Brief
If there is one constant in the current healthcare environment, it is the unrelenting pressure to grow and change. Some growth has come from “bolting on” physician groups or insurance units to an existing delivery system, but creating truly integrated delivery networks requires more than that. It requires a shared vision and accountability among administrators, clinicians and frontline employees, something that is not commonplace in most health systems today. Simply declaring that your strategy will deliver integrated and value-based care is not sufficient. You will need to create a blueprint that mobilizes your organization to change behavior and culture in an unprecedented way. An aligned operating model serves as this blueprint (see Figure 1).
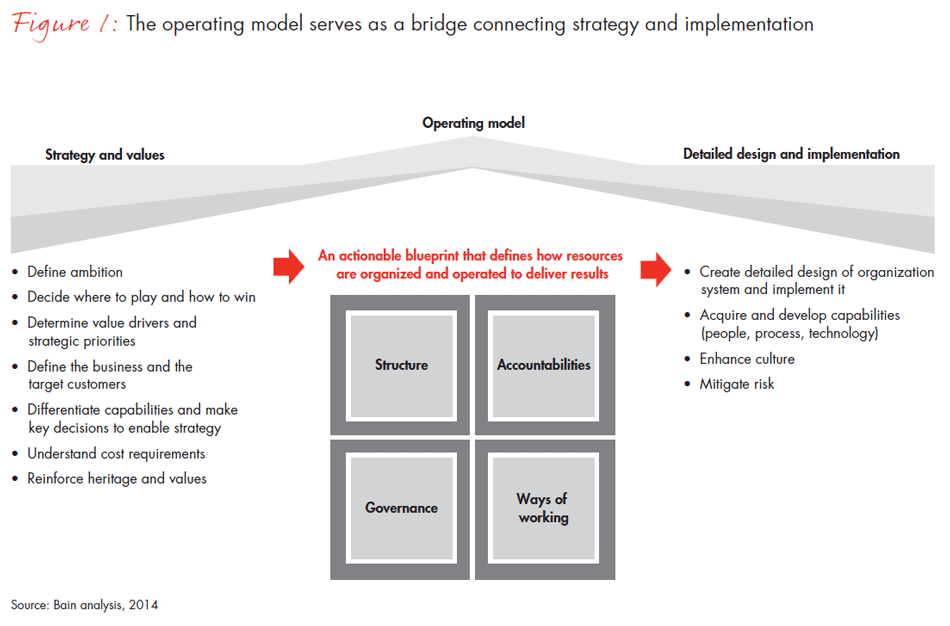
Why is an aligned operating model so important?
In the past, provider systems could coast along with a suboptimal operating model; today, there is less room for error. In the face of increased complexity, demanding patients and payers, and large amounts of data flowing into and around healthcare organizations, for systems aspiring to be truly integrated, the need for a detailed blueprint to guide decisions has become an issue of some urgency. The operating model outlines how resources should be organized and deployed so critical work gets done. It describes the organization’s shape and size, shows where to draw boundaries for each part of the enterprise and clarifies how people should work together within and across these boundaries. It also demonstrates how the center adds value and identifies which behaviors should be encouraged.
Provider systems like Ascension (a health ministry that is the nation’s largest Catholic and nonprofit healthcare system, providing care in 1,900 locations in 23 states and the District of Columbia) have been confronting these very challenges. With a solid strategy rooted in a compelling mission and vision, Ascension’s leaders realized they needed a more aligned operating model to build a bridge between their strategy and the results they desired. This model would help Ascension define how it could best accomplish its mission of serving the poor and the vulnerable with person-centered and high-quality care.
What are the key challenges to getting this right?
If all this were easy, it would be done right every time. In our work with a variety of healthcare provider organizations, we have found there are five keys to success for designing an effective operating model: Ensure that the strategic requirements are defined at a granular level; get the important voices to the table; establish robust design principles; go deep enough to identify and address the most critical processes and decision roles; and use a comprehensive set of Results Delivery® tools to create the best odds of implementation success.
1. Ensure that the strategic requirements for success are defined at a sufficiently granular level.
As an organization defines its mission, vision and overall strategy, it is important to ensure that the strategy is specific enough to design a blueprint. Answering these questions can help:
- Are you clear on your objectives in the marketplace, and can you concretely describe the ways your organization will achieve them? How will you measure physician alignment, network development and person-centered care?
- Which parts of your system are particularly well positioned, and how do you build on your strengths? Which communities, service lines and care models are set up for future success and growth?
- In which new or existing capabilities must you differentially invest to be successful? Where must you be best in class, and where can you afford to be good enough?
- What are your organizational challenges, and how can they be mitigated? How does your organizational structure or culture help or hinder the achievement of results?
Translating answers to these questions into the design and implementation of critical processes and decisions is the next step.
A leading academic medical center on the East Coast invested significant time and energy transforming its operating model. To better support its mission and strategy to become a leader in population health management while remaining a premier episodic care and referral organization, the leadership team identified the system’s core strengths—its brand, reputation and clinical excellence—and also determined the need to further improve the center’s care coordination capabilities and primary care affiliation models. By developing some innovative incentive arrangements, the team built a much stronger community physician partnership program across targeted geographic areas. And many of the center’s world-renowned clinicians collaborated to redesign care delivery models, improving outcomes for target populations.
2. Get all the important voices to the table.
At the very beginning of the change effort, it is critical to identify the many stakeholders who should be well represented. When designing a new operating model not only do you need a mix of leaders from both the corporate and regional offices, but it is particularly important to have clinical leaders, including physicians and nurses, prominently involved from the beginning and in leadership roles all along the way. Ascension had its clinicians on the initial design team, as well as on each of the teams that took the original blueprint and tailored it for specific markets. Beyond these formal teams, Ascension’s leaders took the time to solicit feedback from a broader segment of the clinical leadership community. They organized a Clinical Council, whose members provided periodic updates and participated in brainstorming sessions. This was critical to the success of the change effort.
3. Establish robust design principles to guide the construction and selection of different options.
Principles liberate people to do the right things, as long as they have a framework in which they can make the right choices. Well-constructed design principles take into account strategic intent and the organization’s strengths. They also provide the rubric for evaluating alternatives for critical parts of the operating model. Start by considering your strategic requirements: What care model will be most effective? How can you be competitive in your chosen markets? Which populations should you target? And what critical capabilities do you need to deliver the highest-value care? Having clear principles will help you identify your organization’s strengths and weaknesses. Clear principles will reinforce the heritage and values that carried you to where you are today and help you to consider the legal, labor or policy constraints that might prevent you from achieving your goals.
A regional health delivery system that focused on developing a more integrated statewide network of care identified four main design principles, with detailed imperatives supporting each one:
- Build a culture of growth, supported by aligned incentives;
- Design health delivery networks to meet local need and grow share;
- Standardize evidence-based care delivery and operational processes; and
- Develop clinical leadership and organizational talent.
Developing detailed design principles helped all stakeholders understand which options would result in the best outcomes for the organization.
4. Go deep enough to identify and address the most critical processes and decision roles.
Large provider systems that are pursuing value-based care need to invest in developing core capabilities for the new model, including:
- Network development and management: building the right network of services, physicians and facilities to serve members; managing and coordinating activities and standard processes across the network;
- Person-centered care: managing how the organization delivers care that will improve clinical and financial outcomes while providing patients with information and personalized care that enhances their experience;
- Financial and risk management: creating, implementing and managing risk-based contracts among providers, which result in aligned incentives and equitable sharing of risk and reward; and
- IT infrastructure: developing technology that collects and manages data to improve patient care and health outcomes while improving the provider experience.
Many of the most successful integrated care delivery systems—such as Intermountain Healthcare, Geisinger Health System and Banner Health—have prioritized investment in these capabilities. To help managers own critical decisions and be accountable for them, these systems have also focused on applying the right metrics and achieving performance transparency.
5. Use a comprehensive set of Results Delivery tools to create the best odds of implementation success.
Although there are risks to any change process, a complete failure—which occurs in fewer than 10% of cases—is not as likely as a dilution of results, that is, not achieving full performance from your strategy. To increase the chance of successful implementation, an organization needs to look at its risk history, evaluate how major change efforts have worked in the past and try to assess where the greatest risk will come from in the future. It should also devise ways to engage and support the stakeholders whom the proposed changes will impact most (see Figure 2).
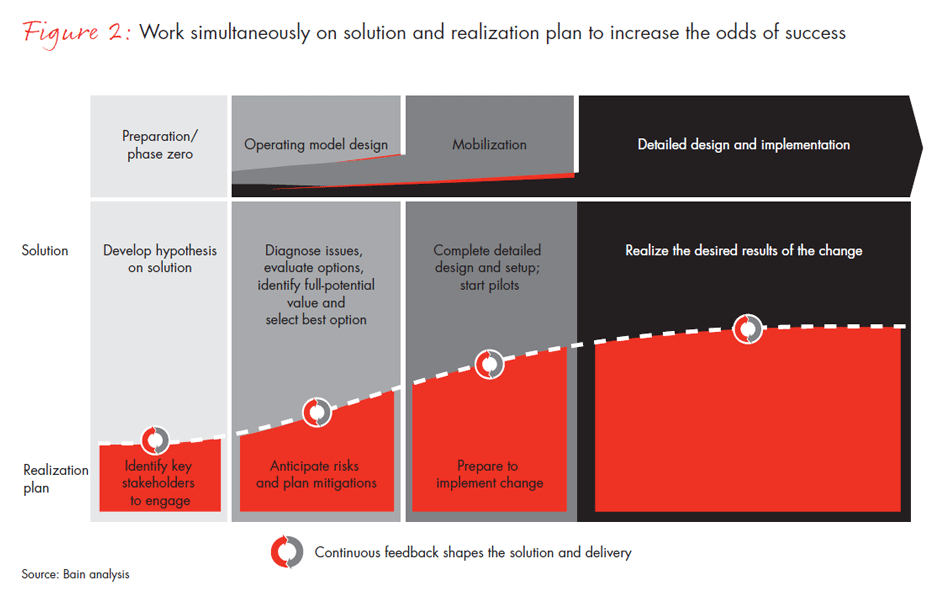
At Ascension, senior leaders identified three ways to reduce risk and enhance performance as they finalized the operating model: Capture the hearts and minds of associates by communicating a compelling reason for how these changes will better equip Ascension to fulfill its mission; invest in engaging committed sponsors to help change cascade down the organization and enroll other leaders in the effort; and get the detailed design right for each market and each function to ensure goals are met.
Establishing a strong sponsorship spine at all levels of the organization will help ensure that everyone understands the goal of the change program. A big part of establishing that spine at Ascension was selecting influential leaders who strongly reinforced their “Virtuous Servant Leadership” behaviors, which identify how people can work collaboratively across functions. Many of these leaders also participated in the ongoing organizational design efforts across the local health ministries.
In a world of constant change, leaders can take these key steps to succeed:
- Formulate your mission and strategy before you develop your operating model.
- Don’t start with boxes and lines on an organization chart. Think instead about accountabilities for critical decisions and how you will implement core processes in the new model.
- Be clear about what works well and include it in the new model.
- Invest to get real clinical engagement as well as management engagement. All players must understand why you are adjusting the operating model and what it means in practice, compared with the current model.
- From the very start, ensure the design effort is collaborative and focuses on managing change and communicating well.
- Don’t underestimate the time required to do this right. The journey is as important as the destination.
Julie Coffman, Sarah Elk and Tamara Olsen are partners in Bain & Company’s Healthcare practice. Julie and Sarah are based in Chicago, and Tamara is based in Boston.

