Report

Резюме
- Intense competition for HCIT deals kept valuations high in 2019. A surge of innovation has attracted a wide range of investors, including corporates and buyout firms that have less history with healthcare.
- Total disclosed value surged to a record $17.5 billion compared with $8.6 billion in 2018. Value was pushed up by the two biggest deals of the year—Press Ganey and Waystar—which accounted for about 40% of disclosed value.
- Some 51 deals closed in 2019, roughly in line with the 48 completed in 2018.
- We saw five themes play out over the year: derivative plays on high-growth sectors; financing fund flows; managing costs of self-funded employer plans; using digital technologies to improve patient outcomes; and data businesses.
This article is part of Bain’s 2020 Global Healthcare Private Equity and Corporate M&A Report. Explore the contents of the report here or download the PDF to read the full report.
A decade ago, much of HCIT activity focused on adoption of electronic medical record (EMR) solutions. Today, the field has advanced to a wide array of solutions helping companies reduce costs and improve outcomes across a range of subsectors. This recent surge of innovation has prompted a wide range of investors, from traditional healthcare and technology buyout firms to corporates, to chase HCIT assets in 2019.
Deal activity held steady at 51 announced deals, matching the record 48 deals in 2018. Most came in the provider sector. Disclosed deal value surged to a record $17.5 billion, up from $8.6 billion in 2018.
The two largest deals of the year accounted for $6.9 billion, or about 40% of total value. Leonard Green and Ares Management led a consortium’s acquisition of Press Ganey; and EQT and CPPIB bought Waystar, with each target company offering a different value proposition.
Many funds with less healthcare experience joined the hunt, especially those that have historically focused predominantly on technology investments, such as Golden Gate Capital.
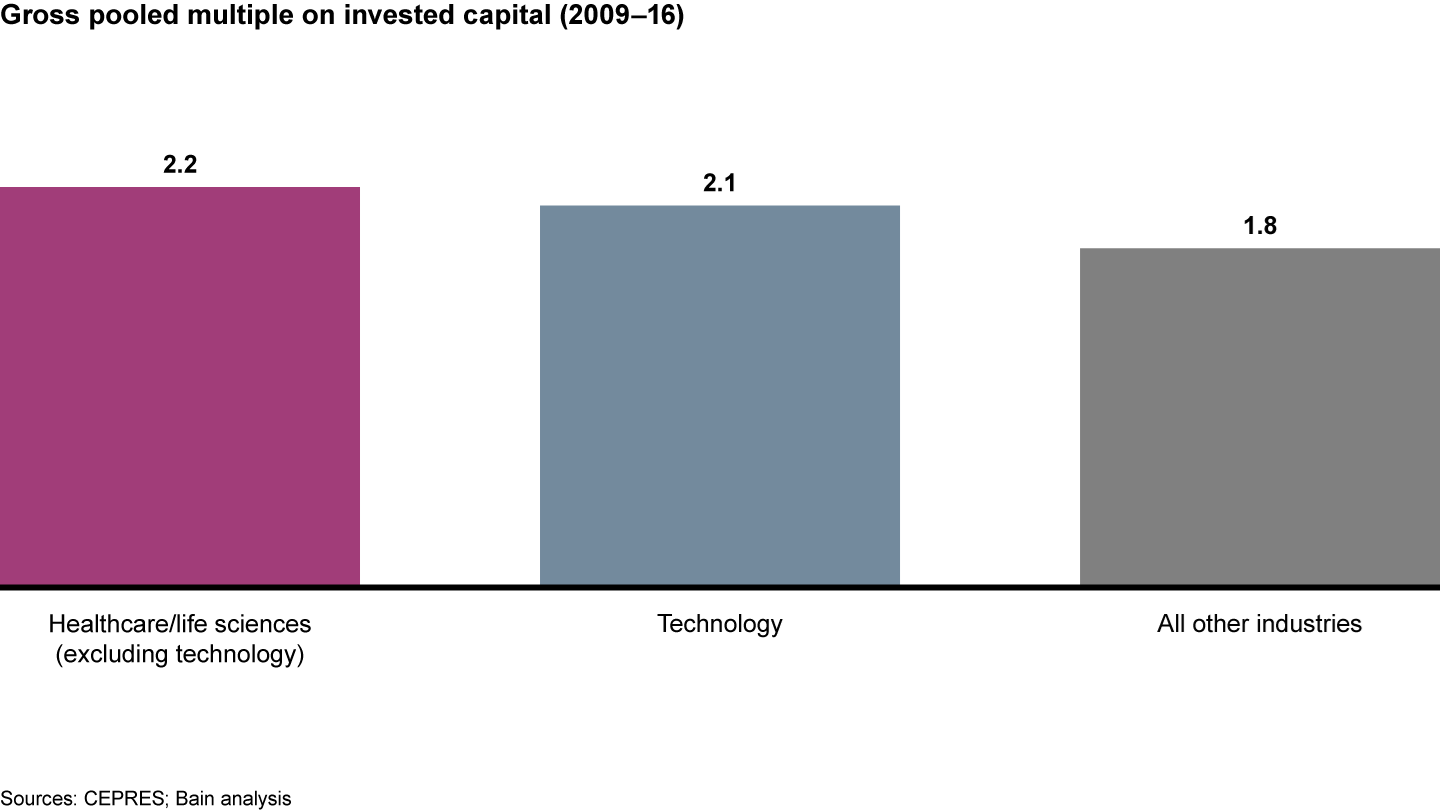
Healthcare private equity enthusiasm stems in part from the fact that healthcare and technology investments both outperformed the average return of other sectors (for investments made between 2009 and 2016, see Figure 7).
The healthcare and technology sectors each outperformed the average return of other industries

We saw five distinct investment themes play out during the year:
- derivative plays on high-growth sectors, such as efficiency in pharma trials or alternative site EMR;
- financing flows such as payments, payment integrity, out-of-network expense management and revenue cycle management (RCM);
- managing costs of self-funded employer plans;
- using digital technologies to improve patient outcomes; and
- data businesses.
Let’s look at each in turn.
1. Derivative plays on high-growth sectors
HCIT assets serving high-growth segments attracted a lot of attention. Derivative plays allow funds to invest in the more fragmented HCIT sector while enjoying the benefits of the strong fundamentals of segments such as pharmaceutical trials management and alternative site providers.
Complexity in therapies and regulatory requirements has put pressure on biopharma companies to run trials efficiently and without errors. Investors warmed to HCIT assets that enable more cost-effective clinical trials. Such assets can fetch multiples on par with software as a service if the underlying technology is proprietary.
For example, a consortium led by Astorg Partners and Nordic Capital invested in ERT, a hybrid HCIT and pharma services company, in the largest biopharma-focused HCIT acquisition of the year. Nordic Capital bought ArisGlobal, a healthcare software firm that helps clients improve efficiency and assure compliance during drug development and commercialization.
The EMR market for acute care providers has already consolidated to a great extent through major companies such as Epic and Cerner. Yet opportunities can still be found in the more fragmented EMR markets for ambulatory surgery centers, behavioral health sites and other specialized providers. These specialty markets have room for winners to emerge.
For example, Warburg Pincus invested in both Qualifacts Systems, maker of EMR software for behavioral health and human services, and WebPT, an EMR provider for outpatient physical therapists, occupational therapists and speech-language pathologists, with the intent of developing category leadership positions.
2. Financing flows
Healthcare billing and payments is notoriously complex and inefficient in the US. That situation creates an opening to improve financing flows in several areas.
Consider payments, the glue binding together payers, providers, patients and employers in the face of several trends: Patient out-of-pocket expenses are rising, network design and benefits get more complex, providers manage against tight financial performance, and payers seek to create and capture value. Integrated payment-processing solutions that connect payers and providers make up much of the market because payer to provider remains the large majority of fund flows.
Other areas of payments are gaining traction, including those serving the growing share of patient-to-provider fund flows and healthcare-specific services for regional payers serving smaller provider bases. JPMorgan Chase paid more than $500 million to buy InstaMed, which enables patient-to-provider payments and improves provider collections.
Turning to out-of-network cost management and payment integrity, activity has ticked up because payers often are on the hook to help reimburse a large pool of out-of-network expense, and errors frequently occur during billing and payment for claims. Companies providing these services help payers reduce the amount they are obligated to reimburse and reduce errors and overpayment before and after a claim is paid.
This logic led Bain Capital to invest in Zelis Healthcare, whose business includes claims repricing tools and third-party networks to reduce payments on out-of-network bills, and merge it with RedCard Systems. On the corporate side, UnitedHealth Group decided to buy Equian, a payment integrity company, for $3.2 billion and then merge Equian with its Optum health services arm.
RCM assets also continued to attract investor attention following Veritas’s major buyouts of GE Healthcare and athenahealth in 2018. While penetration of core RCM modules in the middle and back-end is high, headroom remains in new modules and front-end solutions such as patient portals, bill estimators and denials management, in RCM services, and in small physician practices. In one notable deal, Golden Gate Capital acquired a majority stake in Ensemble Health Partners, formerly a part of Bon Secours Mercy Health.
3. Managing costs of self-funded employer plans
Costs for employer-sponsored healthcare coverage continue to rise, leading many employers to explore ways to reduce their costs through self-funded plans. Many employers are offering more plan options to their employees including high-deductible health plans and narrower network plans as an alternative to rising premiums on traditional preferred provider organizations (PPOs). They have turned to third-party technology vendors that offer employees tools to navigate their care delivery options in order to receive the right care, reduce their costs and improve outcomes. Employers are also adopting solutions that enable them to pool risk.
For example, Collective Health, a software platform that helps US employers manage health insurance programs, received a $205 million investment from SoftBank Vision Fund. Multiple sources reported that Great Hill Partners provided a more than $80 million investment to Pareto, a leading employee benefit group captive manager that helps businesses self-fund health benefits with greater savings and lower volatility. And Livongo, a chronic condition management company backed by General Catalyst and Kinnevik AB, among others, went public in July.
4. Using digital technologies to improve patient outcomes
US providers are finding it increasingly difficult to deliver high-quality care in part due to changing patient expectations. Patients themselves have become more frustrated with wait times and the quality of care.
In response, health institutions want to monitor and improve patient satisfaction through better outcomes and experiences. We expect to see more investments in technologies that can support those goals, such as the $4.2 billion acquisition of Press Ganey, the industry leader in patient surveys, by a consortium led by Leonard Green and Ares Management.
5. Data businesses
Activity has picked up around assets that incorporate data as part of their competitive advantage. For example, Advent International acquired Definitive Healthcare Partners, whose core platform incorporates data from a variety of sources and layers in custom data pulls. We expect to see greater demand for companies that focus on monetizing useful healthcare data (see the chapter “Healthcare Data Moves to Center Stage”).
Looking ahead, underlying trends favor continued growth for investment in HCIT assets.
In other areas that have been fragmented, such as solutions helping employers contain the cost of care, we expect assets with staying power to gain scale. In payments, not many tradable scale assets remain, but more companies that deal with financing flows could be available.
From a regional perspective, HCIT in Europe should benefit from being one of the few sectors that can cross borders to achieve scale. And in Asia-Pacific, where the supply of healthcare is racing to meet demand, IT will help accelerate progress. In short, there are many investment opportunities in HCIT, but each requires a growth equity mindset.
Venture capital directed to HCIT also has been booming. According to Rock Health, annual venture funding for digital health has grown 80% in the last five years, indicating a healthy pipeline of targets for financial sponsors in the future.
This article is part of Bain’s 2020 Global Healthcare Private Equity and Corporate M&A Report. Explore the contents of the report here or download the PDF to read the full report.