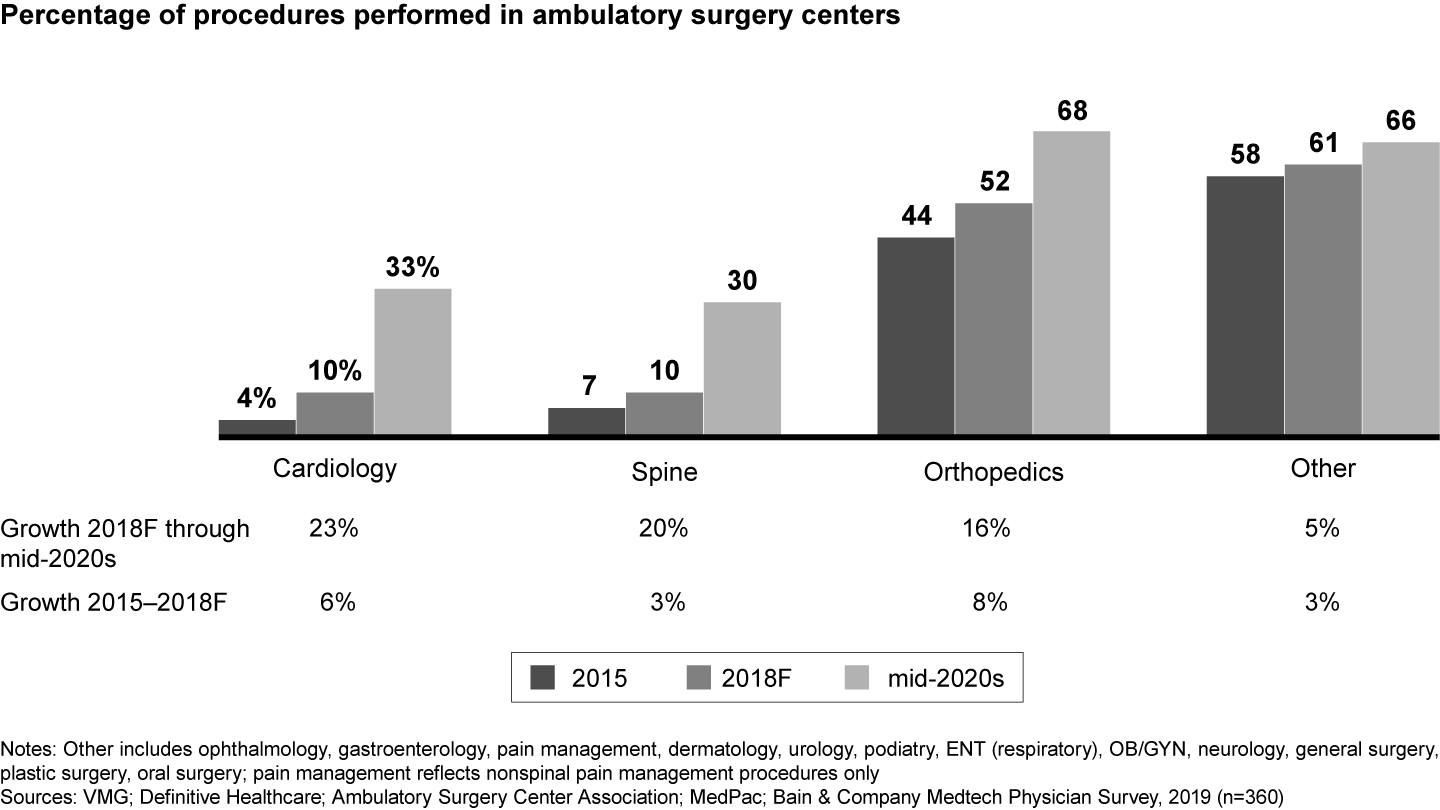

Orthopedics. Commercial payers recently began reimbursing total joint replacements in ASCs, where they typically cost 30% to 35% less than the same procedure in a hospital. That shift has led to an eightfold increase in the number of ASCs offering total joint replacements over the past four years, to a total of 250 in 2018. Medicare is now following suit: In 2018, it removed total knee arthroplasty from the Medicare inpatient-only list, and many expect other orthopedic procedures to follow. The decision to reimburse knee and joint procedures at ASCs will have a significant effect on ASC volumes: Total joint replacements are one of Medicare’s most common inpatient procedures, accounting for more than $7 billion in annual spending. Bain research indicates the share of hip replacements performed in ASCs will grow from slightly more than 9% today to nearly 25% by the mid-2020s, while knee replacements performed in ASCs will rise from 10% today to nearly 30%.
Spine. ASCs performed slightly more than 10% of all spinal surgeries in 2018, but based on our survey findings, we expect that figure to rise to around 30% by the mid-2020s. Physicians still perform the majority of outpatient spinal surgeries in hospital outpatient departments rather than ASCs. The number of ASCs specializing in spinal surgery rose in 2019, however, to 145, up from 35 in 2013, and physicians are increasingly willing to shift these procedures to ASCs. For instance, 86% of spine surgeons expect lumbar discectomies to move to ASCs at accelerating rates over the next three years, while 74% anticipate the same change for cervical-lumbar decompressions. Medicare approval for procedures performed in ASCs will contribute to the shift—the Centers for Medicare & Medicaid Services (CMS) approved two cervical spine procedures in 2018. In addition, spine procedures are among the most profitable for ASCs. That creates an incentive for spine surgeons to shift spinal surgeries to ASCs.
Cardiology. Cardio surgeries also are growing rapidly from a small base. ASCs handled an estimated 10% of all cardio procedures in 2018, but based on our survey findings, we expect ASCs will be performing between 30% and 35% by the mid-2020s, for an annual growth rate of approximately 20%. Diagnostic cardiology procedures began shifting to outpatient settings in 2005 with Medicare’s approval of outpatient arterial endovascular interventions. That approval led to the rapid spread of office-based laboratories across the US, with the total recently surpassing 500. Today, cardiologists and regulators are becoming increasingly comfortable performing procedures such as angiograms and angioplasties in ASCs. Over the first half of 2019, CMS added 12 cardiac catheterization procedures to its ASC-covered list.
A different kind of customer
The business model at most medtech companies is designed for large hospitals and provider systems, which have high patient volumes, a broad range of procedural complexity and well-established buying behaviors. For ASCs, which are smaller, more nimble and have simpler needs, that commercial model is often too costly and overly complex.
Importantly, surgeons at ASCs have greater direct influence over purchasing decisions for medical devices and equipment compared with surgeons working in hospitals, where procurement departments have a role. At ASCs, 70% of physicians are the primary decision maker or have direct influence on the decision to purchase medical devices or equipment compared with slightly less than 45% at hospitals, Bain research shows (see Figure 3).
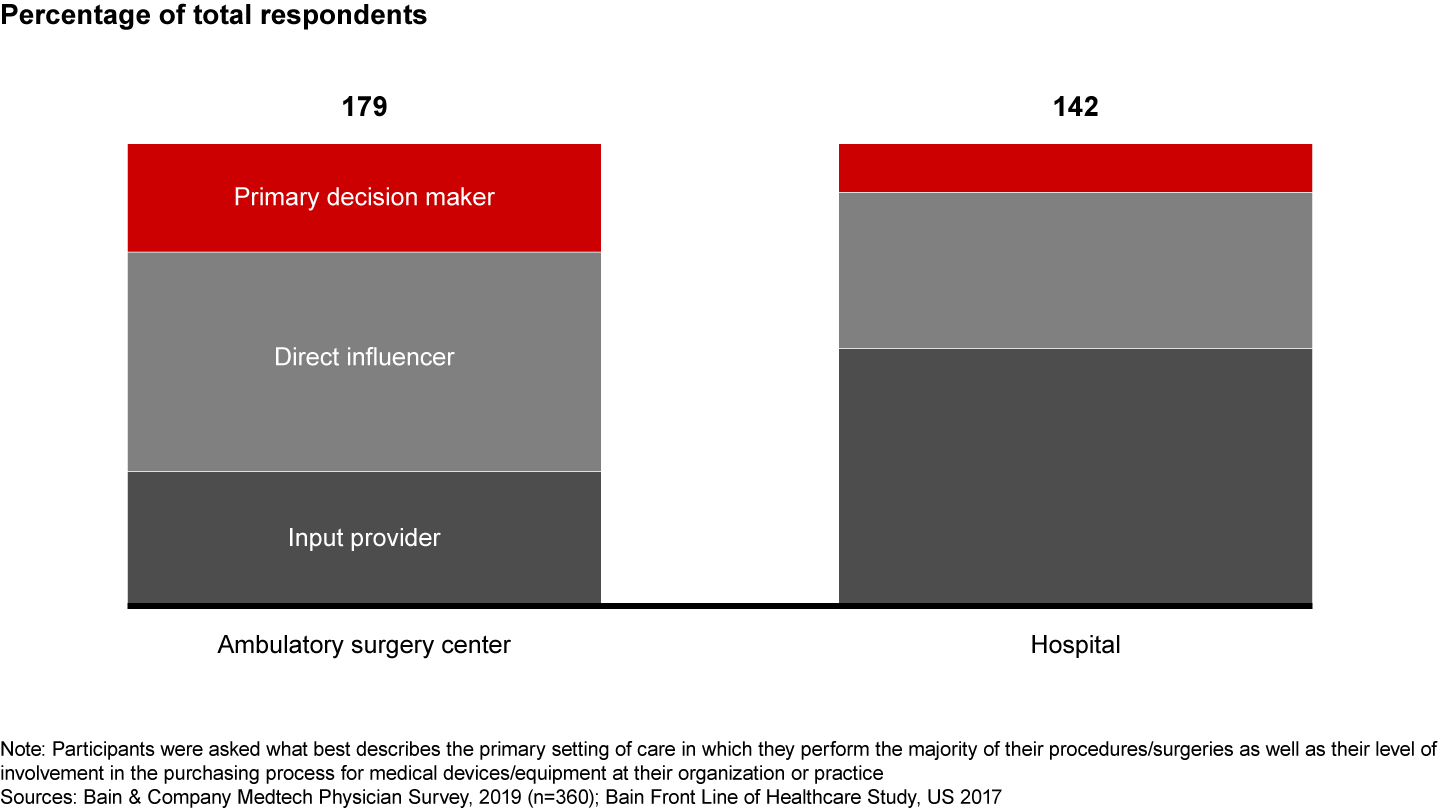

Since payers reimburse ASCs less for the same procedure carried out in a hospital, ASCs are under constant pressure to reduce costs and improve efficiency. The risk to manufacturers is that ASCs will have a greater propensity than hospitals to switch to another manufacturer. Our research shows that ASC physicians are more price sensitive when purchasing medtech devices and expect lower prices than hospitals pay for the same equipment, especially in orthopedics. Sixty percent of ASC physicians said they would purchase a similar device from a different manufacturer if it were offered at a 15% discount (see Figure 4). Physicians in ASCs also are more likely to use innovative purchasing models and are willing to experiment with nontraditional services, such as 24-hour remote service instead of full-time onsite technicians, in exchange for a break on prices. Manufacturers will need to determine how to meet these price expectations without compromising their more comprehensive offerings in the acute care environment.
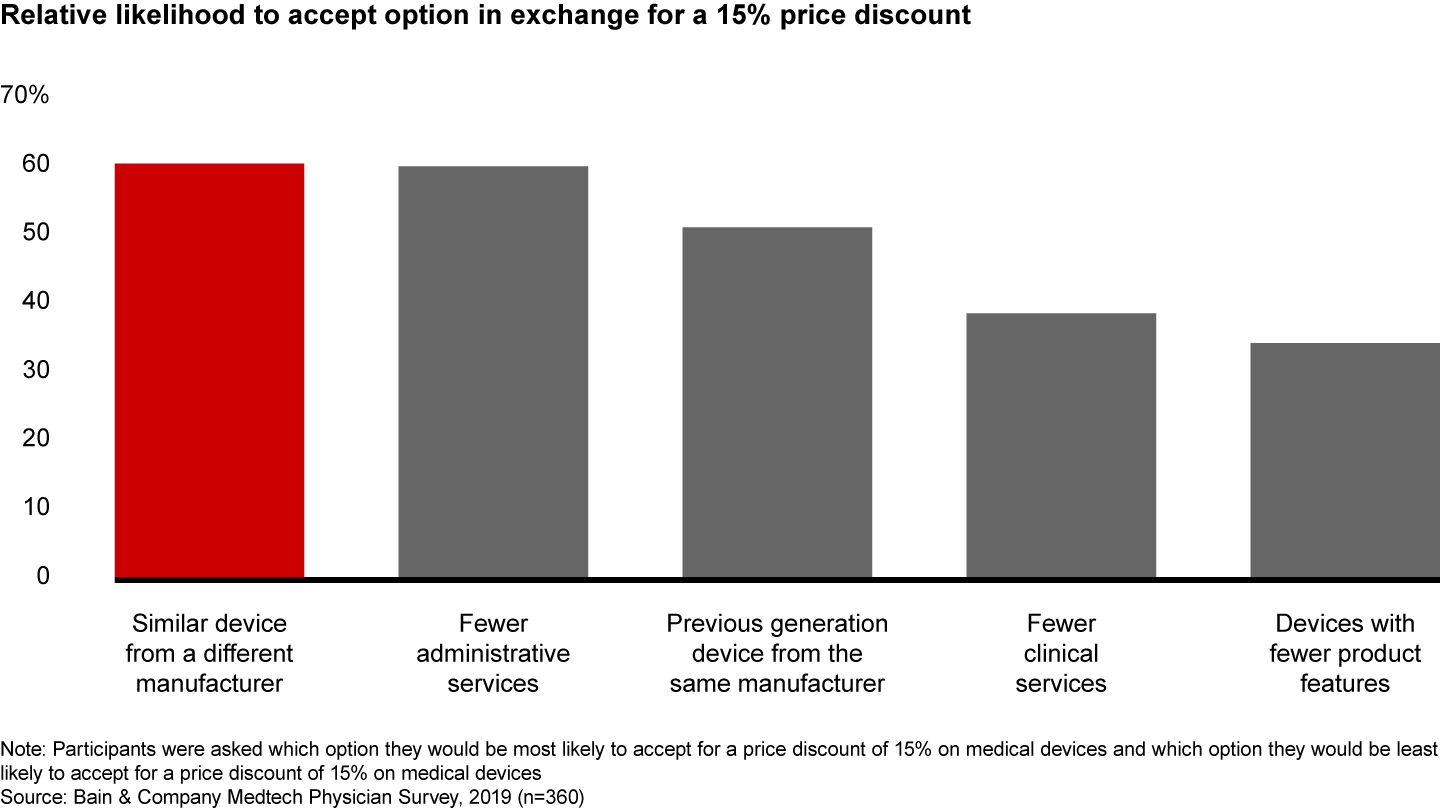

Bain research shows that ASCs differ from hospitals in the services they value most from medtech companies. ASCs rank technical support first, while hospitals say operating room coverage is most important. ASCs also rank information on payer reimbursement as a top service, while hospital physicians include information on product upgrades in their top three choices. It is important to note that ASCs are less willing to compromise on the products themselves; they may be willing to switch to a different device manufacturer to reduce costs, but they are less inclined to use previous generation products or those with fewer features. Similarly, they expect the same high quality of technical and clinical support that medtech companies provide to hospitals, but tailored to their needs.
For medtech sales and distribution teams, serving ASCs efficiently is a challenge. Outpatient centers are more dispersed geographically than hospitals, and they perform a lower volume of procedures than hospitals. They have less space for stocking inventory and don’t have sophisticated inventory management systems. As a result, ASCs have significantly different supply chain needs than hospitals, requiring medtech companies to be more flexible.
Winning in the ASC market
As outpatient surgery centers take an ever-larger slice of profitable business from hospitals, leading medtech companies are rethinking their sales and marketing models, particularly for ASCs specializing in orthopedic, spine and cardiology procedures. To succeed in this fast-growing market, medtech companies are taking four bold steps to target ASCs’ needs.
Developing lower-cost service models. Medtech companies need to adjust their sales and service models to efficiently deliver the services that ASCs value most. One example: virtual operating room representatives. They also are training in-person operating room reps to cover multiple products instead of one, increasing their versatility. In addition, winning medtech companies are adjusting their logistics and distribution models, leaning more heavily on third-party logistics suppliers, for instance, to efficiently deliver and service products in ASCs.
Simplifying products. Medtech devices that reduce customer-holding costs by minimizing required inventory or increasing single-use offerings can help address ASC needs. Medtech companies can also create streamlined procedure-in-a-box kits that are designed for lower-acuity ASC procedures, are less expensive and are easier to manage logistically.
Addressing a broader spectrum of ASC needs. New products and services may help address a wider spectrum of ASC needs to offset pricing pressure. For example, some medtech companies are offering IT services and inventory management as well as innovative partnerships to help ASCs focus on their core business and maintain a streamlined business model.
Considering new business models. As healthcare delivery models change, with payers moving into the provider space and hospitals seeking to expand their networks, medical device companies may see new and innovative opportunities to collaborate with ASCs. For example, some may become equity owners of ASCs, providing cash or capital equipment to help bring the latest technologies to these centers. Others may provide perioperative consulting or marketing services to help ASCs grow faster and improve efficiency. These new models are still experimental, but we expect leading medtech companies to carve out new paths to create value by addressing ASCs’ needs.
ASCs already are transforming the healthcare market. As they capture a growing volume of surgical procedures, outpatient centers will force down prices on medtech devices and trigger changes for payers and providers. Despite these challenges, medtech companies that pivot quickly can take advantage of ASC growth. For leadership teams keen to win their business, the market is wide open—no one has staked a major claim to this fast-moving sector. Those that lead in developing new business models for ASCs will help shape a changing market.
Tim van Biesen leads Bain & Company’s Global Healthcare practice, and Todd Johnson is a partner with Bain’s Healthcare practice. Both are based in the firm’s New York office.