Brief

India's healthcare sector continues to face increasingly complex challenges. A large population and low overall healthcare and public spending have led to skewed access to healthcare across the country. According to a World Health Organization (WHO) global health report, India's per capita health spending is only about 20% of China's.1
As India's growth has increased and as incomes have risen consistently, the country's disease burden also has shifted. In 2016, the majority of deaths in India (61.8%) were due to noncommunicable diseases (NCDs) such as cardiovascular and chronic respiratory diseases, whereas in 1990, the majority of deaths (53.6%) were due to communicable, maternal, neonatal and nutritional diseases, according to a recent study published in the medical journal Lancet.2
In responding to this shift, India's health system faces multipronged challenges. NCDs increasingly threaten the physical health and economic security of many lower- and middle-income people, and challenges from infectious diseases persist in the country. India ranks second in the world in prevalence of diabetes according to The International Diabetes Federation.3
Vikram Kapur, a partner with Bain's Healthcare practice, discusses four areas that providers can focus on to improve their operational excellence.
Highly underindexed in delivery infrastructure
Unfortunately, India is severely underindexed in healthcare delivery infrastructure. The government infrastructure, in particular, is woefully inadequate. India's per capita public and private healthcare spending in 2016 was $87, compared with $10,203 in the US and $471 in China.4
India also has fewer hospital beds and nurses than either China or the US. In 2016, India could provide only 0.8 hospital beds per 1,000 people, whereas the US and China offered 2.8 beds and 3.5 beds, respectively. The private sector accounts for 63% of hospital beds in India, and government reports indicate that the country is 81% short of specialists at rural community health centres.5
India's per capita healthcare spending (as a proportion of GDP) and specifically public spending is among the lowest per capita in the world. (By comparison, per capita healthcare spending in China and in the US are, respectively, 5.4 times and 117.3 times that of India's.) Indians use their personal savings to pay for more than 62.0% of their out-of-pocket healthcare expenses. This figure compares with 13.4% in the US and 54.0% in China.6
The rise of NCDs poses a major threat to India's health and economic security. New, costlier technologies, drugs and infrastructure are driving up delivery costs among private healthcare providers. As a result, the affordability gap is constantly widening, especially for lower- and middle-income groups.7 In addition, domestic healthcare infrastructure is developing slowly, and far too few people are choosing to become physicians, further straining the healthcare ecosystem.
The government has recognised the system's gaps and is introducing several healthcare schemes to benefit the country's underprivileged populations. The government's latest announcement of INR 5 lakh insurance coverage for poor families under the National Health Protection Scheme is notable in this regard.8
The existing healthcare infrastructure, however, simply cannot meet the population's needs. Despite universal healthcare services, free treatments and the availability of essential drugs at government hospitals, lack of staffing and financing often forces rural residents to turn instead to private physicians and hospitals.9
In this context, private Indian healthcare providers are a key link to solving India's burgeoning healthcare burden.
Strong case for change across private healthcare providers in India
Healthcare delivery in India requires a massive change at every stage including prevention, diagnosis and treatment and requires integration of care from each of those stages. Private healthcare providers have a complex and difficult responsibility to provide superior clinical delivery and patient experience while managing costs and providing optimum financial returns. The healthcare sector can only evolve if all stakeholders participate and innovate.10
The government also is trying to curb several costing and pricing practices that have crept into the system. As a result, the margins of private healthcare providers are under pressure. In this context, healthcare providers face multiple demands from multiple stakeholders, including increased pricing pressure from the government, cost and quality concerns and affordability issues from patients and the public, intense competition, increasing payer power and a pressure on margins straining returns on capital.
To better understand existing realities and perspectives, we conducted research among NATHEALTH members across India, engaging healthcare service, diagnostic service and medical equipment providers.
Our research made it abundantly clear that regulation, competition and public trust—or lack thereof—constantly tug at private healthcare providers in India. Eighty per cent of respondents said that regulatory uncertainty and pricing pressures were the top sustainability concerns plaguing India's healthcare providers. Competitive intensity, a severe deficit of public trust and intense activism were other leading factors (see Figure 1). Providers must judiciously manage all these demands to remain sustainable.
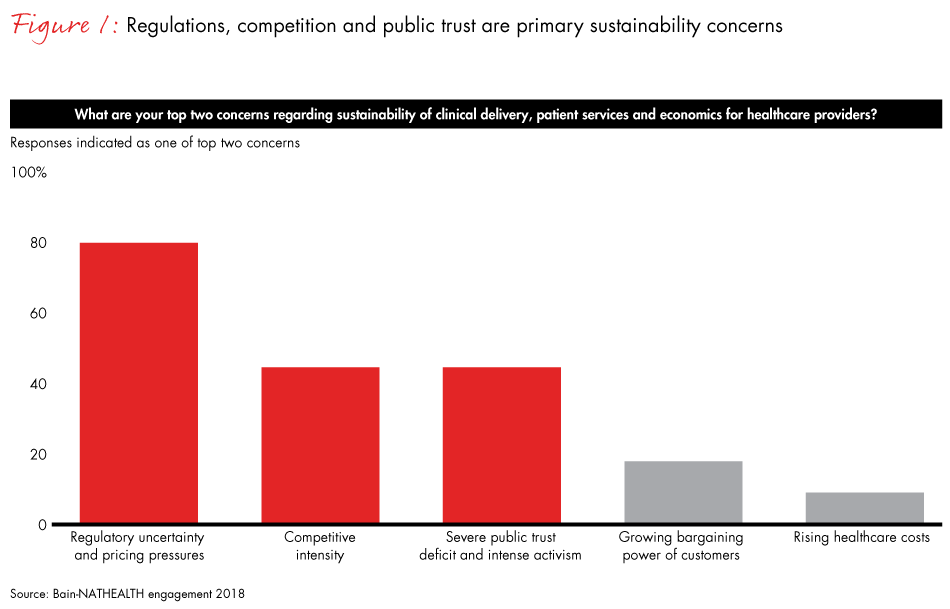
Considering the various pressures in the healthcare industry, the managing director of a leading hospital chain in India said, "If we study healthcare economics in more detail, across the sector, return on capital employed (ROCE) is just 10%, which is just enough to plough back into the business."11
Profitability of private healthcare providers is under pressure, and shareholder returns significantly lag market standards. The consolidated EBITDA margin of the top three hospital chains in India was 12% in March 2013. By March 2016, it had dropped to 9%, according to Bloomberg data. Worse, the annualised total shareholder return (TSR) of the top four hospital chains in the two-year period between August 2015 and August 2017 was negative 8%, compared with the TSR of BSE SENSEX companies offering a positive 11% TSR during the same period, Bloomberg indicates.
Private providers today face major challenges in delivering healthcare services across the country. Most healthcare professionals practice in urban areas, where consumers have a greater ability to pay for services. As a result, rural areas tend to be underserved.12 India meets the global average in its number of physicians, but three-fifths of its doctors cater to one-third of the urban population.13
Consequently, several healthcare service providers in India can’t invest because they are focussed on managing costs. The severity of each medical case varies, care is not standardised and the quality of clinical delivery is variable over time and across providers. Patient experience and service standards could suffer as providers struggle to manage costs in this evolving market.
There is thus a strong case for change across private healthcare providers in India.
Private healthcare: Issues and challenges
For the sake of both private healthcare providers' viability and patients' health, operational improvements are key. However, judging by providers' experience, few have succeeded in making such improvements. Failure of these efforts typically relates to organisational and change-management issues. Only about 20% of the respondents we engaged have benefitted from operational improvement measures. About 65% are still in the process of implementing solutions; most are attempting to optimise only procurement, processes and overhead (see Figure 2).
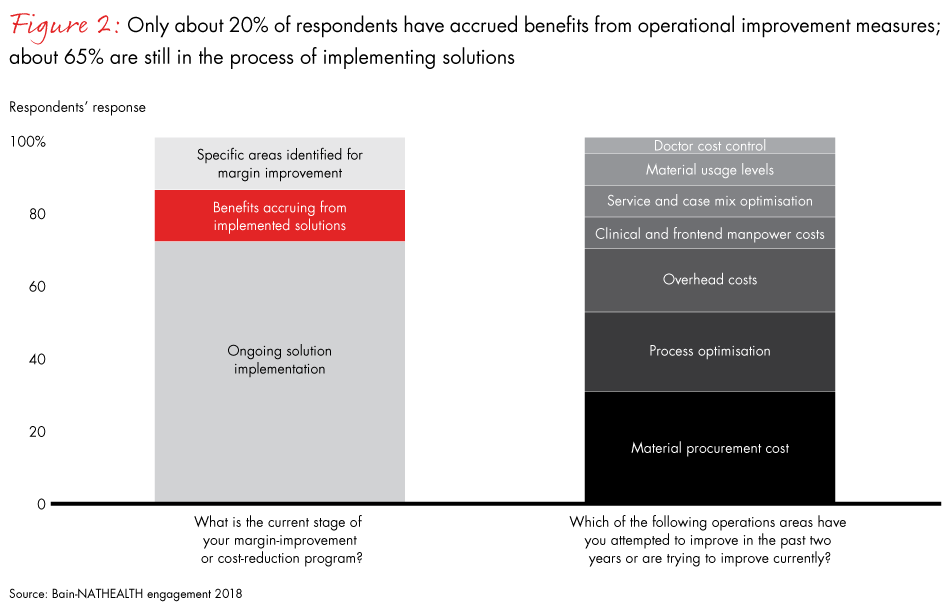
Indeed, operational improvement is easier said than done. Most respondents' goals were unambitious: Approximately 80% targeted a reduction in costs of less than 15%. Yet approximately 60% of respondents met only limited success (see Figure 3).
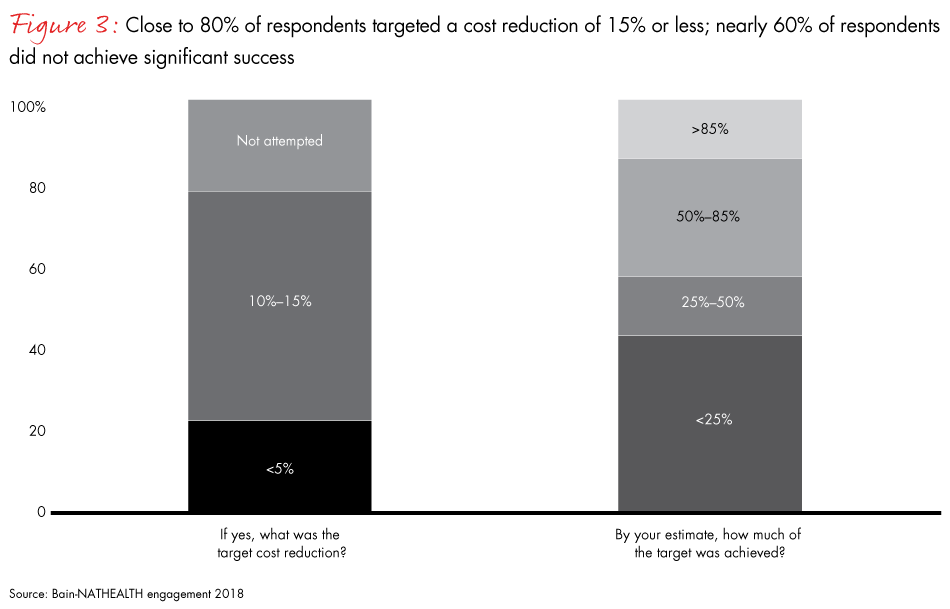
As the government makes patient needs the focus of policy decisions, large private hospitals and other healthcare service providers are also willing emphasise patient needs. For many, patient feedback has emerged as important input in their systems to monitor and improve quality of services. As an indication of this focus on quality, healthcare providers in recent years have opted for accreditations, which lead to higher-quality patient care and safety. This accreditation approach not only benefits patients but also distinguishes hospitals in a competitive environment.14
To be sure, cutting costs to improve profitability has not been easy for healthcare providers. Some are unable to make tough decisions and end up trying to cut costs in easy places that could adversely affect patient experience. Other barriers to operational improvement healthcare providers in India experience include their conservative approach, failure to engage the entire business organisation and lack of tangible improvement in business (see Figure 4).
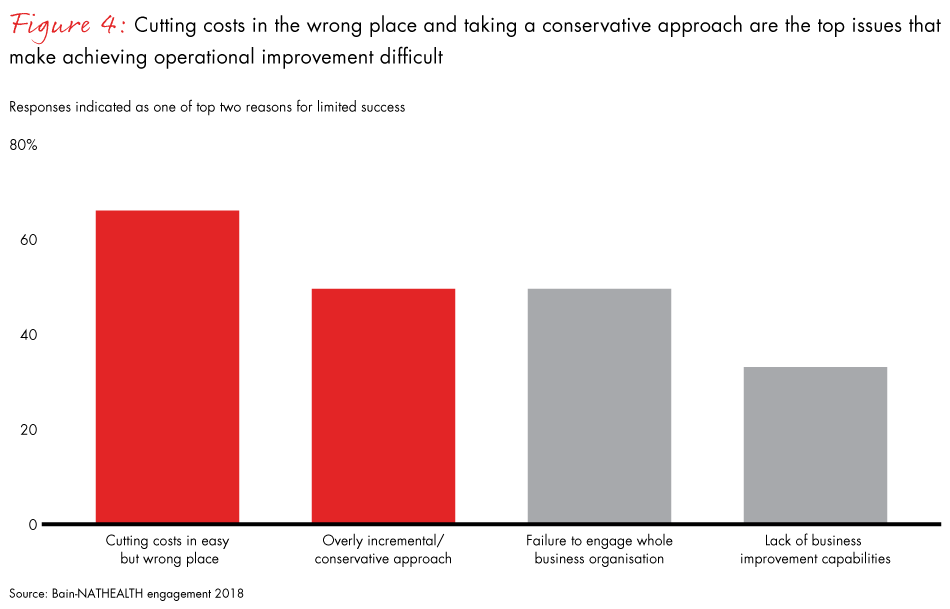
Against such a stark backdrop, one thing is clear: To manage costs with quality, designing operations at hospitals, whether it is pricing, procurement, monitoring consumption or staffing, is at the top of the agenda for Indian healthcare providers today.
A zero-based lens
To improve margins and reduce costs, companies need to adopt a zero-based operations transformation approach. The traditional approach to margin enhancement and cost cutting is typically short-term and unsustainable. It often cuts muscle and there is little stewardship on clinical quality and customer experience. Suboptimal team staffing, weak process and accountability are other frequent issues (see Figure 5).
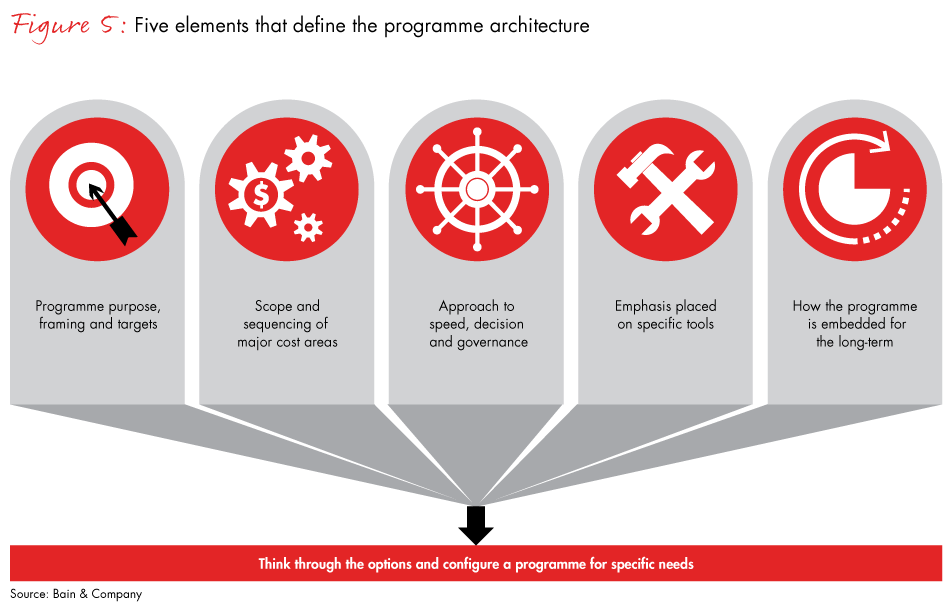
Naturally, improving revenues is the top priority. What short-term actions are needed to improve the top line and margins of a private healthcare provider? Our experience indicates a revenue-enhancement approach that combines value-based pricing, optimised contracting, service mix optimisation and removal of capacity bottlenecks yields the highest returns.
On the pricing front, healthcare providers have optionsfor improving their revenues (see Figure 6). Providers incur significant costs on accreditation, quality upgradation and maintenance, recruiting and building clinical teams. That cost is often designated to standard consumables and diagnostic tests, which angers their patients. Providers could instead take a different approach by focussing on delivering differential value to patients through an ability to handle greater complexity and superior outcomes, then charging differentially for those procedures and specialties.
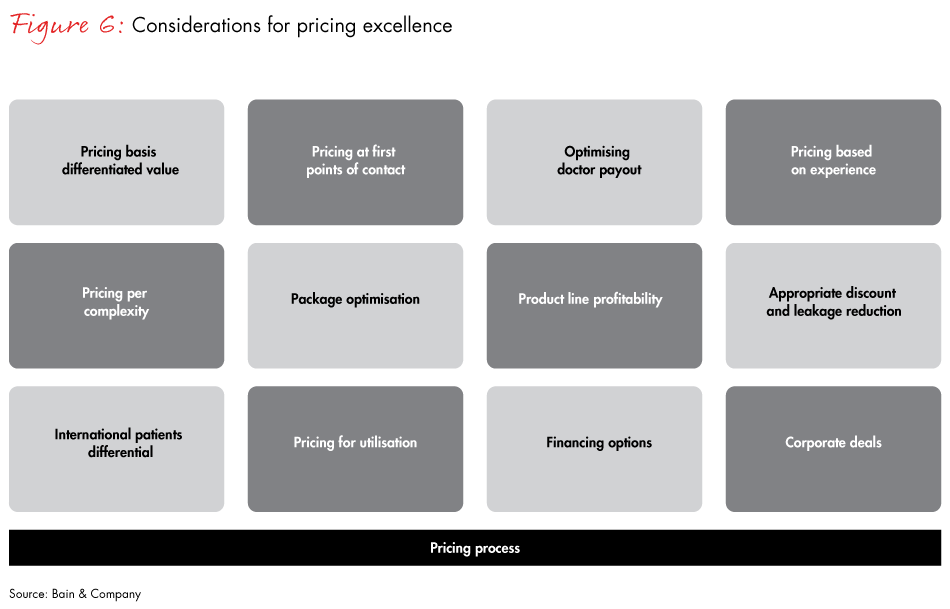
On the costs front, hospitals can take a radical zero-based approach that is focussed on their major cost centres. That approach requires hospitals to distinguish between strategic and nonstrategic costs and to refocus resources for growth. Strategic costs help sell more products at higher prices and link with strategic priorities and "must-win" capabilities. They truly enhance the bottom line and build the business.
All other costs (especially SG&A) are nonstrategic and should be eliminated unless their value can be proved by asking: What would we lose without this spending?
Providers have shaved off substantial costs in the following areas:
- Front-end manpower cost optimisation focusses on the costs associated with staff members (nurses, doctors, residents and so on) who work directly with patients. In our experience, front-end facing staff spends no more than 20% to 25% of their time on patient care and a significant portion of their time on documentation, resolving cross-functional complexity and performing other nonvalue-added processes. In such situations, reducing documentation and process load or automating parts of the job can allow them to focus on the patient and helps energise the staff while eliminating costs.
- Materials cost optimisation harnesses our experience in healthcare to help hospitals buy better (supply tactics) and spend better (demand tactics).
- Overhead optimisation is one of the biggest tools for improving the cost structure. It is important for hospitals to buy better and spend better. Too often, we see hospital groups that are not ambitious enough on these fronts. Their approach is too incremental and focusses on bigger discounts on high-value items from the same suppliers. A segmented approach to physician preference items and nonphysician preference items, with early and fact-based engagement with the physician community, can lead to significant savings.
A good cost transformation strategy focusses on the need, profile and behavioural patterns of customers. This customer-centric approach formulates an integrated roadmap that includes change management as well as zero-based cost accounting.
We believe a well-structured operations transformation programme can create 8% to 15% top-line growth, a 7% to 22% reduction in manpower costs, a 12% to 20% reduction in materials spending and a 20% to 30% reduction in other spending, to achieve an EBITDA growth in the range of 15 to 20 percentage points per year (see Figure 7).
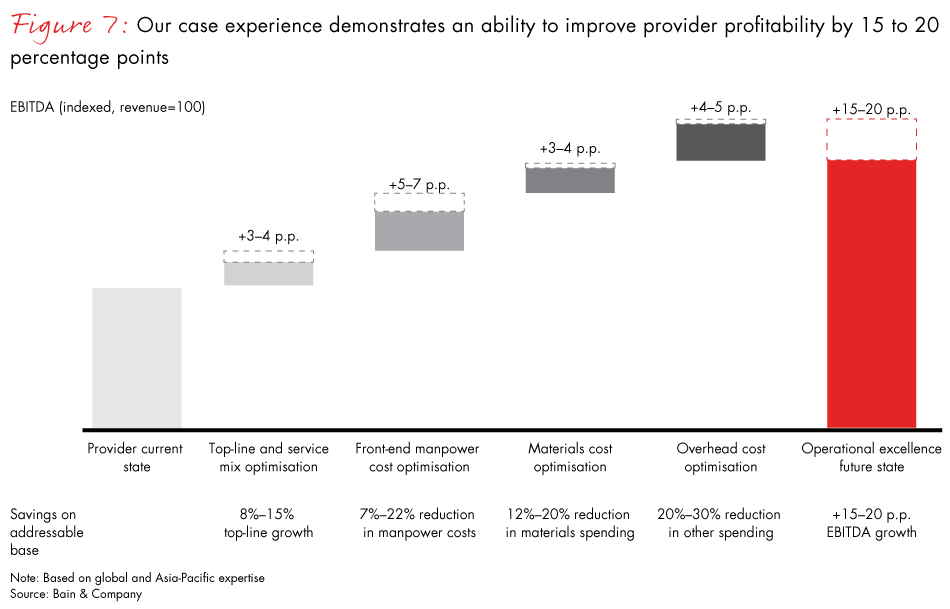
Change management and Results Delivery®
Behaviour change is often the biggest challenge during and after an operations transformation programme. Any management executive embarking on an operations transformation initiative in a provider setting is advised to focus on change management to realise its value. Using a data-based, objective approach identifies delivery risk areas early and measures and mitigates the risk by allowing early intervention.
Early alignment on a bold vision ensures leadership commitment. Additionally, creating clear sponsorship across the organisation, co-creating solutions with the team and ensuring appropriate incentives helps make change stick.
Instances: Case studies
A multispecialty hospital with several primary clinic satellites faced financial and patient advocacy challenges. In addition, the hospital's financial deficit was increasing due to high manpower costs, overstaffing of medical personnel, low legacy pricing and underutilisation of key medical facilities. For this hospital, we managed to achieve a 6% upside on EBIT within the first 12 months. Over the next five years, we expect to reduce the deficit by 30% to 40%. The hospital has seen a more than 20% increase in its Net Promoter Score ® (NPS®).
Another not-for-profit healthcare and senior care provider with which we worked was under margin pressure due to public funding cuts. The provider achieved a 5% savings on spending across eight opportunities in six months. A private hospital chain that had been facing customer loyalty, advocacy, pricing and clinical issues showed a 25% to 30% increase inpatient NPS after working with us. Referral traffic almost doubled, and revenue increased by 8% over baseline growth using strategic pricing.
In addition, another healthcare provider with multiple hospitals and pathology centres identified an 11% uptick in EBITDA through shared services.
1.The World Bank, "Health Expenditure per Capita (Current US$)," World Health Organization Global Health Expenditure database, accessed 18 February, 2018, https://data.worldbank.org/indicator/ SH.XPD.PCAP.
2.India State-Level Disease Burden Initiative Collaborators, "Nations Within a Nation: Variations in Epidemiological Transition Across the States of India, 1990–2016 in the Global Burden of Disease Study," Lancet, 2017; 390: 2,437–60. http://www.thelancet.com/pdfs/journals/lancetPIIS0140-6736 (17)32804-0.pdf.
3.International Diabetes Federation, IDF Diabetes Atlas, Eighth edition 2017, http://www.diabetesatlas.org.
4. Business Monitor International (BMI) Research, "Pharmaceuticals & Healthcare: China, India, United States," accessed 12 February, 2018.
5."Rural Health Statistics 2014–15," Government of India Ministry of Health and Family Welfare Statistics Division. http://wcd.nic.in/sites/default/files/RHS_1.pdf. Accessed March 8, 2018.
6.TNN, "Indians Spend over 62% of Their Savings for Health Expenses, Says PJ Kurien," The Times of India, 14 November, 2017, https://timesofindia.indiatimes.com/city/chennai/indians-spend-over-62- of-their-savings-for-health-expenses-says-p-j-kurien/articleshow/61635289.cms.
7.GE, "How India Can Overcome the Doctor Shortage and Exorbitant Costs of Healthcare," sponsored content in Quartz, accessed 18 February, 2018, https://qz.com/269392/how-india-can-overcome-the- doctor-shortage-and-exorbitant-costs-of-healthcare/; and Government of India, Ministry of Health and Family Welfare, Department of Health and Family Welfare, "Unstarred Question No. 2259," answered 28 July, 2017, http://164.100.47.190/loksabhaquestions/annex/12/AU2259.pdf.
8.Arun Jaitley, Minister of Finance, budget 2018–2019 speech given February 1, 2018. http://www.indiabudget.gov.in/ub2018-19/bs/bs.pdf. Acccessed March 8, 2018.
9.Nayan Kalnad, Niranjan Bose and Hari Menon, "India's Great Healthcare Challenge, Also an Opportunity," Hindustan Times, updated 7 June, 2017, https://www.hindustantimes.com/india-news/ india-s-great-healthcare-challenge-and-opportunity/story-eB691Pj889x57TYo8MobaM.html.
10. Ibid.
11. Prabha Raghavan and Divya Rajagopal, "Healthcare's Dilemma: Balancing Public Needs with Business Sense," The Economic Times, updated 30 November, 2017, https://economictimes.indiatimes.com/ industry/healthcare/biotech/pharmaceuticals/healthcares-dilemma-balancing-public-needs-with- business-sense/articleshow/61855883.cms.
12.Nayan Kalnad, Niranjan Bose and Hari Menon, "India—a Distinctive Healthcare Landscape," The Tincture Collective, Medium, 8 November, 2016, https://tincture.io/india-a-distinctive-healthcare-landscape- bb3d5b1c2452.
13.Kalnad, Bose and Menon, "India's Great Healthcare Challenge."
14.Manu Gupta, "Accreditation: India's Journey Towards Quality of Care," IHP, 22 September, 2017, http://www.internationalhealthpolicies.org/accreditation-indias-journey-towards-quality-of-care/.
Other sources:
Indrani Gupta and Mrigesh Bhatia, "The Indian Health Care System," International Health Care System Profiles, accessed 18 February, 2018, http://international.commonwealthfund.org/countries/india/.
John LaMattina, "India's Solution to Drug Costs: Ignore Patents and Control Prices—Except for Home Grown Drugs," Forbes, 8 April, 2013, https://www.forbes.com/sites/johnlamattina/2013/04/08/indias-solution- to-drug-costs-ignore-patents-and-control-prices-except-for-home-grown-drugs/#410354832cba.
J.S. Thakur, Shankar Prinja, Charu C. Carg, Shanthi Mendis and Nata Menabde, "Social and Economic Implications of Noncommunicable Diseases in India," Indian Journal of Community Medicine, December 2011, 36(Suppl1): S13–S22: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3354895/.
Manu Gupta, "Accreditation: India's Journey Towards Quality of Care," IHP, 22 September, 2017, http://www.internationalhealthpolicies.org/accreditation-indias-journey-towards-quality-of-care/.
The World Bank Human Development Network, The Growing Danger of Non-Communicable Diseases, Conference Edition, vii (September 2011). http://siteresources.worldbank.org/HEALTHNUTRITIONAND POPULATION/Resources/Peer-Reviewed-Publications/WBDeepeningCrisis.pdf.
Parijat Ghosh and Satyam Mehra are partners in Bain & Company's New Delhi office and leaders in Bain India's Healthcare practice. Arunava Saha Dalal is a principal in Bain India's Healthcare practice.
Copyright© 2018 Bain & Company, Inc. All rights reserved.
Net Promoter®, Net Promoter System®, Net Promoter Score® and NPS® are registered trademarks of Bain & Company, Inc., Fred Reichheld and Satmetrix Systems, Inc.
Repeatable Models® is a trademark of Bain & Company, Inc.







