Report

Резюме
- Healthcare payer buyout activity in 2020, including services sold to self-insured employers, more than doubled to 23 deals, from 10 in 2019, and disclosed value increased to $4.4 billion, compared with $3.6 billion the year earlier.
- Three private equity investment themes stood out: direct-to-employer offerings that improve patient experience and lower employer costs, IT capabilities designed to reduce payer cost positions, and expansion of services to the growing Medicare Advantage population.
- We expect investors to keep hunting for assets focused on cost reduction and care improvement, as the most successful companies in the sector are able to demonstrate a measurable ROI for both patients and employers.
This article is part of Bain's 2021 Global Healthcare Private Equity and M&A Report.
Healthcare payer buyout activity in 2020 was driven by North American deals, given the private payer system in the US. There were 23 deals, up from 10 in 2019. Disclosed value also increased to $4.4 billion from $3.6 billion in 2019 (see Figure 1).
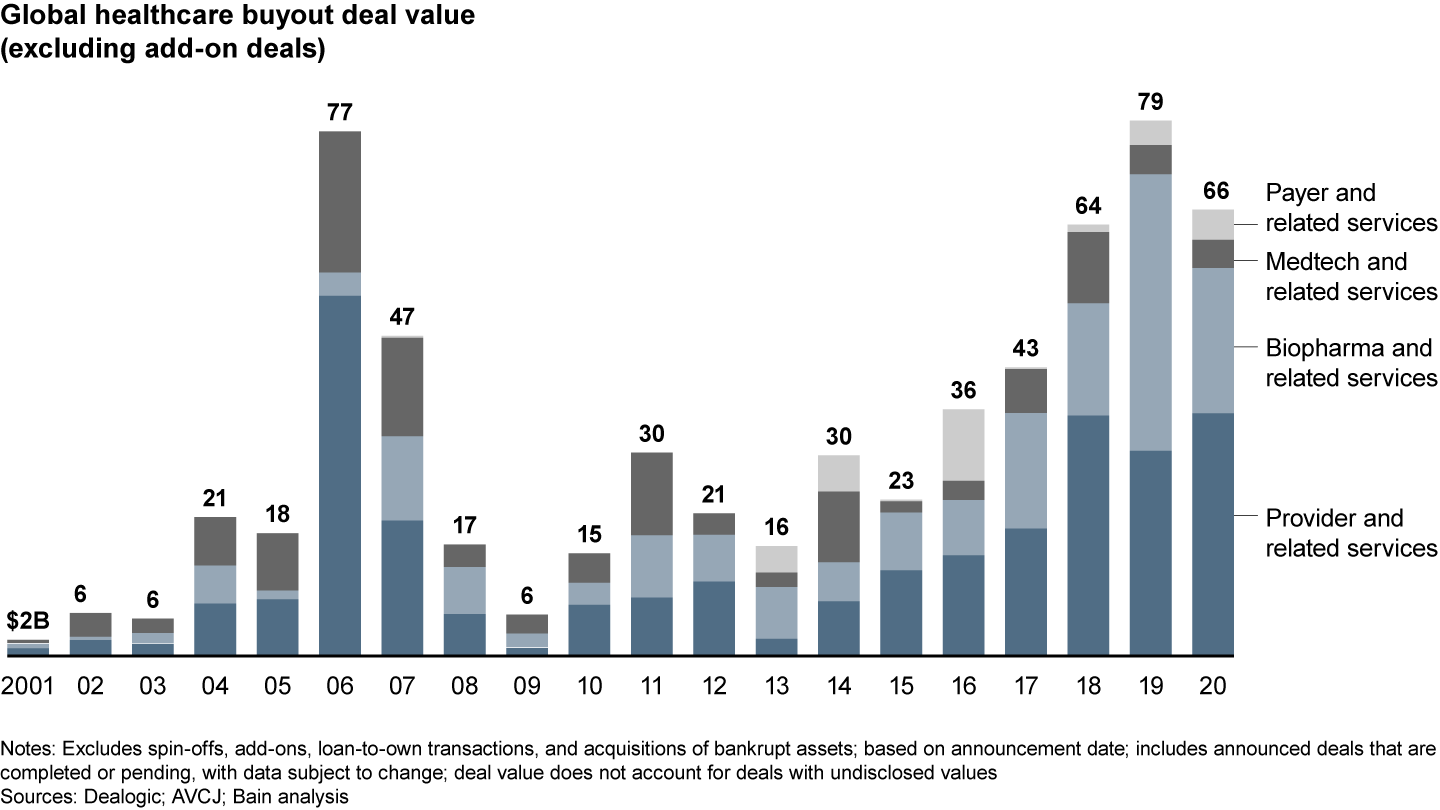

Private equity investments centered on three themes:
- direct-to-employer offerings that improve patient outcomes and lower costs;
- IT capabilities designed to reduce payer cost positions; and
- expansion of ancillary services to the growing risk-bearing Medicare Advantage (MA) providers.
Meet the members of Bain’s Healthcare Private Equity practice.
Direct-to-employer offerings to improve patient outcomes and reduce costs
Care management companies, focused on offerings for self-insured employers and patients, sparked enthusiasm among investors. These firms partner with employers and offer the dual value proposition of providing benefits to employees while lowering health expenses.
One deal exemplifying this trend from 2020 was Quantum Health, a care navigation and coordination company that received an investment by Warburg Pincus in partnership with Great Hill Partners. Quantum works closely with patients throughout the care continuum. For instance, it engages with members at the time of prior authorization to help manage care utilization and navigation to in-network healthcare providers, in addition to providing care coordination and patient follow-ups. Similarly, Grand Rounds, which secured a $175 million investment from The Carlyle Group, provides virtual expert medical opinions with specialists in addition to broader benefits navigation.
On the pharmacy side, employers also turn to pharmacy benefit managers (PBMs) and related service providers to improve patient outcomes and lower their prescription costs. PBM-related service companies—firms that provide technology or consultative services to employers or other pharmacy intermediaries on managing PBM services—have garnered interest from investors due to their technology and clinical advisory support. Attractive targets have shown that they can help simplify administration and reduce the cost of drugs to employers and their members.
For example, Advent invested in RxBenefits in partnership with Great Hill Partners. RxBenefits provides services and analytics to self-funded employers to aid in pharmacy benefit plan design and optimization. Further, RxSense, invested in by Parthenon Capital Partners, provides a cash pay discount card under the SingleCare brand, as well as a broader pharmacy benefits platform solution for employers.
IT capabilities designed to reduce payer cost positions
Payers are increasingly looking to leverage the mass of data that they generate and to improve upon older, often siloed, legacy technology infrastructure. One goal is to better use their data to make operations more efficient. Several deals from 2020 support the flow of payer data among various healthcare stakeholders, ultimately enabling better decisions and outcomes.
For instance, TA Associates, in partnership with Francisco Partners, acquired a majority stake in Edifecs, which helps payers optimize the exchange and processing of administrative and clinical data, automate workflows, and reduce the cost of regulatory compliance. Deerwalk, acquired by GTCR portfolio company Cedar Gate, aggregates and helps analyze patient data, which is shared to support insights for payers, third-party administrators, and employers.
As mentioned above, other deals focus on core payer operations and on improving existing baseline tech and infrastructure. Administrative systems support business activities such as claims processing and policy administration. These digital offerings provide shorter plan configuration lead times, lower administrative costs, higher interoperability, and greater visibility into incoming claims through strong data management. Healthedge, acquired by Blackstone, offers a digital platform for claims and benefit administration and care management assistance, ultimately helping payers manage existing plans and enroll new participants.
Expansion of services to growing Medicare Advantage providers
Private equity investor interest in Medicare Advantage (MA) plans has grown alongside increasing MA enrollment. As consumer interest in these plans grows, so has competition, and the need for plans to differentiate themselves in the MA market has become apparent. As a result, sponsors have shown interest in supplemental benefits that support patient health and can help create such differentiation. Food services were the most active supplemental benefit for investments during 2020, though we expect others to spark activity in the future.
PurFoods and GA Food, invested in by Berkshire Partners and Warburg Pincus, respectively, illustrate this movement to supplemental benefits, providing tailored, home-delivered meals for MA patients. This also fits in a broader theme of payers looking more closely at social determinants of health, including food security and nutrition, as a means to improve outcomes.
Additionally, several deals in marketing services for MA plans also occurred in 2020. Similar to supplemental benefits, these services aim to help differentiate plans and increase patient recruitment.
Lightyear acquired a controlling stake in Healthplan One, which offers digital marketing and distribution of senior health insurance products in the Medicare space, matching people with the right insurance. Similarly, Benefytt, bought by Madison Dearborn, offers health insurance technology and distribution of Medicare-related plans to assist individuals in finding an appropriate MA plan.
Still in search of affordability
Over the next year, we expect investors to keep hunting for assets focused on cost reduction and care improvement, as the most successful companies in the sector have been able to demonstrate a measurable ROI for patients and employers. In 2020, this trend was illustrated by one of the largest healthcare exits, Multiplan’s $9.7 billion exit to the public market via a special purpose acquisition company.
We also expect growth in MA supplemental services to continue. Additional services, such as patient transportation and vision services, should garner investor activity as healthcare payers aim to differentiate their offerings to the growing MA population.
Another notable trend to watch involves moves by large payers to offer more robust, coordinated, and well-funded healthcare services to other plans, third-party administrators, and providers. The net effect on payer deals is too early to call, because these offerings may create opportunities for sponsor assets, but could also pose a longer-term threat given the additional competition they will present to deals in the payer sector. One example is Cigna’s Evernorth, a new brand offering benefit management, behavioral and clinical care plans, and pharmacy benefits for partner providers that want their own sponsored plans, but lack experience in pricing or risk assessment.
More from the report
-
Welcome Letter: Fertile Conditions for Healthcare Private Equity Investment
-
Healthcare Private Equity Market 2020: The Year in Review
-
The Covid-19 Paradox: Widespread Repercussions for Demand, but New Healthcare Investment Opportunities as Well
-
Healthcare Private Equity in North America: Bring On the Gem Assets
-
Healthcare Private Equity in Europe: Steady Dealmaking despite Many Deferrals
-
Healthcare Private Equity in Asia-Pacific: Riding a Wave of Domestic Innovation
-
Healthcare Providers: New Roll-Up Candidates and a New Look for Risk-Bearing Providers
-
Healthcare Payers: A Bid to Reduce Costs for Patients and Employers
-
Biopharma: Commercialization Support Services Are Thriving
-
Medtech: Four Themes Fueled Deals despite the Pandemic
-
Healthcare IT: Technologies Help Improve Patient Experiences at Lower Costs
-
Healthcare M&A: A Pandemic-Induced Slowdown in Every Sector
-
Healthcare Exit Activity: Robust Capital Markets Spur a Surge of IPOs
-
Healthcare Private Equity Outlook: 2021 and Beyond