Brief

Резюме
- Simply working harder or increasing funding alone will not fully address the rapidly growing backlog of deferred elective care. Instead, the growing crisis should be seen as an opportunity for innovation.
- As Covid-19 pressures subside, a bold and ambitious mission to reimagine elective care can help the NHS recover increasingly long wait times whilst meeting pent-up demand for services.
- Frontline clinicians and provider leadership play a key role in calculating how best to accelerate recovery by giving provider collaboratives the operating freedom, incentives, data, and best practices to develop systemwide solutions.
- Isolated innovations from a first wave of systems will not be enough: Planning must be embedded up-front for how to scale great ideas through a community of practitioners and a repeatable menu of solutions that act as the foundation of a proven Win-Scale-Amplify approach.
The waitlist—and public dissatisfaction—will get worse
The UK’s National Health Service (NHS) hospitals managed to treat millions of people with non–Covid-19 conditions whilst also admitting more than 400,000 severely ill Covid-19 patients. Still, delays in accessing elective diagnostics and treatments have grown rapidly—exacerbating issues that were building even before the pandemic. How much irreversible harm will result is yet to be fully realised, but the subsequent anxiety and discomfort is already very real for millions of patients.
A significant growth in the total elective waiting list (from 4.4 million in February 2020 to 5.0 million in March 2021) also masks two alarming shifts over such a short period:
- A decline in new referrals to treatment (RTTs) from about 20 million in 2019 to about 14 million in 2020
- An increasing failure to meet national standards of care, with those treated within 18 weeks down from 83% in February 2020 to 64% in March 2021 (against a target of 92%) and those waiting more than 52 weeks up from about 2,000 to over 436,000 (against a target of 0)
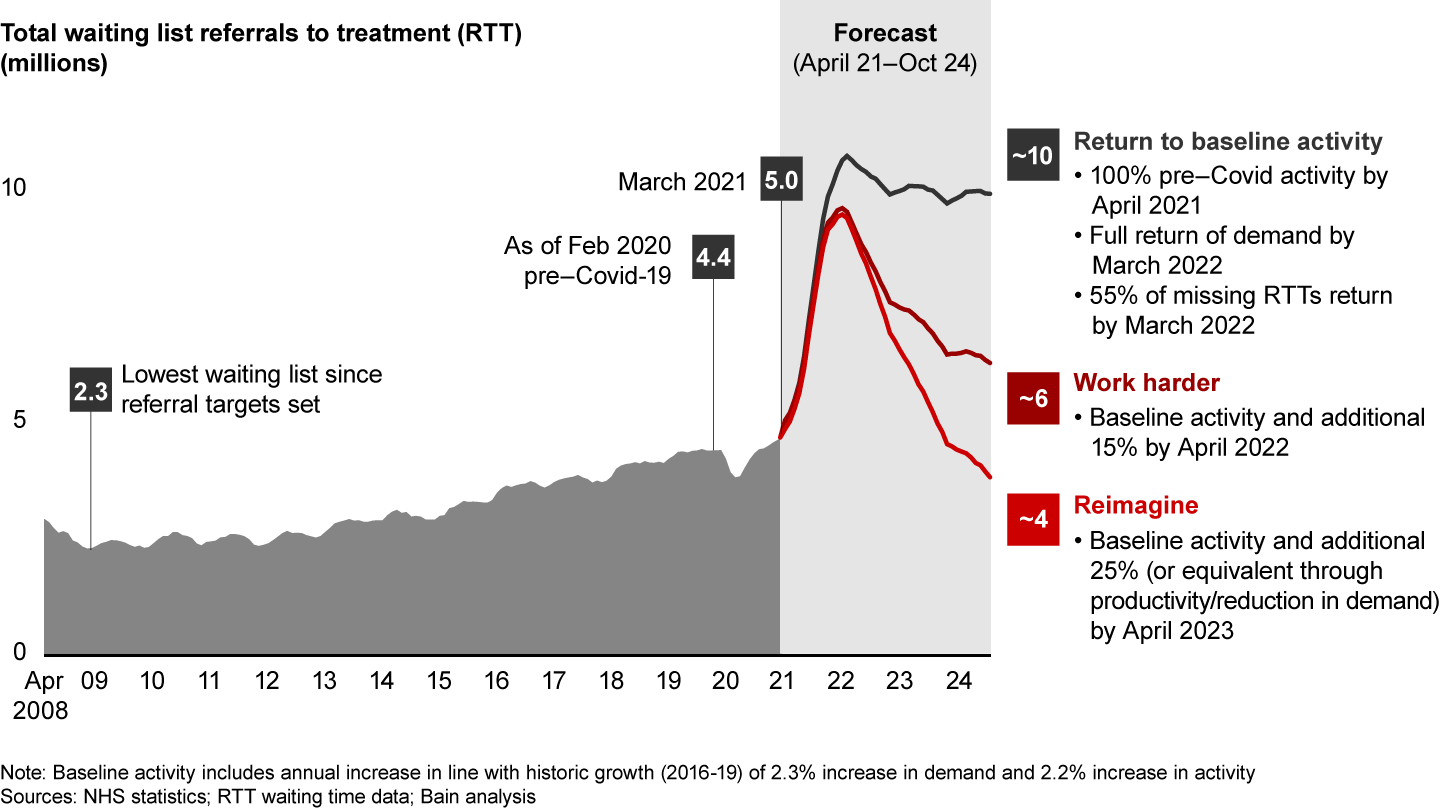
As the waiting list lengthens and levels of NHS satisfaction ratings decline, the need for a solution is becoming an increasingly urgent and public priority. Our forecasts show that by the end of the 2021–22 fiscal year, the total waiting list could range from 8 million to 10 million, driven by the return of millions of missing RTTs that did not present as expected during the height of the pandemic (see Figure 1).

Success requires transformation, not just more money or work
In the past (e.g., the 2000s), the NHS was able to reduce waiting lists through massive amounts of additional funding or by squeezing more work out of already thinly stretched staff and assets. Now, however, neither of these options by themselves are recommended—politically, practically, or physically.
This is the next great challenge for the NHS. We’ve modelled three possible scenarios for addressing the waitlist and elective care demand:
- Return to baseline. As the Covid-19 disruption subsides, elective activity returns to and remains at pre-pandemic levels. The waiting list peaks at well over 10 million. NHS systems have no way to get a grip on the need, as activity in recent years has continuously lagged demand.
- Work harder. NHS systems ramp up to 115% of pre–Covid-19 activity by April 2022. This effort reduces the waiting list, but slowly. By 2024, the list is still higher than before the pandemic—not to mention the toll that this sustained effort will have taken on an already exhausted workforce.
- Reimagine. We suggest a third path, one that sees the current crisis as a catalyst for transformation. Covid-19 has revealed the potential for rapid medical advancement and the launch of successful programmes (such as the vaccination campaign) in record time. Harnessing the collaborative mindset achieved during the pandemic, NHS systems can move beyond existing access standards and build the long-term capability and capacity to achieve new, aspirational levels of care and to inspire the workforce.
Following the success of its vaccine campaign, the NHS can reimagine the future of universal healthcare.
Our ambition is to reengineer care pathways equivalent to 125% of pre-pandemic activity levels. Funding alone is not the answer; training, recruiting, and retaining sufficient skilled clinicians to generate 125% capacity within the necessary timeline is not feasible.
Rather, the NHS will need collaboration, innovation, rapid testing and learning, and diffusion of winning initiatives to promote faster treatments, improved productivity, and earlier alternatives to costly and risky late-stage treatments.
“What we have before us are some breathtaking opportunities disguised as insoluble problems.”—John Gardner, US secretary of health, education, and welfare, 1965–68
Past successes point the way
Transforming patient treatment at scale is not new to the NHS. Past examples provide important lessons on what works—and what does not. Six efforts illustrate the possibilities (see Figure 2).
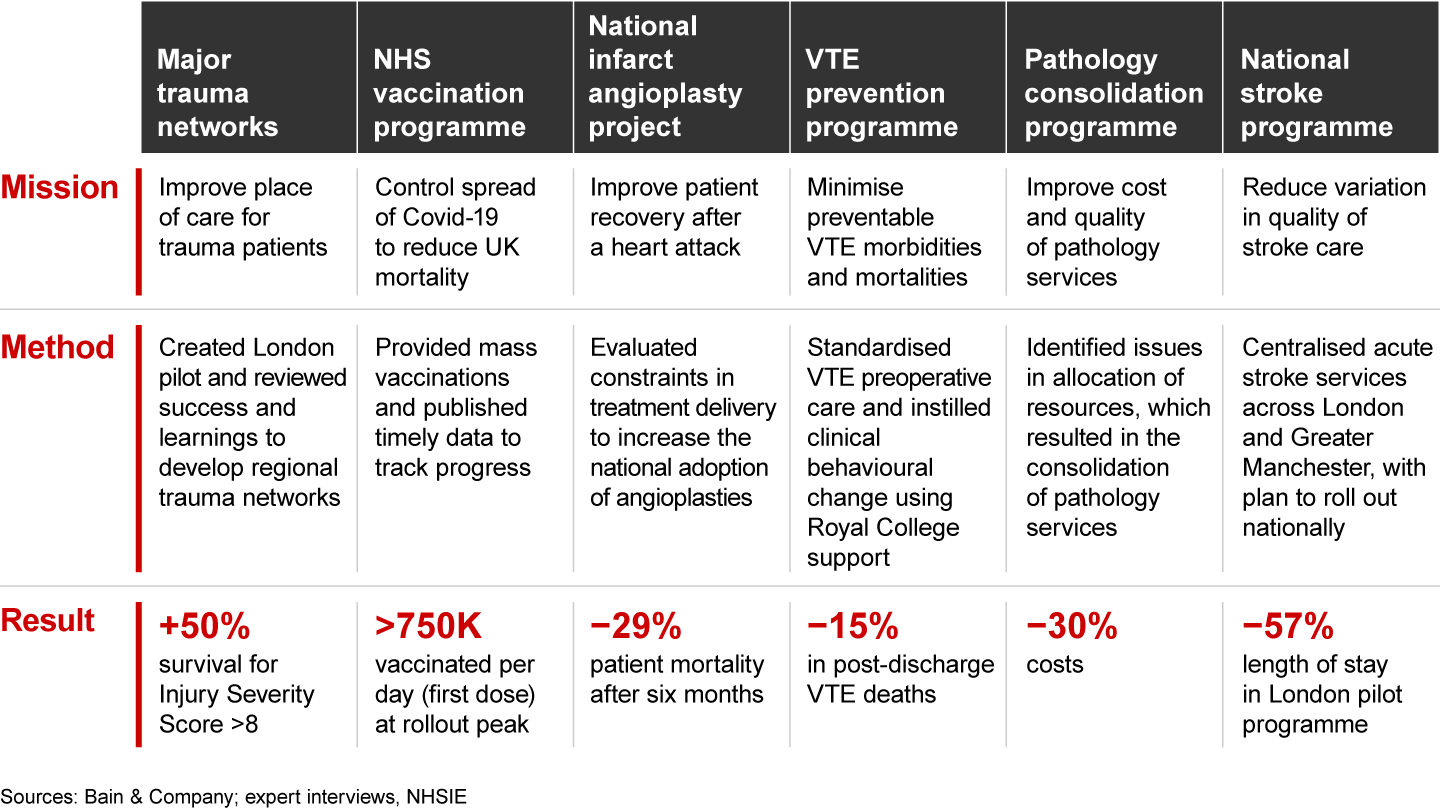

These examples provide powerful insights into how best to tackle the elective backlog and reimagine the possible. Each of the six demonstrates four critical success factors:
- Shrink the problem. NHS systems can better understand and tackle the mission (i.e., national waiting-time performance) by translating it into the smallest possible issues (e.g., cataract patients waiting more than a year in a specific ophthalmology department). For example, the NHS Getting It Right First Time (GIRFT) programme’s peer-to-peer encouragement to challenge practices and performance against best-practice pathways enables clinicians to pinpoint root causes and local constraints, thus leading to tailored solutions.
- Start fast locally, scale virally. The NHS can empower local providers and specialities to rapidly trial behaviour-changing solutions, learn from failures, review successes, and then scale the best. For example, the National Trauma Network was initially started in London. After review, this successful trauma network was scaled to a national level and increased patient survival rates by close to 20% with no major new funding or centrally dictated mandate.
- Win hearts and minds. Truly transformational change is the result not of operating models but of changes in human behaviour. Such change across the NHS requires support from the public, leaders, and external stakeholders (e.g., Royal Colleges, Treasury). The venous thromboembolism (VTE) programme, for example, aimed to reduce VTE deaths for hospital inpatients through an assessment of every patient on admission. But it wasn’t until the Royal Colleges backed the programme that assessments increased from 25% to 95% and, in turn, post-discharge VTE deaths decreased by about 15%.
- Deploy data for decisions. The NHS should use simple, accurate, and timely data to track progress and drive decision making at both the local and national levels. For example, during the Covid-19 vaccination programme, daily updates on the number of vaccinations and clear targets made progress clear to everyone and enabled early, course-correcting interventions.
A micro-battles approach and Win-Scale-Amplify model can achieve success
These lessons, which align with those learnt from other large-scale transformations, lead us to propose a micro-battles approach (see Figure 3). This tried and tested approach enables the development of systemwide solutions for the highest-priority pathways, which can then scale across the NHS via peer-to-peer sharing.
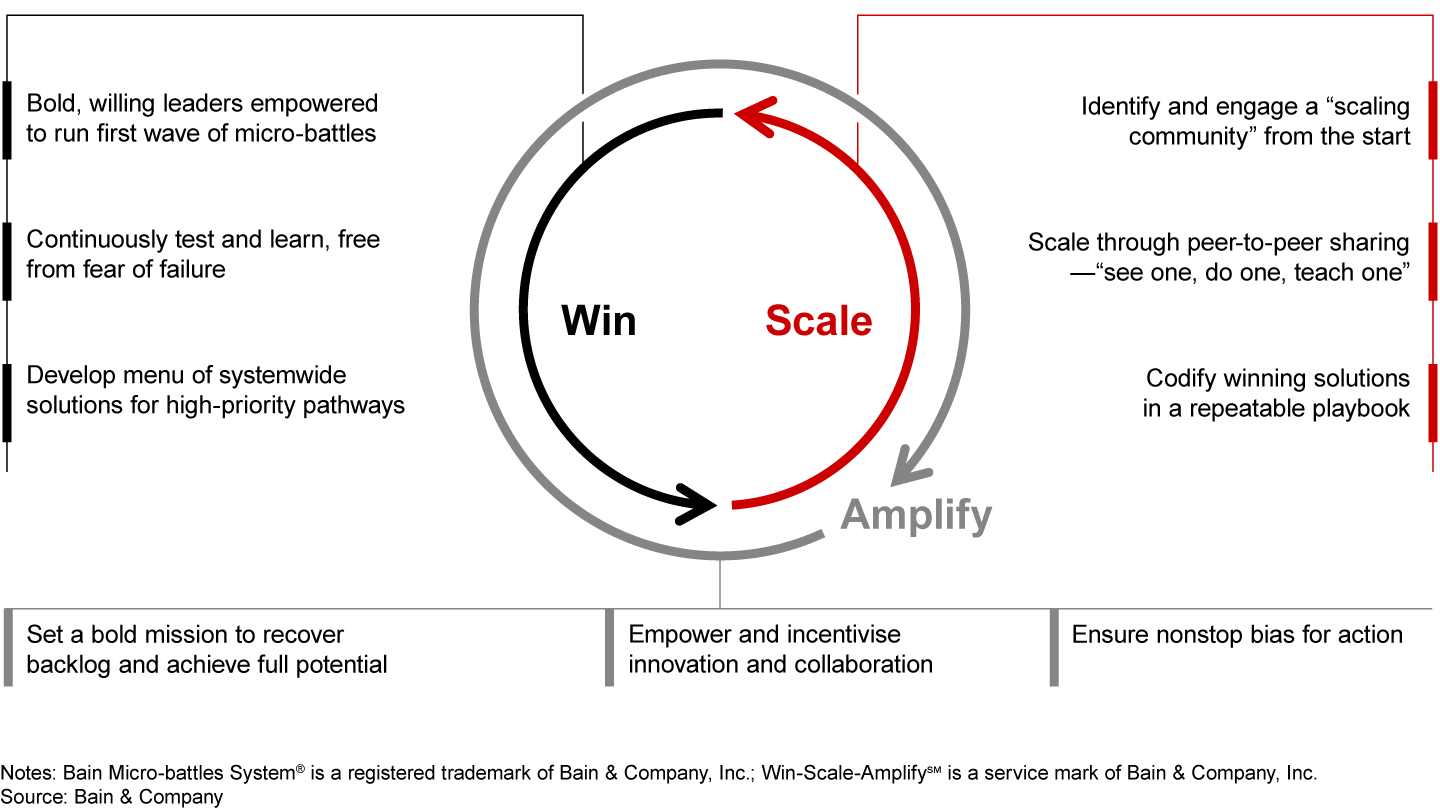

The Bain Micro-battles System® follows a Win-Scale-Amplify model. For the NHS, this model would look like the following:
- Win. Ambitious systems with engaged, bold leaders lead an initial wave, empowering frontline clinicians and management within care providers (including primary care) to develop their own solutions for how to defeat the backlog.
- Scale. If appropriate, these solutions are then scaled within the system and nationally, with the help of a repeatable, tailored playbook (when appropriate) and a scaling community.
- Amplify. NHS England and NHS Improvement (NHSE/I) and other parts of the government are responsible for amplifying the speed and impact of solutions by helping to unblock constraints, effectively allocate resources, and regularly communicate progress nationally.
“Beware the two rules for pilots. First, they always work because you over-resource them. Then they never scale because early lessons are not translated into a repeatable model.” —James Allen, Bain partner, creator of the micro-battle approach
How to win: The role of bold provider collaboratives
NHS systems have a key role in rapidly identifying winning solutions that can accelerate recovery. The boldest and most willing will lead this mission.
A first wave of systems with the potential to excel must have the operational freedom and financial incentives to shrink the problem. Following the micro-battle approach, each system will first translate the mission to eliminate the waiting list into the constraining themes (e.g., shrink the orthopaedic waiting list), then break each theme into specific issues and actions within each provider organisation and specialty (e.g., increase orthopaedic theatre throughput). Within this first wave, agility, speed, and a test-and-learn mindset are crucial.
Freedom to solve by providers, for providers
Even the most willing and capable providers will require critical freedoms, incentives, and support from the NHSE/I to win faster and better:
- Operational freedom …
- To create a cohesive plan and choose their own priority pathways: “act now” micro-battles for areas with the greatest potential for harm (e.g., cancer services) or the longest waiting lists (e.g., orthopaedics, ophthalmology) and “plan now” micro-battles to develop longer lead times and improvements (see Figure 4)
- From time-consuming reporting and top-down initiatives
- To work across the system by using collaborative governance and operating processes, many of which were developed during the pandemic


- Financial incentives, including …
- Payment for measurable results that matter to the patient and taxpayer and enable providers to compensate and reward staff for their efforts
- Freedom to utilise existing capital budgets
- Transparent access to additional funds set aside for recovery
- Incentives that do not penalise the whole collaborative for any one organisation’s poor performance
- Other support, including …
- Allocated resources from the relevant GIRFT clinical teams and specialty leads
- Advice and input from other NHS national capabilities, when requested
- Programme support for expert capabilities to help mobilise an agile and high-tempo operating model and to design and build underpinning data flows and real-time management information
Pathway transformation, be it in the best way to care for and inform patients as they wait or in how to offer clinically suitable alternatives and diversions for specialist medical and surgical treatments, must also become an essential part of primary care. Equally, solutions can and should address ongoing care and rehabilitation where appropriate.
“We need the freedom to test and learn—and, really importantly, the freedom to fail. We must be able to come up with solutions as a collaborative that looks at things in the round.”—CEO of an NHS provider
In all of this, early engagement of independent-sector providers can generate additional capacity in the short term, provide valuable perspectives in the test-and-learn process, and establish important relationships for many collaboratives.
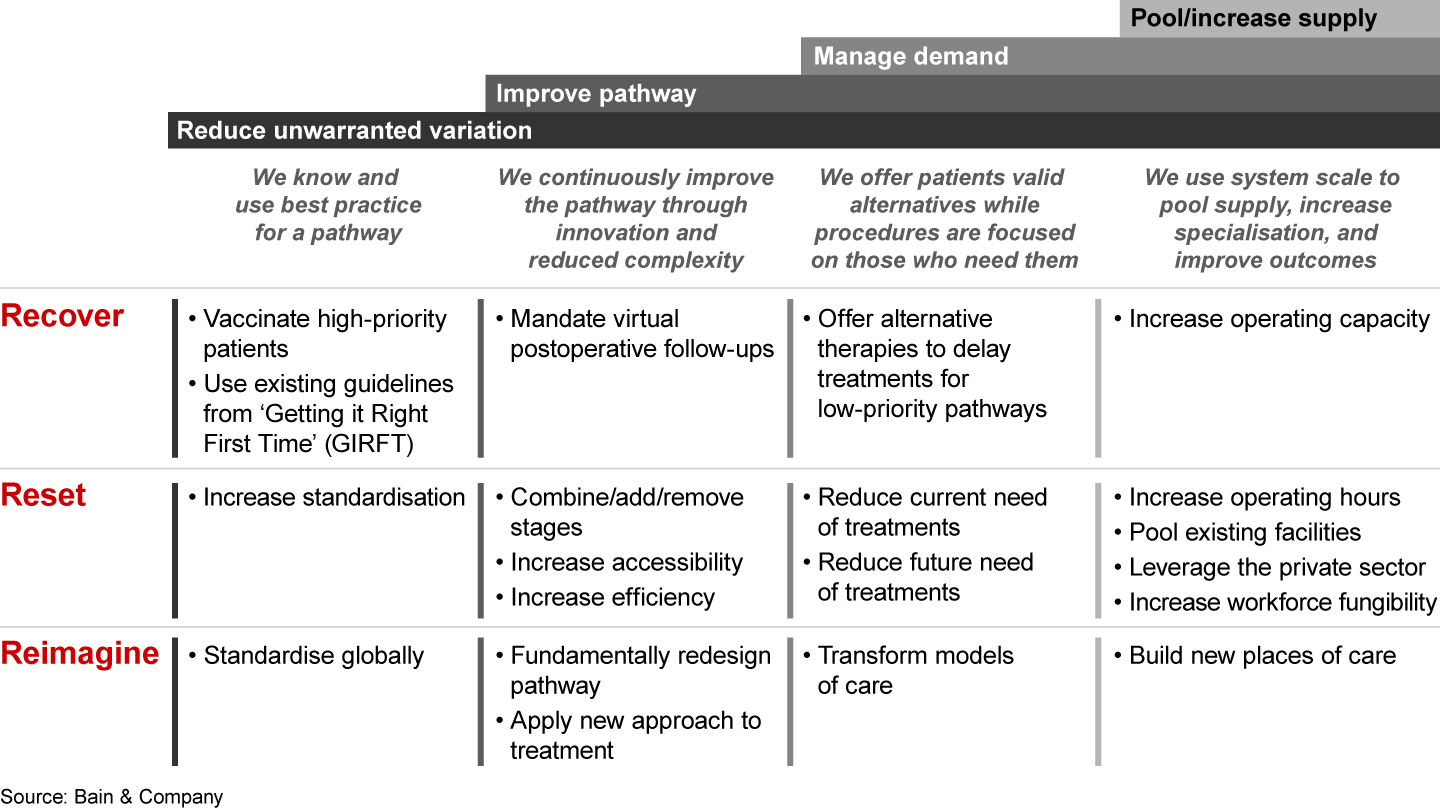
Most importantly, these providers can immediately increase activity, reduce the backlog, and improve the patient experience by increasing standardisation, improving and transforming pathways, reducing demand, and pooling or increasing supply (see Figure 5). In addition, they will provide the NHSE/I with investment business cases, trajectories for full recovery by mid-2024, a motivated and retained workforce, and evidence and input for how to scale to other systems.

Great systems are already on the journey
Providers are already tackling their own backlogs, and excellent examples of solutions are emerging:
- A specialist children’s hospital is proactively contacting elective patients and using a simple survey to identify red-flag patients and those who are happy to delay treatment.
- An acute provider in the north of England is reducing the total waiting list by differentially focusing resources towards increasing procedure volume (about 20% over baselines) for those with a diagnosis and reducing focus on outpatient review and follow-up (about 25% below baselines).
- Providers across one London integrated care system are collaborating with GIRFT to standardise about 30 low-complexity, high-volume pathways (e.g., increasing use of remote and one-stop clinics).
However, providers lack a clear, common target as well as a standard mechanism for rapidly scaling these isolated successes nationwide.
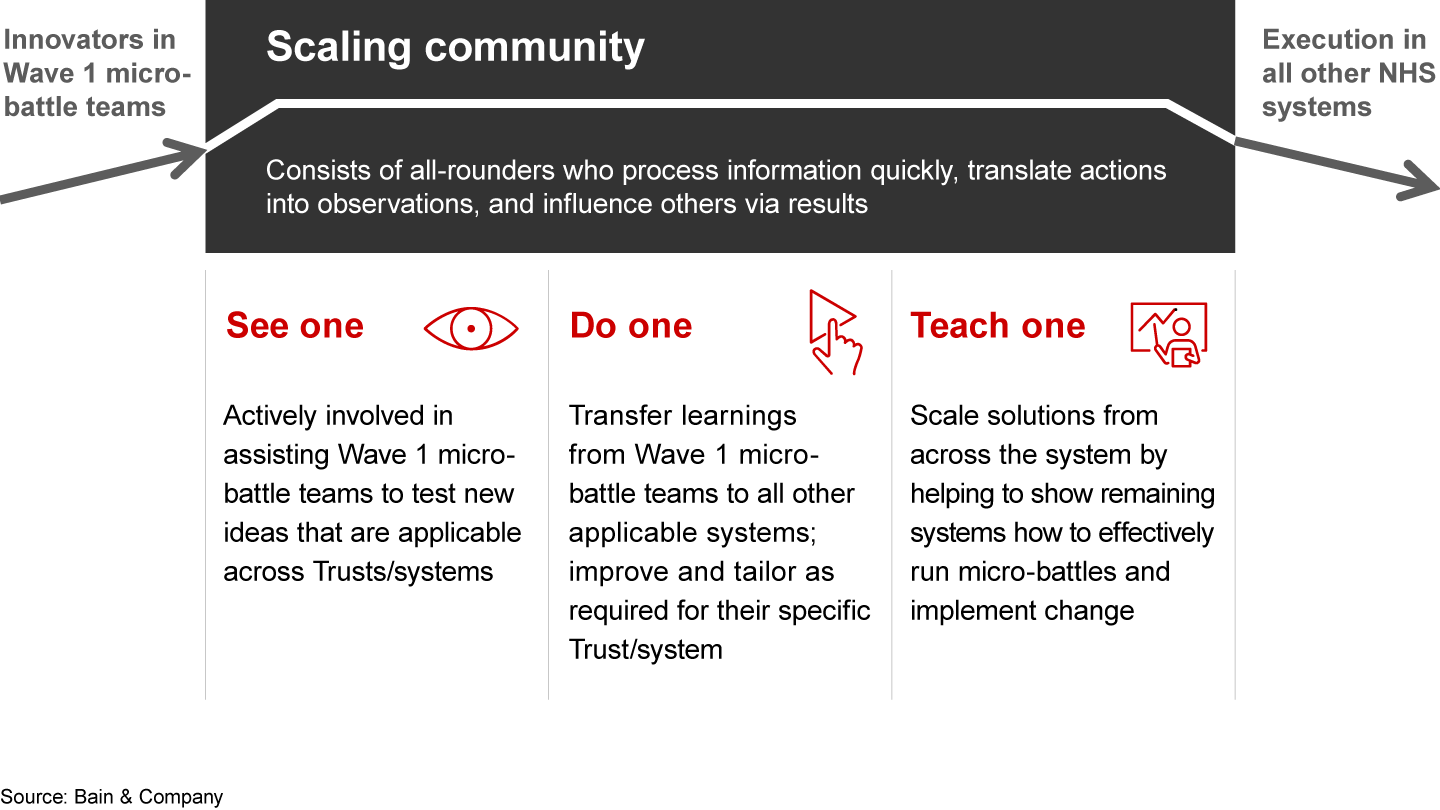
How to scale: See one, do one, teach one
Scaling of winning ideas in parallel with the first wave of system transformations will be crucial to resolving the elective backlog. We suggest a “see one, do one, teach one” approach, in which ideas spread through a scaling community: engaged and inspired individuals who take successes back to their home provider or system (see Figure 6). To encourage this viral scaling, we encourage a three-step process:
- Identify scalers. These influential all-rounders focus on results, inspire others, and act as bridges between providers.
- Engage early. Involve these scalers from day one in wave one—creating solutions, learning what works, and taking their experience home to start a new micro-battle.
- Teach the next wave. Support scalers as they figure out the best option for how to repeat, tailor, or recreate specific solutions.

Amplify: The role of NHSE/I in supporting systems
With a wave of systems and innovation underway, NHSE/I and other national agencies can, in parallel, help to deliver rapid results at scale. To do this they can:
- Communicate. Continuously and publicly communicate progress towards the bold mission. This is a multiyear journey that will require sustained effort and attention to achieve success in 2024.
- Coordinate. Develop and run the rollout plan across all systems.
- Track. Set up a central dashboard or platform that feeds on timely and actionable data to track system-level progress and facilitate intervention when required.
- Train. Build an underlying leadership development programme to inspire the next generation of leaders, develop critical innovation skills, and conduct targeted rotations and peer-group sharing to maximise the dissemination of great ideas.
Everyone has a role in reimagined care
Whether you are a system leader or frontline worker, in the heart of NHSE/I or partnering with the NHS through the independent sector, you have a role in achieving the bold mission to reimagine the approach to elective care.
Now is the time to trust and empower the frontline to improve patient services. Now is the time to encourage peer-to-peer collaboration and the scaling of winning solutions. The sooner the first wave gets to work, the better—just don’t forget to invite the second wave along to be inspired.
The authors wish to thank Freddie Quiney, orthopaedic trainee and Bain senior associate consultant, for his support and for the benefit of his clinical experience, and Mythili Sutharson for her analytic modelling support.
Win-Scale-AmplifySM is a service mark of Bain & Company, Inc.
Bain Micro-battles System® is a registered trademark of Bain & Company, Inc.