Brief
The need to build an RMNCH+A sector
Historically, developing countries have struggled to tackle large-scale health initiatives. In India, a significant portion of the population still lacks access to healthcare. While recent research indicates that the country has made some healthcare advances, India still has a ways to go to reach the Millennium Development Goals or catch up with developed countries like the US. In particular, healthcare services for women and children are disappointing compared with the rest of the world. A 2012 survey by TrustLaw, a division of the Thomson Reuters Foundation, placed India at the bottom of the ranking among G20 countries for policies that promote gender equality and give women access to healthcare, among other criteria.
That said, it is important to note that we are currently at an important juncture. The post-liberalisation period has been marked by significant economic progress: growing incomes and a consumption boom. To ensure social progress with economic development, it is critical to quickly address basic social and health issues. Only then will we see India’s population completely empowered.
The Indian government has made strategic investments in reproductive, maternal, newborn, child and adolescent health (RMNCH+A) to reduce maternal and child mortality. The RMNCH+A approach traces women’s well-being through their lifespans, including infancy, childhood and adolescence, and provides a “continuum of care”. The “+” refers to the recent focus on adolescent health because of the growing realisation that measures applied in adolescence prevent complications for mothers and their children.
Unlike previous efforts to fight HIV and eradicate polio, the urgency of addressing the RMNCH+A challenge has not translated into substantial efforts to build this ecosystem. Therefore it is imperative to create an ecosystem of strong participants from the public, private and philanthropic sectors. In the past, much of the efforts to improve women’s and children’s health have had limited support, but government agencies and nonprofits have begun to develop an understanding of the services or interventions, as it is commonly referred to in the sector, to pinpoint areas of maximum impact.
Our India Philanthropy Report 2014 seeks to inform the next level of ecosystem building required to address the RMNCH+A challenge in India.
Because understanding stakeholder ecosystems is critical to achieving the desired outcomes, we will analyse what comprises successful ecosystems and the stages of ecosystem development involved in meeting these societal challenges. Over the past few decades, we have witnessed coordinated responses and multisector participation for similar challenges. For a clearer perspective of the RMNCH+A issues, we have used specific examples from the HIV, polio and microfinance ecosystems, which we have been examining closely.
Recent research in The Lancet points to the evidence that RMNCH+A outcomes, like the under-five mortality rate, can be substantially improved by 2035 with the right investment plan. In our report, we first present those estimates for India and point to potential participants who could bridge the gap. We then demonstrate that investing in this strategic approach is reasonable.
To prepare this report, we studied the outcomes associated with the RMNCH+A approach, observed the progress made to date and noted the distance from the target. We also studied the private, public and philanthropic sectors’ participation to determine where there are gaps in their engagement. Finally, our report articulates where the RMNCH+A sector is in its evolution.
Executive summary
A vibrant ecosystem that addresses maternal and child health is the need of the hour
- An ecosystem of stakeholders is needed to tackle society-wide problems like poor access to essential healthcare for women and children. Achieving large-scale goals without such a setup would be slow and suboptimal.
- India has a successful track record in addressing society-wide issues on a large scale. Developing comprehensive ecosystems for polio, HIV and microfinance was critical to India’s successes in those areas.
- Studying those successes led us to conclude that there are six critical actors in the ecosystem: beneficiaries, interventionists, coordination bodies, infrastructure providers, funders and organisations that promote awareness.
- A reasonable base for RMNCH+A has been established, with strong government and emerging nonprofit participation, despite long periods of stasis since India’s independence.
- The RMNCH+A ecosystem will need to address issues across health, nutrition, education and sanitation.
- There has been significant improvement in women and children’s health over the last 15 to 20 years: Maternal and infant mortality rates, the number of underweight children and child marriages and the total fertility rate have all declined. However, several areas of concern remain; for example, a high rate of anaemia among mothers and children.
- The successes of other ecosystems also suggest that non-state actors and funding can be game changers. But this can’t occur in a vacuum and will need strong coordination bodies, infrastructure and innovation.
Developing a mature RMNCH+A ecosystem by 2035 is a reasonable proposition
- India’s economic growth is expected to be strong: about 5% in real terms, on average, until 2035.
- On the back of this growing economy and through government interventions like the National Health Mission (NHM), the share of GDP spent on public health is expected to increase from 1% currently to 1 .7% in 2035, generating additional public funds to meet the agenda for RMNCH+A.
- However, public funds alone will be insufficient; other participants will have to step in. By 2025, India will need an incremental $12 billion over the public health expenditure. With economic growth and rising spending, that amount will be reduced to an incremental spending of about $3 billion in 2035.
- To achieve the 2035 outcomes, it will be necessary to address the funding gap through non-state sources of funding and by building an ecosystem to effectively deploy the funds.
With the right strategy, the RMNCH+A agenda for 2035 can be achieved
- Non-state funding will have to be generated by private sources; multilaterals and bilaterals are unlikely to increase their current giving of about $0.7 billion.
- Doubling the current share of contributions to health through corporate social responsibility (CSR) and high-net-worth individuals (HNWIs) in India can provide an additional $2.7 billion by 2025.
- This will leave a gap of approximately $8.6 billion by 2025, which will have to be funded through private foreign donations to achieve the 2035 objectives.
- Non-state participants focused on strengthening health systems and scaling up programmatic interventions can also act as catalysts in the development of a vibrant ecosystem. They can also help expand the delivery system facilities, quality of care, technologies and awareness.
- Support networks will need to help channel funds from private and philanthropic sources to grass-root organisations. And to grow, these organisations will need regulatory and legal support.
- Incrementally, government agencies like the NHM must meet their mandates, and vertical programmes must find a way to work with one another.
- New innovations will also be needed to drive disruption via low-cost technologies, multisector partnership models and direct community outreach.
Achieving RMNCH+A goals in India
An ecosystem is needed to deliver value to end recipients . . .
India has faced several critical health issues in the past and tackled them by building ecosystems. The importance of this approach comes from realising that developing a response to large-scale societal issues is a difficult process. Several actors are critical to success, with each being important at different stages of the ecosystem’s evolution.
Successful efforts to overcome crises like polio and HIV provide a lens through which an ecosystem can be defined. Even issues unrelated to health, like financial empowerment achieved by the microfinance sector, have lessons to offer.
Six actors typically form the critical parts of an ecosystem (see Figure 1):
- Beneficiaries: recipients of the services
- Interventionists: skilled and semi-skilled workers who execute the needed services in the field
- Infrastructure providers: physical establishments, technology and training to enable the services
- Funders: sources of capital that support the activities of various stakeholders
- Coordination bodies: strategic monitoring and decision-making entities for systemic progress
- Organisations that promote awareness: development agencies, mass media and research institutions
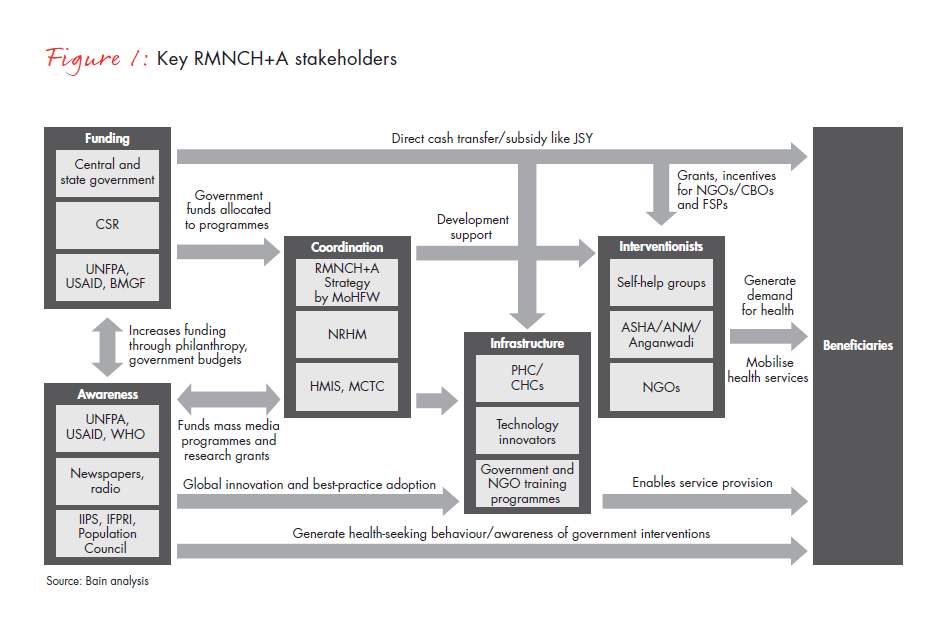
A reasonable base for RMNCH+A has been established in the last few years of early growth. The government has been actively involved in all aspects of the RMNCH+A approach. Today, the government’s action forms the backbone of this sector. The National Rural Health Mission (NRHM) has assumed the role of a “nodal agency,” promoting awareness, building infrastructure and so on. Field service providers, such as accredited social health activists (ASHAs), auxiliary nurse-midwives and anganwadi workers, take health services to the doorsteps of the underprivileged. Public facilities such as primary health centres (PHCs) and community health centres (CHCs) have been expanded for improved coverage in rural areas.
The private sector is nascent in addressing maternal and child health issues. Largely concentrated in the urban tertiary segment, providing quality care has been challenging in rural areas, especially for primary care. A significant part of the private market lies in the informal sector, with an unqualified or insufficiently qualified workforce delivering interventions.
Although external development agencies have been around for several years, innovative market strategies and expertise have been making an impact in recent years. Meanwhile, philanthropic activity is in the early stage of development. Non-governmental organisations (NGOs) have suffered from the lack of a government framework, but they are well poised to grow with an expected increase in donations from private foundations and individuals. CSR strategies have matured, and recent policy moves have set the base for massive investments going forward.
. . . to tackle the long-standing health issues for women and children
The RMNCH+A approach is a holistic strategy to ensure the well-being of adolescents, women and children. The “+” denotes the retrospective addition of adolescents because of a realisation that several challenges faced by women in their later years can be addressed early on. Interventions, or services, are envisaged to be provided through this “continuum of care”. This approach seeks to provide a whole spectrum of services, including health, nutrition, education, empowerment, water and sanitation.
The RMNCH+A approach is an improved response to the health challenges, which have been largely unaddressed. It is critical to achieve success with this holistic approach because women’s health and well-being positively affects the overall Human Development Index for the country. Unless basic social issues are addressed, India’s economic progress will at best be muted for its population at large.
For mothers, this new holistic approach has brought about moderate improvement in the last 15 or more years (see Figure 2). However, there is a significant distance to cover, based on the targets and outcomes achieved by developed nations. The maternal mortality ratio (MMR) has declined at an annual rate of about 5% and is halfway to achieving the Millennium Development Goals articulated by the United Nations. Anaemia, however, presents a worrying sign, having increased at a rate of around 2%.
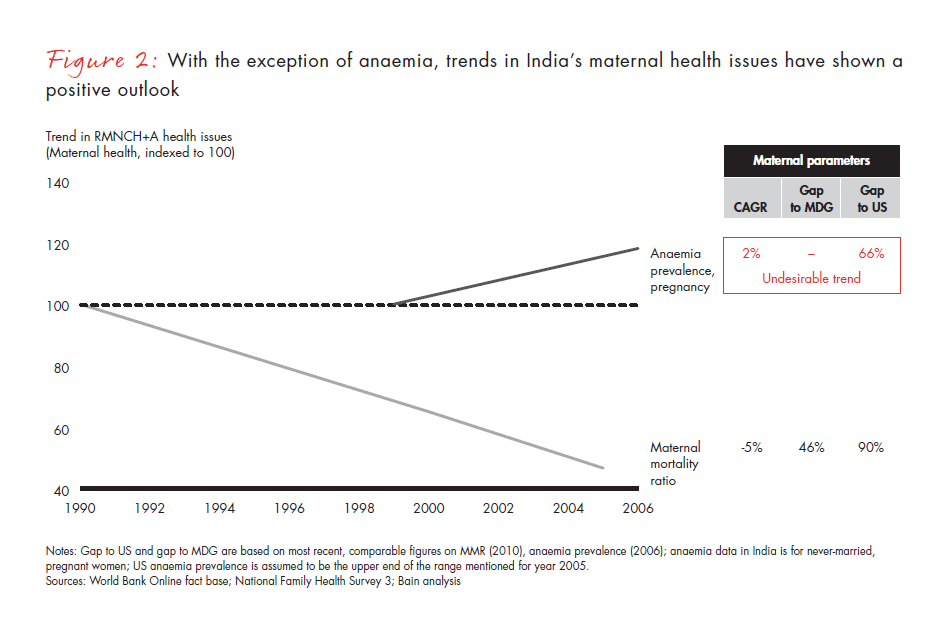
The number of cases of anaemia in children has fallen, albeit slowly (see Figure 3). And significant improvements have been seen with underweight children and in the declining number of infant deaths. In both areas, India is two-thirds of the way to achieving the Millennium Development Goals.
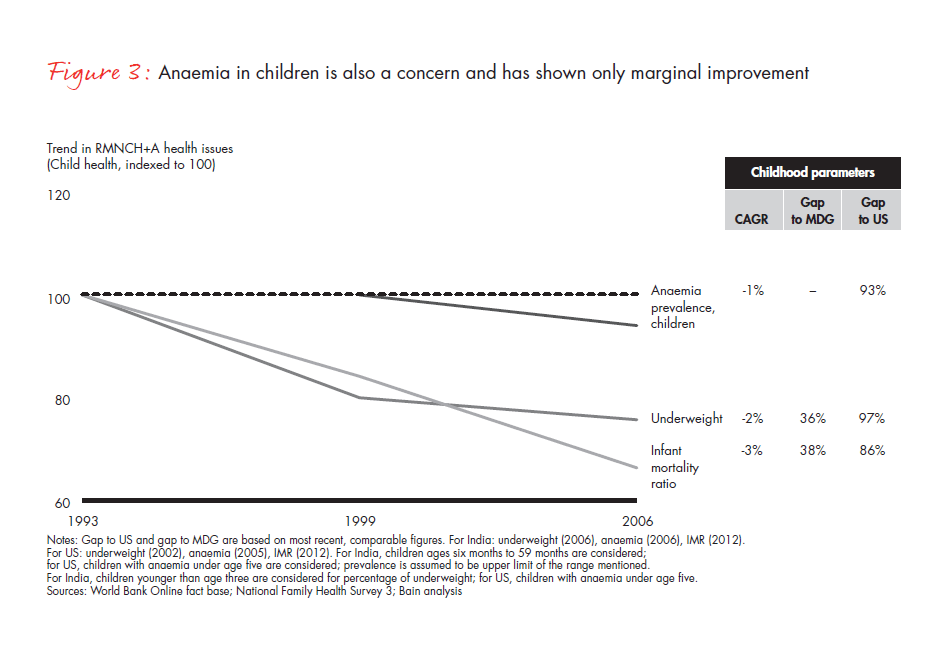
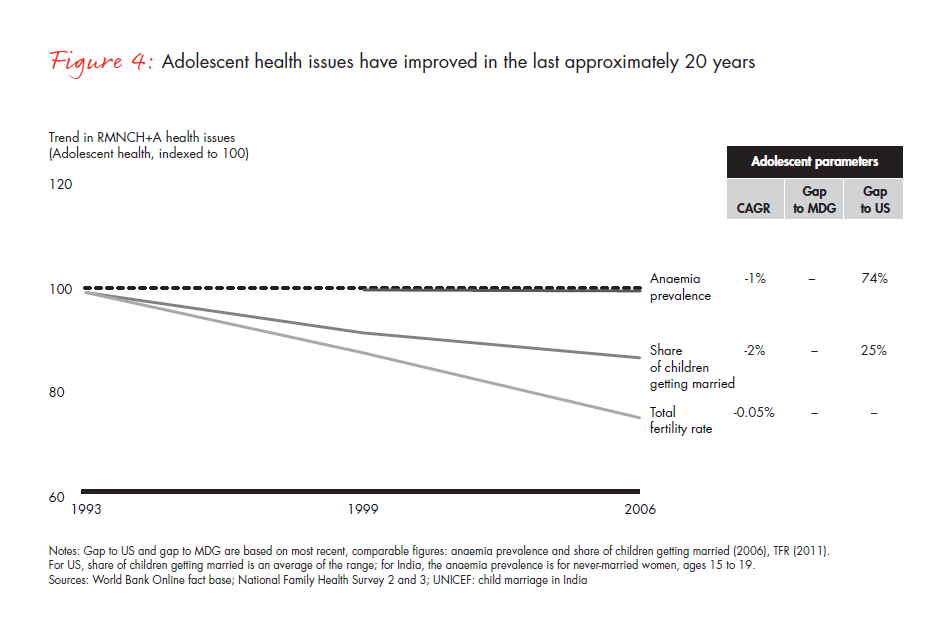
For adolescents, we see a flat trend for cases of anaemia (see Figure 4), and the number of child marriages has decreased. Also, total fertility rates have seen aggressive reductions, and urban India has reached government mandates.
We can learn from similar challenges of the past
In the past, India has achieved remarkable success resolving societal challenges in healthcare and beyond. Examining the four distinct stages of evolution similar to a business investment cycle can help define the agenda for RMNCH+A:
- Seeding: an early stage of evolution, characterised by ad hoc actions to address a perceived issue and understand its scope
- Early growth: characterised by the emergence of a coordinating body and by a better understanding and estimate of the full crisis
- Rapid growth: marked by the emergence of non-government participants (donors, philanthropic and private organisations), whose activities both complement and surpass those of organised government or quasi-government participants
- Maturity: reached when the ecosystem’s growth rate stabilises, with players developing their own distinct roles and functions
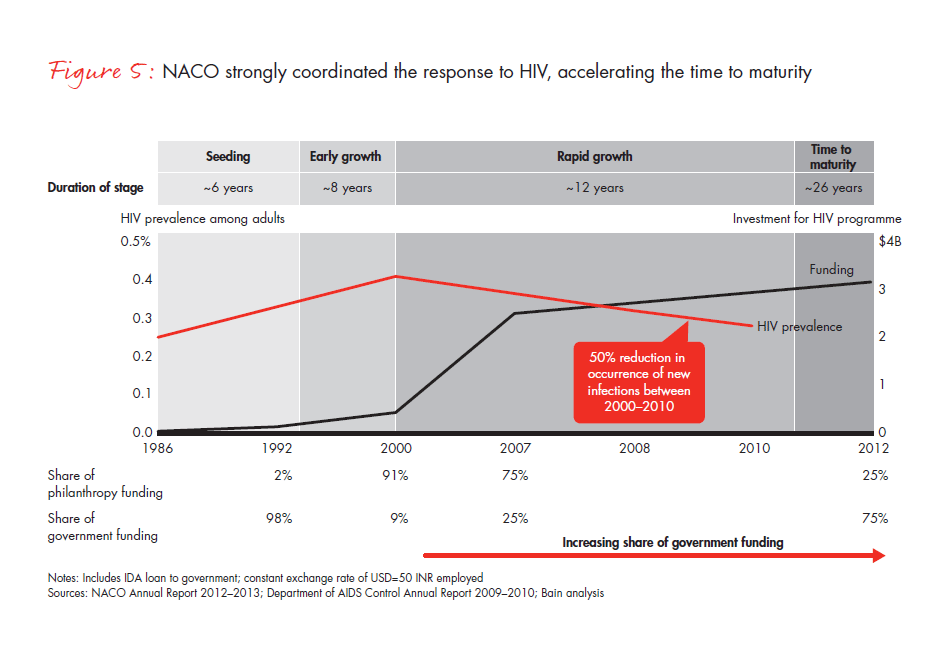
Ecosystem outcomes and funding track the four stages of evolution. For example, prior to 1992, in the seeding stage of the HIV ecosystem, the prevalence of the disease was high but the funding was low. Over the next 20 or more years, as the ecosystem was built out, the funding increased and the disease was brought under control (see Figure 5).
Based on such examples of success, there are several lessons for us to learn:
Strong coordinating agencies will accelerate the pace of development. Some ecosystems (for example, HIV) evolve rapidly, at a uniformly fast rate, and take about 25 years to reach maturity. Others develop in spurts and have long periods of stasis between stages. The microfinance ecosystem, for example, remained in the seeding stage for nearly 30 years before entering the growth stages. The differences can be attributed to the National AIDS Control Organisation’s (NACO’s) effective coordination and the microfinance institutions’ lack of organisation.
Expansion of delivery and support systems will determine the time to maturity. The microfinance sector’s mandate was to provide financial inclusion through rural banking services, but for almost 30 years, several public initiatives failed. Then the SHG Bank Linkage programme established a sustainable channel for the flow of funding and pushed the ecosystem through the early growth phase. The polio ecosystem is another example of how organised government action can move the sector through the growth stages. In the case of HIV, a strong delivery system and untiring efforts made by nonprofits to raise awareness provided the necessary interventions to high-risk groups.
Philanthropic and development agencies have been effective in spurring rapid growth. The microfinance ecosystem matured with the private sector’s participation, but it is important to note that philanthropic and development agencies set the ball rolling. With the failure of the government’s social banking initiatives, external funds like the International Fund for Agricultural Development and the Department for International Development stepped in and set up the National Microfinance Support Project, establishing much-needed momentum. Coupled with other government initiatives, like the SHG Bank Linkage Programme, scale was established in these operations, which eventually spurred the private sector’s participation, especially mainstream banks. A similar trajectory was seen with the HIV ecosystem.
Step-growth increases in funding can bring about rapid growth. For the HIV epidemic, the role that the National AIDS Control Programme (NACP) played was pivotal, increasing total funding by nearly eightfold in 12 years. New HIV infections dropped by 50% in that time, and India managed to control what was a crisis.
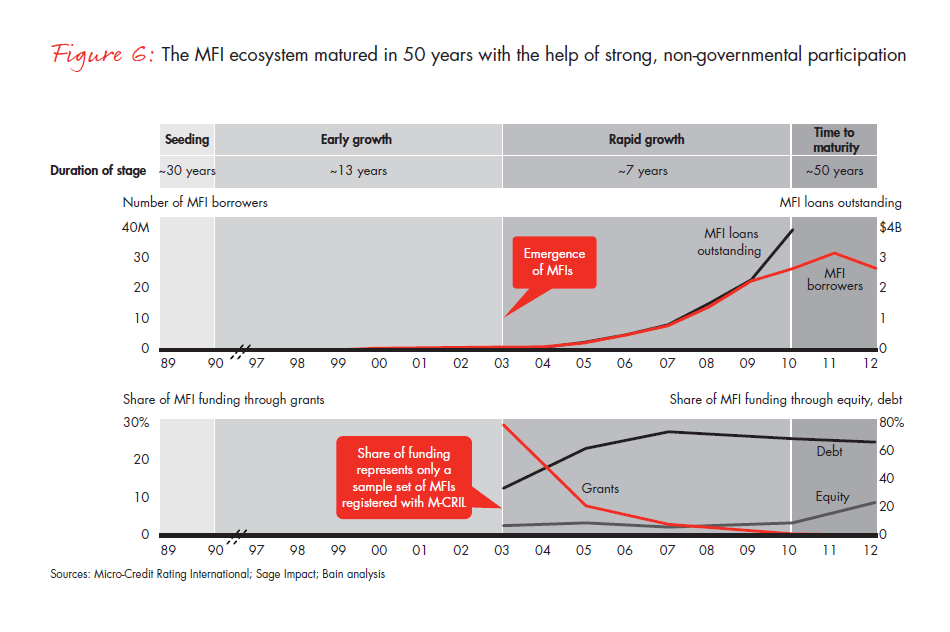
The front-loading strategy for philanthropic funding works. Sensing a growing HIV crisis, external development funds and philanthropic organisations contributed to the second phase of the NACP, funding nearly 90% of the programme. Their support continued to flow into the third and much larger phase of the NACP. By providing the government with much-needed support in the fledgling stages, they helped develop a critical ecosystem for HIV. After achieving critical targets set by the fourth phase of the NACP, overall funding growth has flattened, with contributions falling to just 25% of the total funding received in the fourth phase. In microfinance, this trend can also be seen, with the grant funding to microfinance institutions dwindling in recent years (see Figure 6).
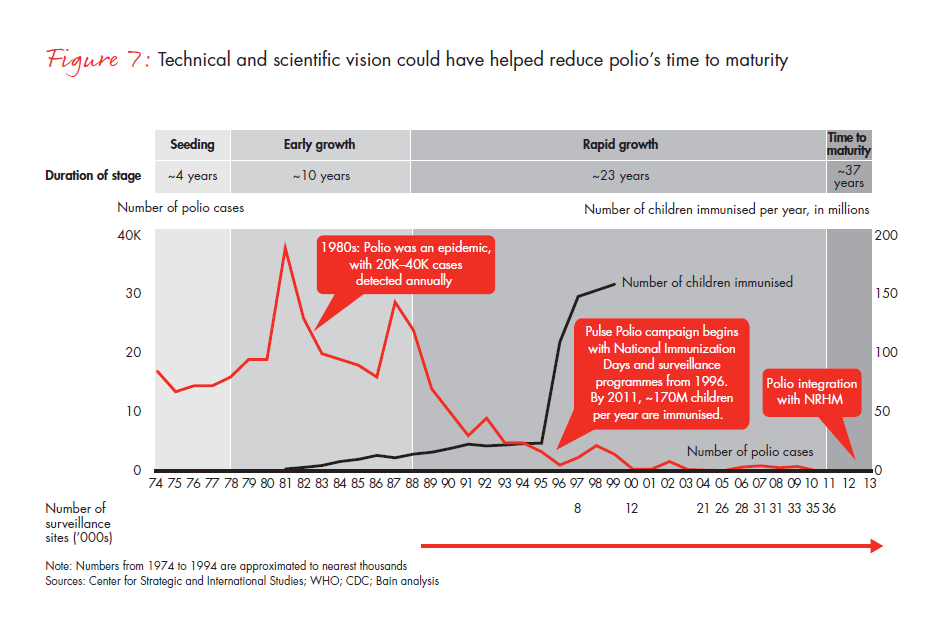
Innovation has the potential to reduce response times. Scientific and technical vision was especially critical for controlling the polio epidemic (see Figure 7). The unfortunate choice to go with OPV drops (the low-cost option) instead of IPV shots lengthened the fight against polio by, it is believed, 10 years beyond 2000—the target eradication year. In the fight against HIV, however, low-cost anti-retroviral drugs were vital, being easily accessible and affordable to all patients. The private sector will have to take the lead in R&D.
A reasonable proposition for 2035
Creating the diverse and robust ecosystem envisaged for RMNCH+A will require careful consideration based on recent research findings about maternal and child health as well as lessons from other sectors.
According to the Global Health 2035 report, published in The Lancet in December 2013, it is possible for India to address the big challenge of providing comprehensive healthcare for women and children. And a “pro-poor investment plan” has been laid out to overcome the inertia seen in this sector. By adopting this agenda, the research suggests, India can be on par with the best-in-class globally.
After gaining independence, India was plagued by wars, lack of healthcare and nascent infrastructure. Barring the Child Survival and Safe Motherhood programme, which was set up with support from the World Bank and the United Nations, unorganised and ad hoc government actions were at play. This is clearly reflected in the slow improvement in the child mortality rate, which decreased by only a 2.8% compound annual rate in the seeding phase.
But things changed for the better after 1997. India made real progress in reducing child mortality: The rate fell by an average of 3.8% annually, a 38% improvement which marked the onset of the early growth stage. Focused government action can be attributed to this advance; the Reproductive and Child Health policy (RCH-1) and the establishment of the NRHM brought much-needed focus. External development agencies also continued to be engaged, and a base for philanthropic action was established.
With a child mortality rate of 63 deaths per 1,000 live births as of 2011, a target of 19 deaths per 1,000 live births can be achieved by 2035. This is close to China’s current child mortality rate of 14 deaths per 1,000 live births. But if we don’t act now, instead of in 20 to 25 years, we may not reach our goal until 2055. A 20-year delay is avoidable and would be unfortunate.
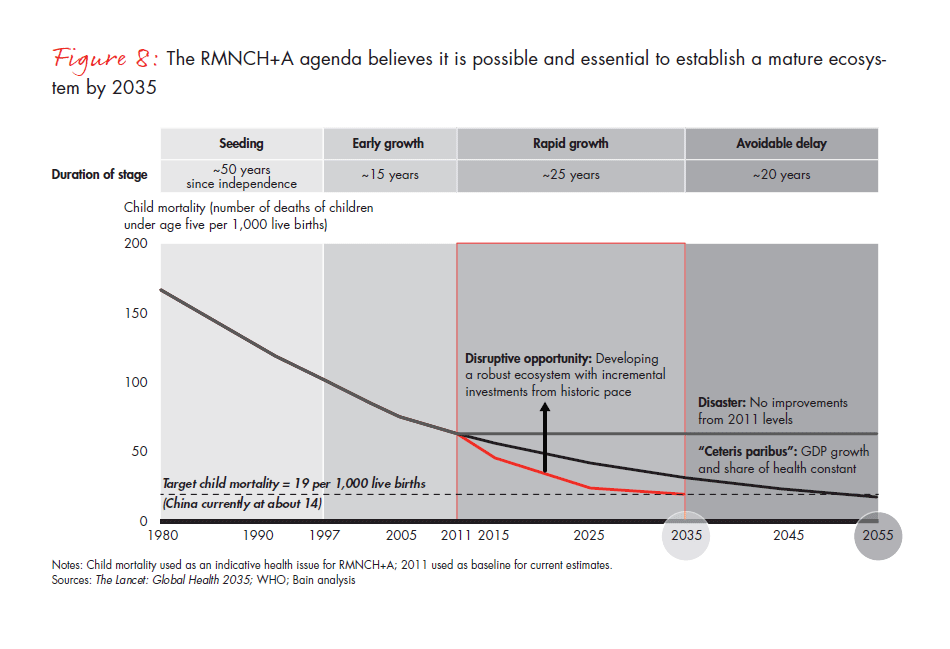
There are three possible scenarios before us (see Figure 8):
- Disaster: Negligible GDP growth and limited incremental healthcare investment would worsen the situation. RMNCH+A outcomes would stay at the 2011 level in this scenario. We believe this is an extremely unlikely scenario, however, based on several public estimates.
- “Ceteris paribus”: India continues to chug along at 5% real GDP growth, with no disruptive changes in the ecosystem and rate of investments. This would lead to improvement in the outcomes at the historical rate, reaching targets in 2055.
- Disruptive opportunity: GDP growth of 5%, coupled with an enhanced rate of investment and changes in the ecosystem, can drive transformational outcomes. Targets may be reached by 2035, the optimal scenario.
For India to achieve transformational outcomes, sector investment will need to increase to $50 billion by 2025 and $73 billion by 2035, according to the Global Health 2035 report.
The government will have to do its share of the heavy lifting:
- As of 2011, the share of RMNCH+A spending as a percentage of GDP is 0.8%, which is 70% of India’s total public health expenditure. This $13 billion comes through four funding programmes relevant to the RMNCH+A agenda: the central NRHM (recently integrated into NHM), NACO, state budgets and local bodies.
- At the current pace, with a real GDP growth assumption of 5% (based on OECD estimates) until 2035, the government expenditure for RMNCH+A is estimated to be $25.6 billion in 2025 and $42 billion in 2035.
- Organisations like the World Health Organization expect that total public health spending will increase from current levels of 1% of GDP to 1.5% by 2025 and 1.7% by 2035 in India.
- With a constant share of RMNCH+A spending at 67% of total health spending, this will translate into an additional RMNCH+A spending of $12 billion by 2025 and $27 billion by 2035 (see Figure 9).
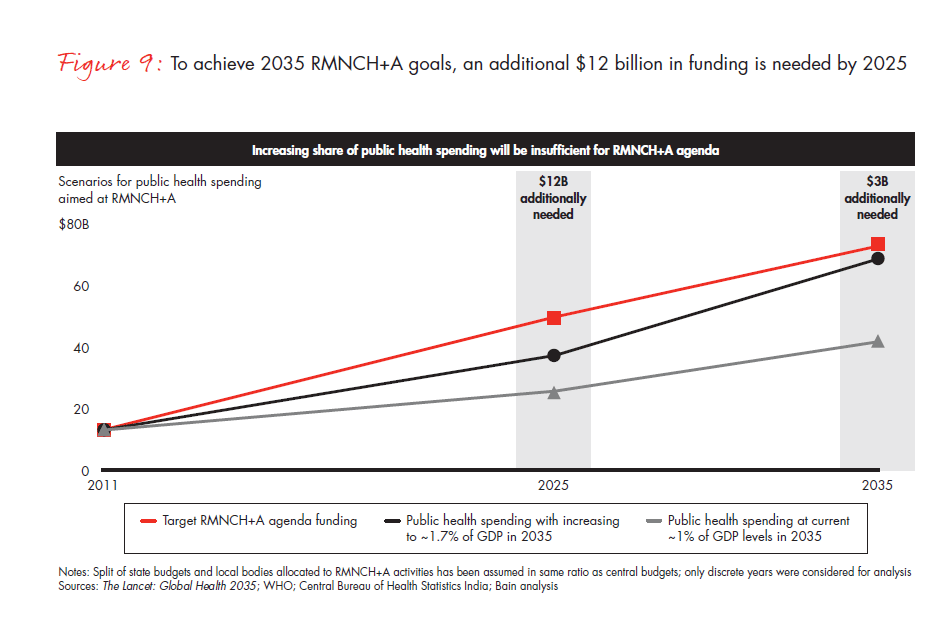
But despite government assistance, there will still be a gap in target RMNCH+A funding. In an ideal scenario, a short burst of more funding is needed until 2025. A gap of $12 billion will need to be filled by other sources focused on social systemic investments. Funding can then begin tapering off once maturity is achieved in 2035. Due to the continued investment through NHM and state bodies, an additional annual spending of only $3 billion will be needed.
In a less optimistic (and less likely) scenario, spending by the NHM and other bodies would remain at 1.5% of GDP in 2035. The gap would then be much larger than $3 billion and would be expected to reach $12 billion, Similar to 2025 requirements. Unless this support until 2025 continues, addressing the need for basic health services will take longer to accomplish.
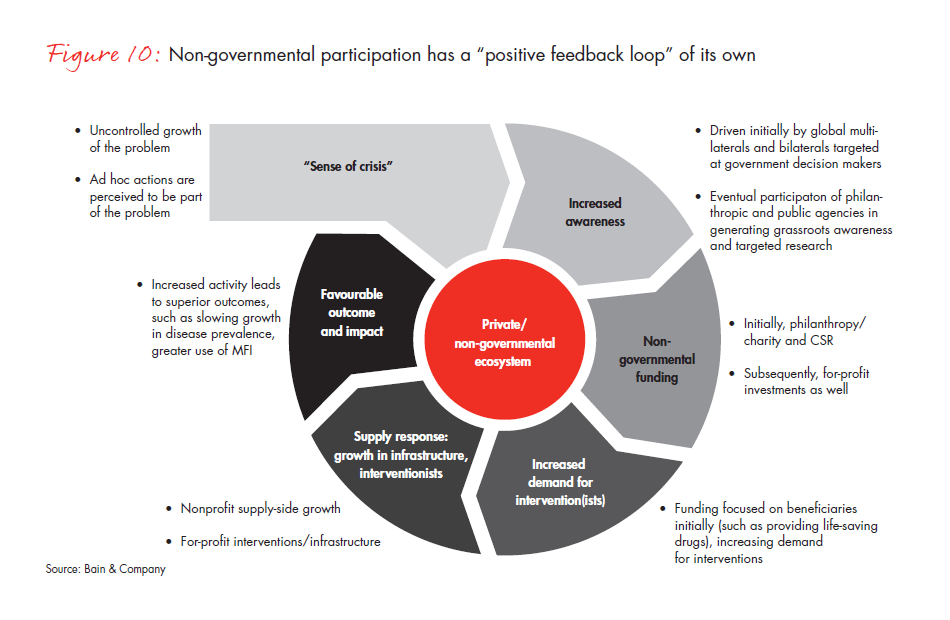
In either scenario, it is imperative that there be a strong push in non-state spending in the sector over the next 10 to 12 years, with a potential ramp-up after that time as the public sector completely fills the void (see Figure 10). This front-loading of investments in the healthcare system is a typical element of developing a mature ecosystem.
Investing in RMNCH+A has a positive impact on people and the economy
Preventing deaths creates value through additional life years, which is estimated to have contributed 11% of recent economic growth in low- and middle-income countries.
Low public spending on healthcare has resulted in India being far worse off than other similar income countries like China and Cuba (see Figure 11). Cuba has an economy devoted to healthcare, with the highest number of doctors per capita. Even China, with just 1% more of GDP spending on healthcare, is already at an under-five mortality rate of 14 deaths per 1,000 live births.
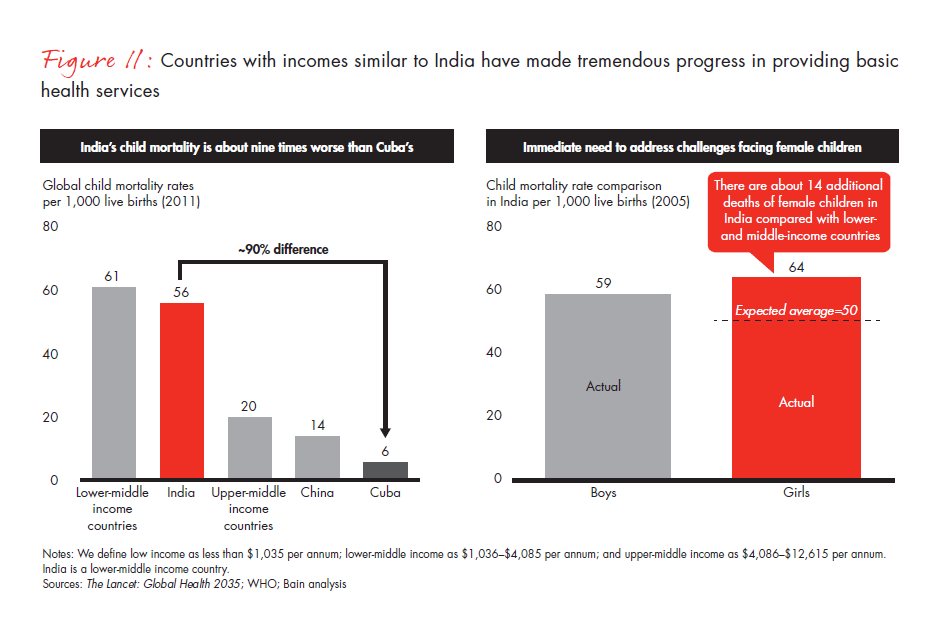
This shortcoming puts girls in India at a particular disadvantage. India’s mortality rate for girls is higher than those in most other low- and middle-income countries. In addition, by investing in healthcare, India can avoid the high cost of emergency care. India’s Planning Commission acknowledges that a poor primary health network, especially in the rural areas, has led patients to delay seeking treatment. Eventually, patients are forced to visit private hospitals, and many households spend 40% of their income on treatment. Where the government is unable to provide interventions, philanthropic organisations must step in and set up services on a larger scale.
The road to 2035
RMNCH+A will need to transition to a stage of rapid growth to make the sort of lasting social impact desired of an emerging economy. It has experienced a long period of stasis over the last 50 years, with only the last 20 years receiving significant attention. Clearly, a set of triggers is required to segue the ecosystem to this stage of rapidity, where each stakeholder will have to pull its weight in the transition.
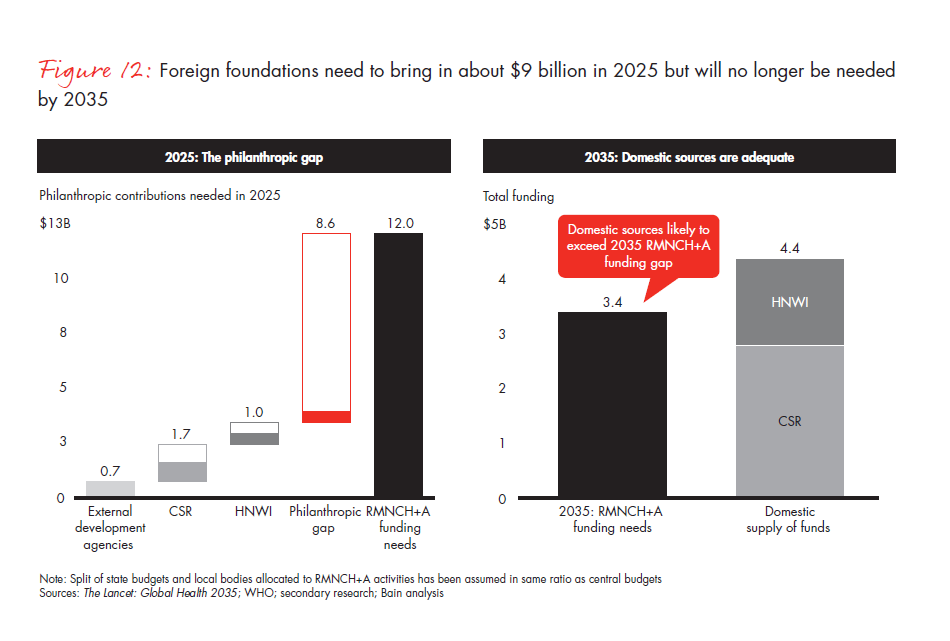
Funding from non-state sources will be critical to meet targets. Funding from donors will need to replicate the HIV story. A clear road map for 2025 and 2035 has been laid out (see Figure 12). The urgent need is quite evident: According to our estimates, only 7% of funding in this space comes from philanthropic sources, with the NRHM dominating the fund pool.
Corporate social responsibility is expected to take off. The new Companies Act formalises the role of corporate social responsibility (CSR) which is at 2% of profit after tax for big companies. This regulatory change is likely to unlock $3.7 billion in CSR total spending in 2014. However, this largely corporate kitty is highly competitive with several causes likely to compete for attention and spending, such as education and the environment. Public health accounts for 20% of the total CSR spending currently. Doubling contributions to healthcare with a constant share going to RMNCH+A funding in 2025 could contribute $1.7 billion (see Figure 13).
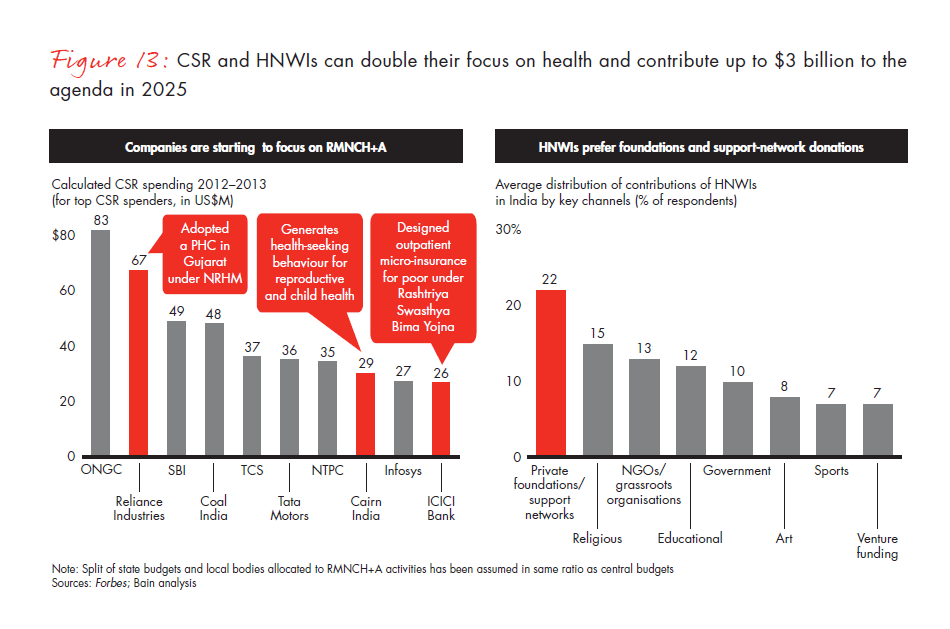
Positive outlook on HNWI contributions. Philanthropy by Indian HNWIs accounts for 0.1% of GDP. As Indians get wealthier by 2025, HNWIs can help plug the gap by $1 billion. Doubling the share healthcare gets from overall philanthropy could potentially raise an incremental $1 billion.
Bilaterals and multilaterals are unlikely to increase investments. Historically, these donors have had strong track records of funding Indian projects; however, going forward, as Indians become wealthier, their commitment may begin to weaken and funding levels may come down. By 2025, we don’t expect external donors to increase their contributions from their current levels (see Figure 14).
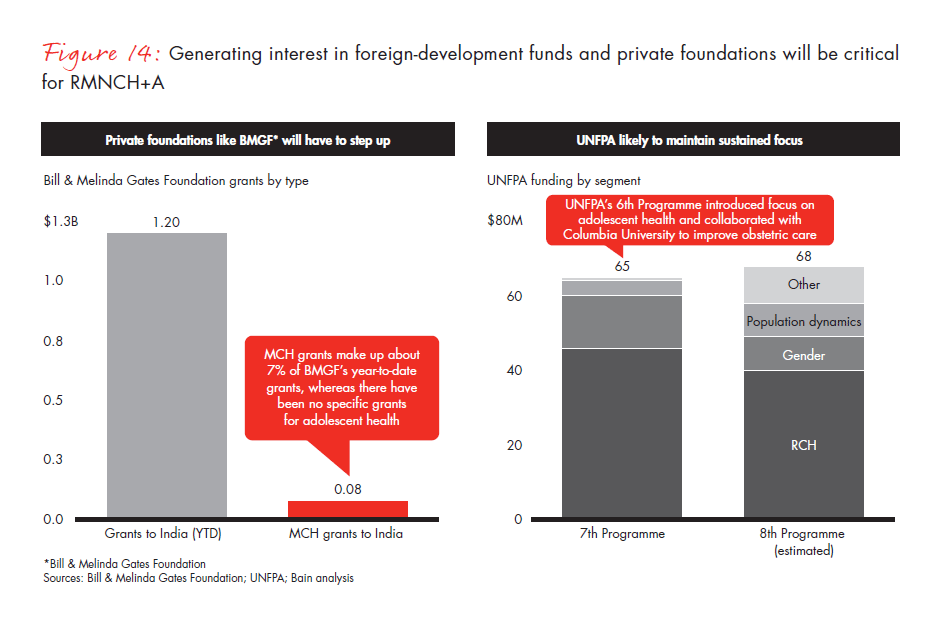
Private global philanthropy is likely to be the most important source of funds. Contributions from donors (both individuals and funds) abroad could be the game changer for RMNCH+A. In an upside scenario for corporate and individual philanthropy, along with external development funds, only $3.4 billion is accounted for. The rest of the $8.6 billion will have to come from these foreign donors. Large philanthropic organisations—such as the Bill & Melinda Gates Foundation, and the Michael & Susan Dell Foundation, among others—will have to realise their potential for making an impact and prioritise their contributions to improving women and children’s health.
Multisector partnership models like the “RMNCH+A Coalition”, where external funds, private foundations and the Indian government come together, can further provide critical funding and technical assistance that will help make the 2035 dream a reality.
Philanthropy will also need to strengthen other areas of the ecosystem
Support networks will need to support CSR funding. Given the rush of capital expected with the passing of the CSR bill, assessing the quality of grass-roots organisations has become most important. Corporations will need assurance that their money is being put to good use by competent organisations. Support networks will be critical to achieving this, by bringing experienced teams and best practices to conducing nonprofit due diligence (see Figure 15).
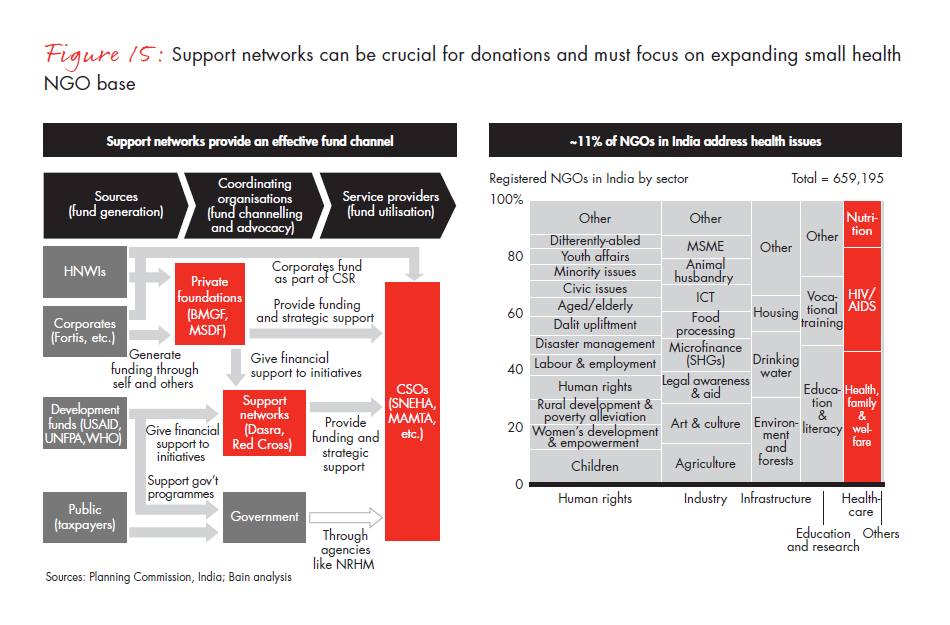
NGO participation needs to be formalized. NGOs are currently participating in a regulatory and legal vacuum, so a framework needs to be developed. Self-help groups need to expand their attention to health issues, and civil society organisations need to scale up. According to our estimates, the current coverage of 30 health-focused NGOs per 1 lakh women will need to increase to 125 per 1 lakh women if the scale of HIV is to be achieved. Clearly, potential exists for a large scale-up.
Government training programmes need assistance. Apart from a full-scale rollout of interventions, prioritised by the Ministry of Health and Family Welfare, nonprofits must also focus on training programmes for government field workers like ASHAs. This will improve the efficiency of established large-scale networks and create significant impact. Examples like the nursing institute set up by the Clinton Health Access Initiative for AIDS should serve as a useful template.
An integrated national health mission is the key to successful government intervention. Several issues on the priority agenda are likely to get impetus, with greater mindshare owing to the merger of the NRHM with its urban counterpart. More important, the share of funds left undisbursed will need to come down from the current 20% to 30% levels. Better process management and transparency of coordination efforts can help achieve this.
Coordination units will require last-mile expansion. The Rogi Kalyan Samiti societies pool funding from various sources and develop medical facilities and training institutes. They have remarkably achieved 77% coverage of primary health facilities across India. Village Health and Sanitation Committees engage people and officials in villages, as well as improve processes, to monitor field workers like ASHAs, and 75% of villages have been equipped so far.
Convergence of vertical health programmes is needed. Awareness of health issues must continue to be programme based, and a holistic awareness campaign is required to achieve long-term results. Ministry-level coordination needs political will to establish linkages with one another and reduce inefficiencies.
The delivery and support system needs to scale up with the help of innovative approaches to change
Better healthcare facilities are needed. The current system is skewed towards the urban tertiary care space and limited participation of the private sector (see Figure 16).
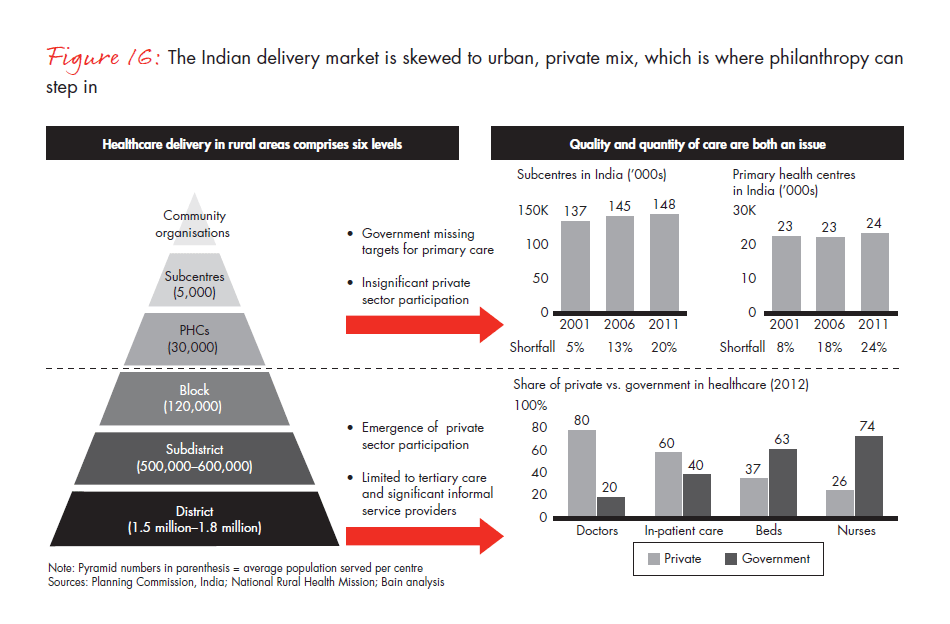
Infrastructure gaps will need attention if targets are to be reached. The availability of facilities such as subcentres, PHCs and CHCs fill some of these gaps and bring us closer to the government’s targets: Currently, there are 70 subcentres, 12 PHCs and 2 CHCs per 1 lakh women, respectively. These targets will need to keep expanding until 2035 to improve penetration in hilly and tribal areas, where health services are not currently available.
Workforce effectiveness needs improvement. Community workers like ASHAs and anganwadi workers have almost achieved government targets with current levels at 90%. A revamped training mechanism will need to be institutionalised, as many workers are semi-skilled and will need specific training.
It is estimated that 50% of the private sector network is in the informal sector. Regulating these networks and bringing them into the mainstream can help scale up quality interventions. Bangladesh, which has a much larger proportion of the informal private sector, has proved that this can also be a strength.
Academic institutions provide a platform for game-changing technologies. Academic institutions provide a suitable platform for incubator networks because talent, mentors and technology facilities are available. Rolling out such infrastructure requires active government support. The Israeli entrepreneurship success story proves that central policy making can create this support network from the ground up.
Successful awareness campaigns need to be replicated. Family planning awareness strategies through mass media registered substantial success. The achievement of infant mortality targets in Tamil Nadu generated large-scale news interest recently, and similar results will drive the awareness at all levels. That said, the need for the government to ramp up efforts is pressing. There are several other programmes that need similar treatment, such as anaemia, which has been troubling in recent times. Nonprofits too can support this area as they have done with HIV in the past.
Forge strong partnerships with diverse players. Multisector collaborations multiply the strengths of their participants, and this makes them an effective vehicle to implement initiatives. Public, private and nonprofit participation models need encouragement.
Help technologies achieve scale. Social enterprises like Embrace have proved that technology can alter the RMNCH+A landscape. Impact investment funds and donors can support this area, especially to scale up promising concepts. The next few years will need to see successes in areas like mobile health, with the help of global innovation.
Target outreach at the community level. Services need to be deployed at the grassroots level. The World Health Organization’s research has established that a 20% increase in community interventions can save the lives of 486,000 women, infants and children. This can be achieved at a cost of $1.2 per capita. Quality improvements in facility-based care can save an additional 105,000 lives at a cost of $0.5 per capita. Preventive care during childbirth can reduce maternal mortality by 29%, and training of skilled birth attendants can reduce infant mortality by 27% from current levels.
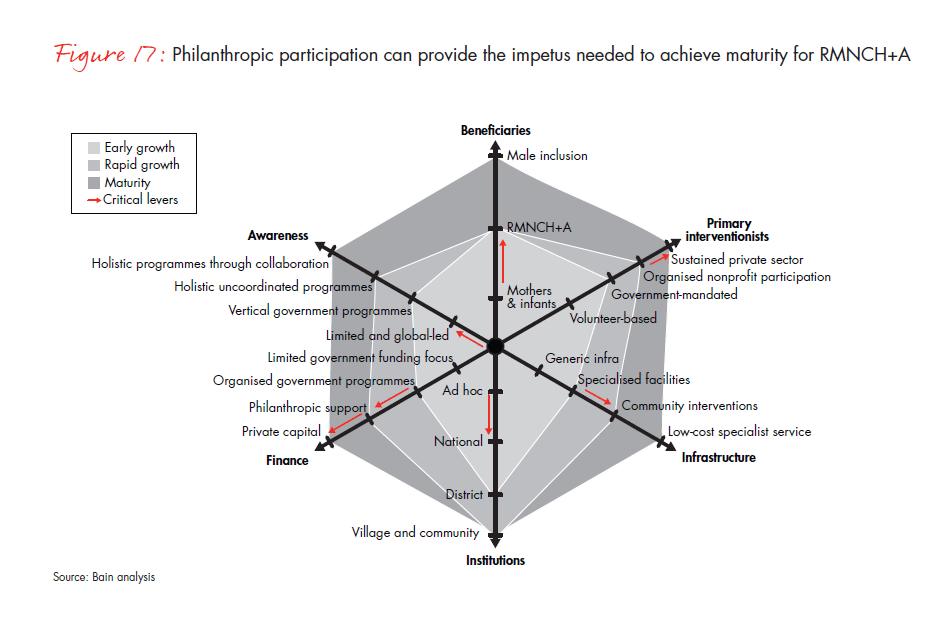
In summary, there is clear evidence that tackling RMNCH+A in India is realistic and feasible (see Figure 17). By realizing the clear importance of this space to the long-term social goals of India, the public machinery has started gathering momentum. With the right support from the private and philanthropic sectors, we will hopefully see a much-needed change.
Arpan Sheth is a partner with Bain & Company in Mumbai. He leads the firm’s Private Equity practice in India. Karan Singh is a partner based in Bain & Company’s New Delhi office. He leads Bain’s Healthcare practice in Asia-Pacific. Dinkar Ayilavarapu is a principal with Bain and is a member of the firm’s Healthcare practice based in New Delhi.
Dasra is India’s leading strategic philanthropy foundation that works to build ecosystems that bring together knowledge, funding and people for social change. Dasra ensures that strategic funding and capacity building skills reach nonprofit organisations and social businesses, thereby enabling 700 million Indians to move out of poverty faster. In order to empower adolescent girls and address the healthcare needs of the mothers and children in the country, Dasra has launched a five-year, $14 million initiative in collaboration with USAID and Kiawah Trust to build an ecosystem that fosters innovation, improves outcomes and reaches scale.
















