Report

At a Glance
- The payer sector continued to have the most modest buyout activity in healthcare in 2018, accounting for $1.1 billion in disclosed deal value, which excludes the undisclosed naviHealth buyout by CD&R, across 11 deals.
- Most deal activity focused on HCIT and other service segments that enable payers to operate more efficiently.
- Corporate buyers continue to be more active than buyout firms, as large traditional health plans vertically integrate and seek operational efficiencies.
This article is part of Bain’s 2019 Global Healthcare Private Equity and Corporate M&A Report. Explore the contents of the report here or download the PDF to read the full report.
Activity in the payer and related services sector in global healthcare private equity stayed relatively flat during 2018, as deal volume fell to 11 in 2018 from 13 in 2017, while disclosed values increased to $1.1 billion from $220 million in 2017 (see Figure 7). Despite relatively modest activity, there was increased interest for payer services, especially at the intersection of provider as risk-bearing organizations begin to contemplate value-based care models.
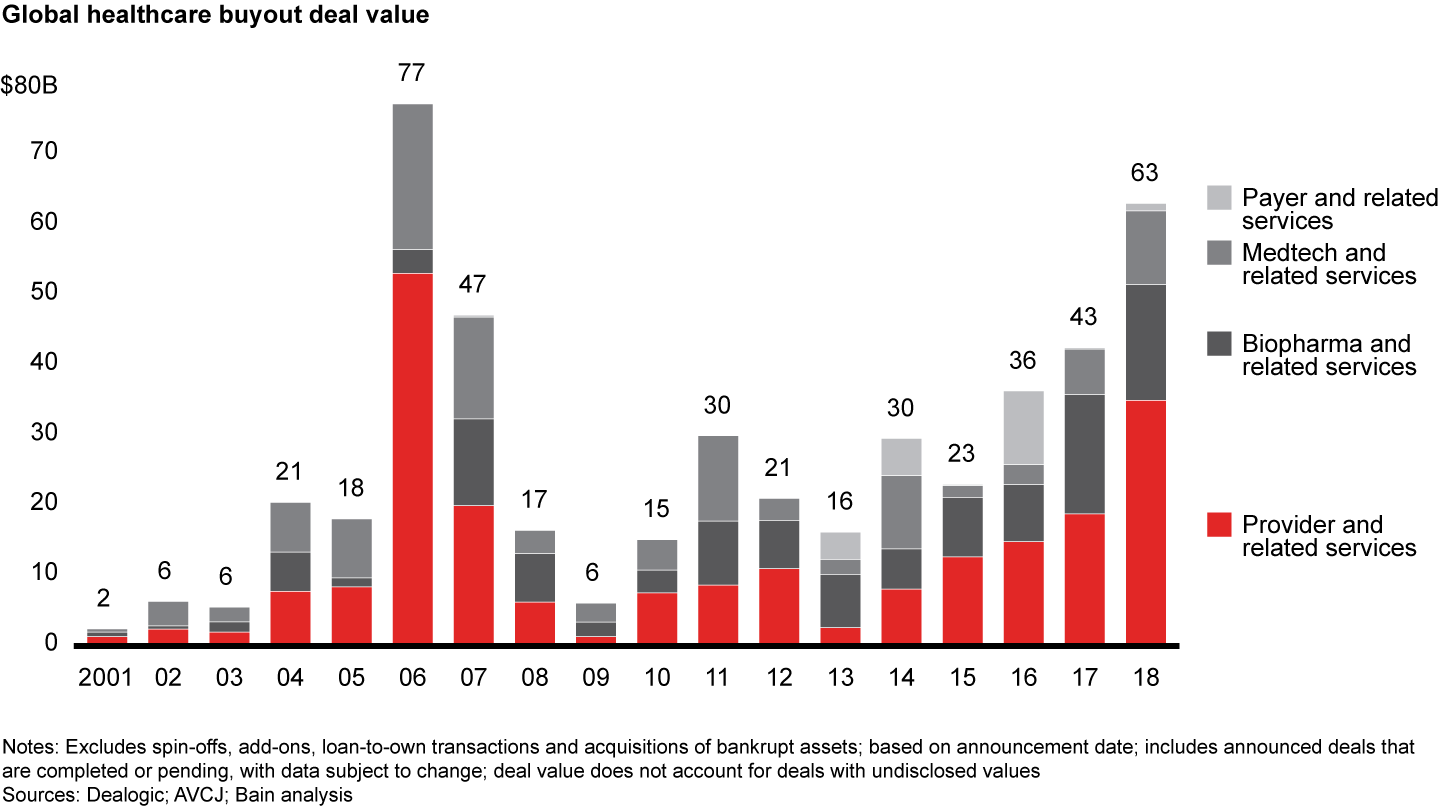

Investors displayed increasing interest for payer and related services in 2018 as both funds and corporates made intriguing investments across the payer landscape. While the payer sector continued to experience the most modest buyout activity in healthcare, accounting for just $1.1 billion across 11 deals in 2018, there were also several notable portfolio add-on and corporate investments made throughout the year. While deal count remained relatively consistent with 2017, deal value rose because of a single large transaction: WestBridge Capital and Madison Capital Partners acquired Star Health and Allied Insurance, a standalone Indian health insurer, for $1 billion. The total disclosed deal value does not include notable transactions such as naviHealth or Cotiviti.
Total disclosed values vary from year to year in the payer sector because only a few large assets get acquired. For example, in 2016, two megadeals, MultiPlan and ExamWorks, closed for a combined $9.7 billion. In 2017, the largest deal was the $200 million acquisition of Indian health insurance company Religare Health Insurance by a consortium of buyers.
India may have had the largest deal of the year, but North America continues as the most active region in deal count. The region saw all payer activity aside from the Star Health and Allied Insurance transaction. The US historically has accounted for the most investment activity as the complicated patchwork payment environment represents opportunities for innovation and more service providers.
Given stiff competition from corporate acquirers better suited to pay a premium for payer-related assets because they can integrate them into existing operations, PE investors have had to settle for relatively few investment opportunities. Traditional health plans in the US are vertically integrating to better control costs throughout the system, from providing healthcare services to dispensing prescription drugs. For example, the second-largest corporate acquisition of 2018 occurred in the payer space, with health insurer Cigna Corporation buying pharmacy benefit manager (PBM) Express Scripts Holdings for nearly $70 billion. Further, corporate payers believe that disruptive primary care can reduce healthcare costs and provide better patient outcomes. That’s the logic behind UnitedHealth Group’s intended purchase of DaVita Medical Group, which focuses on primary and urgent care services, announced in December 2017 for $4.9 billion. Payers also are partnering with providers to deliver healthcare, such as Humana’s partnership with Walgreens to pilot senior-focused primary care clinics (see “Provider and related services: Intense competition and a push into new segments”).
The vast majority of payer investment historically has gone to services and HCIT assets that help payers operate more cost effectively. Aside from a few deals in Asia, funds find it cost prohibitive to invest directly in payers. Nine of 11 deals in 2018 involved either services for traditional payers or HCIT assets catering to payer clients. For example, Francisco Partners completed a take-private transaction of Connecture, which offers a personalized online health insurance marketplace that allows health plans, brokers and exchange operators to improve the accuracy and efficiency of their insurance distribution. And Veritas portfolio company Verscend acquired Cotiviti, which provides payment accuracy and analytics solutions for healthcare organizations, for $4.9 billion.
Several deals sit at the intersection of the provider and payer sectors, with the intent of reducing costs across the system. This is timely as players prepare for the inevitable but gradual shift from fee-for-service to more value-based care models. For example, General Atlantic backed in-home care provider Landmark Health, which is focused on managing complex patient populations. And in another prominent example, CD&R acquired a majority ownership in naviHealth from Cardinal Health for an undisclosed value. NaviHealth provides technology-enabled data analytics and post–acute care management expertise to help providers manage the appropriate length of stay, tier of care, and network for patients in order to limit hospital readmissions and reduce costs. NaviHealth also provides technological support services to providers that participate in the BPCI program, which is a Centers for Medicare and Medicaid Services–led initiative designed to link payments and accountability for the multiple services patients receive during an episode of care. The program is now beginning its second phase following a well-received first phase, and while there continues to be excitement about its possibilities, it is too early to determine the longer-term implications for providers and other risk-bearing entities. Similarly, New Mountain Capital invested in Remedy Partners, which provides software and services that enable payers to manage bundled payment models.
Payer services assets supporting worksite healthcare have also been popular with investors as organizations continue to seek comprehensive, high-quality care for their employees while lowering costs. For example, OMERS Private Equity invested in Premise Health, a US-based provider of workplace health and wellness solutions. Additionally, Vista Equity Partners acquired Alegeus Technology, a healthcare benefits administrator with a consumer healthcare funding platform that helps support benefits management for 225,000 employer groups.
We expect payer-related buyout interest to remain high but deal activity to remain modest in 2019 because of continued competition from corporate acquirers that can justify higher premiums and investor concerns about competing in a consolidated landscape. Early 2019 indications, however, suggest that a few scale opportunities may become available for buyout funds through either direct investment or as an add-on acquisition to existing portfolio companies. Buyout activity will likely concentrate in payer services and HCIT assets that help payers operate more efficiently, help ease the shift to fee-for-value payment models and help payers connect more deeply with engaged consumers. Over the long term, investors will want to keep an eye on trends in consumer engagement and payment as well as technologies that have the potential to disrupt the payer and provider services landscape—for example, automation and machine learning tools applied to administrative functions such as billing and coding or more sophisticated applications such as network models or clinical pathways. Over the next few years, though, we expect competition for payer services assets to intensify as major health insurers continue to bring more services in house.