Report

Executive summary
In the two years since we last surveyed physicians working on the front line of European healthcare, their discontent has risen to an alarming level. Many say they would not recommend their hospital as a place to work or to receive care. Physicians and surgeons also have grown increasingly dissatisfied with pharma companies and medtech manufacturers over the past two years.
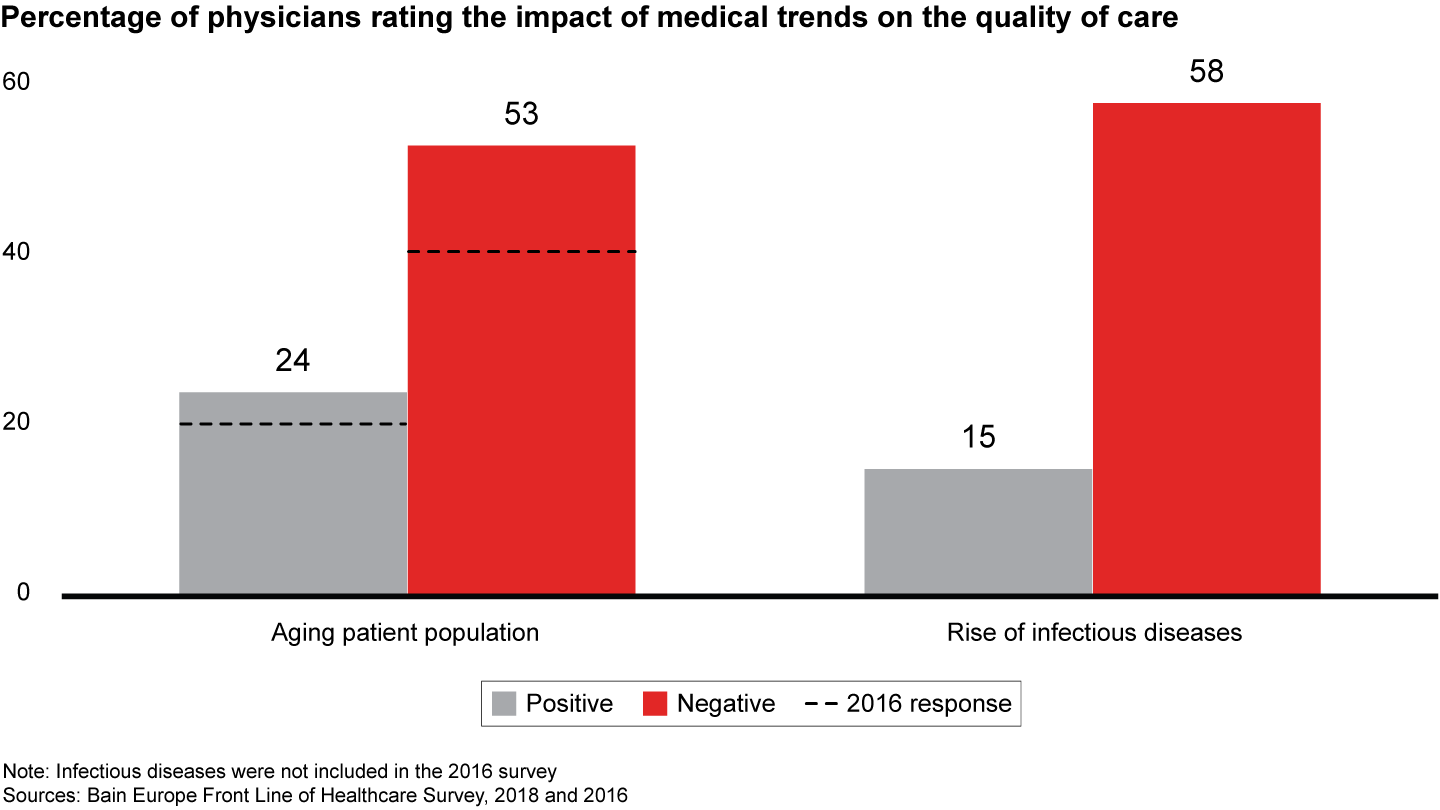
Citing staffing shortages, budget cuts, aging equipment and inadequate facilities, physicians warn they are unprepared to cope with looming healthcare challenges, including aging populations and the reemergence of infectious diseases (see Figure 1). In addition to inadequate resources, physicians also cite a lack of unbiased information, which impedes sound decision making. More than 70% say they are dissatisfied with the information pharma and medtech companies provide.

Our 2018 Europe Front Line of Healthcare Survey reveals an industry in dire need of change, but lacking a clear way forward. Hospitals, pharma companies and medtech manufacturers continue to rely on an outdated model of care delivery that is operating under increasing strain. Few have begun to fundamentally rethink care delivery and engage physicians in that process.
The swing in physicians’ attitudes from bad to worse is striking. Two years ago, though unsatisfied with the status quo, most physicians were broadly optimistic that new structures, systems and digital tools eventually would help them deliver better care at lower cost in the future. In 2018, that vision remains a distant goal. Despite high expectations of change, healthcare organizations across Europe have been reluctant to embrace new approaches to care delivery and the digital technologies that enable them.
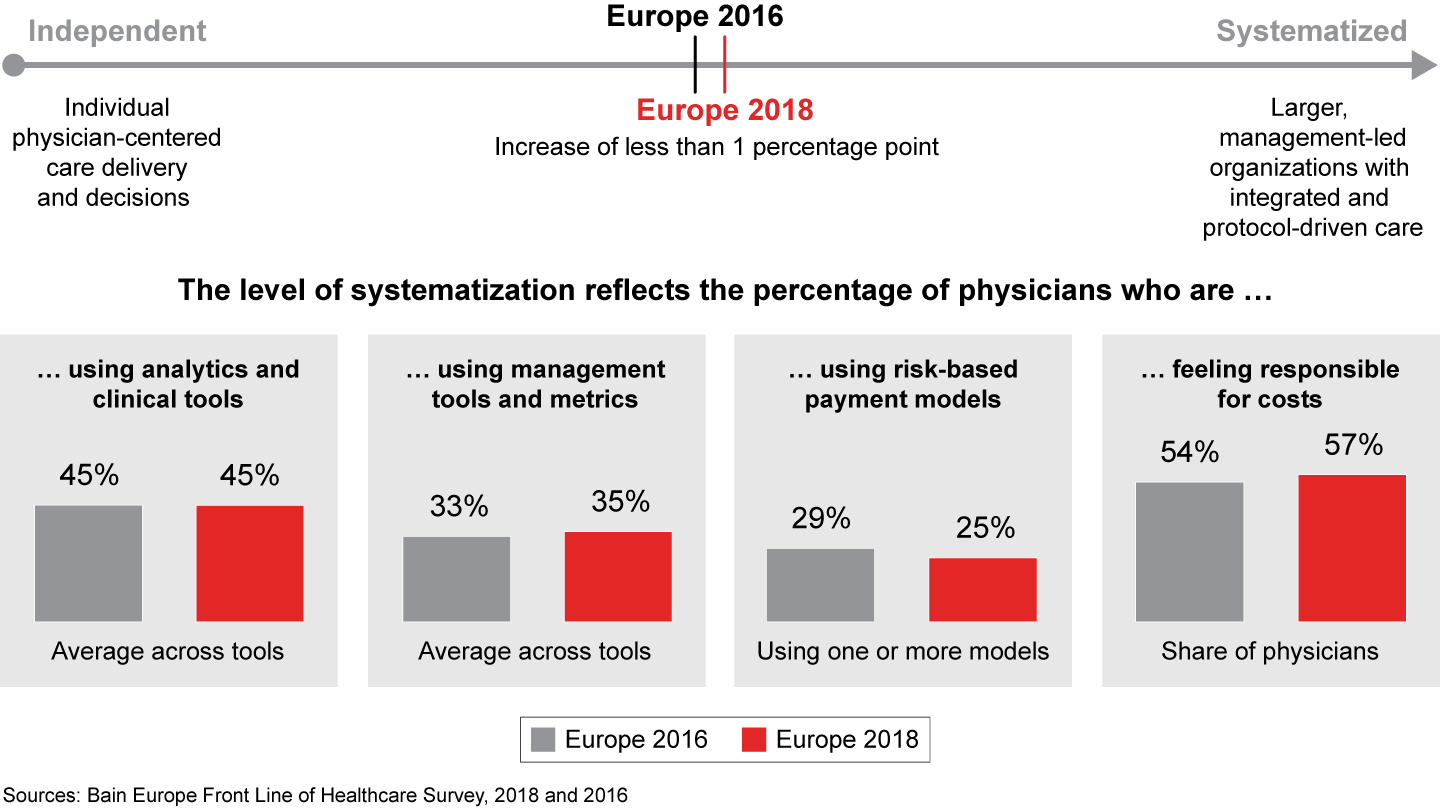
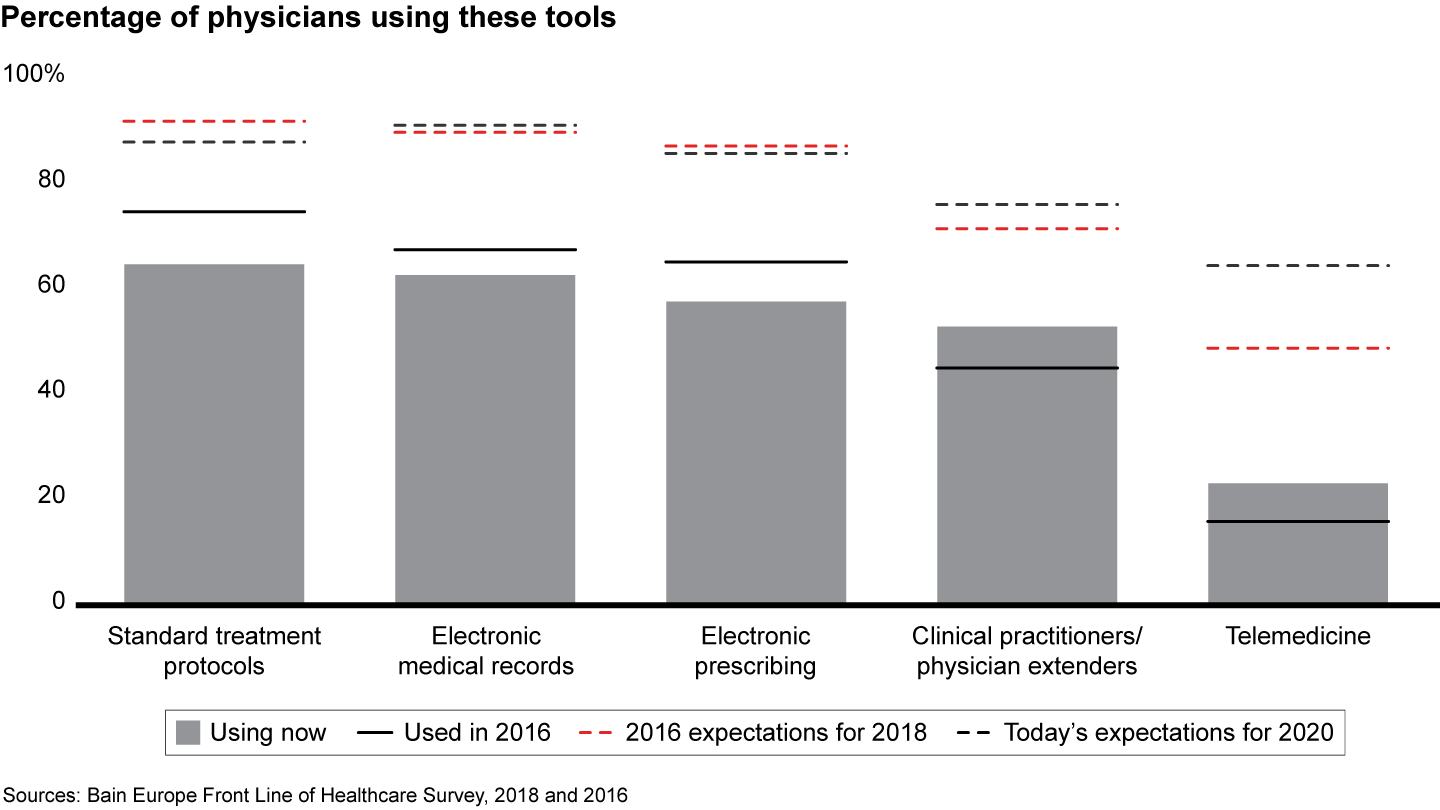
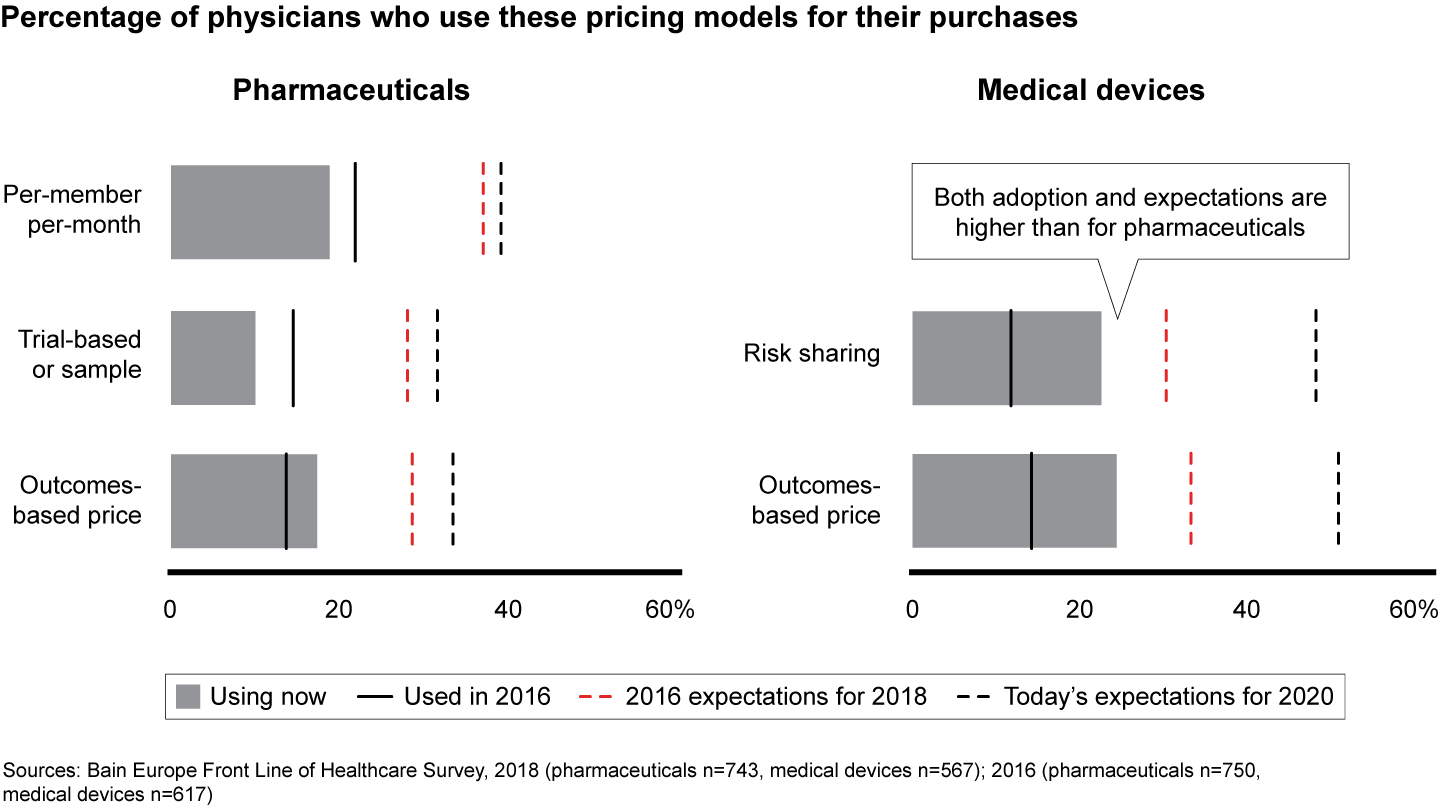
Our research shows that the pace of change in Europe has stalled (see Figures 2 to 4). The leap in adoption of clinical tools such as electronic medical records that physicians anticipated two years ago, for example, has not materialized, and few institutions have embraced new management or payment models. Physicians’ use of analytics and clinical tools remained flat at 45% over the past two years, and the use of risk-based payment models actually declined.



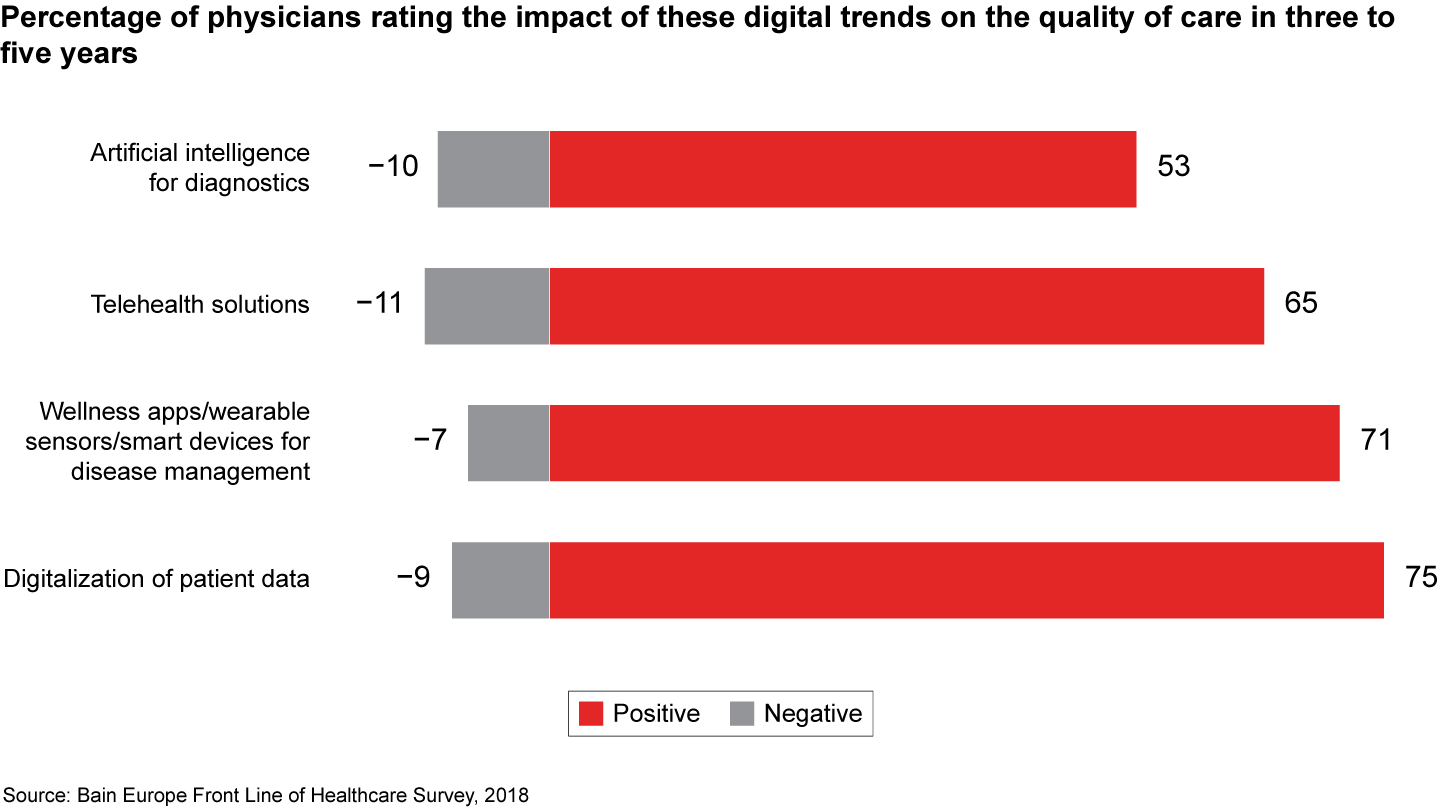
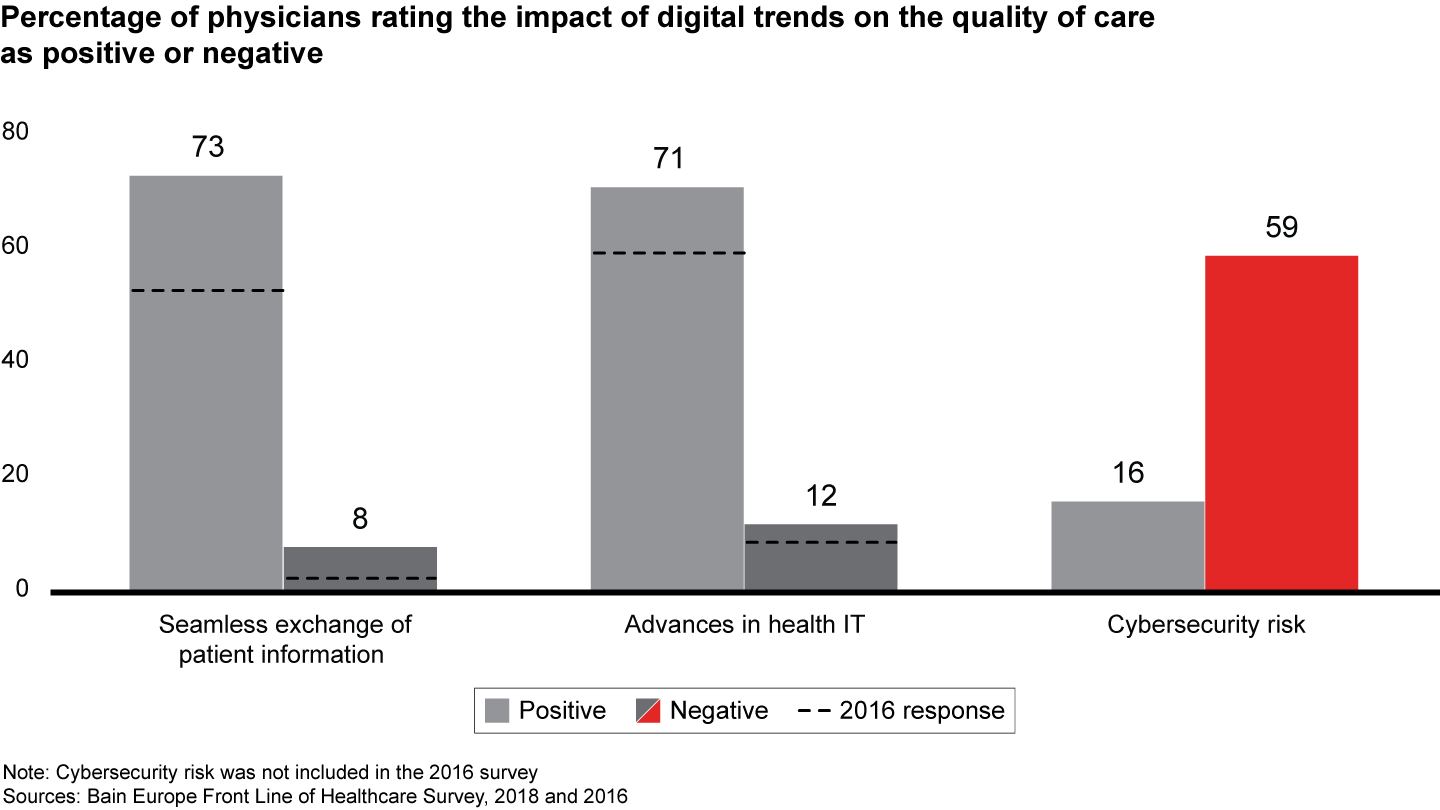
Though progress on many fronts has stalled, more than 75% of physicians believe that the digitalization of patient data could help them improve the quality of care in the next three to five years, as long as new systems ensure that information is secure. Cybersecurity risks, however, remain a major obstacle to rapid change (see Figures 5 and 6).


High levels of physician discontent will have consequences for all businesses in Europe’s healthcare ecosystem. Any company that has seen dissatisfaction of its front line spike is in trouble. The same goes for those whose services and products generate negative customer ratings. That’s the situation confronting many of Europe’s healthcare providers, pharmaceutical companies and medtech manufacturers.
The aim of Bain’s Front Line of Healthcare Survey is to provide leadership teams with data, insights and analysis that can help them better manage their businesses through a period of pivotal change for the industry. To understand physicians’ evolving reality, our survey tracks European practitioners’ attitudes, priorities and decision-making power. The findings are based on input from 1,156 physicians across nine specialties and 154 hospital procurement administrators in Germany, France, the UK and Italy. The 2018 survey highlights national differences in healthcare systems across the four European countries we studied.

The European Healthcare Landscape by the Numbers
A look at the impact of the shifting healthcare landscape in Europe on physicians, medtech and pharma.
Implications for providers
Physicians’ warnings about adverse working conditions have become the norm in Europe rather than the exception. The root cause of the problem is clear: healthcare systems in Germany, France, the UK and Italy are among the most expensive in the world and costs are steadily rising. Providers are struggling to bring costs down and improve patient outcomes, but they are falling far short of that goal.
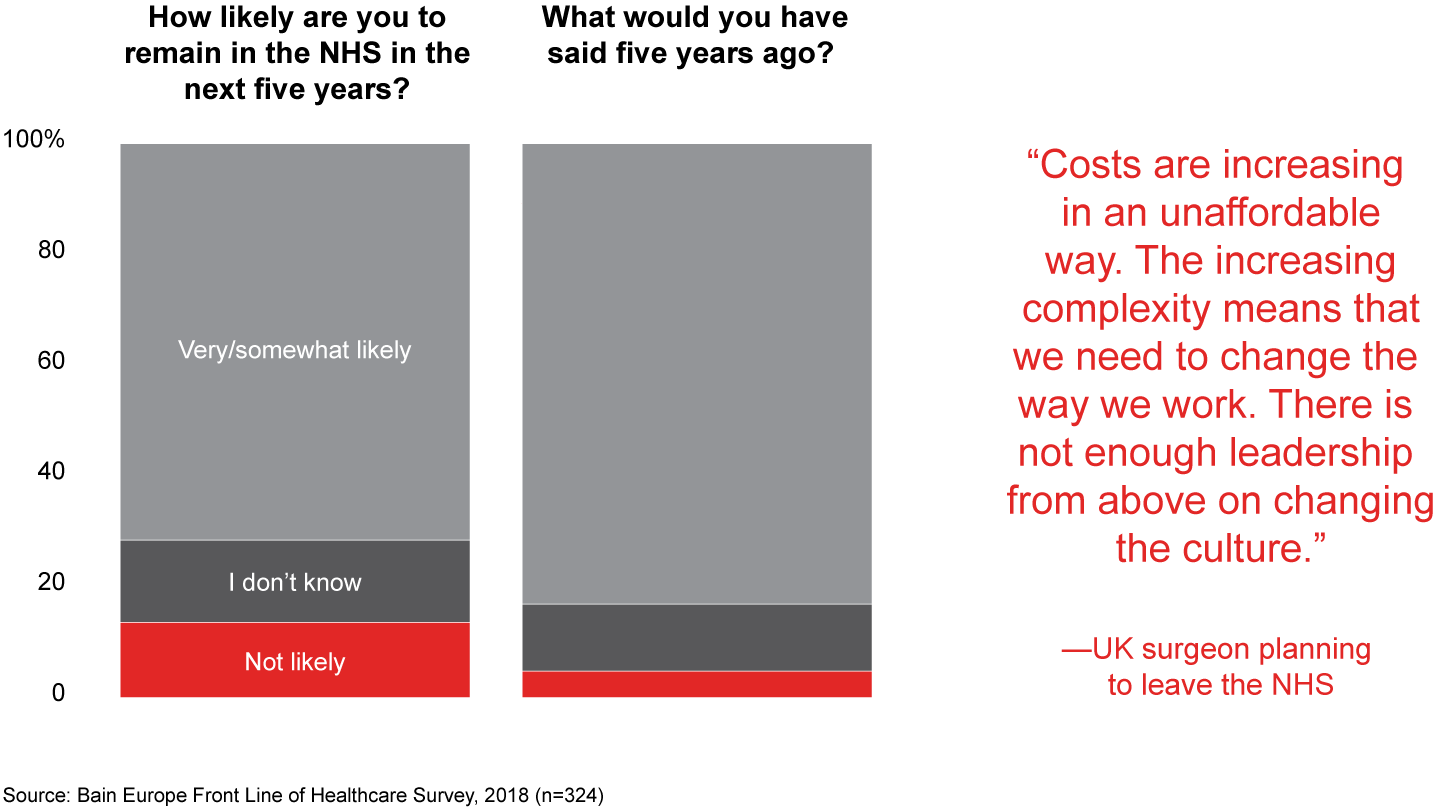
Our findings reveal unsustainable levels of physician discontent. Doctors are extremely dissatisfied, not only with hospital working conditions, including poor management and organization, but with the quality of care that hospitals deliver and the quality of physician training. The front line has put providers on notice that patient care is at risk—and doing nothing is no longer an option. The number of UK physicians saying they are not likely to remain in the country’s National Health Service in the next five years, for example, has more than doubled to 14%. In Germany, one physician reflected a common concern by reporting, “Current budget restrictions are increasingly limiting our ability to work well.”

A Call to Action for Europe's Hospitals
Rising discontent among doctors signals the need for change.
Physicians’ growing discontent goes beyond workplace conditions: it signals a growing risk to patient care. The responses varied from country to country, but 20% to 35% of respondents in Germany, Italy and the UK are unwilling to recommend their hospitals to friends and family, with German hospitals receiving the most negative rating. German physicians note that cost pressures have resulted in nursing cuts in some hospitals, forcing already overstretched physicians to take on roles that nurses previously handled in intensive care.
A 2017 report by the Organization for Economic Cooperation and Development (OECD) underscores the need for urgent change. In high-income countries, one in 10 patients is adversely affected during treatment, according to the report, and around 15% of hospital expenditure in high-income countries is due to mistakes in care or patients being infected while in the hospital.
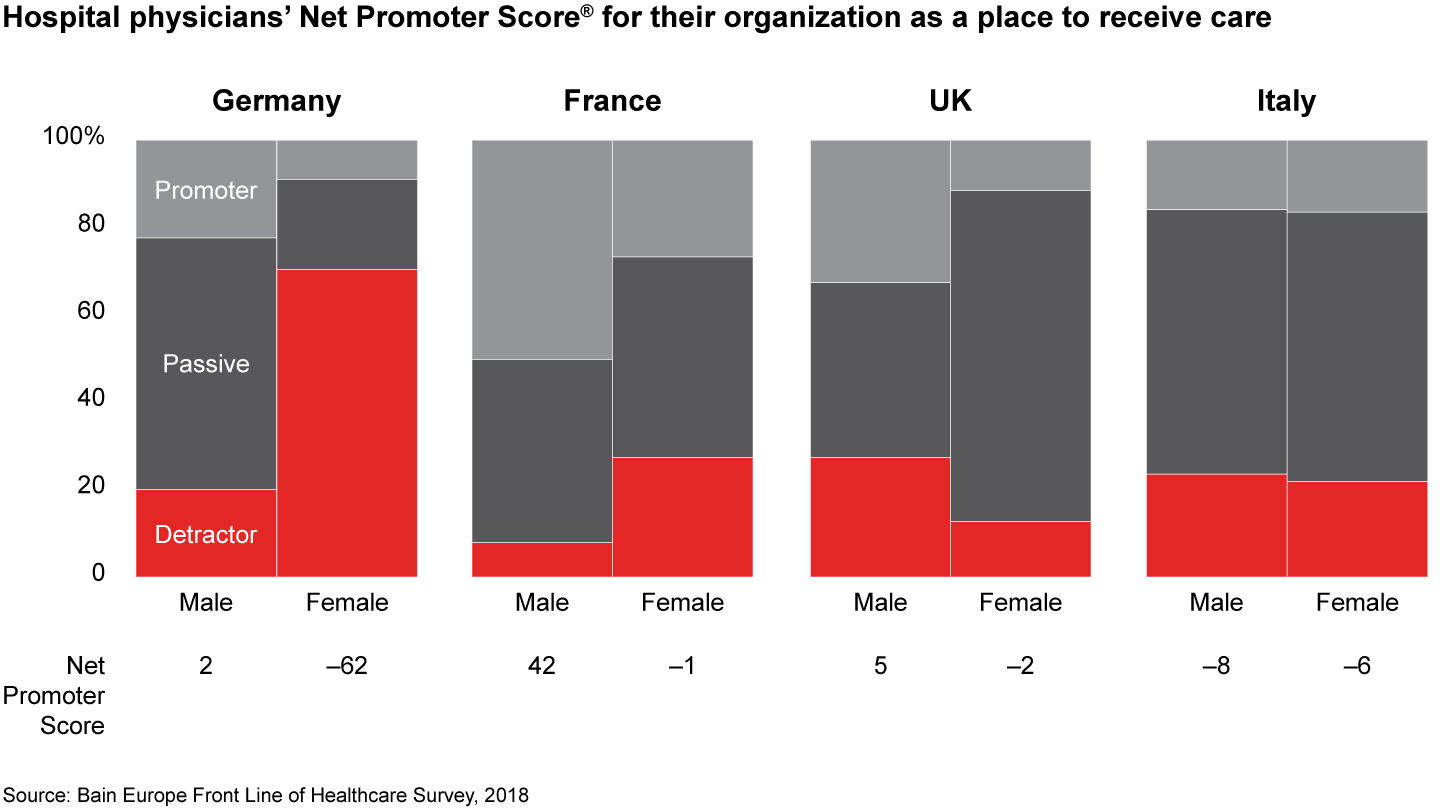
Dissatisfaction among female physicians with their hospitals as a place to work or receive care is far more pronounced than among male colleagues, and the gap is alarmingly wide in Germany. More than 70% of female physicians working in German hospitals would not recommend their hospital as a place to receive care, compared with about 20% of male colleagues.
Loïc Plantevin, who leads Bain's Healthcare practice in Europe, the Middle East and Africa, explains how the European healthcare industry can benefit from a redesign of care delivery models and a demonstration of new sources of economic and medical value.
Physicians who say they would not recommend their hospital to family or friends cite quality of care and clinical outcomes as the main reasons. One pointed to “a worrying frequency of complications.” Physicians who are dissatisfied with their institution as a place to work complain about insufficient resources, poor organization and poor management.
For providers, the survey findings are an urgent call to action to take bolder steps redesigning healthcare delivery. They also highlight an opportunity. Providers that seek new ways to deliver high-quality care at lower cost will be better positioned as the industry evolves to address 21st century needs. Three initiatives can help hospitals and other healthcare providers begin to reverse negative attitudes and lay the foundations for change: modernize management structures, engage physicians in rethinking care delivery and improve talent management.
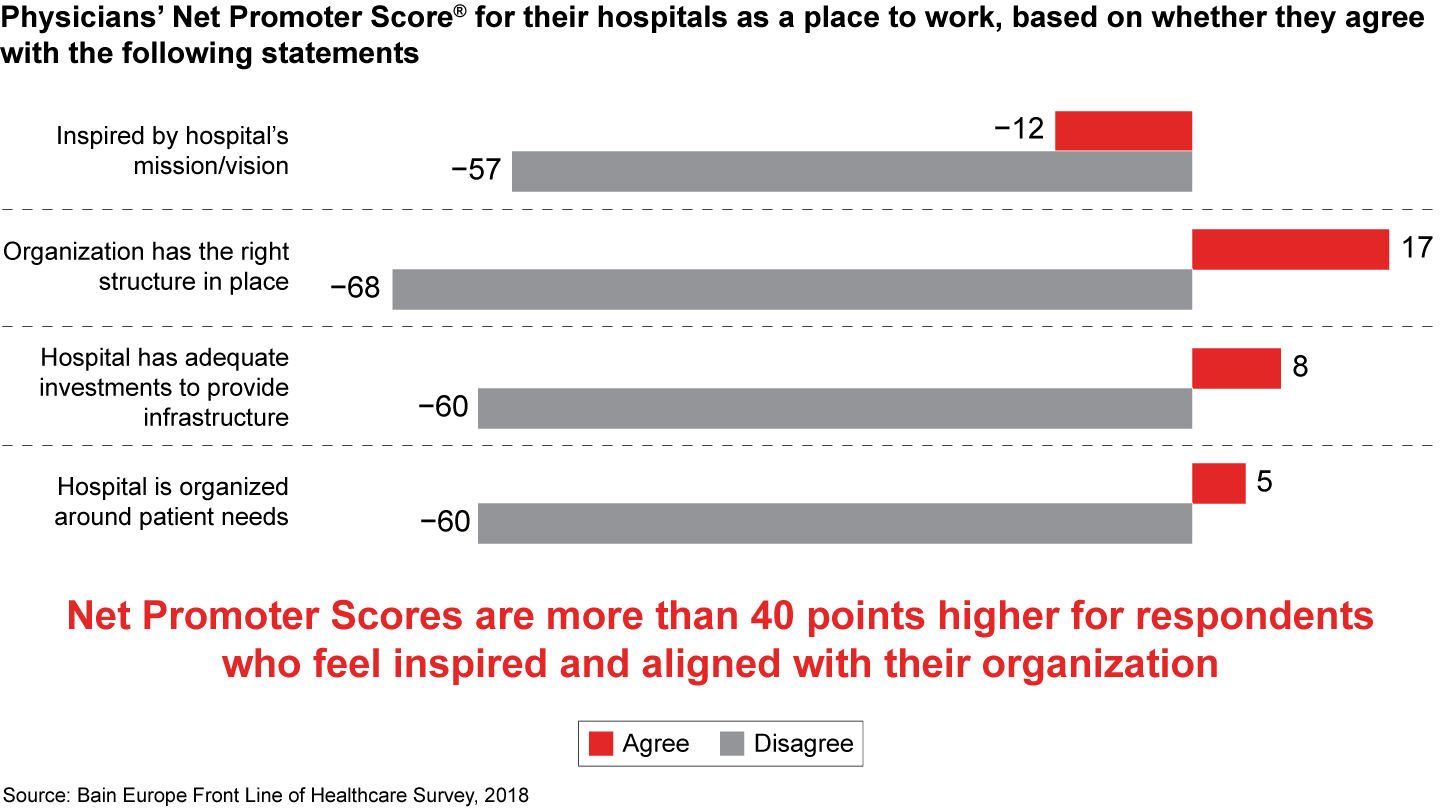
Bain research shows organizations with engaged and inspired employees are far more productive. Specifically, our Front Line of Healthcare Surveys show providers that invest in creating alignment around their mission and put the right organizational structures in place to fulfill it have significantly higher physician advocacy.
Some French hospitals have started down that path. Since mid-2016, 79 French providers have been participating in a government pilot program to promote greater dialogue between healthcare administrators and caregivers, with the goal of improving working concerns and patient care. While our survey did not examine this program, France is the only country in our 2018 survey to show a sharp improvement in physician satisfaction with their hospitals as a place to work and to receive care.
Similarly, our 2017 US Front Line of Healthcare Survey highlighted the importance of engaging physicians in the quest for new healthcare models. Physicians told us they were open to new cost-saving models, but needed to participate in the change to help identify which approaches create value for patients and which don’t.
Healthcare organizations that ignore the warning signals from the front line will increase the likelihood of disruptive change. Soaring healthcare costs and eroding quality of care already have encouraged nontraditional companies such as Amazon to enter the field with disruptive new care-delivery models. Mayo Clinic Health System CEO John Noseworthy summed up the challenge the industry faces as the institution began investing $1.5 billion in a new electronic medical-record system: “Everything is going to have to change, from the way insurance companies run, to how medicine is practiced, the way life science companies work, [and] the way pharmacy benefit managers work.”
Implications for pharma
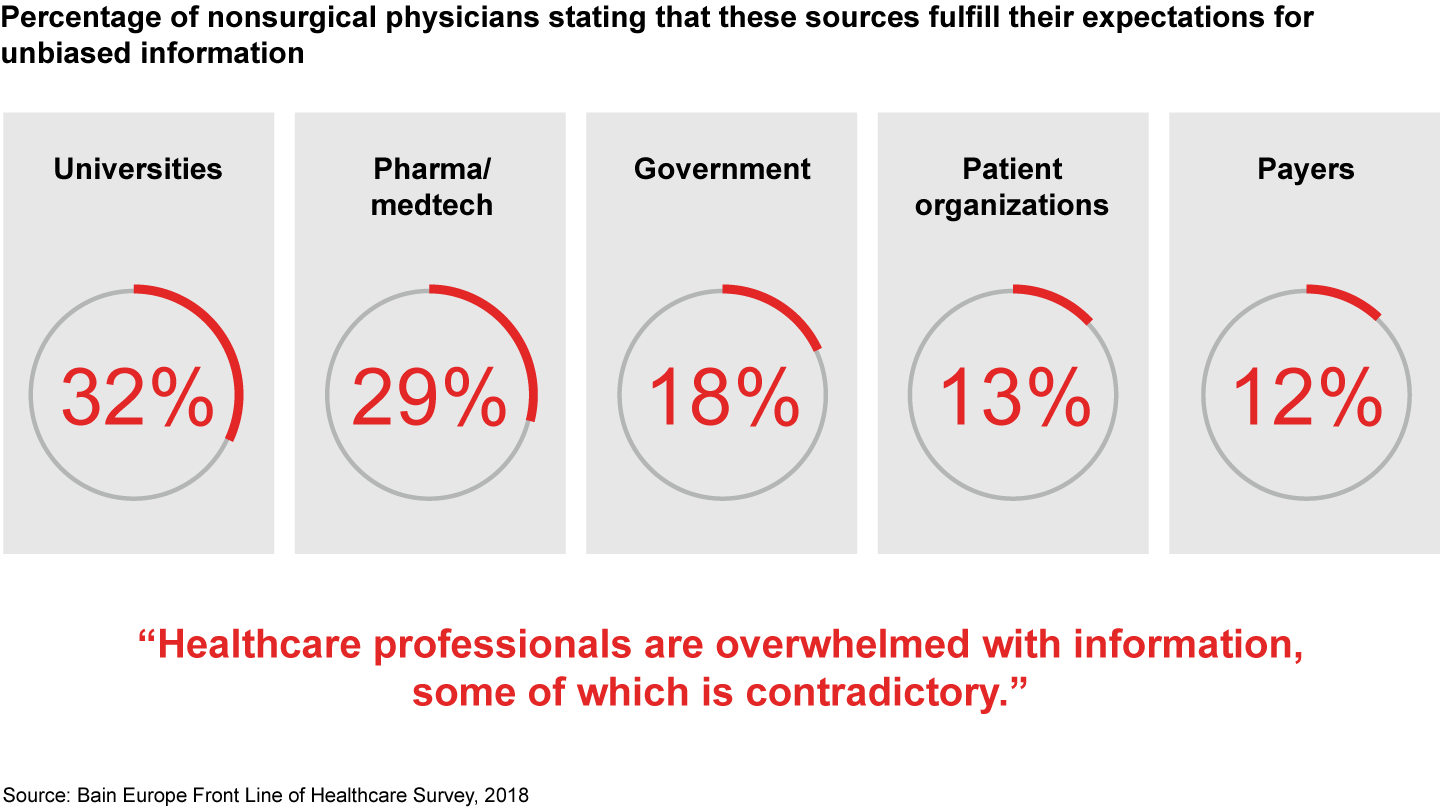
In our 2018 survey, physicians again affirmed the critical role that high-quality data plays in helping them take the most appropriate treatment decisions. An overwhelming majority of physicians say they are dissatisfied with all sources of information available to them, be it from payers, patient organizations, government agencies, pharma and medtech companies or universities. More than 70% say pharma companies did not fulfill their expectation in providing unbiased scientific information—and few expect them to improve. That finding highlights a significant opportunity for improvement among pharma companies.
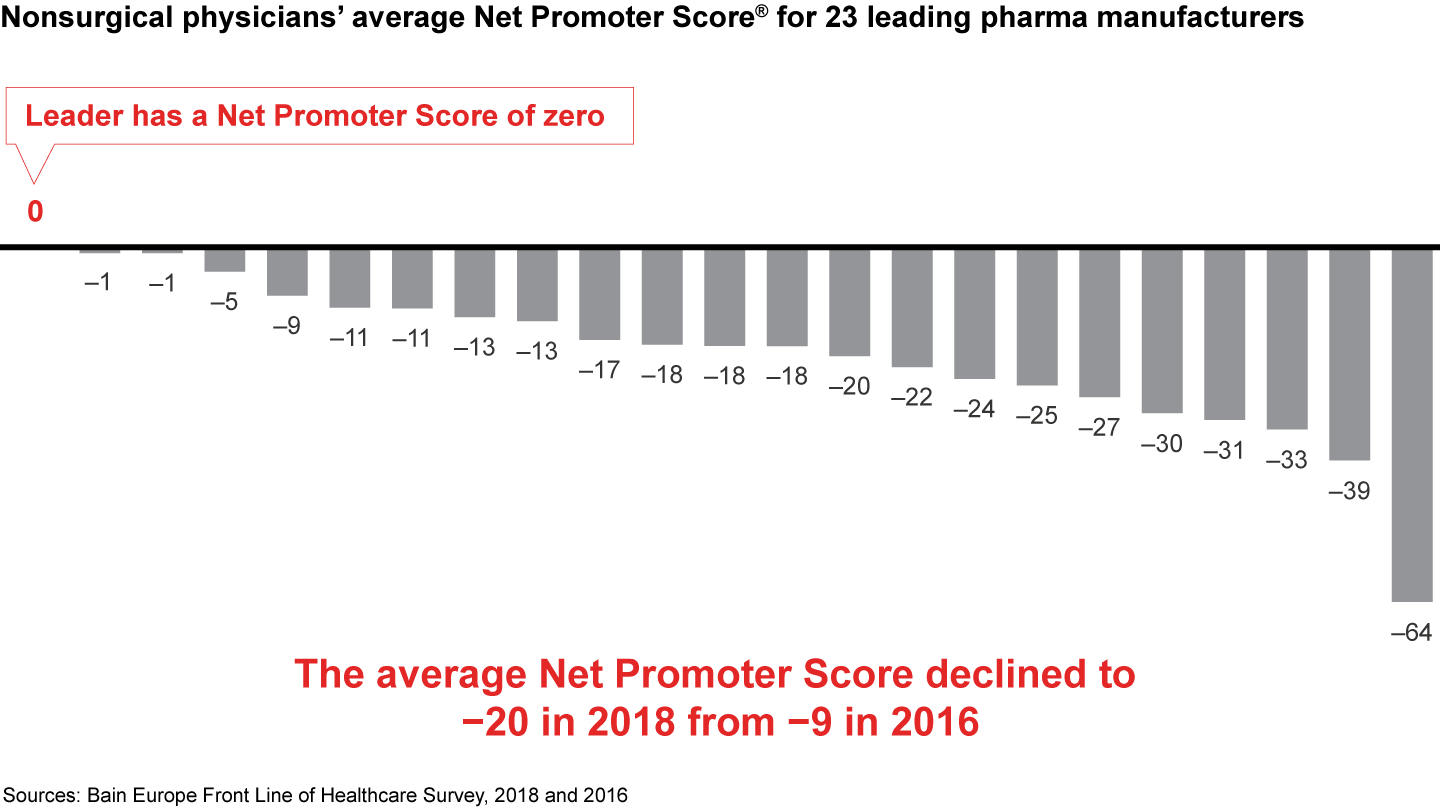
Physicians’ overall satisfaction in their interactions with pharma manufacturers also declined over the past two years, highlighting a need to improve customer points of contact and service. Our findings show the average Net Promoter Score®, a key measure of customer loyalty and satisfaction, for 23 leading pharma manufacturers fell to negative 20 in 2018, from negative 9 in 2016 (see the appendix for an explanation of Net Promoter Scores). The key reasons physicians cite for disappointment in their interactions with pharma companies included poor support and communication. Twenty percent say pharma companies they worked with had no clear point of contact.

European Physicians' Pharma Frustration
How drug companies can combat doctors' growing discontent.
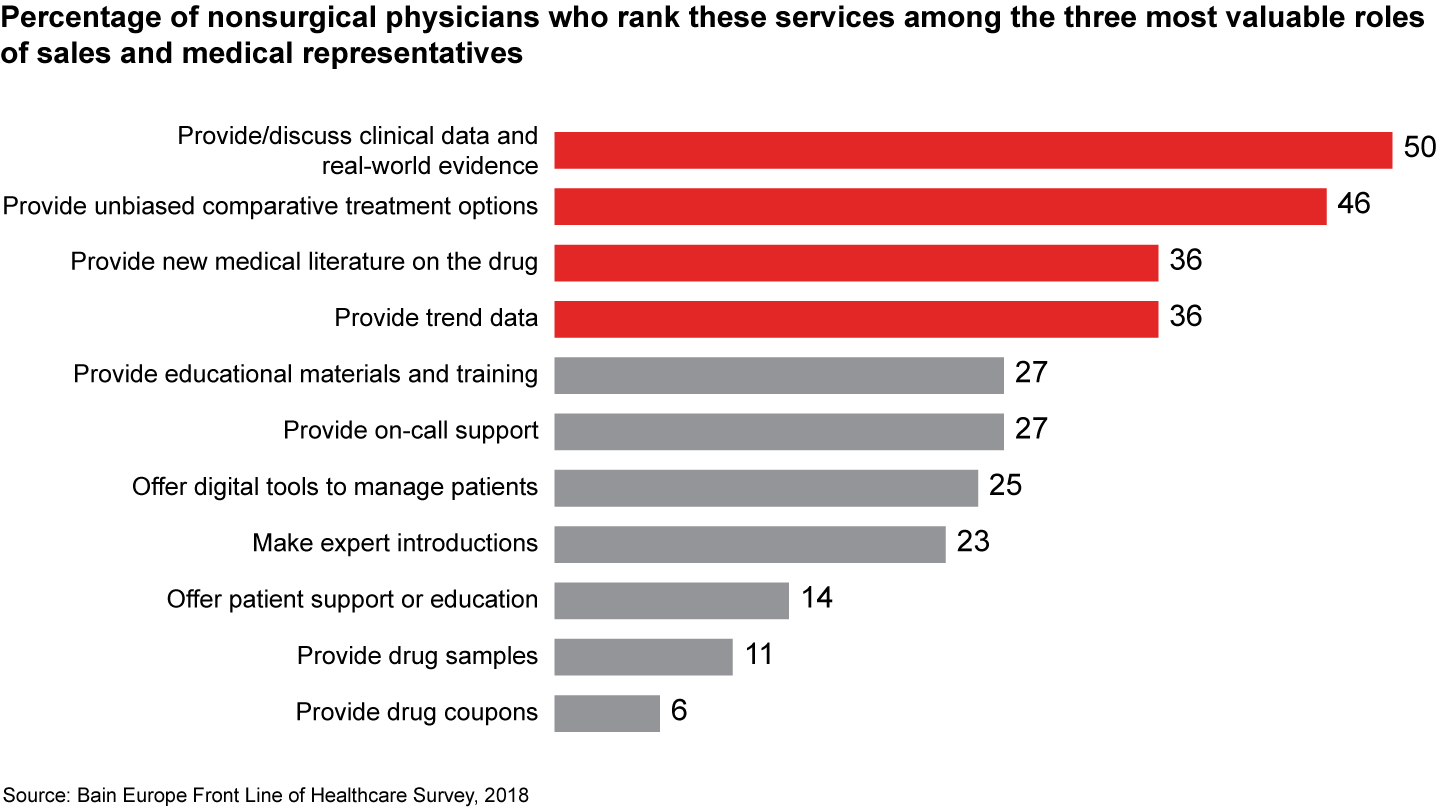
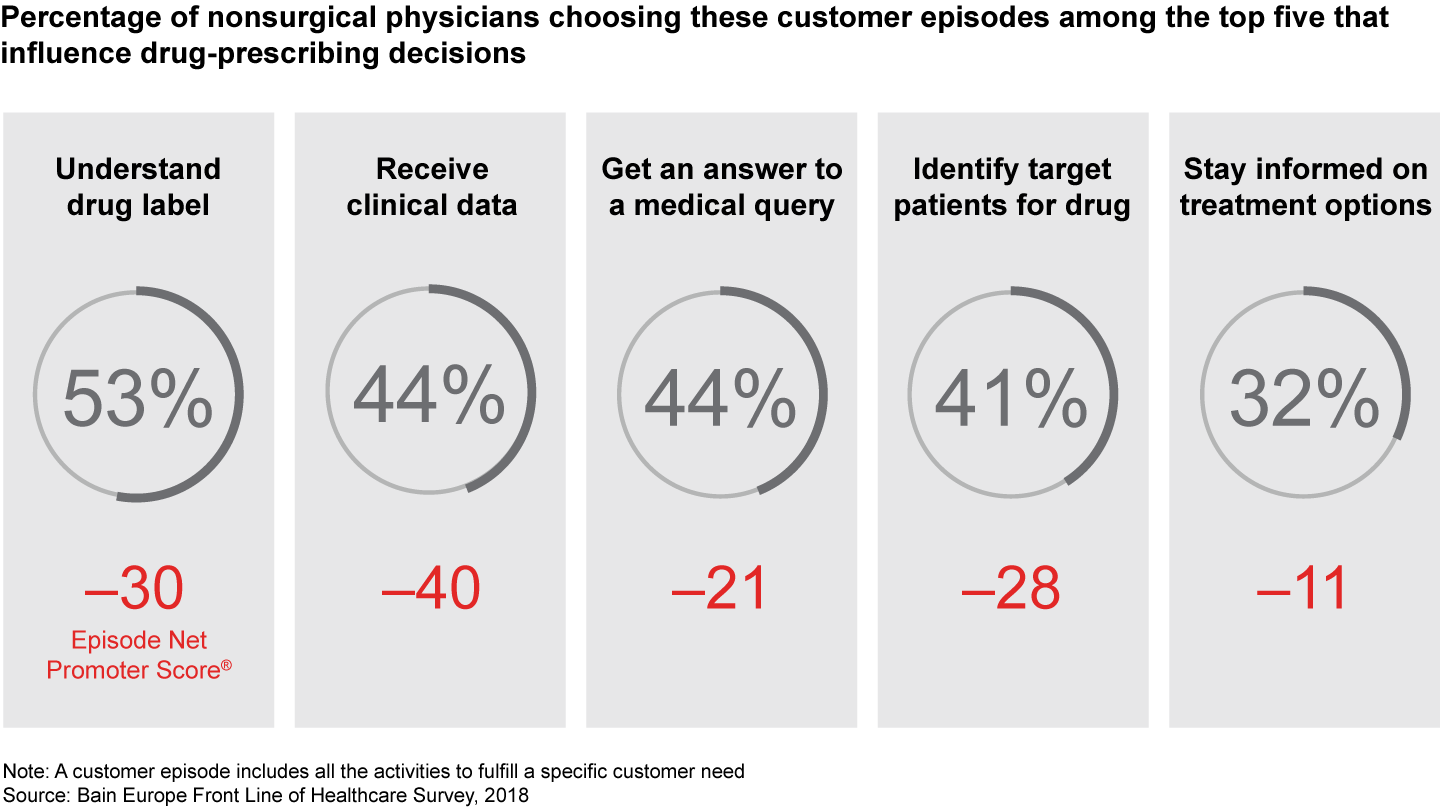
As information about new pharmaceutical products grows increasingly complex, companies need to become more adept at communicating complex data. In particular, physicians evaluating new drugs want unbiased scientific information such as clinical trial data, real-world evidence and comparative treatment options.
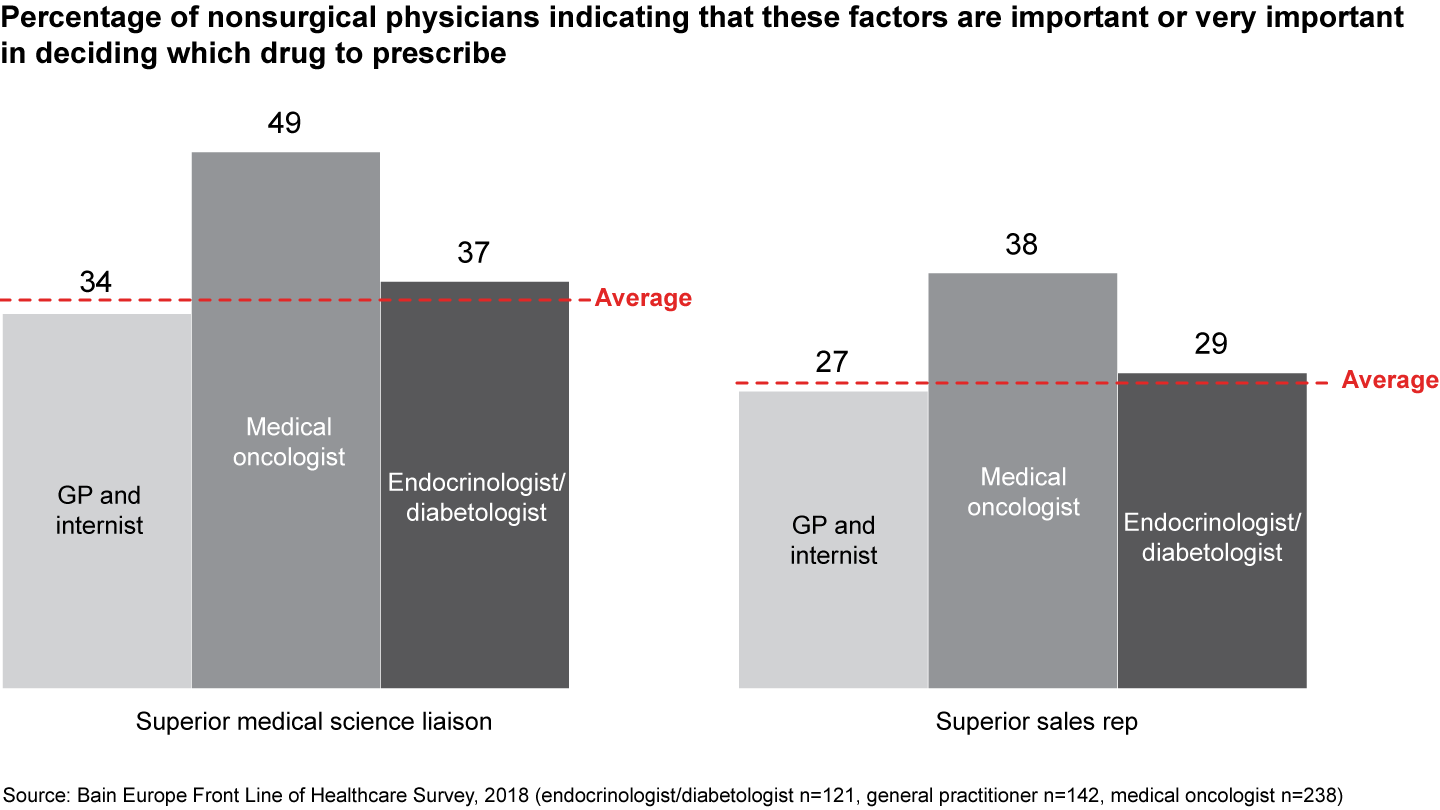
That trend helps explain the growing importance of the role of medical science liaisons as a source of information. For prescribing drugs, 35% of physicians say information from medical science liaisons played an important or very important role, compared with 28% for sales representatives. Since medical science liaisons are a limited resource, pharma manufacturers can also improve customer focus by making better use of multiple new digital channels to disseminate data to physicians efficiently.
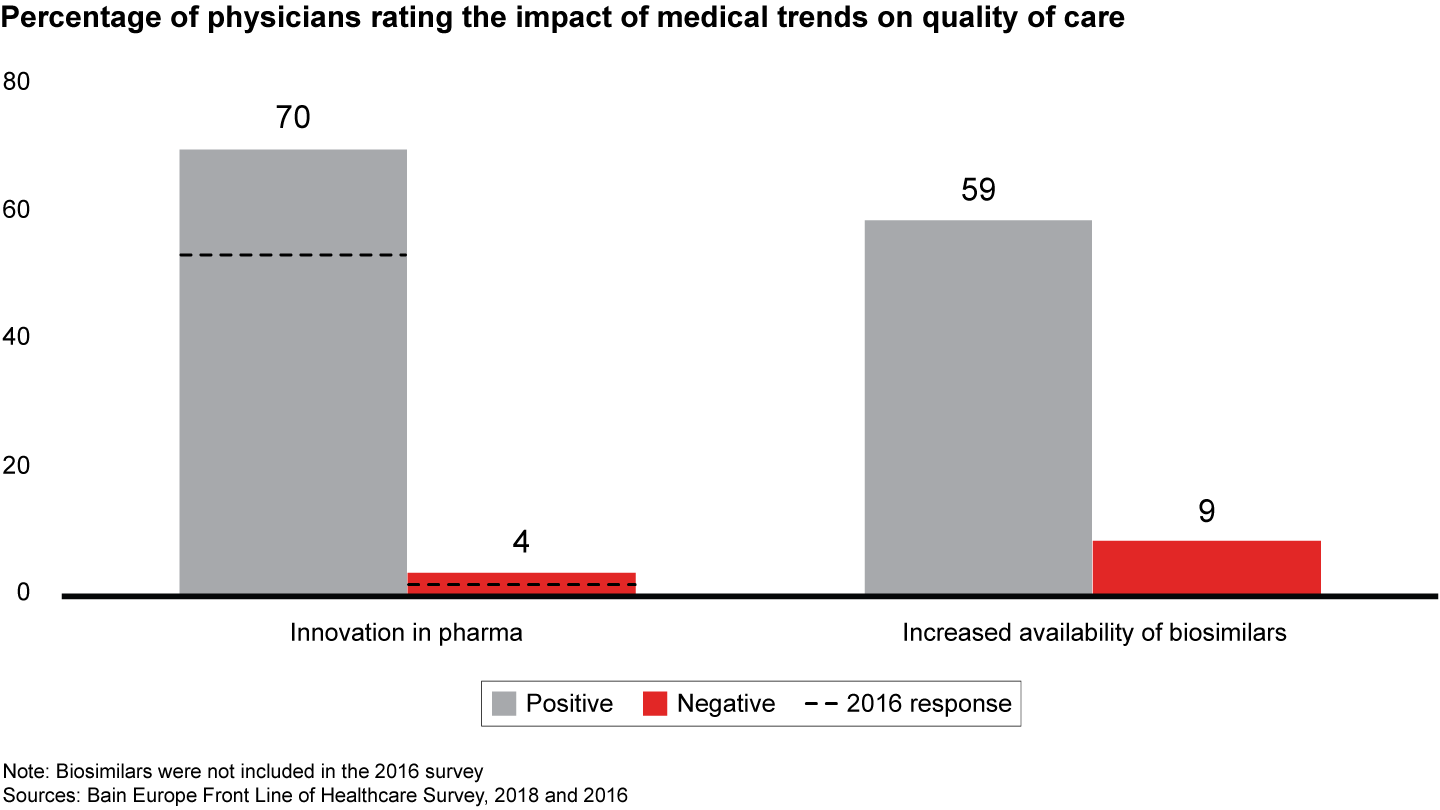
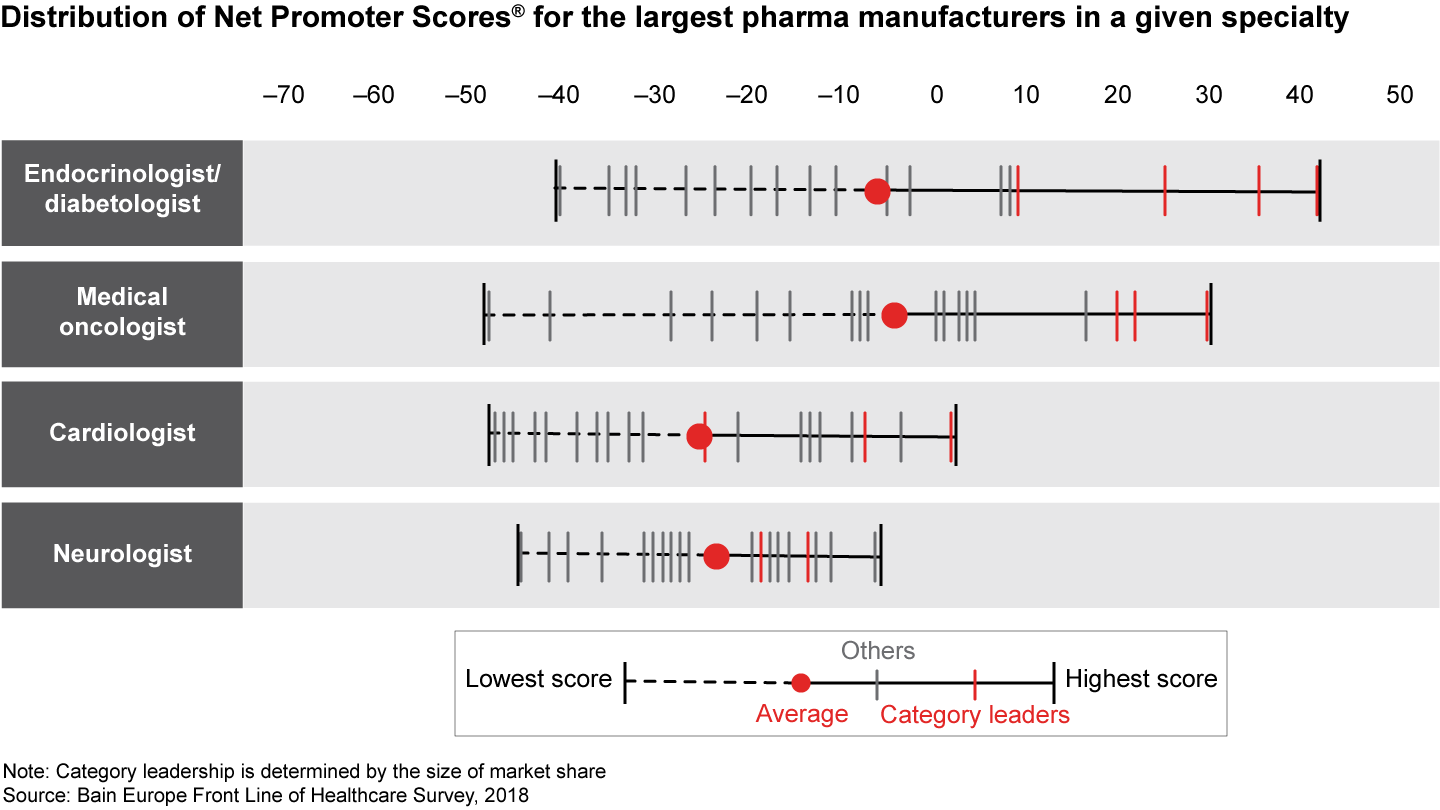
Our findings showed physicians continue to see pharma innovation as part of the solution, and they view category leaders in a much more positive light than the industry as a whole. Seventy percent of physicians expect pharma innovation to contribute to high-quality care in the future, and 59% of them say the increased availability of biosimilar drugs improved the quality of care. In our 2018 survey, physicians consistently recommend category leaders above other players, and give category leaders more positive (or less negative) Net Promoter Scores than their peers.
Pharma manufacturers face increasing demand for proof of the value of their products. The winners in the coming decade will be those that can demonstrate new and meaningful sources of medical and economic value. Leadership teams can start taking immediate steps to provide physicians with real-world evidence that highlights the benefits of their products compared with those on the market. In the long term, a strategic focus on category leadership can help position pharma companies to become a more trusted partner to physicians.
Implications for medtech
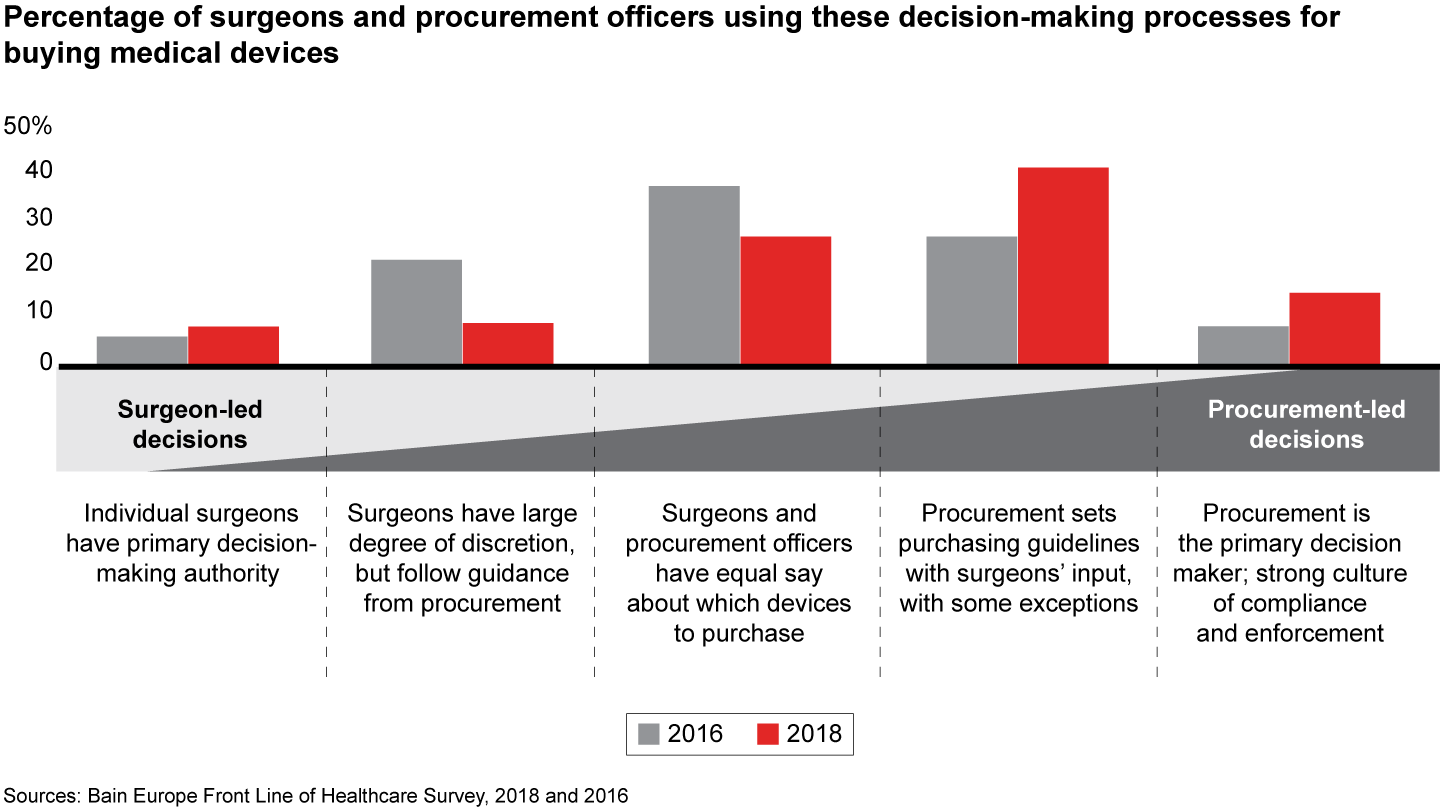
As hospitals and healthcare organizations strive to reduce costs, procurement managers are playing a growing role in decisions to purchase medical equipment. Centralized purchasing decisions in which procurement officers are the primary decision maker have doubled over the past two years. Nearly 60% of physicians report that purchasing decisions for medical equipment are predominantly led by procurement officers, with some physician input. Only 17% of surgeons say they have a large degree of discretion over purchasing. About 25% report the two stakeholders have equal say.
The challenge for medtech manufacturers in this changing environment is addressing the different needs and preferences of both surgeons and procurement officers. In fact, our 2018 survey highlighted a growing dissatisfaction of both physicians and procurement officers with medtech manufacturers.

A Balancing Act for Medtech in Europe
As purchasing power shifts, device makers need to rethink their customer focus.
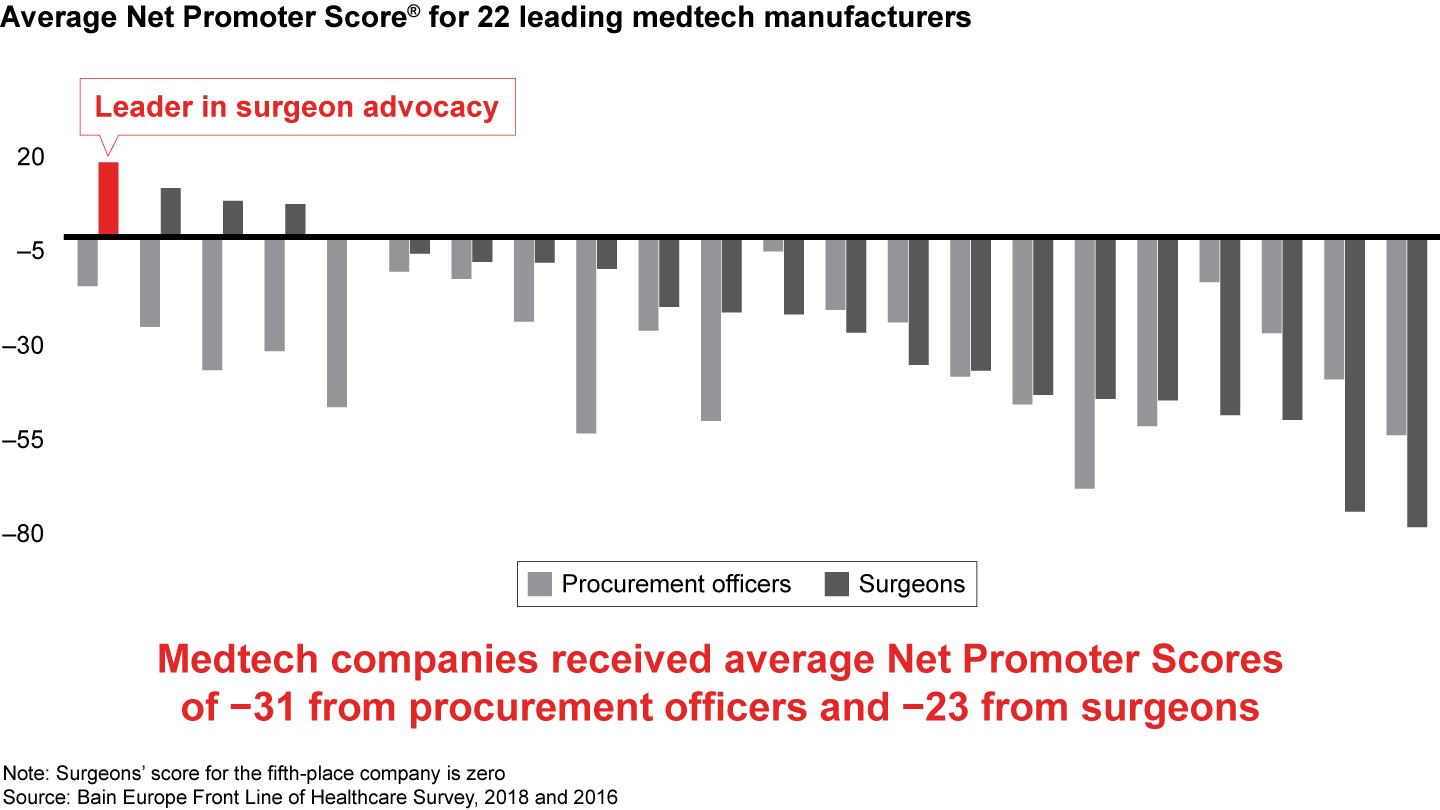
Surgeons gave medtech companies an average Net Promoter Score of negative 23, down from negative 14 in 2016. Procurement officers gave medtech companies a score of negative 31, compared with 1 in 2016.
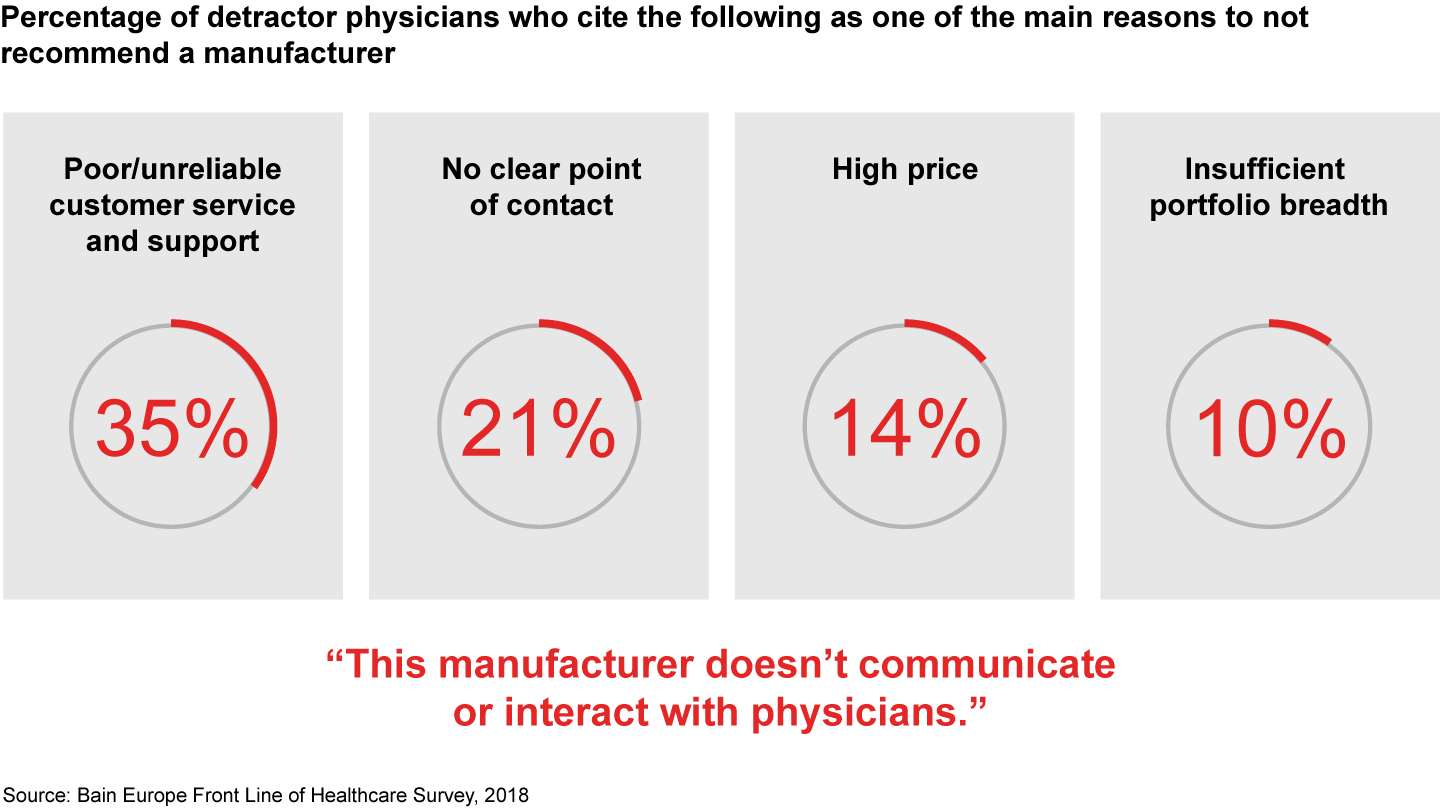
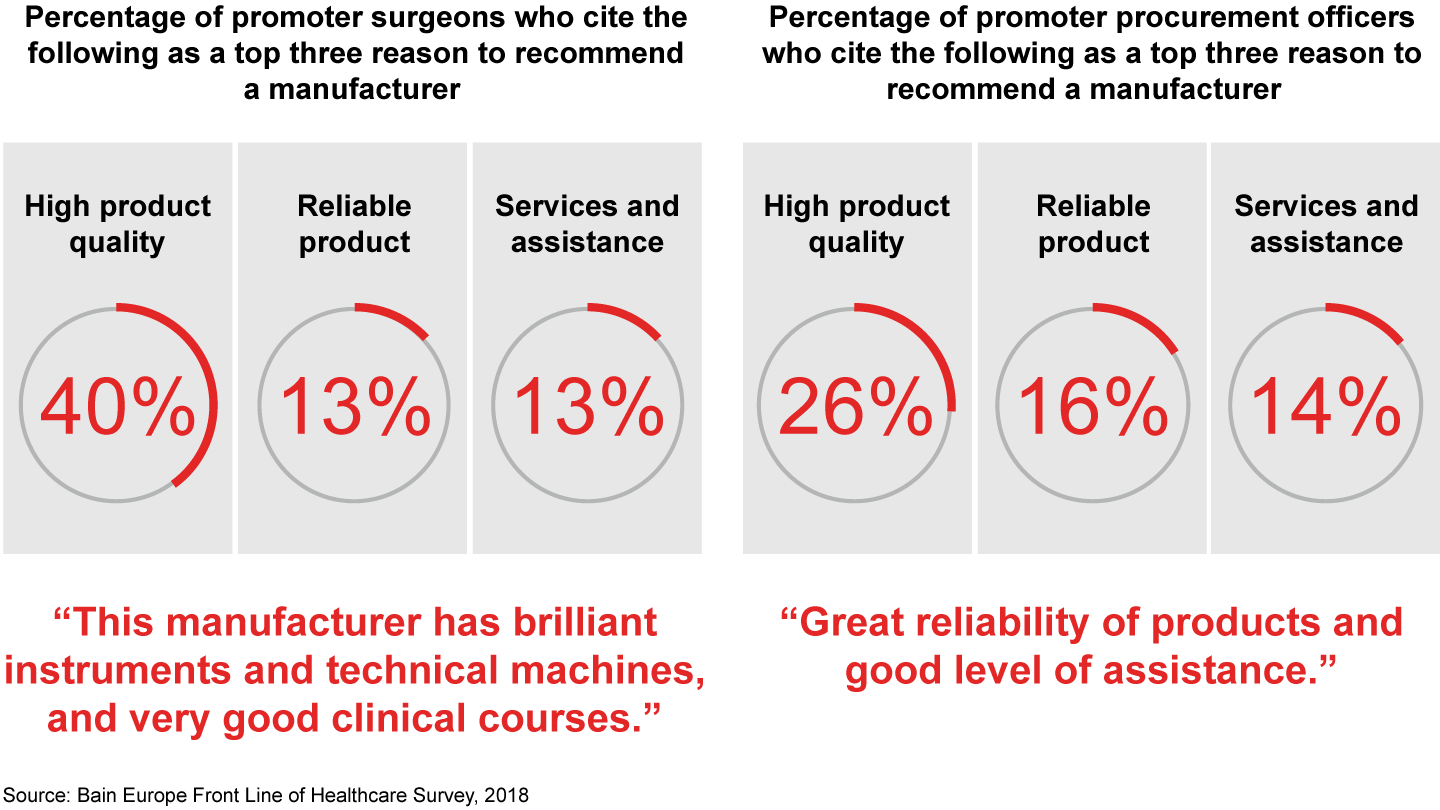
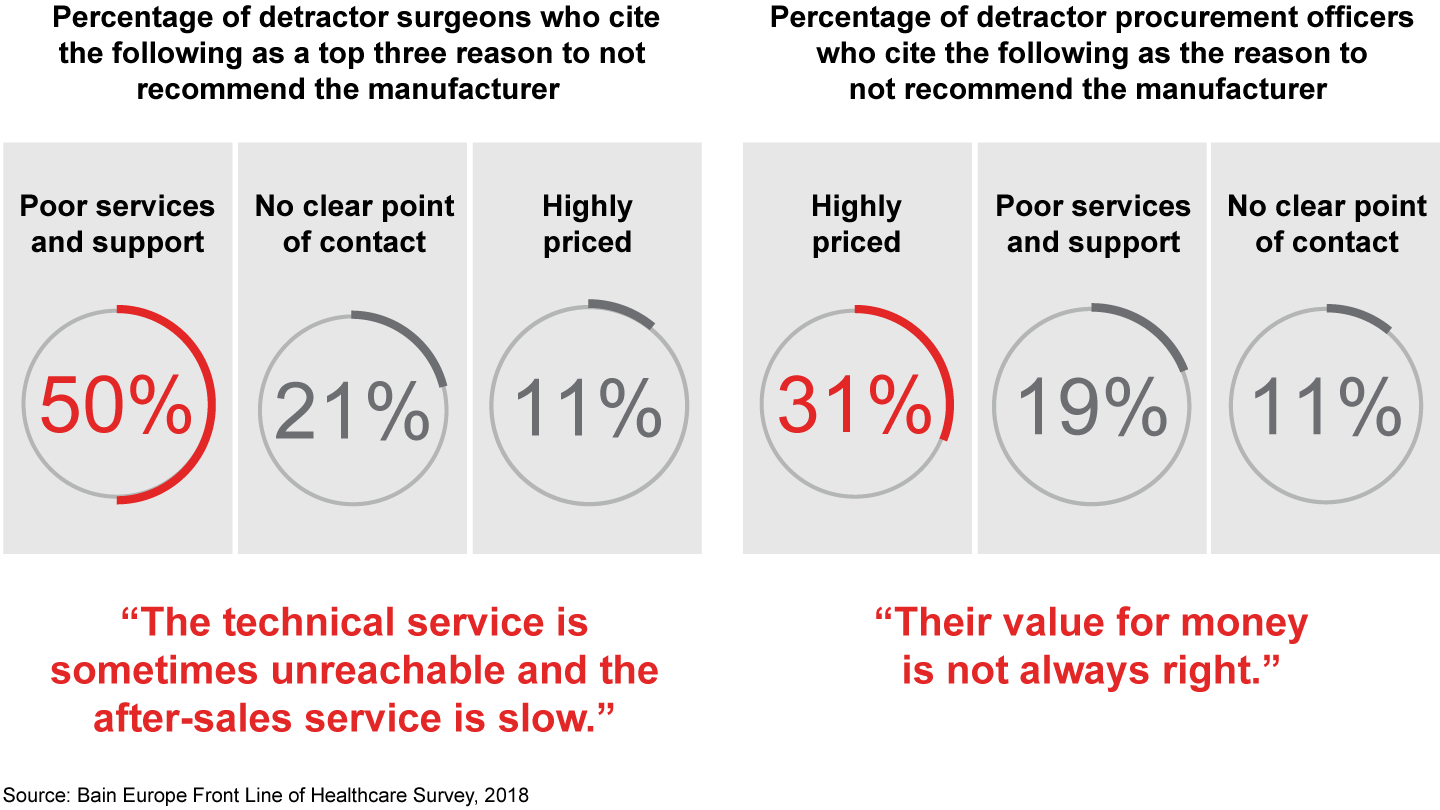
While surgeons and procurement officers both value high-quality products, reliability and service, the key reason for low advocacy differ for these two groups of medtech stakeholders. Surgeons rate poor service and support as their main cause of dissatisfaction. Only 11% of dissatisfied surgeons cite high prices as a reason for not recommending a manufacturer. By contrast, the main reason procurement officers would not recommend a manufacturer is the price of its equipment.
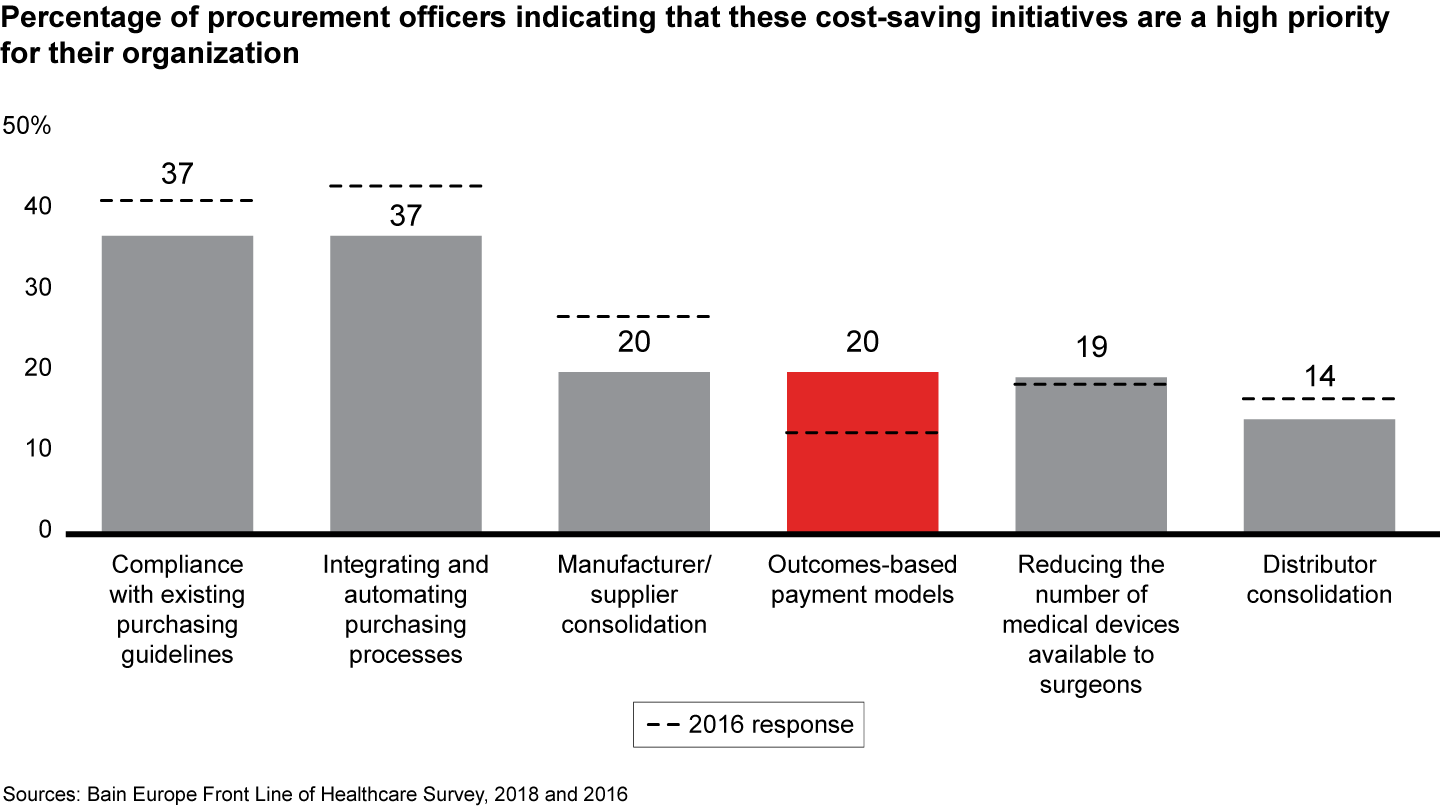
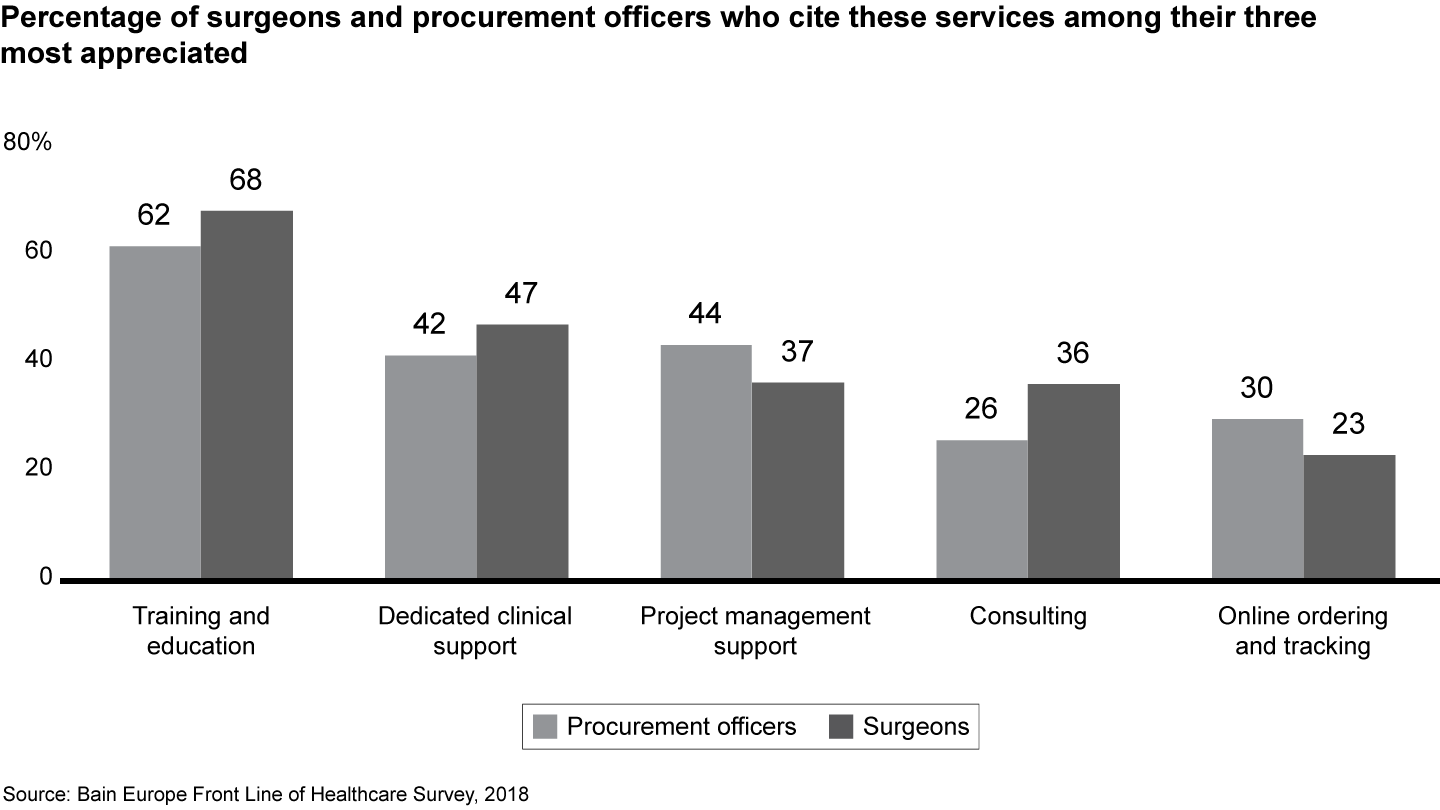
Medical technology companies can adapt to this changing landscape by better understanding what these two sets of customers value most. Understanding the needs and preferences of surgeons and procurement officers will improve their interactions with both. For procurement officers, total cost of ownership is a far more important purchasing criterion. They value project management support, automated purchasing processes and outcomes-based payment models. Surgeons place a higher value on clinical support and consulting. Companies that build on customer knowledge and commercial success to become category leaders will be best positioned to deliver value to a diverse set of stakeholders.
The way forward
Change is overdue. That is the key message of our 2018 Front Line of Healthcare Survey. Alarming levels of physician discontent describe a care-delivery model that has lost its ability to evolve. In fact, the pace of change is stalling as physicians struggle to live up to the changing needs and rising demands of patients and other stakeholders.
While our report shows that providers as well as pharma and medtech manufacturers all have many opportunities to start improving the situation incrementally, the shift to better and more sustainable care will require a more holistic approach to care delivery. Leaders in every sector of the healthcare industry will need the courage to disrupt and redesign today’s structures and systems, leveraging digital innovation. Broader collaboration can help the industry achieve high-quality outcomes.

How Engaged Physicians Can Help Usher In a New Era in the UK
Bain’s 2018 UK Front Line of Healthcare Survey reveals the National Health Service is at a crossroads.
1. Providers
- The satisfaction of physicians working in hospitals declined on average in 2018, as physicians grappled with staffing shortages, budget cuts, aging equipment and inadequate facilities.
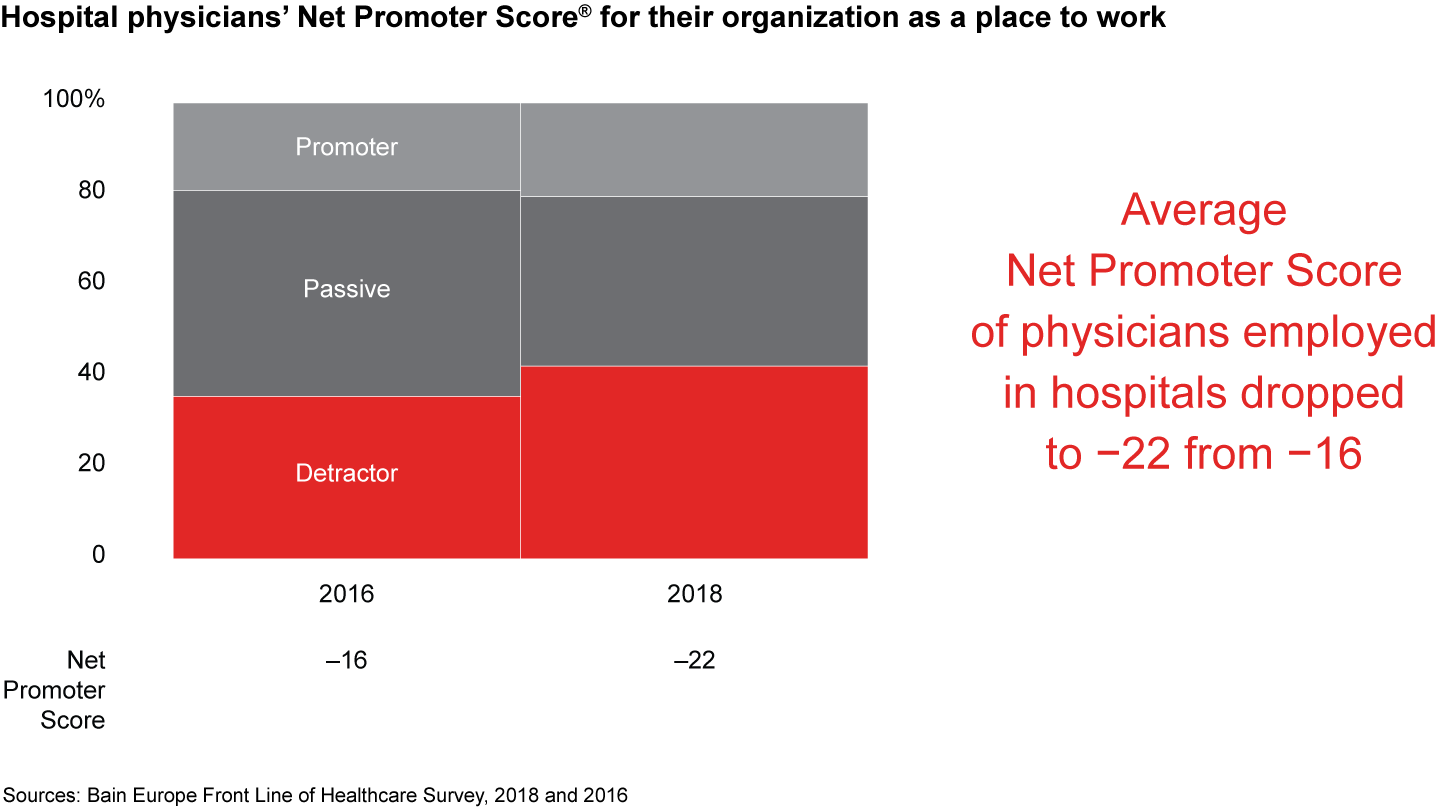
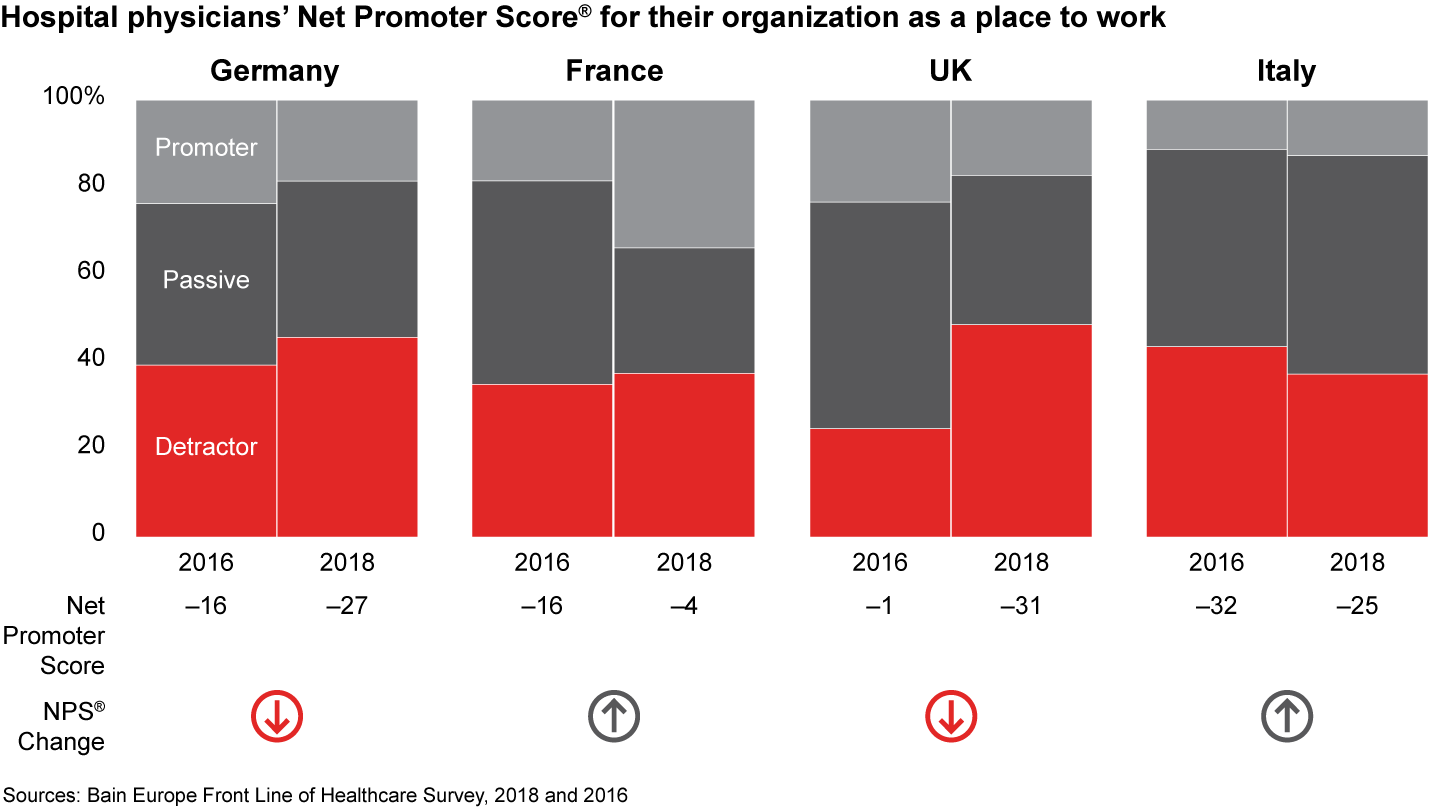
- The overall Net Promoter Score for hospitals as a place to work dropped to negative 22 from negative 16 in 2016. The Net Promoter Scores for German and UK hospitals declined significantly; the score of French hospitals improved, but the average was still a negative 4. The number of UK hospital physicians likely to leave the National Health Service in the next five years more than doubled.
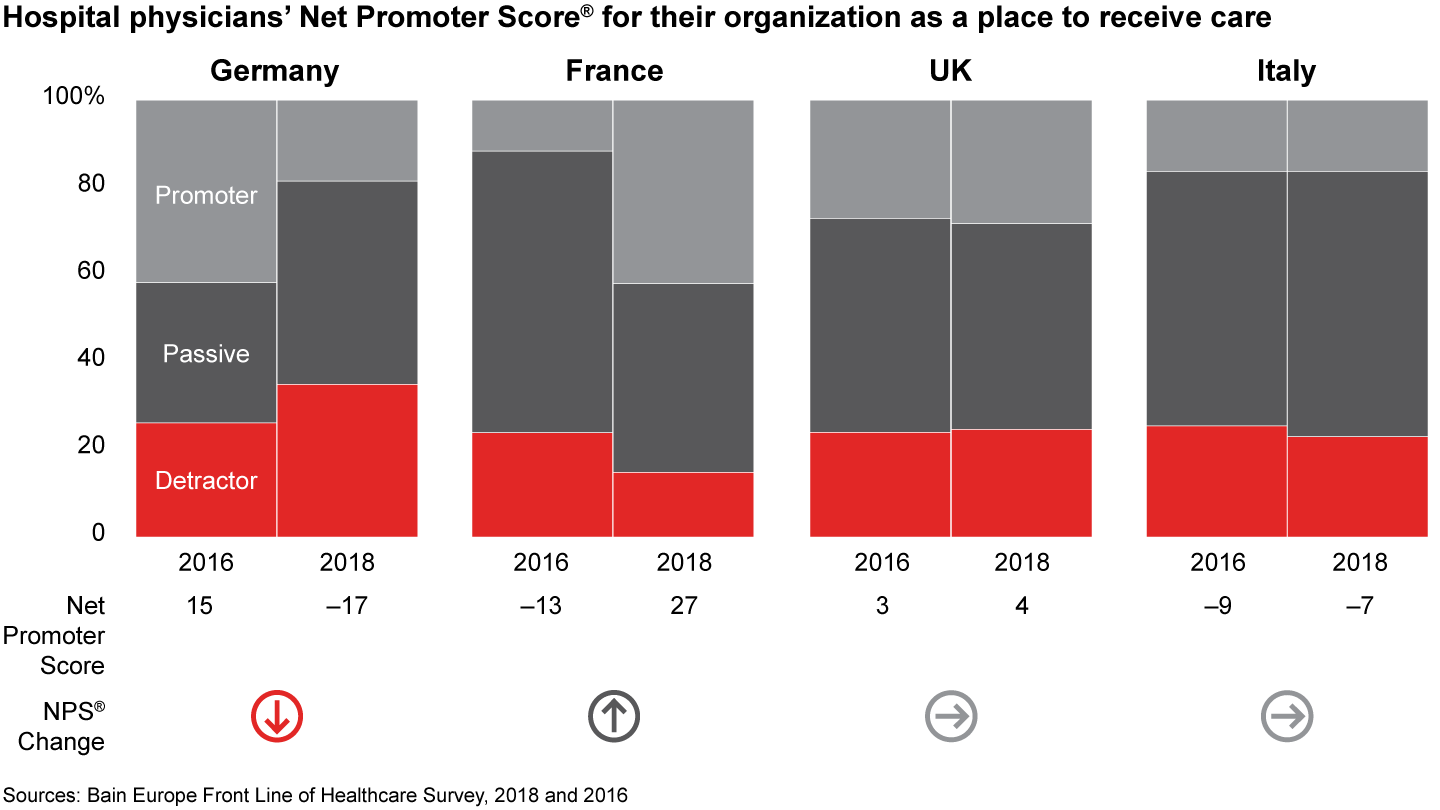
- Physicians’ growing discontent goes beyond workplace conditions—it highlights a growing risk to patient care. Thirty-five percent of German physicians and about 20% of physicians in the UK and Italy say they would not recommend their hospitals to family and friends as a place to receive care. French hospitals’ Net Promoter Scores as a place to receive care was 27, up from negative 13 in 2016—the only country to show a sharp improvement over the past two years.
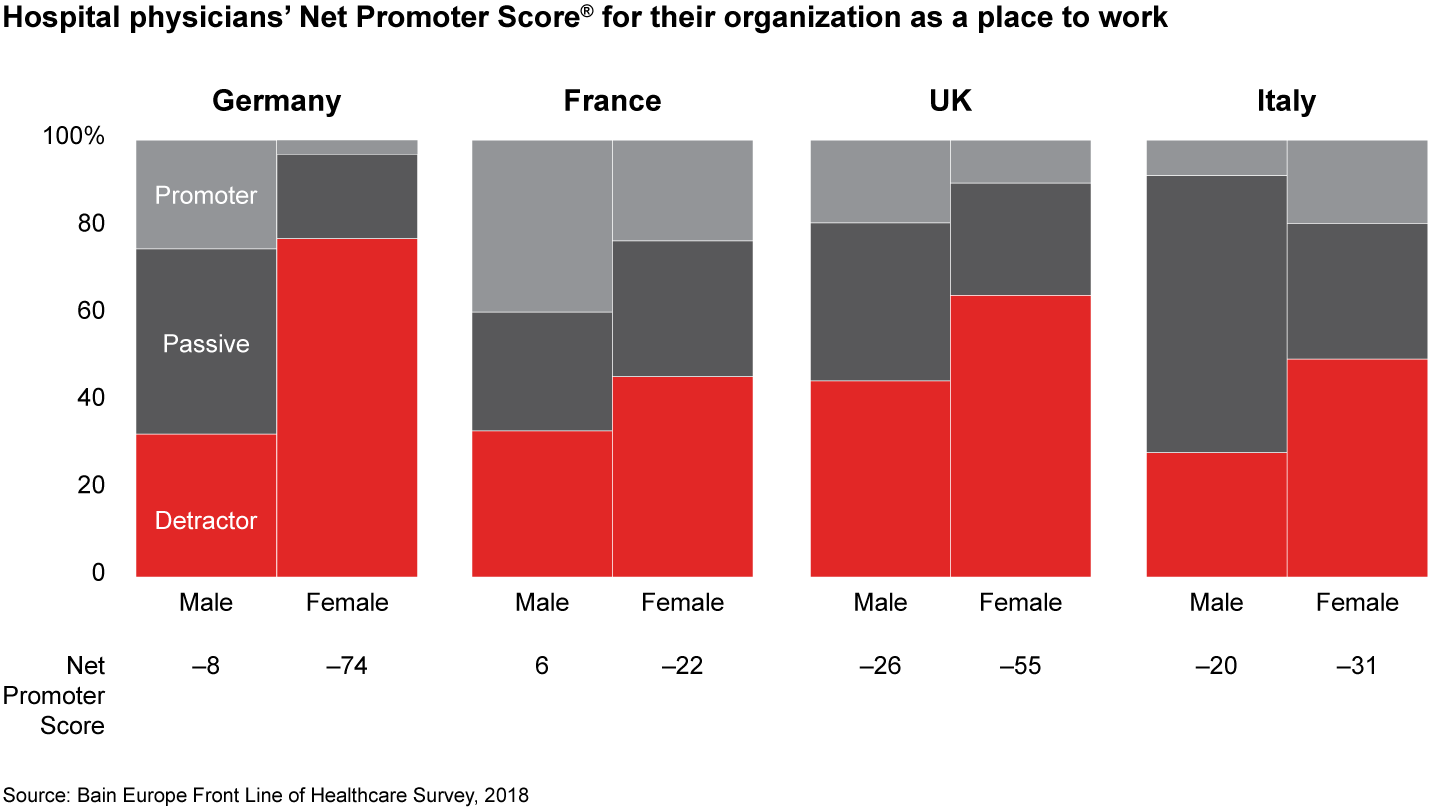
- Dissatisfaction of female physicians with their hospitals as a place to work or receive care is significantly more pronounced than among male colleagues, especially in Germany, where women give hospitals an average Net Promoter Score of negative 74 as a place to work and negative 62 as a place to receive medical care.
- The survey findings are an urgent call to action for public hospitals to take rapid, bold actions to improve healthcare delivery. Three initiatives can help hospitals and other healthcare providers begin to reverse negative attitudes: modernizing management structures, engaging physicians to rethink care delivery, and improving talent management.
- Bain research shows organizations with engaged and inspired employees are more productive. Providers that invest in creating alignment around their mission and put the right organizational structures in place to fulfill it have significantly higher physician advocacy.







2. Pharma
- Pharma innovation is a positive force for change: 70% of physicians expect pharma innovation to contribute to high-quality care in the future, and 59% point to the increased availability of biosimilar drugs as having a positive impact on care.
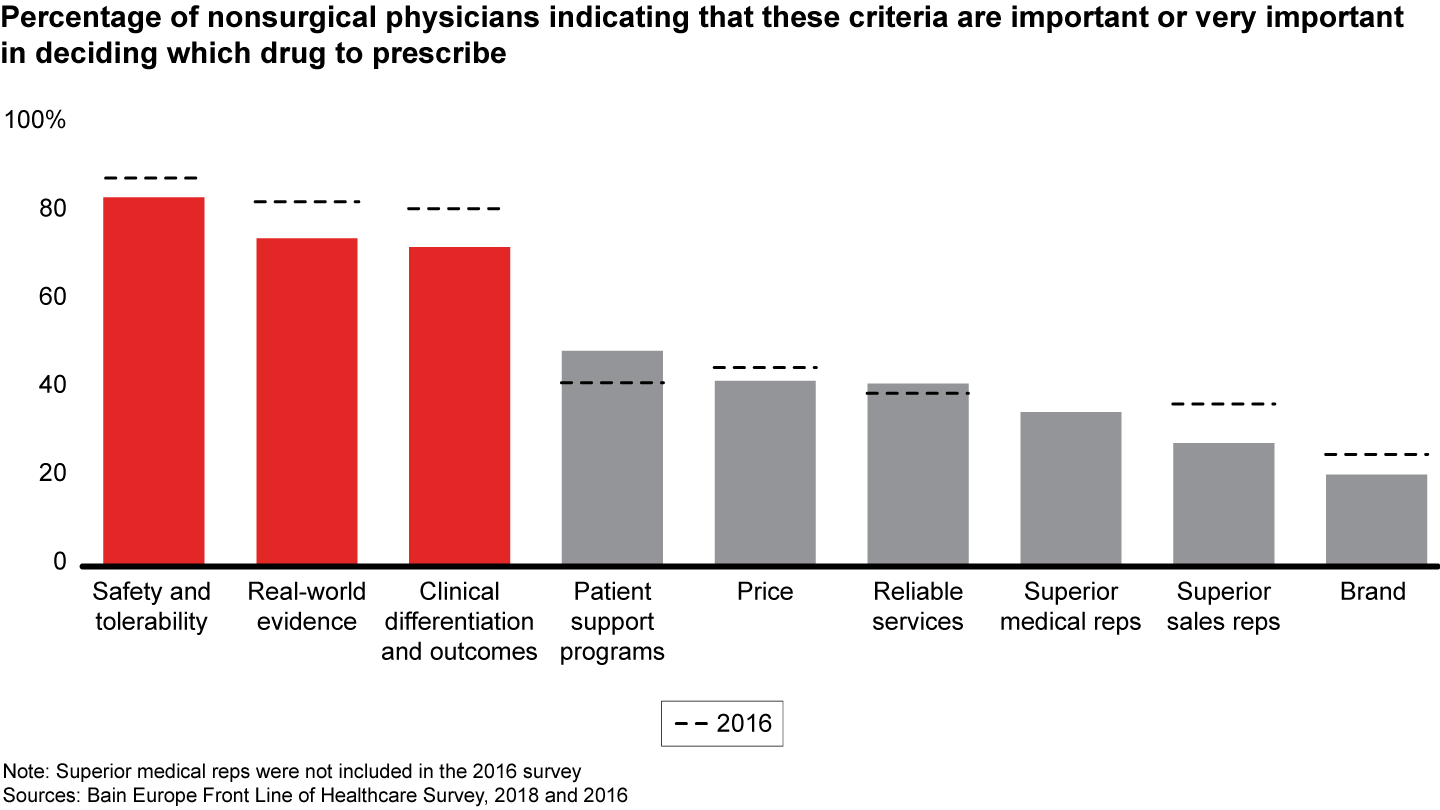
- High-quality data plays a key role in helping physicians to make treatment decisions. When deciding which drug to prescribe, physicians again rank safety, real-world evidence and clinical outcomes as the most important criteria.
- In their search for unbiased scientific information, physicians are relying less on traditional sources, including sales representatives. Increasingly, they are turning to new sources such as online information and medical science liaisons.
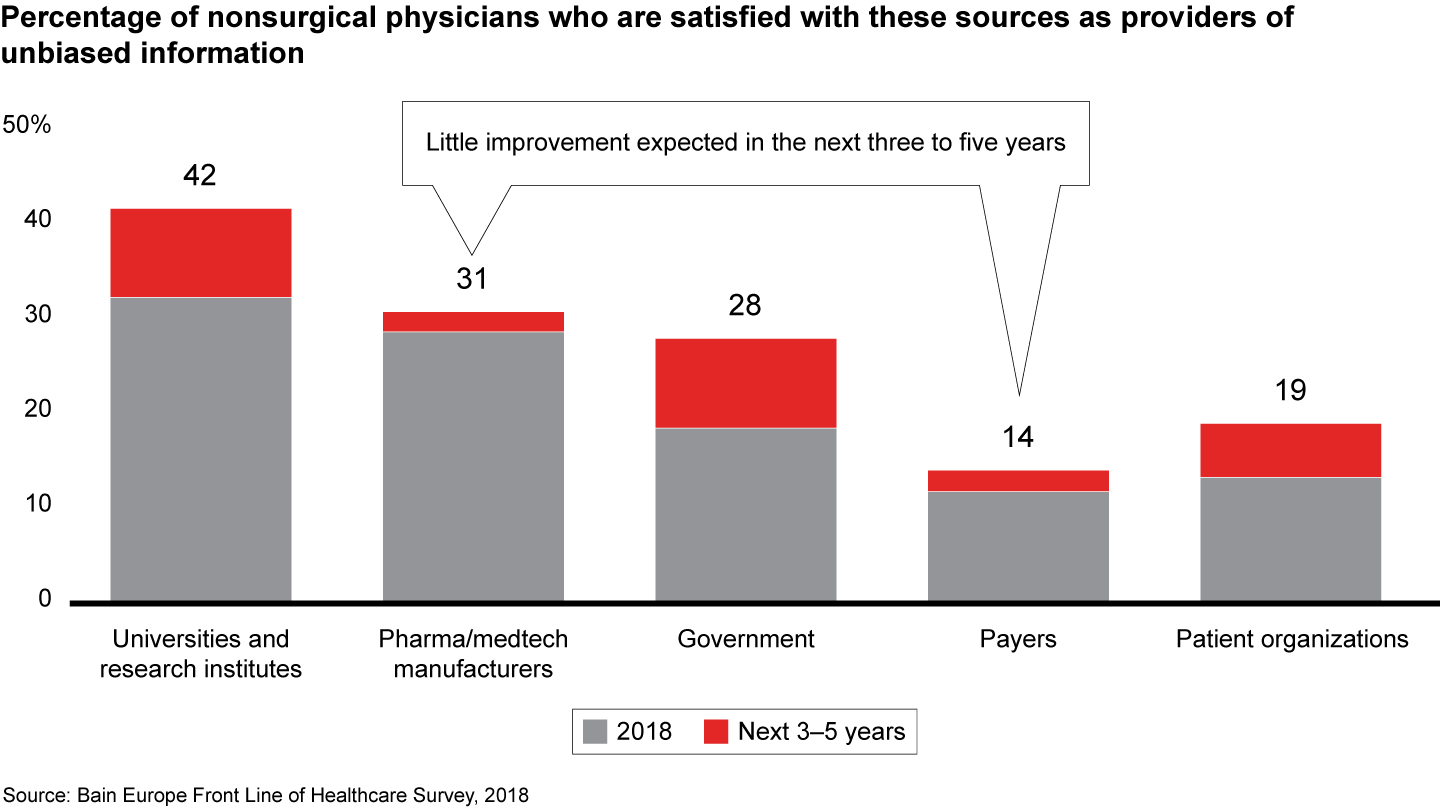
- Physicians are dissatisfied with all sources of unbiased information, including universities, pharma and medtech companies, governments, patient organizations and payers. In particular, physicians’ discontent with pharma manufacturers increased over the last two years. The average Net Promoter Score for 23 leading companies fell to negative 20 from negative 9 in 2016, and physicians remain skeptical that manufacturers will improve their support and communication much in the next three to five years.
- As information about new pharma products becomes increasingly complex and at times contradictory, physicians’ demand for clear and unbiased information is likely to grow. Pharma companies can meet that demand by developing objective, value-based data about their products. Those that fail to develop unbiased information may see other stakeholders fill the gap.
- Overall, physicians view category leaders in a more positive light than the industry as a whole, and recommend them over other companies. Endocrinologists and oncologists are particularly satisfied with their respective category leaders.










3. Medtech
- As hospitals seek to curb rising costs, procurement managers are increasingly taking the lead in decisions to purchase medical equipment. Centralized purchasing decisions have doubled over the past two years, and nearly 60% of physicians report that these decisions are predominantly led by procurement officers, with some input from physicians.
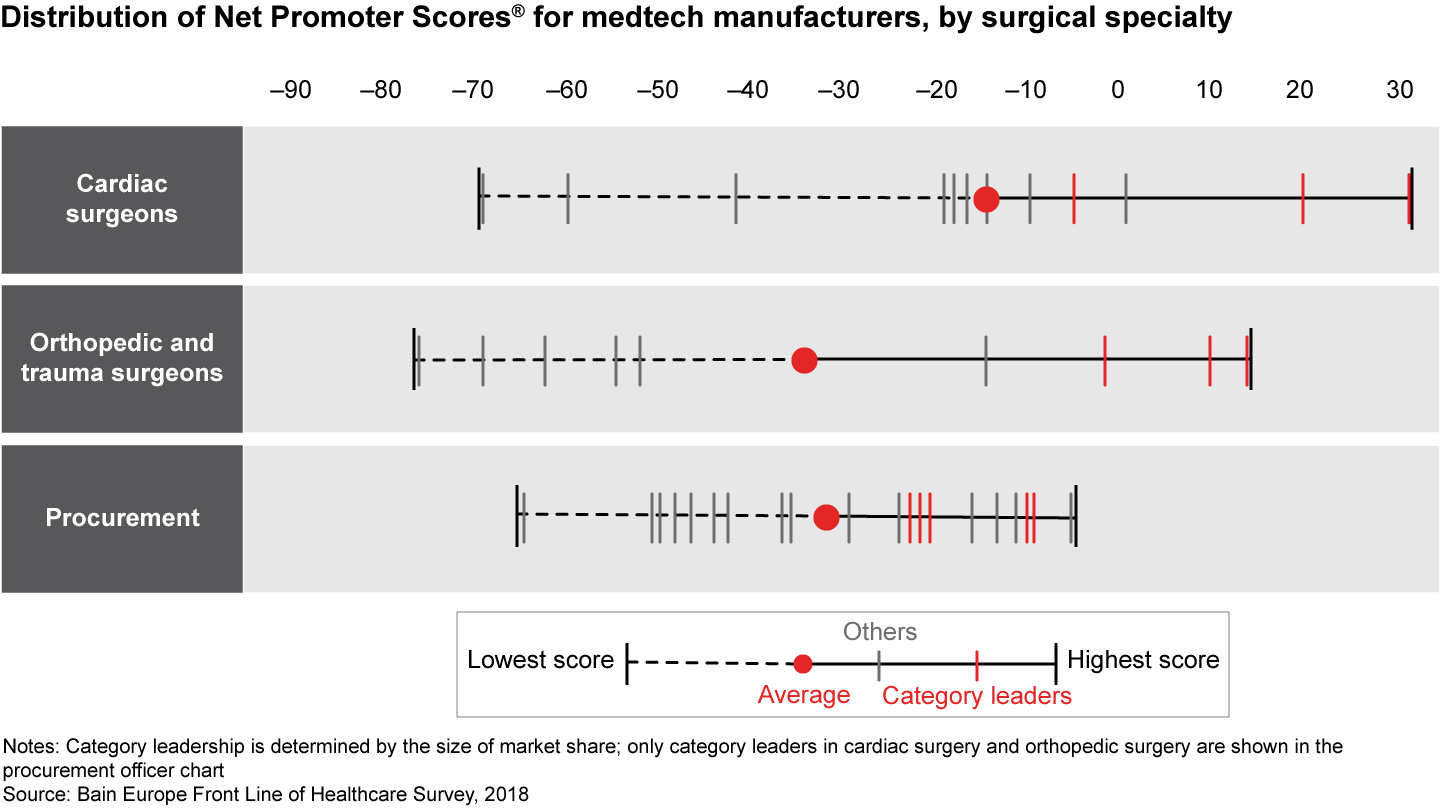
- Compared with pharma manufacturers, which uniformly received negative Net Promoter Scores, some medtech manufacturers received positive scores from surgeons, their traditional stakeholder. But none managed to receive positive scores in 2018 from procurement officers, an increasingly important stakeholder.
- Surgeons’ average Net Promoter Score for 22 medtech manufacturers fell to negative 23 from negative 14 in 2016, while purchasing officers’ score dropped to negative 31 from 1 two years ago.
- Medtech companies can improve their interactions with physicians and procurement officers by better understanding what these two sets of customers value most. Surgeons and procurement officers both value high-quality products, reliability and service. But surgeons rate poor service and support as their main reason for dissatisfaction. Only 11% of physicians identify price as a negative factor. By contrast, procurement officers cite price as the main reason they would not recommend a manufacturer.
- Surgeons and procurement officers also differ in their preferences for services beyond the product. Surgeons value clinical support and consulting more, while procurement officers express a preference for project management support and online ordering and tracking.
- Building category leadership can help medtech companies address the top concerns of both physicians and procurement officers. Overall, physicians view category leaders in a more positive light than the industry as a whole, and recommend them over other companies.







Appendix: Methodology and survey questions
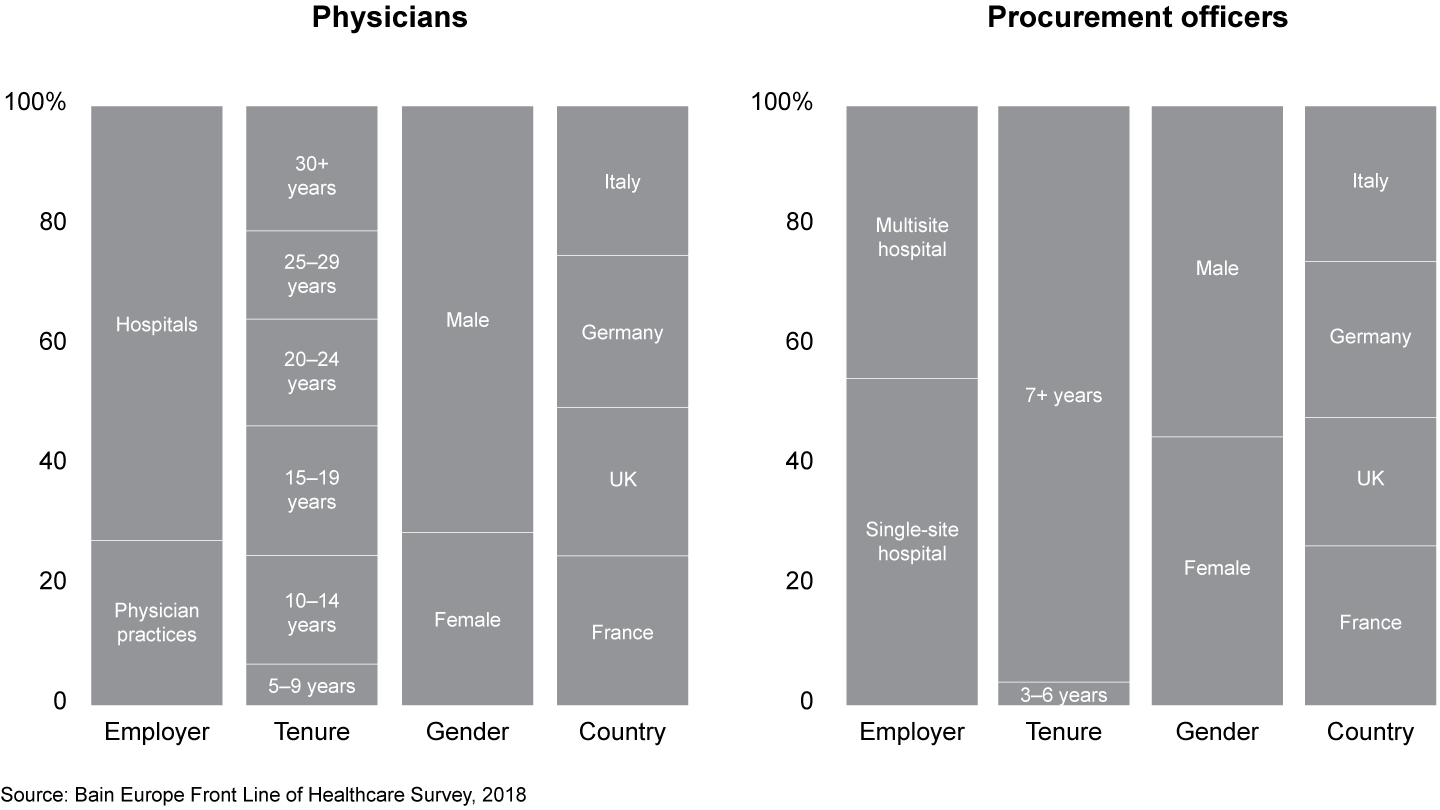
The Bain Europe Front Line of Healthcare Survey was conducted in 2018 by the physician panel at SERMO, a leading global social network for physicians and healthcare market researcher. It included a total of 1,156 physicians and 154 procurement officers from Germany, France, Italy and the UK. The survey evenly sampled physicians across these countries: Sample size was between 324 and 332 physicians in each country, and within countries, no geographic region was overrepresented.
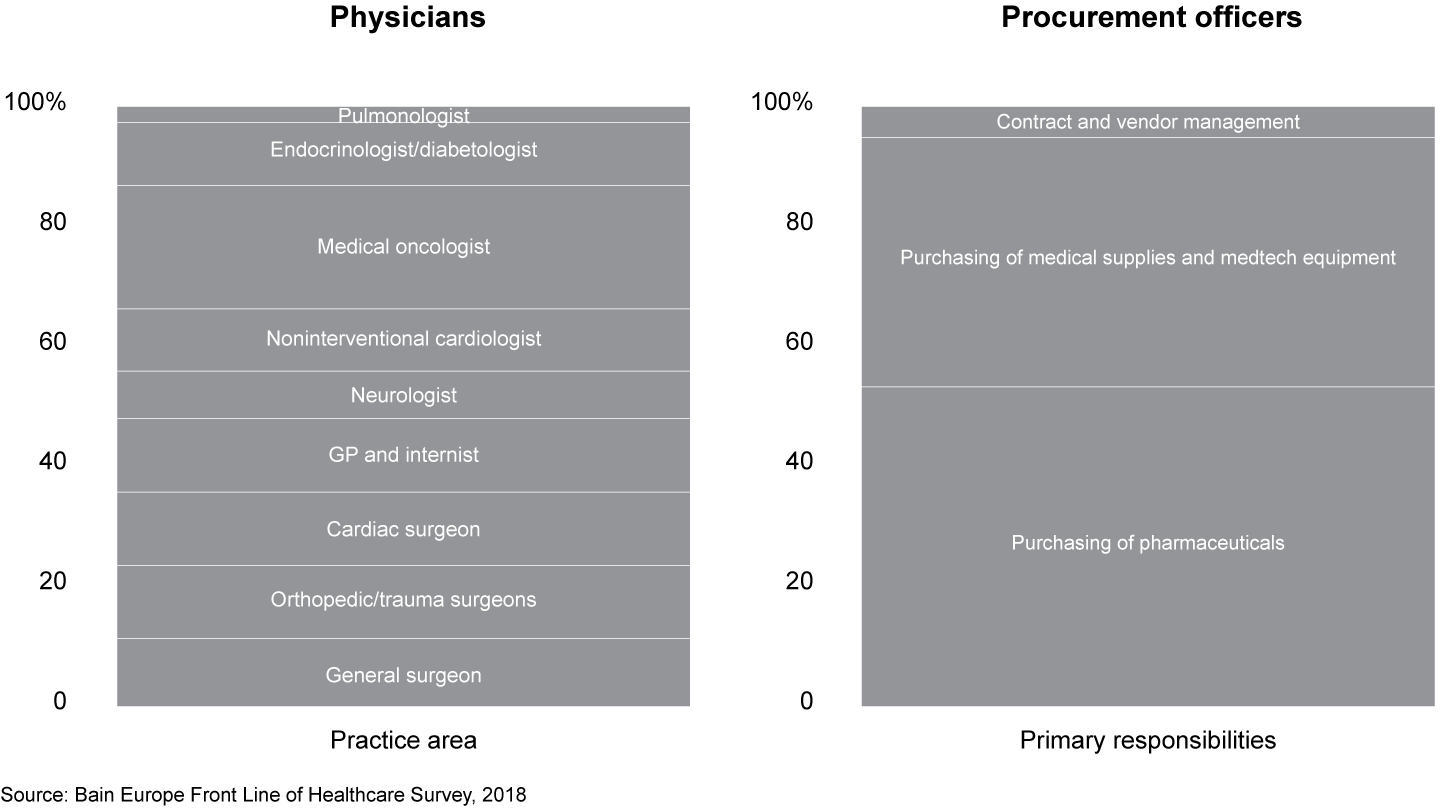
The survey focused on nine specialties: three surgical and six nonsurgical. The surgical specialties were general, cardiac and orthopedic surgery, and participants in these specialties provided input for the care delivery, medtech and hospital sections of this report. Nonsurgical specialties were primary care, medical oncology, noninterventional cardiology, endocrinology/diabetology and, in the UK, Germany and France, neurology; in Italy, we replaced neurology with pulmonology. Participants in these non-surgical specialties provided input for the sections about care delivery, pharma and hospitals. The specialties were chosen based on their global and regional revenue bases and the degree of ongoing change in the shifting healthcare environment. We also surveyed procurement officers to capture purchasing trends for medical devices.
SERMO’s online panel of healthcare professionals conducted the survey in local languages. The company carried out strict quality checks to ensure maximum data integrity, such as consistency and straight lining checks, speed control and quality assessments of free-text answers. The sample was weighted by specialty per country such that our results are nationally representative and internationally comparable for the specialties we selected. For overall European results, the sample was additionally weighted according to the number of physicians per country.


When measuring advocacy, we used the Net Promoter Score, which was developed by Bain & Company and is a tested indicator of advocacy. We asked two Net Promoter questions to assess physicians’ likelihood of recommending their organizations to friends or colleagues (a) as a place to work or (b) when in need of medical services. Ratings of zero to 6 signify detractors, 7 and 8 signify passives, and 9 and 10 signify promoters. The Net Promoter Score is calculated by subtracting the percentage of detractors from the percentage of promoters. A positive score indicates advocacy and support, while a negative score shows the opposite.
Survey questions
Figure 1: Please rate the impact of the trends below on your ability/the ability of your organization to deliver high-quality care to your patients today (undecided/neutral answers not shown); n=1,156
Figure 2: To show use of analytics and clinical tools, we calculated the percentage of physicians currently using a variety of tools. For risk-based payment models, we looked at the percentage currently using at least one of the following models: pay for performance, bundled payments, shared savings and capitation. For use of management tools and physician cost-consciousness, we based percentages on the number of physicians agreeing or strongly agreeing on a Likert scale to statements. For use of metrics, we calculated the percentage of physicians who said they are evaluated on three or more metrics; n=1,156
Figure 3: Please indicate if you have used the following tools or participated in the following programs (whether by your own choice or your organization’s or hospital’s choice); n=1,156
Figure 4: Which of the payment models for pharmaceutical/medtech products listed below are being utilized by your patients’ insurance coverage providers now and in the next two years? Nonsurgical physicians n=743, surgical physicians and procurement officers n=567
Figure 5: Please rate the impact of the following innovations in digital on your ability to deliver high-quality care in the next three to five years (undecided/neutral answers not shown); n=1,156
Figure 6: Please rate the impact of the trends below on your ability/the ability of your organization to deliver high-quality care to your patients today (undecided/neutral answers not shown); n=1,156
Figures 7, 8, 11, 13: On a scale of zero to 10, where “zero” means “not at all likely” and “10” means “extremely likely,” how likely are you to recommend your practice/organization to a friend or colleague as a place to work? Physicians working in hospitals n=838
Figure 9: How likely are you to remain working for the NHS in the next five years? UK physicians only n=324
Figures 10, 12: On a scale of zero to 10, where “zero” means “not at all likely” and “10” means “extremely likely,” how likely are you to recommend your practice/organization to a friend or family member as a place to receive care? Physicians working in hospitals n=838
Figure 13: To what extent do you agree with the following statements about your employer? Physicians working in hospitals n=838
Figure 14: Please rate the impact of the trends below on your ability/the ability of your organization to deliver high-quality care to your patients today (undecided/neutral answers not shown). Physicians working in hospitals n=838
Figures 15, 16: How important are the following criteria when deciding which drug(s) to prescribe to a patient? Nonsurgical physicians n=743
Figure 17: What are the three most valuable roles a medical science liaison representative/sales representative can play? Percentage of respondents selecting each role among top three. Nonsurgical physicians n=743
Figures 18, 19: How well are the individual stakeholders currently fulfilling your expectations when it comes to providing unbiased scientific information? How well do you think they will fulfill your expectations in the next three to five years? Nonsurgical physicians n=743
Figures 20, 23: Please answer the following question about pharmaceutical manufacturers with which you are most familiar. On a scale of zero to 10, where “zero” means “not at all likely” and “10” means “extremely likely,” how likely are you to recommend this manufacturer to another physician? Nonsurgical physicians n= 743
Figure 21: Below is a list of physician needs (episodes) that pharmaceutical manufacturers can help to fulfill. Please select and rank the five physician needs (episodes) that have the greatest influence on your decision to prescribe a certain drug if fulfilled appropriately. For five most important episodes: On average, how satisfied are you with these interaction sequences (episodes)? Nonsurgical physicians n=743
Figure 22: Please answer the following question about pharmaceutical manufacturers with which you are most familiar. On a scale of zero to 10, where “zero” means “not at all likely” and “10” means “extremely likely,” how likely are you to recommend this manufacturer to another physician? If answer is zero to 6: Why would you not recommend this manufacturer? If answer is 9 or 10: Why would you recommend this manufacturer? Nonsurgical physicians n=743.
Figure 24: There are several purchasing methods that healthcare facilities use when purchasing medical devices. Please check the option that best describes the hospital/organization where you spend the majority of your time today and three years ago. Surgical physicians n=413
Figures 25, 26, 27, 30: Please answer the following question about medical device manufacturers with which you are most familiar. On a scale of zero to 10, where “zero” means “not at all likely” and “10” means “extremely likely,” how likely are you to recommend this manufacturer to another physician? If answer is zero to 6: Why would you not recommend this manufacturer? If answer is 9 or 10: Why would you recommend this manufacturer? Surgical physicians n=413
Figure 28: To what extent are the following cost-saving initiatives a priority for your organization? Procurement officers n=154
Figure 29: Which of the following value-added services would you most appreciate from a supplier, if they were offered? Please select the top three services. Surgical physicians n=413, procurement officers n=154
Authors
This report was prepared by Michael Kunst, Nitin Chaturvedi, Loïc Plantevin, Valerio Di Filippo, Dieter Meyer and Christian Rebhan. Michael Kunst and Loïc Plantevin colead Bain & Company’s Healthcare practice in Europe, the Middle East and Africa, and are based in Munich and Paris, respectively. Nitin Chaturvedi is a Bain partner in the firm’s London office. Valerio Di Filippo is a partner based in Milan. Dieter Meyer is a partner in the Zürich office. Christian Rebhan is a partner in Bain’s Zürich office.
Acknowledgments
The authors wish to give special thanks to Nathalie Fetzer-Hoernig and Anna Boleininger for their work on this report and to the physician panel at healthcare market researcher SERMO for conducting the Bain Europe Front Line of Healthcare Survey.
Net Promoter Score®, Net Promoter System®, Net Promoter® and NPS® are registered trademarks of Bain & Company, Inc., Fred Reichheld and Satmetrix Systems, Inc.