Brief

As healthcare costs continue to escalate, healthcare providers in Europe are under intense pressure to improve efficiencies without compromising patient outcomes. Retail health consolidation could help alleviate some of these challenges.
Retail health consists of outpatient healthcare in freestanding, commercially owned and often branded clinic chains. Typically, retail health chains have dedicated teams for administrative tasks, allowing physicians and nurses to focus on patient care. Common retail health clinics in Europe include dental clinics, ophthalmology and radiology clinics, and veterinary practice chains. As in the US, many European retail health clinics rely on patient self-payment for much of their revenue.
Consolidation of retail health has been uneven across Europe. This could change as the advantages inherent in the model—such as improved quality of care for less cost—are realised across the value chain. Reaping the benefits, however, requires the ability to navigate Europe’s highly fragmented regulatory landscape and a savvy understanding of retail health models.
Unlocking value through efficiency
Healthcare systems around the world suffer from inefficiencies, and Europe’s healthcare systems are no exception. The rise of retail health is rooted in the desire to manage costs better, increase productivity and improve the quality of patient care. The fundamental appeal of consolidation is the ability to unlock value through efficiency, which benefits patients, physicians, payers and investors alike.
The trend toward retail health is supported by medical advancements that make it easier to shift services out of hospitals and into outpatient settings. This can offer greater convenience to patients, and payers are naturally keen to transfer patients to lower-cost outpatient environments.
Retail health chains are also more responsive to physicians’ changing attitudes about ownership. They offer a more stable and flexible alternative to the risks of running a practice. And for physicians who are preparing for retirement and looking for a solid exit for their practice, retail health chains are welcome buyers.
For investors, consolidation offers opportunities for value creation at the top and bottom line, and significant expansion of multiples. Revenues can be boosted by increased utilisation, category management, higher patient volumes, pricing sophistication, network optimisation, and improved branding and marketing. At the bottom line, there are scale-driven economies in such areas as purchasing and supply chain management, real estate management and the centralisation of administration.
The number of outlets is key to capturing better economies.
Opportunity within a fragmented landscape
The trends driving consolidation are the same in Europe and the US. Retail health chains are not popping up in European shopping centres or grocery stores as they are in the US, where the number of retail buyout deals increased at a compound annual growth rate of 34% from 2012 to 2017. But both markets are grappling with demands for cost management and consumer choice, and stakeholders in both regions see that consolidation can deliver high-quality, repeatable outcomes for less cost.
In Europe, however, payer, regulator and physician attitude shifts are slower than in the US. In addition, the region is highly fragmented by different national payer systems and regulations. The result is a disparate consolidation landscape in Europe (see Figure 1).
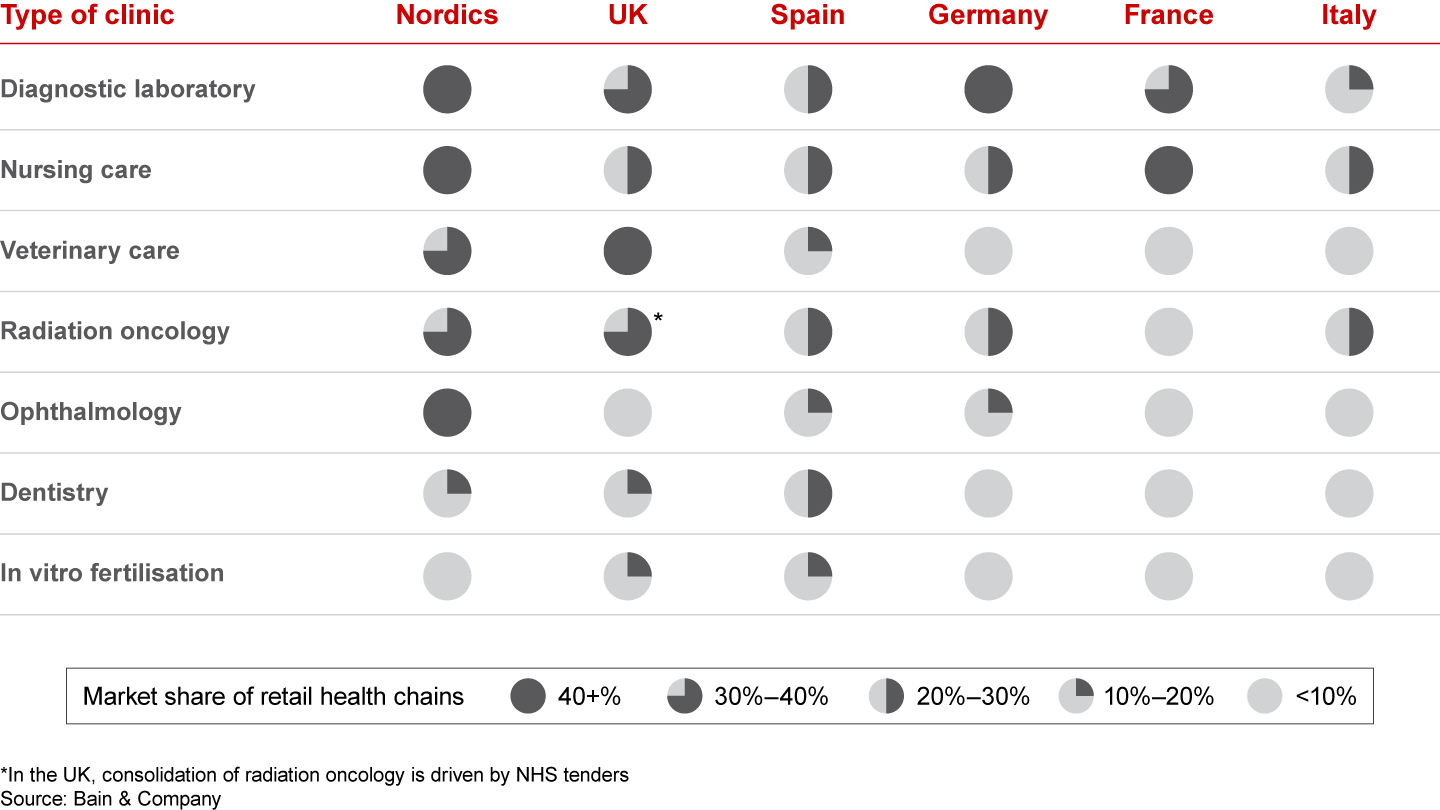

Across Europe, consolidation is most advanced in countries such as the Nordics, where regulators have been more liberal regarding consolidation and ownership models. Where corporate ownership of health clinics is highly regulated, as in France, care provision remains comparably fragmented. Countries that have recently eased regulations, such as Germany, have seen a spike in retail health consolidation.
Roll-ups can happen rather rapidly. Veterinary care in Sweden, for example, had a retail health market share of about 50% in 2013. By 2018, this share had increased to 60% to 65%, representing a 20% to 30% increase within five years. Similar trends have emerged in Norway and Denmark, where the retail health-chain share in 2013 was 20% and 10%, respectively, but increased to 25% to 30% in Norway and about 15% in Denmark by 2018.
Naturally, roll-ups happen faster with some clinic types than with others. Consolidation can accelerate, for example, when linking multiple clinics provides scale benefits. These benefits can occur on the front end, such as improved access to nursing care services or the creation of loyalty schemes in veterinary practices. Back-end benefits allow for sharing back-office functions, such as finance, human resources and other administrative tasks, across multiple practices.
In contrast, the benefits of consolidating purchasing vary by subsector. For example, veterinary practices may derive significant value from consolidated procurement of medicine, and dental practices may be able to invest in expensive equipment when purchasing jointly.
Integrated clinic chains that combine key specialties are beginning to emerge. For instance, Vivanta, a Spanish clinic chain formed through the merger of six legacy brands, offers dental, aesthetic and nutritional services. In Germany, healthcare reforms dating to the early 2000s introduced ambulatory care centres called Medizinische Versorgungszentren (MVZs). MVZs can be single-specialty or multispecialty clinics and can include nonphysicians within their operating structures. The clinics save costs by sharing resources such as equipment, rooms and staff; integrating patient care through the close cooperation of several specialties within short distances; and relieving physicians of administrative tasks.
Multiple avenues for value creation
There are two main routes for value creation in retail health consolidation: clinic improvements and network effects (see Figure 2).
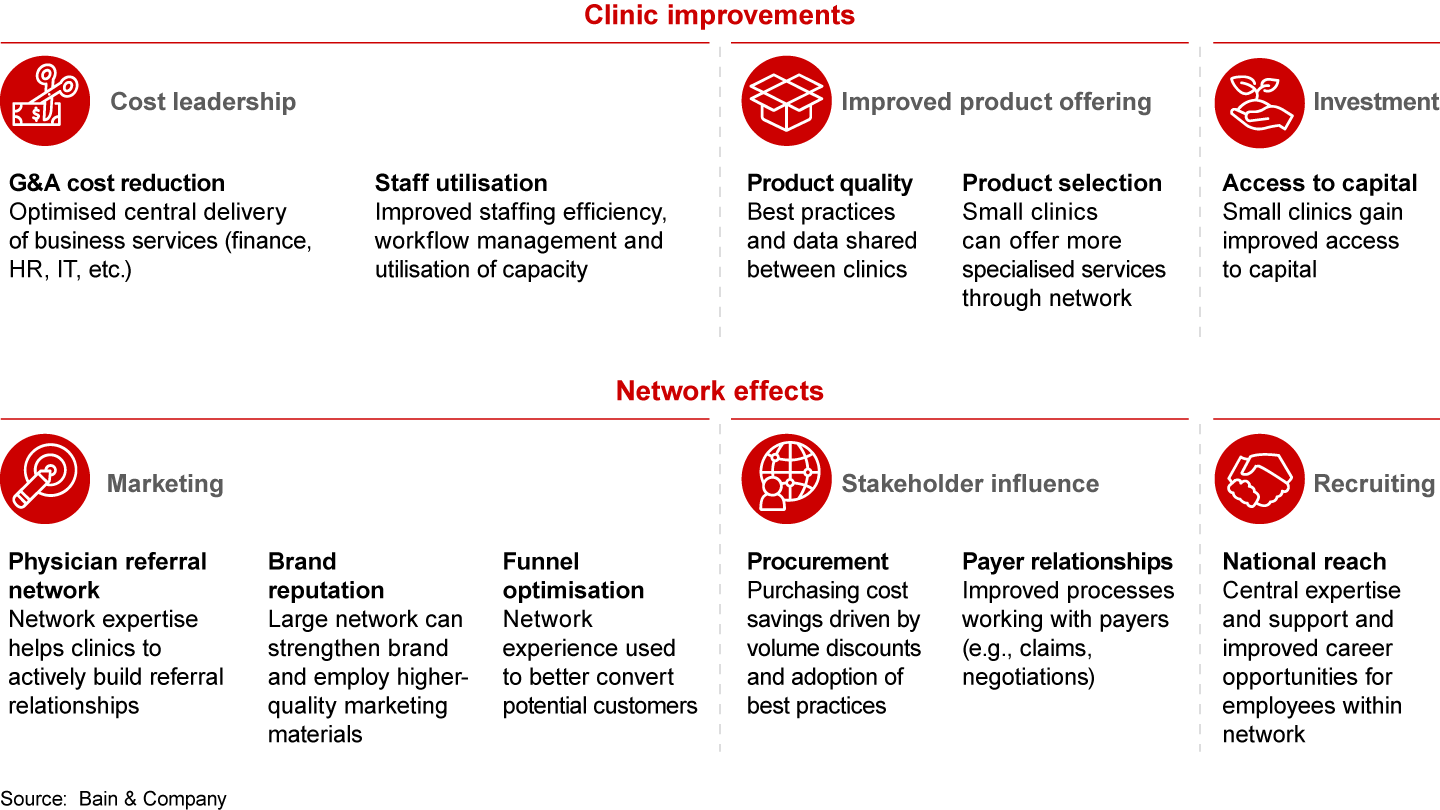

Clinic improvements refer to initiatives to help manage individual clinics, such as price optimisation, utilisation management at the outlet level, cost management and an improved product offering. Digital and IT can be effective areas in which to consolidate services, but they first must reach a minimum scale.
Network effects are the benefits specifically linked to the number of outlets in a chain. They include purchasing on a larger scale, patient referrals between clinics in the same chain, and better access to talent across all clinics within the chain. Network effects can improve marketing, the ability to influence payers and suppliers, and recruiting. Just as with digital and IT improvements, network effects require a minimum scale to be significant.
Examples of successful European roll-ups include AniCura, a veterinary chain that until recently was owned by Nordic Capital, and KKR-backed GenesisCare, an Australian provider of radiation oncology. Part of AniCura’s winning formula was a structured approach to buy clinics one by one, implement clinic improvements and then integrate the clinics into the chain to optimise network effects. Similarly, GenesisCare ensured operational improvements at the clinic level before capturing network effects by closely coordinating cancer care across the network.
This approach needs to be fine-tuned according to the type of clinic and local regulations.
Some incentives, such as utilisation of staff and equipment, offer benefits across clinic chains and geographies. Access to capital can also be a significant advantage. Dental clinic chains, for example, can centralise expensive equipment and investments, such as a digital lab for 3-D printing.
In contrast, the ability to extract value through procurement may vary by country or clinic type. For example, government regulations in Finland limit potential profits from improved medicine procurement by mandating that all patients pay the same price for medicines, regardless of point of sale. In addition, the Finnish government determines acceptable wholesale prices, pharmacy margins and taxes.
Europe’s fragmented regulatory programmes make it difficult, if not impossible, to prescribe a generalised approach to making investments across borders. The most successful strategies adapt to the clinic type and local and countrywide regulations.
Strategic approach is key
In addition to addressing the right initiatives in the right order, investors need to acquire the right clinics at an attractive price and balance rapid roll-up with the ability to make improvements.
The quickest way to scale up is to operate a light decentralised model that does little more than integrate some back-end functions using the “umbrella model” (see Figure 3). Physicians essentially operate as they did before the acquisition, even under their original brand, with little or no input from the owner. The downside is that clinic improvements are more difficult to implement and enforce, and network effects are harder to capture.


Conversely, the most effective way to execute value-creation initiatives is to use a “central model” in which the owner exercises much tighter control on the acquired unit. However, this method has proved to be a tougher sell to clinic owners. As a result, it can take longer to acquire new clinics to add to the existing network.
Whatever the clinic type or model, success depends on physician buy-in. Rather than adopt a onetime, all-in approach, investors may consider phasing in different elements, starting with functions that are most useful to physicians. That way, physicians perceive the venture as a value-creation opportunity rather than a constraint.
Ample room to grow
The macroeconomic trends that are driving retail health consolidation will sharpen in the foreseeable future. Competition for acquisitions of single practices will intensify, particularly in easy-to-consolidate countries and specialties. Yet there is plenty of “white space” in most European countries and sectors. And any healthcare service that can be provided in an outpatient setting can be consolidated into a retail health chain, offering further potential for innovation and future growth.
Investors—whether they are entrepreneurial physicians or professional private equity funds—will need to carefully navigate the regulatory landscape of each country and ensure that incentive schemes do not conflict with medical ethics. They will also need to invest in initiatives selectively, balancing clinical improvements and efficiency gains against further acquisitions. This requires deep insights into the healthcare sector and retail growth models.
With the right strategy in place, all stakeholders stand to benefit from retail health consolidation. Patients gain improved access to care, physicians have more flexibility and choice, and investors acquire long-term, stable returns. The outlook is promising for countries that foster the right conditions for retail health consolidation and growth.
Franz-Robert Klingan is a Bain & Company partner who leads the firm’s Healthcare Private Equity practice. He is based in Munich. Christoffer Precht is a Bain partner and a leader in the firm’s Private Equity practice, and is based in Stockholm. Giovanni Battista Miani is a Bain principal and a leader in the Private Equity practice. He is based in London.
The authors thank Anna Kestner and Edie Wu for their contributions to this brief.