Brief
Executive summary
Today, healthcare in India is at a crossroads. As a nation, we have made noteworthy progress across several dimensions, and India is healthier today than ever. We have successfully eradicated multiple diseases, including smallpox, polio and guinea worm disease. HIV infections and AIDS-related deaths have dropped significantly. India has emerged as a hub for generic-drug manufacturing and boasts a large public-health infrastructure.
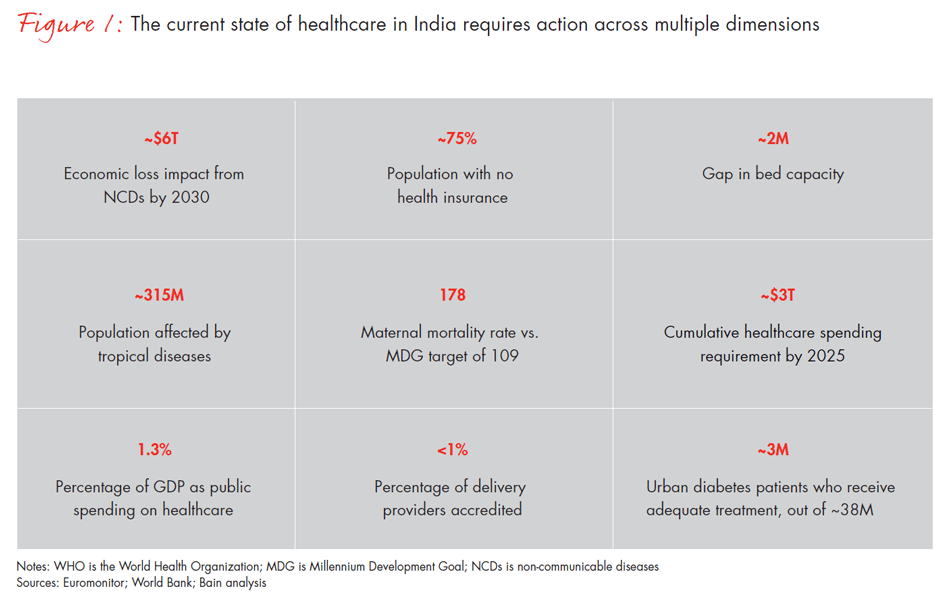
Despite evolution on multiple fronts, however, India still struggles with substantial issues and gaps in its healthcare system (see Figure 1). Healthcare is under-served and under-consumed. Insurance covers less than a quarter of the population, and out-of-pocket spending is considerably high. India faces a severe shortage of both hard infrastructure and talent, with regional imbalances and variations in healthcare delivery. The strong bias towards curative care reflects a culture in which prevention and wellness receive only limited focus and investments in primary care and public health have long been inadequate. Quality of care is questionable, hindered by limited accreditation and adoption of basic technologies.
Megatrends observed for India will combine with these underlying issues and gaps to make India’s health system further unsustainable:
- Increasing urbanisation has led to an explosion of non-communicable diseases (NCDs), and India now carries a dual burden of communicable diseases (CDs) and NCDs.
- India’s population is evolving and ageing, with the geriatric age group expected to constitute 11% share by 2025.
- Sustained cost pressures are limiting affordability in the largely uninsured environment, even as a rising mass market is demanding greater access to quality care.
- Particularly disturbing is the allocation of public healthcare spending, which is among the lowest in the world and has stagnated in the last few decades.
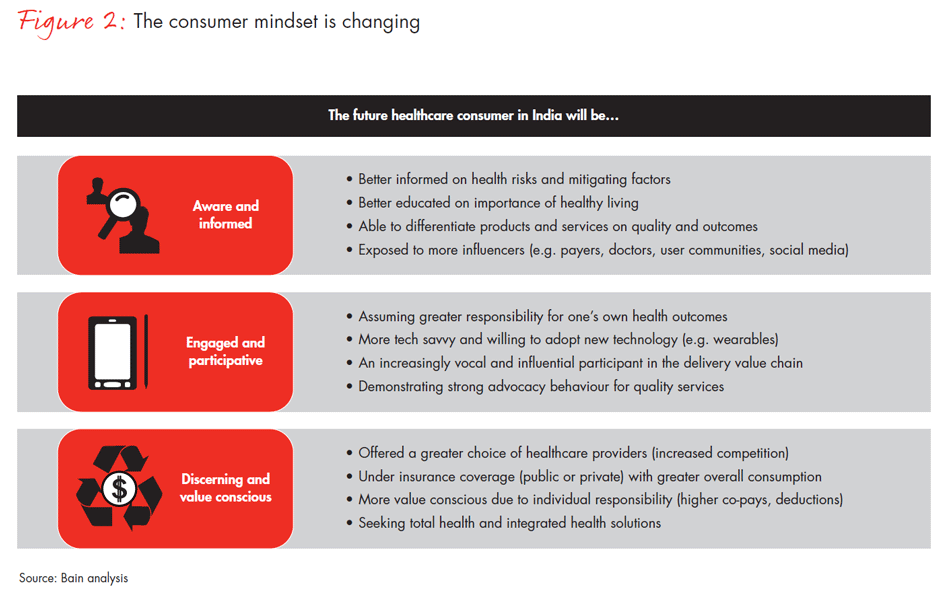
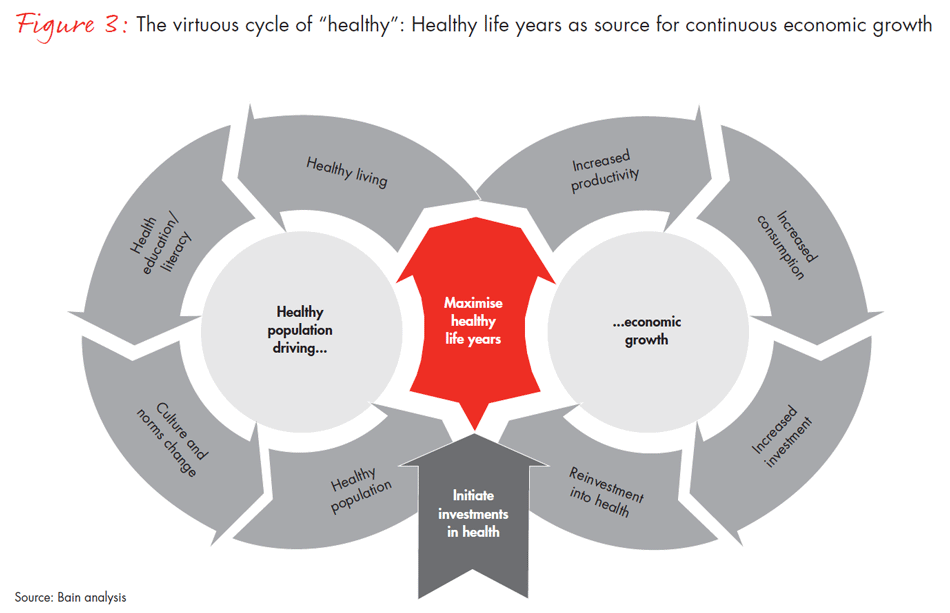
Now is an opportune time to define India’s health system in order to power India’s growth and development. Healthcare consumption is expected to increase progressively in the future, in line with economic growth. The emergence of disruptive technologies is likely to aid care delivery and lead to consumers who are more informed, engaged, discerning and value conscious (see Figure 2). Significant growth and refinement of health infrastructure are anticipated: Investments by financial investors (PE/VCs) in healthcare have surged recently, the government has announced a sharp focus on transforming India’s health system and an emerging paradigm emphasises access to quality healthcare as a basic human right. Investment in healthcare will create a virtuous cycle of productivity, employment and consumption, resulting in overall economic growth (see Figure 3).
Today, all stakeholders have an exciting opportunity to transform India’s health system in several ways:
- Creating a healthy India to power the country’s development and growth and minimising disability-adjusted life years (DALYs) lost to preventable sickness.
- Seizing the potential for significant job creation from healthcare services (15 million to 20 million additional jobs by 2025).
- Helping India move beyond the manufacture of generic drugs to emerge as an innovation hub in lower-cost health products and services and decrease dependence on costly imports.
- Providing health insurance to the masses, with a commensurate decline in out-of-pocket spending, thereby preventing people from falling into poverty due to healthcare spending.
- Reducing the urban-rural divide in the supply and consumption of healthcare.
- Adopting greater use of technology to create scalable and more sustainable made-for-India solutions and to increase health awareness and engagement.
- Turning India into an exporter of new paradigms in affordable quality care among emerging economies.
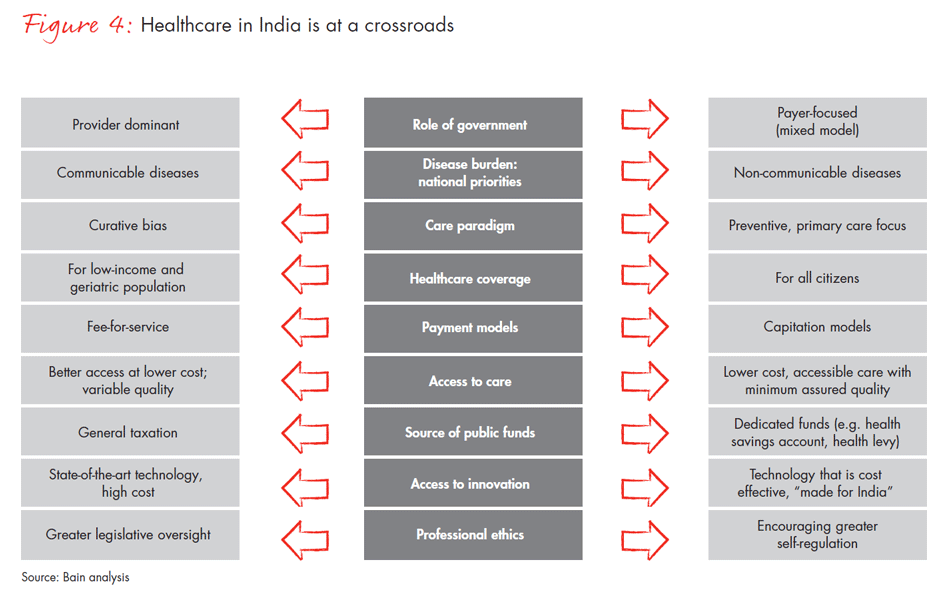
India must choose its evolutionary trajectory wisely. Clear choices must be made regarding the role that government will play and how it will prioritise and fund healthcare. We need to reshape the paradigm of care in India and create a culture of health and wellness. To undertake this journey, we will need to redefine the health system and clearly lay out the preferred path on three key dimensions of health delivery: Access, Cost and Quality. Making the right choices in areas such as role of government, regulations on essential healthcare goods and services, innovation in payment models, use of technology and sources of funding will be critical in defining the future trajectory of Indian healthcare (see Figure 4).
India has a narrow window of opportunity in which it must act quickly. If we can succeed in capitalising on the immense opportunity, we can aspire to achieve a massive shift in healthcare within a decade (see Figure 5).

We can aim for equitable access to affordable healthcare, along with minimum quality standards for highly aware and engaged consumers, by 2025. This sustainable healthcare ecosystem would be centred on a wellness-oriented culture focussing on prevention and early diagnosis.
Key recommendations
Several steps are necessary to ensure that the transformation of India’s health system is a success, and multiple stakeholders need to collaborate to develop a holistic and sustainable healthcare system, with central and state governments playing pivotal roles.
Immediate priorities
- Ensure that the government assigns national priority to the healthcare agenda, commits to spending more on public health and defines a holistic framework for an India-centric health system. The government must also set clear health priorities, clarify roles and establish enabling incentives and regulations for stakeholders.
- Enable a paradigm shift to healthy living, with a focus on prevention and primary care through greater public spending on prevention, individual incentives for healthy living and broader engagement of multiple stakeholders (for example, technology and food and beverage companies, media, schools and others).
- Scale up and expand current programmes to control NCDs—such as mental illness, diabetes, cardiovascular disease and cancer—with care offerings that integrate screening, prevention, treatment and follow-up, enabled by partnerships—both private-private and public-private, and across the delivery, insurance, technology and pharmaceutical sectors of the healthcare industry.
- Drive insurance adoption and reduce out-of-pocket expenses by rolling out a universal healthcare-coverage scheme for essential care. Provide government support for disadvantaged populations, such as the elderly and low-income deciles.
- Institutionalise standards for the minimum quality of delivery across products and services, and initiate tracking of outcomes. Use health-technology-assessment (HTA) tools to determine access to innovation.
- Use technology and IT in healthcare to overcome access barriers in remote areas and engage patients. Focus investments on India-specific solutions.
- Expand the supply of healthcare talent in critical roles, rejuvenate AYUSH (ayurveda, yoga and naturopathy, unani, siddha and homeopathy) and encourage private investment in education. Improve the talent quality using a clear roadmap for governance and continuing medical education (CME) for professionals.
- Give an impetus to local manufacturing. Transform India into an export hub for medical products and equipment and into an R&D hub for tropical diseases.
Short-term priorities
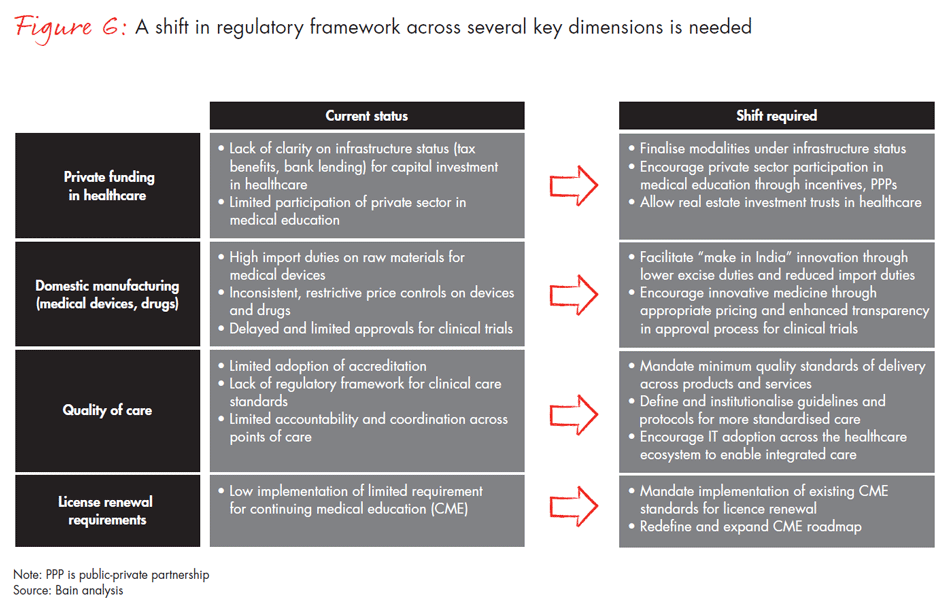
- Create enabling regulations to foster private enterprise in healthcare, at sustainable returns (see Figure 6).
- Inculcate a culture of personal responsibility for health through education, awareness, schooling, public mandates and incentives—for example, through health savings accounts and co-payments.
- Encourage the build-out of healthcare infrastructure beyond the metropolitan areas and in under-served areas.
- Focus on preventive capabilities and public health measures to meet post-2015 Millennium Development Goals (or Sustainable Development Goals) for maternal and child health outcomes, with a special focus on reducing the dual burden of CDs and NCDs.
Medium-term priorities
- Build capacity in both the health system and the community to provide long-term care, especially for the indigent and elderly, and mental healthcare to those who need it.
- Encourage innovation in care models. Shift from hospital-centred delivery and procedure-centred, fee-for-service models towards low-cost delivery, capitation-based payments and population health models.
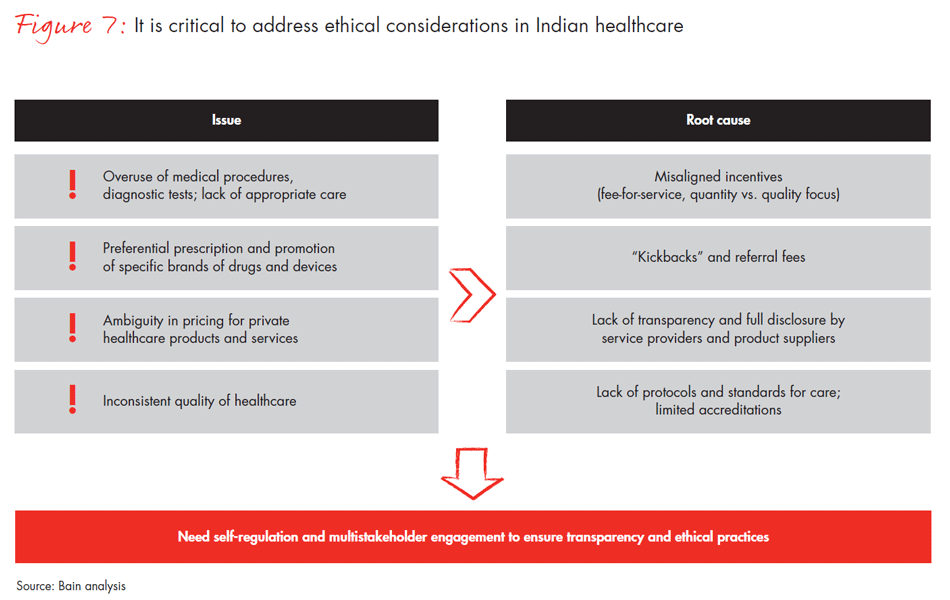
- Encourage greater self-regulation and ethical behaviour among medical professionals, enabled through oversight from professional councils (see Figure 7).
What we ask of the government
The central government has shown encouraging signs that it intends to make healthcare a national priority and to take transformational steps in this sector. We ask the government to take the lead in bringing about key changes to enable the shift in India’s healthcare system over the next decade:
- Increase public spending on healthcare from 1.3% in 2012 to 3% of GDP by 2025.
- Apportion a greater share of public spending on prevention, including mass screenings, and on primary care coverage.
- Pilot and scale up universal-coverage models to guarantee essential care.
- Drive policy consensus among the central and state governments to ensure that high priority is given to health and uniformity in health regulations.
- Define a vision and roadmap for NCDs and healthy living, roll out high-impact public-health interventions and ensure multistakeholder engagement.
- Mandate that delivery and diagnostic providers and device manufacturers meet minimum quality standards.
- Invest in an IT backbone and interoperability standards in healthcare, and provide incentives for adoption.
- Build competency in HTAs, and implement them to manage access to innovation in publicly funded products and services.
- Create an enabling ecosystem that provides incentives for private investment in delivery infrastructure, medical education, R&D and domestic manufacturing.
- Establish systems to rationally determine the pricing of publicly funded products and services; for example, procedures through Rashtriya Swasthya Bima Yojana (RSBY), India’s national health programme.
- Adopt a mission approach for India-focussed drug R&D, for example, for tropical diseases, and for public health initiatives such as vaccination coverage.
Commitment from NATHEALTH members
We recognise that there is a significant deficit of trust between the private and public sectors in healthcare today. Private players in the healthcare industry have a significant role to play in bridging that gap and enabling a healthier future. Members of NATHEALTH should aspire to the following:
- Invest in expanding the supply of affordable care, especially beyond metropolitan cities and in rural areas, with the right incentives.
- Continue innovation with new delivery models, including in government partnerships, to improve quality of care.
- Invest in frugal innovation in drugs and device manufacturing to transform India into an Asian hub for high-value products.
- Harness technology to expand the reach of existing services such as telemedicine.
- Prioritise investments in the right technology tools, such as electronic health records (EHRs), to enhance care quality and coordination.
- Encourage the adoption of minimum quality standards to improve delivery.
- Invest in enhancing the skills and capabilities of doctors, nurses and allied health personnel through training, career progression and CME.
- Engage with the government on health policy, and share expertise on, for example, procedure costs, pricing and new technology assessments.
- Commit to adopting and promoting ethical behaviours and norms.
- Focus on education and general awareness of healthy living and prevention; invest in worksite wellness programmes for employees.
- Invest a proportion of profits in corporate social responsibility activities, and support social enterprises and causes for a better India.
Must-haves in the health system to achieve the aspirations
As India’s health system transitions towards the aspirational state, multiple underlying factors must be in place:
- Availability of public funds, across the central and state governments, with a greater share of Capex than exists now.
- Adequate investments in the private sector, especially incentives to invest in local manufacturing and healthcare delivery in under-served areas.
- Rational pricing for publicly funded services, ensuring fair returns for private providers.
- Supply-side infrastructure readiness to meet anticipated growth in demand, especially following universal coverage.
- Availability of trained talent across geography tiers and among doctors, nurses and allied health professionals.
- High levels of health awareness and individual ownership of health outcomes.
- Health IT and data serving as the backbone for effective implementation of initiatives, tracking outcomes and providing disease surveillance.
- Improved cooperation between the central and state governments for consistent implementation of public initiatives.
A few signposts need to be monitored periodically to measure success and judge whether the transformation of India’s healthcare system is on course (see Figure 8).