Report

At a Glance
- New payer business models attracted a surge of investment in 2021, with deal value more than tripling and five deals of over $1 billion.
- Payers expanded investments in the provider space to strengthen patients’ overall care and to tap the provider profit pool.
- Private equity also flowed to deals involving specialty-specific value-based care, Medicaid, and social determinants of health.
- With payers promoting the health of their members, investments that align incentives for all stakeholders could realize outsized returns.
This article is part of Bain's 2022 Global Healthcare Private Equity and M&A Report
As the lines between payers and providers continue to blur, companies that support new payer business models have benefited from a surge in investment. While the number of payer buyouts in 2021 increased slightly to 24 deals from 23 the year prior, disclosed value rose dramatically to $15.3 billion from $4.4 billion (see Figure 1). Five of the deals were valued at more than $1 billion, and three exceeded $3 billion. Consistent with previous years, the activity was concentrated in North America, given the diverse and largely private payer landscape in the US. North America accounted for 83% of payer deals and 98% of disclosed deal value.
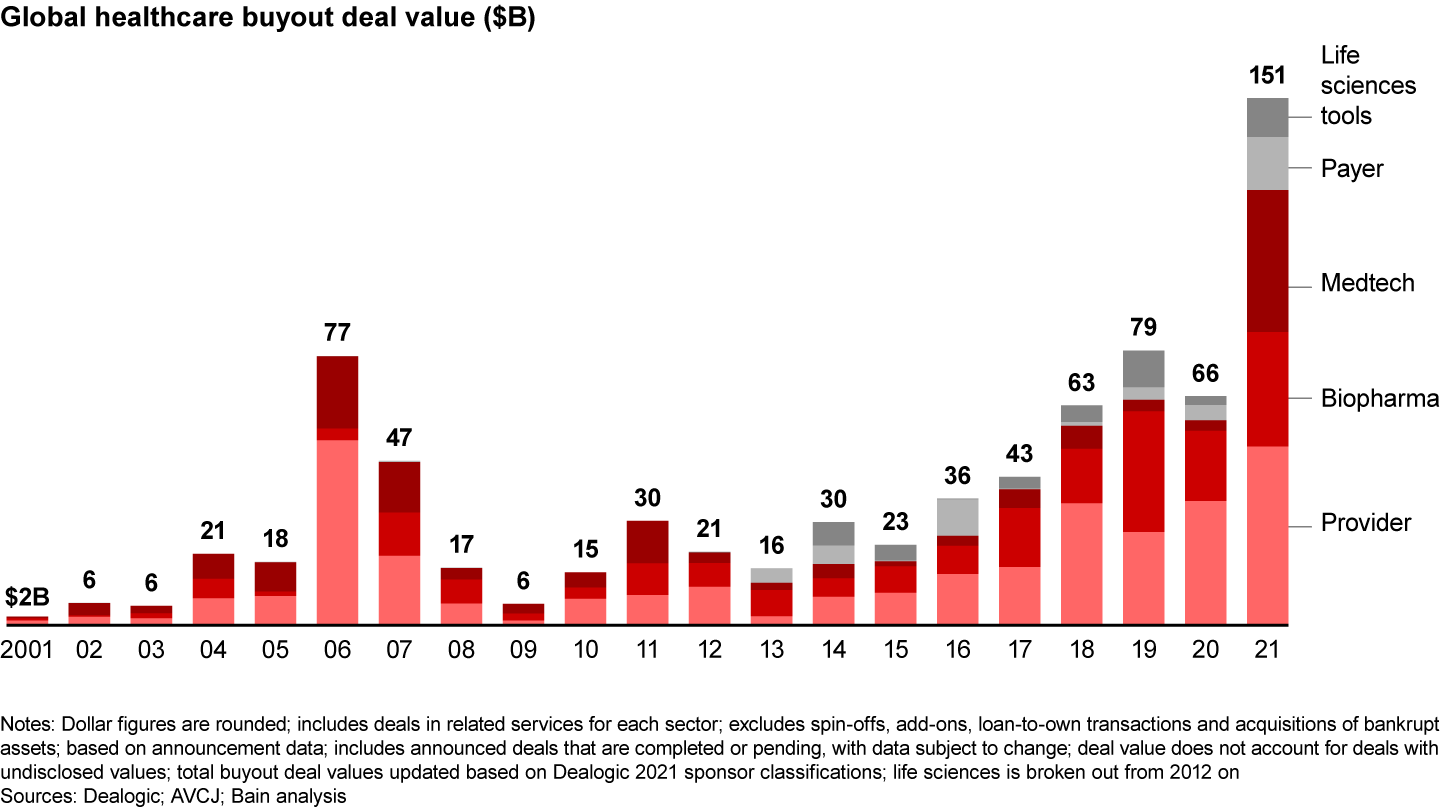

With costs rising rapidly and value-based care models maturing, the role of US payers is being redefined, leading to major opportunities for value creation. Outside the US, insurgent European companies such as Alan and Best Doctors received growth-equity investments, proving that tech-enabled, customer-centered insurance services can also thrive in different payer markets.
Our analysis finds that private equity funds pursued assets along four dimensions in 2021:
- expanding payers’ role in providing services to patients;
- using data to improve member engagement and outcomes;
- Medicaid and the social determinants of health; and
- cost-containment solutions for specialty insurance markets.
Expanding payers’ role in providing services to patients
Commercial payers ramped up investments in the provider space as part of a broader move to strengthen their role with patients’ overall care and to tap the provider profit pool. UnitedHealth’s Optum further expanded its physician network with the acquisition of physician groups Atrius Health and Beaver Medical Group, widening its lead as the largest employer of US physicians. Centene acquired Magellan Health, a benefits manager for behavioral health, for $2.2 billion, to solidify its foothold in that field.
Private equity investors also found ways to partner with payers in strategic investments focused on value-based care. In primary care, Blackstone Growth, Anthem, and digital health start-up K Health launched Hydrogen Health, which delivers on-demand virtual primary care powered by artificial intelligence.
Turning to specialty-specific value-based care models, these target the roughly 90% of commercial healthcare spending controlled by specialists. For example, Welsh, Carson, Anderson & Stowe’s subsidiary Valtruis led an $83.5 million Series B for Cricket Health, a value-based kidney care provider, alongside Blue Shield of California, Cigna Ventures, and Oak HC/FT. Valtrius, Centene, and other investors took part in a $75 million investment in Wayspring, which leverages data analytics to deliver value-based care for patients with substance use disorder.
Despite these investments, insurance hasn’t truly integrated with care delivery to create value. These investments represent a long-term bid by payers to excel in an increasingly fee-for-value world where providers stand to capture more of the profits.
Using data to improve member engagement and outcomes
More and more payers view members’ health outcomes as critical to their bottom line. Reining in costs for all members requires insights that can inform new ways of working, combined with outreach to targeted members derived from clinical and claims data sets.
Companies that help payers translate data into interventions attracted a surge in investor activity. Notably, Nordic Capital, Insight Venture Management, and 22C Capital acquired Inovalon Holdings, a healthcare data platform that offers a range of solutions that improve member health outcomes, for $7.3 billion. CVC also took a majority stake in Icario, a technology platform that translates data into targeted member engagement for better health outcomes. And on the heels of 2020 purchases of Altruista and the Burgess Group, Blackstone portfolio company HealthEdge acquired Wellframe, a software platform that uses real-time member data and artificial intelligence to help payers identify when and how to intervene with high-risk members.
Medicaid and the social determinants of health
Inspired by the success stories in Medicare Advantage, investors have turned to Medicaid. As with Medicare Advantage, success in managed Medicaid involves actively engaging with members to keep them healthy and out of the hospital. However, there’s another ingredient in serving Medicaid patients: a greater emphasis on addressing the social determinants of health.
In one such deal, Gainwell Technologies, a portfolio company of Veritas Capital, bought HMS Holdings, a Medicaid-focused healthcare technology, analytics, and engagement solutions provider, for $3.3 billion. One HMS product identifies high- and rising-risk members, triggering adjustment of a members’ disease management before they need to be hospitalized.
Growth-equity investors increasingly look for companies that address the nonmedical social conditions that influence health outcomes. Payers stand to reduce healthcare costs when they tackle the root causes of disease. For example, Cityblock Health, which helps Medicaid plans provide coordinated, tech-enabled care for physical, mental, and social health, raised $400 million in a late-stage round led by SoftBank. Unite Us, which connects patients with social services, will expand its nationwide social care infrastructure with $150 million of funding led by ICONIQ Growth. For-profit initiatives to address social problems are a mostly American phenomenon, and the infusion of private capital increases their potential for broad impact.
Cost-containment solutions for specialty insurance markets
While cost-containment tools for traditional payers have long attracted private equity, investors are now focusing on specialty insurance markets, especially workers’ compensation, for returns. For example, CVC acquired a controlling stake in ExamWorks, a provider of independent medical examinations as well as medical record and bill-review services, from Leonard Green for $4 billion. CVC also bought a majority interest in MedRisk, a managed care organization performing physical therapy under workers’ compensation, for $1.2 billion from Carlyle, which will retain a significant stake.
Aligning incentives could lead to outsized returns
We feel confident in noting several trends for the next few years.
First, payers will continue to build new business lines, seek partners, and make acquisitions that help them deliver a differentiated member experience and tap into new profit pools. In turn, valuations will rise for companies that support a better member experience or the integration of diverse healthcare services businesses.
As payers evolve into diversified health services companies, technology that helps them streamline or automate core payer functions will attract investor interest. Digital brokerages, transparent pharmacy benefit managers, and other tech-enabled firms will present outsized opportunities.
Companies that work at the interface of payers and providers, through such things as data exchange or population health management, will grow quickly. In particular, firms that enable payers to reduce costs across member populations will remain in demand.
Larger physician groups will be attractive acquisition targets for payers building out their physician networks, particularly groups with a track record of accepting risk beyond simple upside-only agreements.
Medicare Advantage will continue to attract investment as the fundamentals of an aging population, rising enrollment, and large profit pools remain strong. Investments will accelerate in value-based Medicaid and commercial models, as value-based care takes off in the Medicaid and employer-sponsored insurance markets.
Specialty-specific benefit management solutions—especially in high-cost disciplines such as cardiology, dialysis, oncology, and orthopedics—will see a surge in investor interest, but require thoughtful strategic planning to optimize value creation.
Finally, firms that help payers address the social determinants of health will attract more investment. The Covid-19 pandemic exposed the profound effects of social circumstances on health outcomes, and as payers take on more responsibility for these outcomes, they’ll look for partners to address what influences health outside the traditional purview of medicine. And companies that can prove cost savings to managed Medicaid, other value-based care plans, risk-bearing providers, or self-insured employers will also benefit from new investment.
Payers are well along their transition from insurers to diversified healthcare services companies. It’s a promising shift toward aligning incentives for all involved—payers, providers, and patients—in order to improve health. Investments that create value in this context could realize outsized returns.