Report

In evidenza
- In 2018, the UK’s National Health Service received a long-overdue budget increase: £20 billion annually through 2023. But funding alone will not help the resource-stretched NHS keep pace with growing demand.
- A transformational approach is needed—one grounded in strategic investments and deep engagement of frontline physicians. But which investments are best? And how can the NHS reinvigorate its demoralised front line?
- Our 2018 UK Front Line of Healthcare Survey tackled this question, revealing five strategies for boosting service delivery through investments in innovation, operational efficiencies and, above all, frontline engagement.
The UK’s National Health Service (NHS) turned 70 years old in July, an occasion that was marked by the government’s commitment to increase the health system’s budget by £20 billion annually through 2023. No doubt, this was welcome news to the healthcare system’s frontline providers who have laboured under anaemic spending for nearly a decade.
But the system is straining under burdens that will not be alleviated by more spending alone. If it is going to remain viable for the next 10 years—to say nothing of the next 70—the NHS needs to adopt a transformational approach. New models leveraging technology and realising the full potential of the workforce must be implemented for the resource-stretched NHS to keep pace with growing demand. Key to this will be the engagement of the physicians who serve on the front line.
To dig deeper into the challenges and opportunities facing the NHS, Bain & Company surveyed 1,156 physicians and 154 procurement officers from Germany, France, Italy and the UK. Of these, 324 physicians were from the UK. The resulting 2018 UK Front Line of Healthcare Survey reveals a healthcare system at a crossroads.
Our survey found that for any significant transformation efforts to stick, physicians will need to truly believe in, and commit to, helping to shape improvements—yet morale is at an all-time low. In fact, the NHS has the lowest physician Net Promoter Score® among its peers from other major European countries. Furthermore, physicians feel they have little visibility into, or ownership of, shaping change. Perhaps that is why a majority of respondents do not believe that integration between primary and secondary care will happen over the next three to five years.
Notably, 14% of NHS doctors expect to change their profession or leave the country over the next five years, amplifying the pressure on an already overburdened workforce. Given these sentiments, it’s no surprise that 91% of the physicians we surveyed do not expect the NHS to survive another 20 years in its current state.
The sources of frontline disengagement are manifold. Years of inadequate funding and pay freezes have gradually eroded morale. Recently announced salary increases may help. Yet below the surface are other, more systemic factors that cannot be easily addressed with a simple funding boost. Metrics that have focused on process measures, rather than patient outcomes, have contributed to a sense of physicians feeling undervalued. Operational inefficiencies resulting from too many hospitals and not enough world-class centres of excellence (CoEs) are stretching already scarce resources. And the large-scale adoption of digital innovation to improve productivity has thus far eluded the NHS.
But with the new tailwind arising from additional funding—and hopefully a bolder ambition to innovate—there is an opportunity to revitalise frontline engagement. Our survey uncovered five key strategies for boosting service delivery, starting with setting a bold vision for NHS trusts as catalysts for sustained systematic change that goes beyond a myopic in-year, acute-care view. The NHS should also encourage consolidation, led by trusts that have demonstrated a proven model of best-in-class clinical outcomes and economic productivity. Most importantly, the NHS needs to commit to instilling the most vital enablers for this transformation—namely, clinician empowerment, a high-quality leadership development programme, and focusing technology investment on use cases with established improvement in clinical outcomes and/or productivity.
The survey findings underscore how critical it will be for the NHS to invest in solutions that support innovation, operational efficiencies and frontline engagement, rather than simply bandage over legacy issues. To be successful, decision makers will need to tackle the issue of a disheartened healthcare front line. But by advancing an ambitious agenda—one that engages and empowers physicians in setting and pursuing a superior model for healthcare delivery—the NHS will be better positioned to continue delivering high-quality care in a changing economic landscape.

Challenges, Opportunities Facing the UK’s NHS
A closer look at the areas the National Health Service can focus on for a successful transformation.
Disempowered and unengaged
Persuading frontline physicians to adopt new processes, tools and mindsets will be essential to making successful and sustainable improvements throughout the NHS. Yet deep dissatisfaction among physician ranks could hinder long-term improvement efforts.
Our 2018 survey revealed an alarming rise in physician disillusionment, as indicated by the Net Promoter Score. Between 2016 and 2018, the NHS’s Net Promoter Score declined by 30%, putting the health system last among its comparable European counterparts. This is a sharp reversal from 2016, when the NHS was a leader on Net Promoter Score. In the span of just two years, two times as many physicians have become detractors, rather than promoters, of the NHS (see Figure 1).
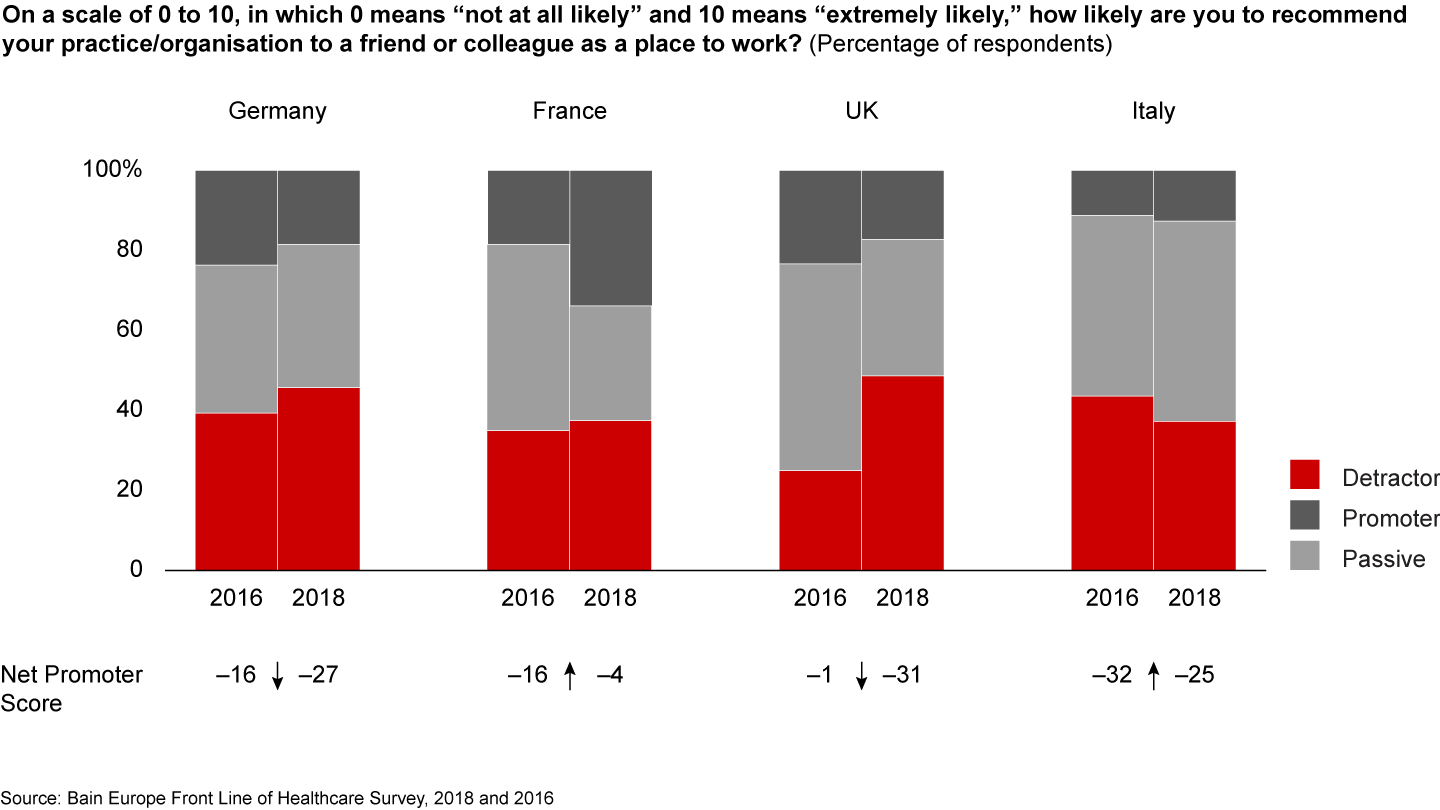

In light of these findings, it is not surprising that 9 out of 10 NHS physicians do not expect the NHS to survive in its current state. Specifically, 91% of doctors believe the NHS will not survive another 20 years without major reforms (see Figure 2).
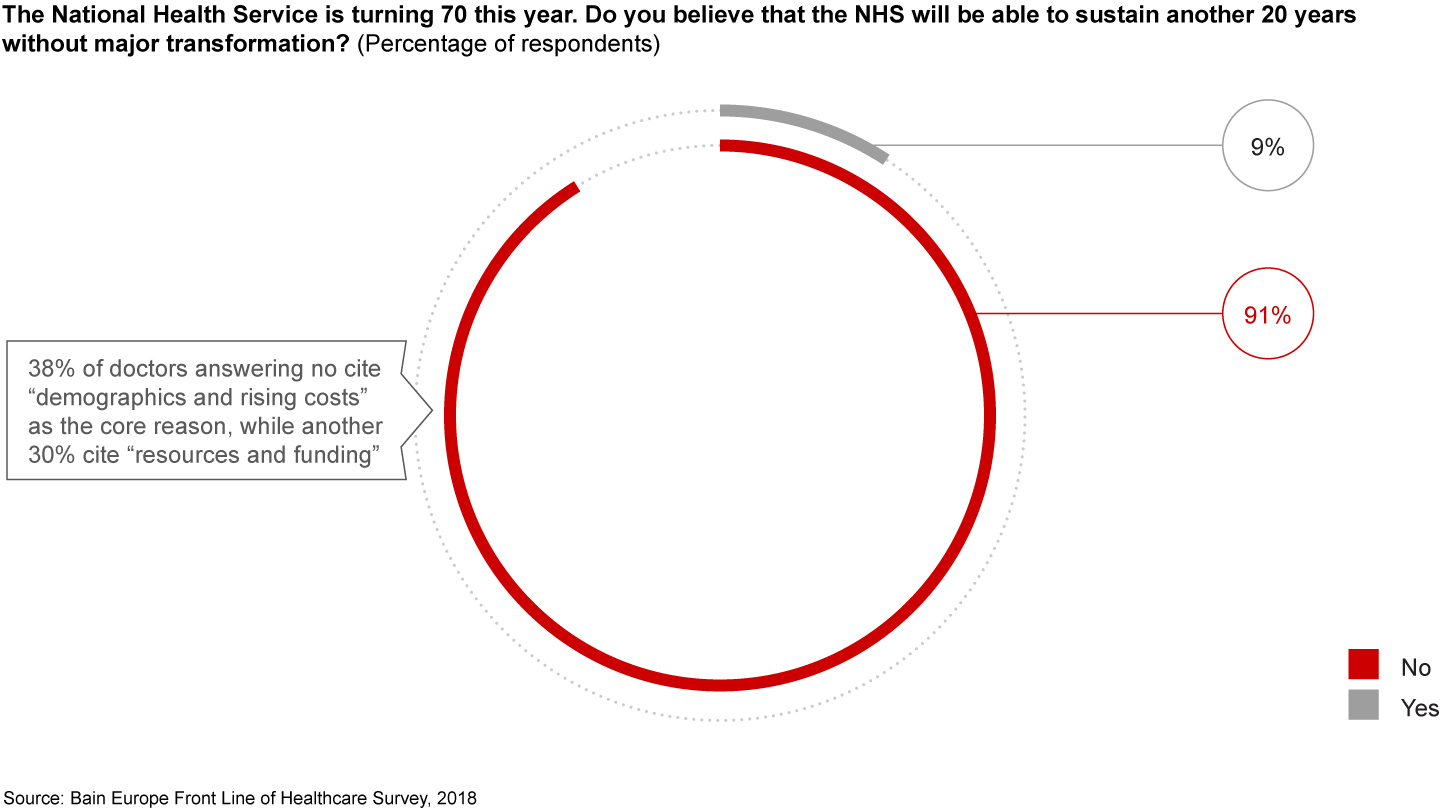

Recognising the need for transformation, however, does not always translate into the enthusiastic embrace of new strategies or processes. Physicians who do not understand the course of action will be less likely to buy into, much less rally around, sustainability and transformation partnerships (STPs).
Indeed, our survey found that three out of four hospital physicians have no or limited understanding of the STPs affecting their hospital (see Figure 3). Likewise, The King’s Fund reported that, together with general practitioners (GPs) and primary care teams, clinical engagement in STPs has also been weak. Furthermore, a recent study conducted by the Hospital Consultants and Specialists Association concluded that hospital physicians are unhappy with their own lack of engagement, fear that it will lead to negative patient outcomes and are undecided as to whether to support STPs.
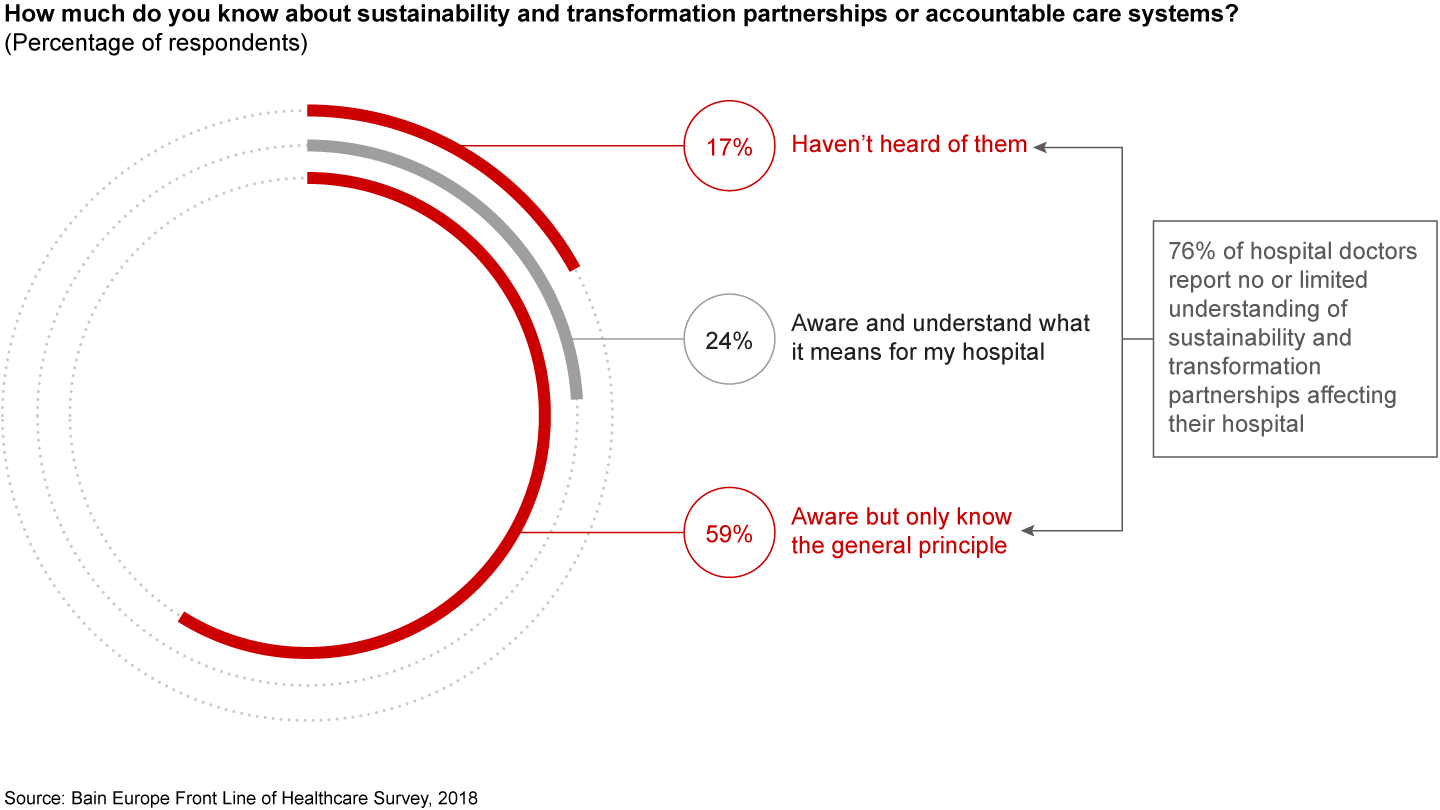

The front line must engage early and often to spur success, or else current STPs are unlikely to deliver on their promise. Given the limited level of clinical engagement, it is unlikely that current STPs will fulfil their comprehensive potential.
Predictably, this lack of frontline engagement and limited understanding of STP objectives has led to a crisis of confidence among NHS physicians. Only 7% of respondents believe that the integration of primary and secondary care will happen during the next three to five years, delivering positive patient outcomes or cost efficiencies. More than 65% of physicians believe that integration will not happen during the next three to five years. The remaining percentage of respondents feel that it will happen over the next three to five years and that it may deliver some benefits (see Figure 4).
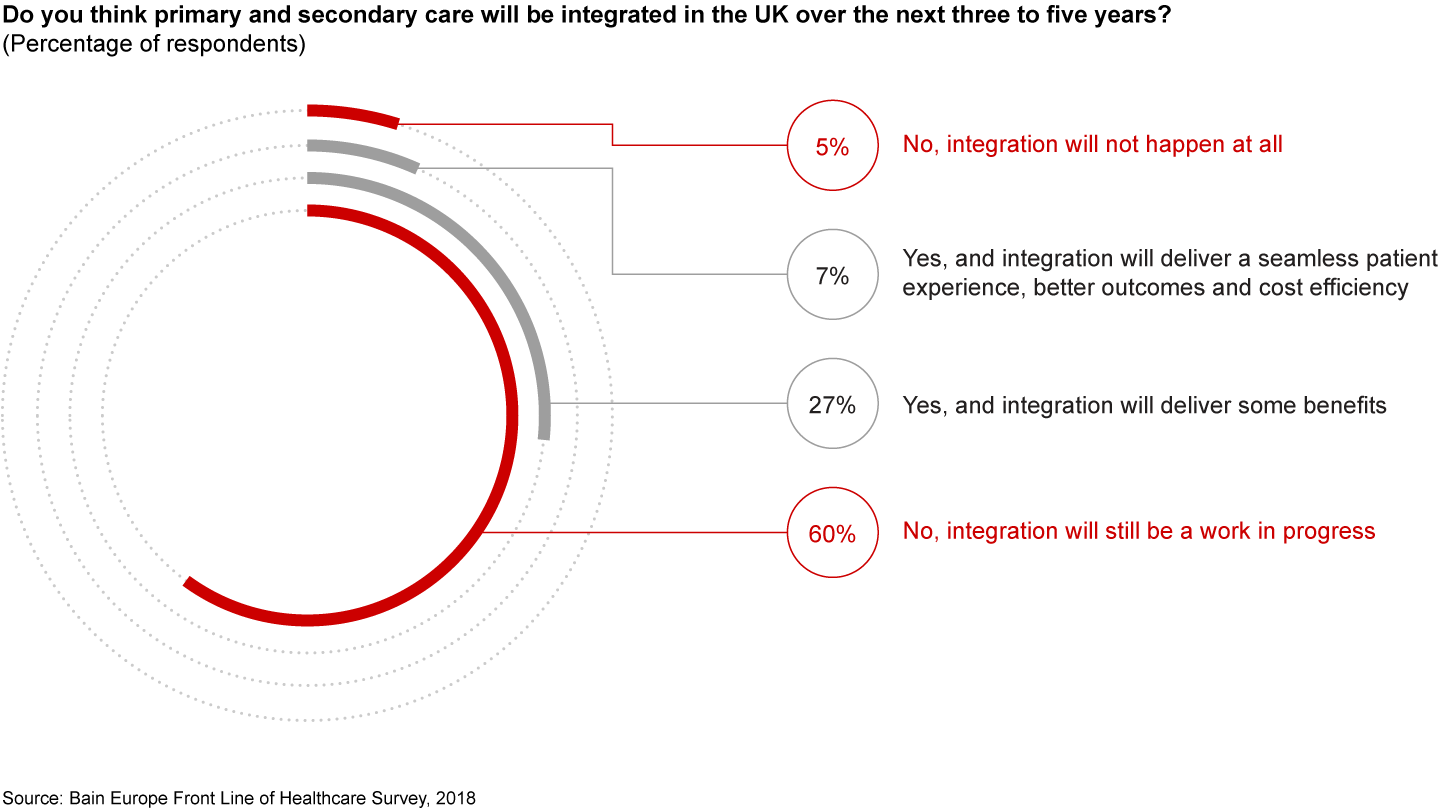

This dissatisfaction, combined with pessimism about the likelihood of meaningful improvements, could escalate the already high attrition rate for NHS physicians. Only 38% of doctors answered “very” when asked how likely they were to remain with the NHS over the next five years; 62% of the same cohort indicated that they would've been "very" likely to remain with the NHS if asked the same question five years ago. Also, 14% have indicated that they wish to either leave the profession or move to another country over the next five years; only 5% of the same cohort indicated that they would've had similar wishes to exit the NHS if asked the same question five years ago (see Figure 5).
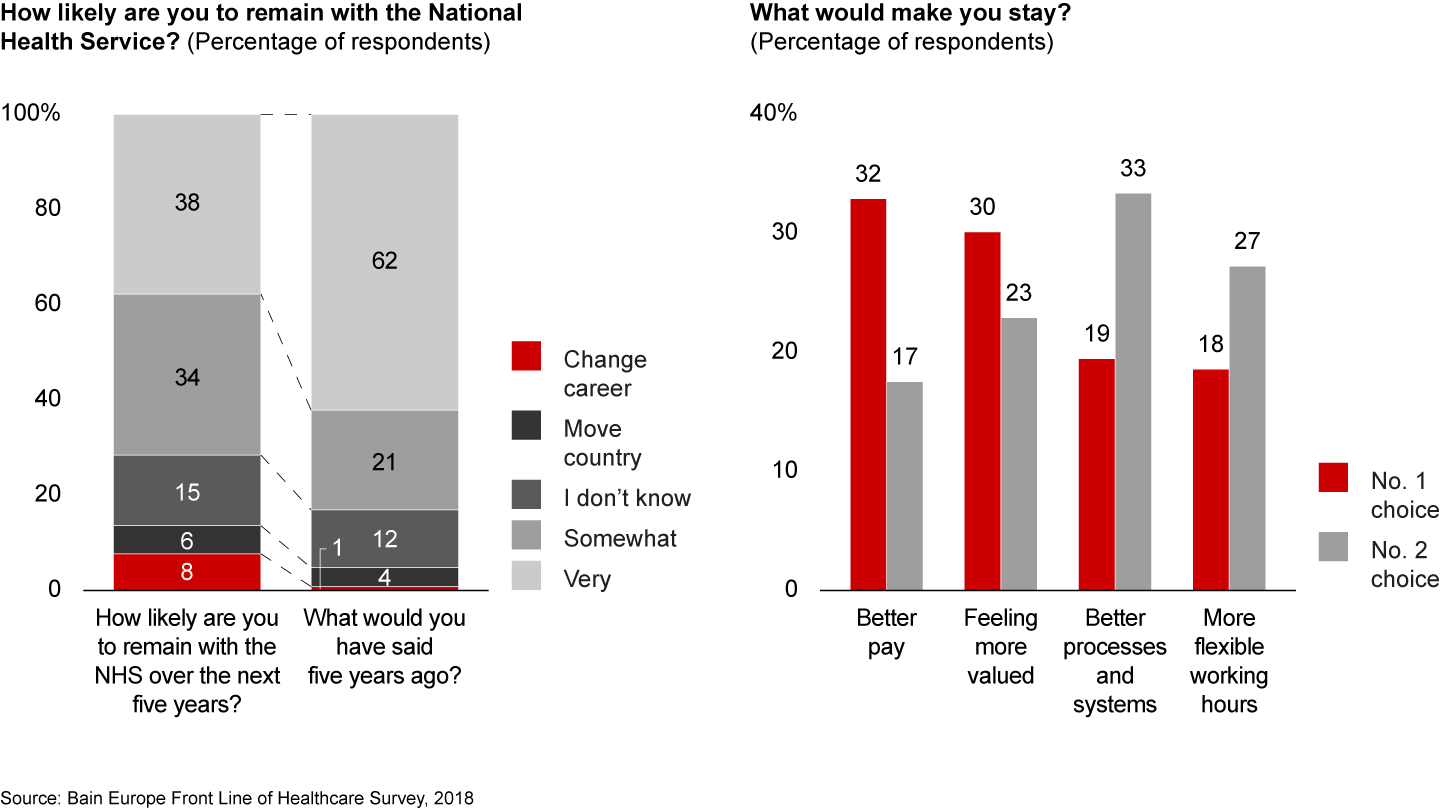

This potential exodus of qualified physicians will compound the existing staffing crisis within the NHS as demand for high-quality care outpaces available resources. Stemming this crisis will require the NHS to understand the sources of disaffection so that they can adequately address them.
Multiple factors cause frontline disengagement
Flat spending levels and deeply rooted operational inefficiencies have conspired to dampen frontline provider engagement. The 2018 Bain survey discovered five primary factors that are contributing to this decline.
Factor No. 1: Historically flat funding for healthcare. The UK’s spending on healthcare as a proportion of GDP has long been lower than that of comparable European peers (see Figure 6).
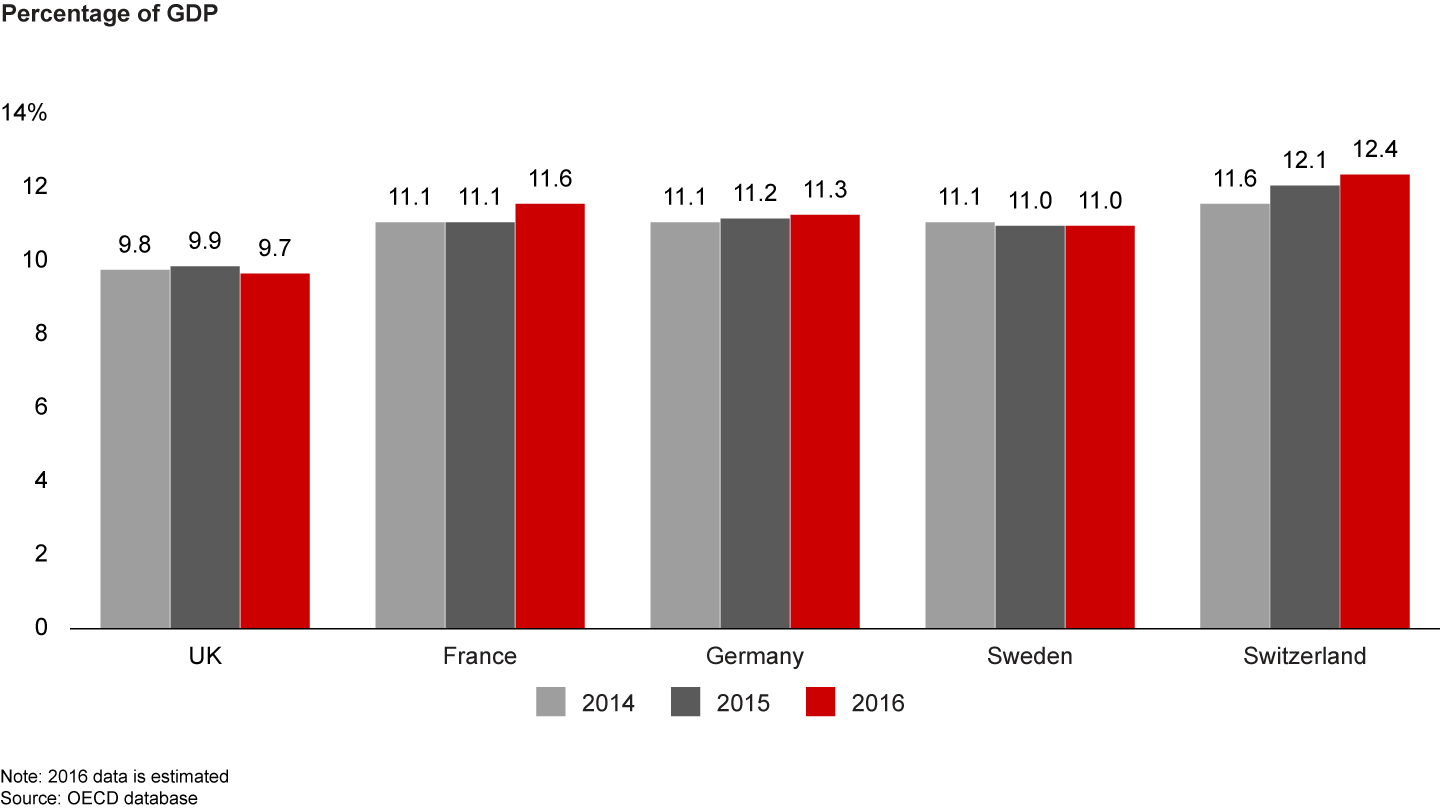

Though NHS funding has increased year over year to reach £124.7 billion in 2017–2018, growth has been far below historic levels. Between 2010–2011 and 2016–2017, health spending increased by an average of 1.2% above inflation. These increases are set to continue in real terms at a similar rate until the end of this parliament. This is far below the pre-2010 NHS annual inflation-proof growth rate of almost 4% that stretched back to the 1950s.
The flat budget is problematic for a host of reasons, including ever-increasing strains from higher demand, advances in medical technology, increased cost pressures from a growing and ageing population, and the rise of chronic diseases. Most tellingly, respondents who are contemplating leaving the NHS state that better pay is the No. 1 factor that would persuade them to stay.
Factor No. 2: Targets focus on process measures rather than outcomes. Inadequate funding is not the only source of discouragement for physicians. Over the past 25 years, successive governments have set a series of national targets for the NHS. While these targets have had an overall positive impact on patient care, they have also had unintended consequences that have compounded over time.
For example, top-down targets have segmented the NHS into silos by focusing on specific parts of the system rather than taking a holistic approach. Moreover, these targets generally reward providers for focusing on short-term goals to the detriment of enduring, long-term institutional improvements.
In addition, the majority of these targets are process oriented and input driven, rather than patient centric or outcome driven. As hospitals pivot to accommodate these national targets, frontline providers are forced to absorb the pressure of this operational shift. Physicians and frontline workers carry the burden of meeting targets when their focus should be on treating their individual patients. Ultimately, these targets, though well intentioned, have diminished staff motivation.
Factor No. 3: Trusts provide too many competing services. The NHS has been hamstrung by over-seeing many of the same hospitals it inherited with its creation in 1948. The majority of these hospitals provide similar acute care and elective services, and some are located just a few miles apart. The NHS has successfully reduced the number of hospital beds over the past 30 years in response to changes in clinical practices. Yet room for improvement remains: 152 acute trusts in England still operate around 200 to 300 hospitals.
This duplication has resulted in a lack of staffing levels, expertise and resources to deliver higher-quality care. For example, research conducted by the Royal College of Paediatrics and Child Health concluded that the NHS’s 220 specialist paediatric units should be reduced to 170. In addition, a higher number of NHS hospital trusts are facing financial deficits, even as workloads increase. Case in point: Four times as many trusts presently have a financial deficit when compared with less than five years ago (10% in 2012–2013 vs. 44% in 2017–2018). Indeed, less is more (see Figure 7).
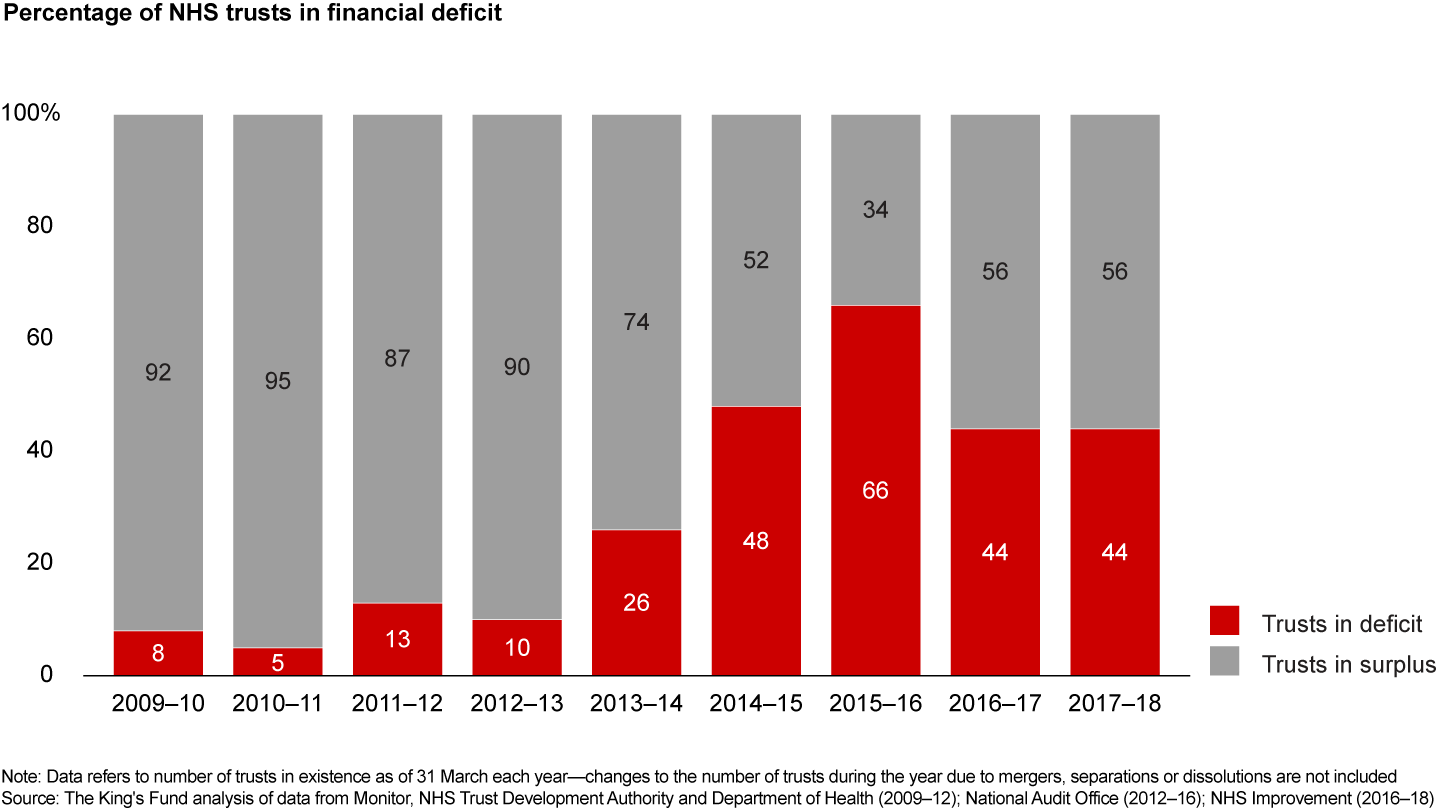

Factor No. 4: Provider inertia in scaling up technology and fragmentation of resources for digital innovation. Digital and IT practices have by far the greatest impact when compared with other initiatives (see Figure 8). In line with this, Prime Minister Theresa May has called for digital innovations to help transform and ease pressures on the NHS. The NHS has historically struggled, however, to apply technology effectively to drive improvement or realise efficiencies. Only 15% of physicians reported seeing an example of a pilot or best practice of a technology solution that has the potential to scale across the UK (see Figure 9).
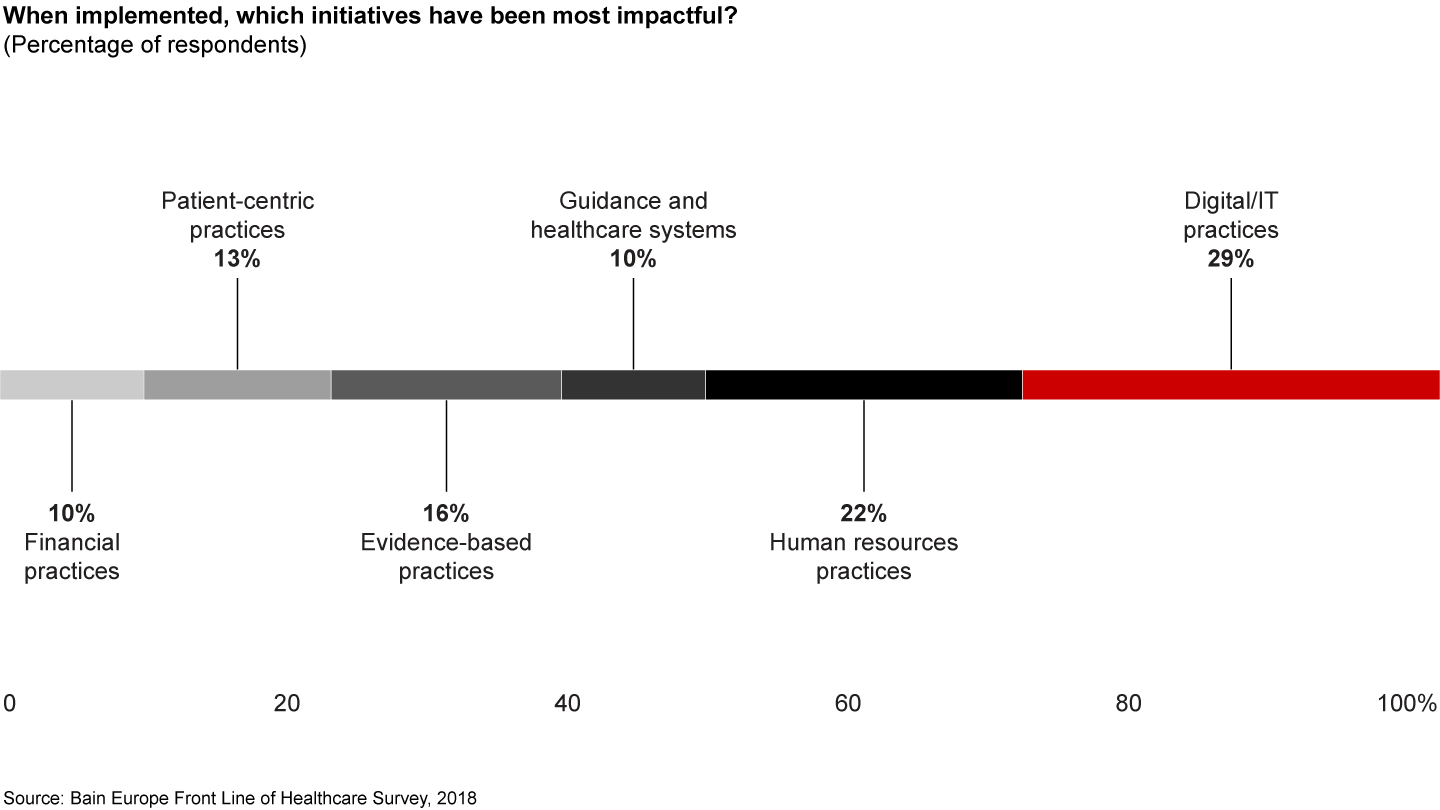

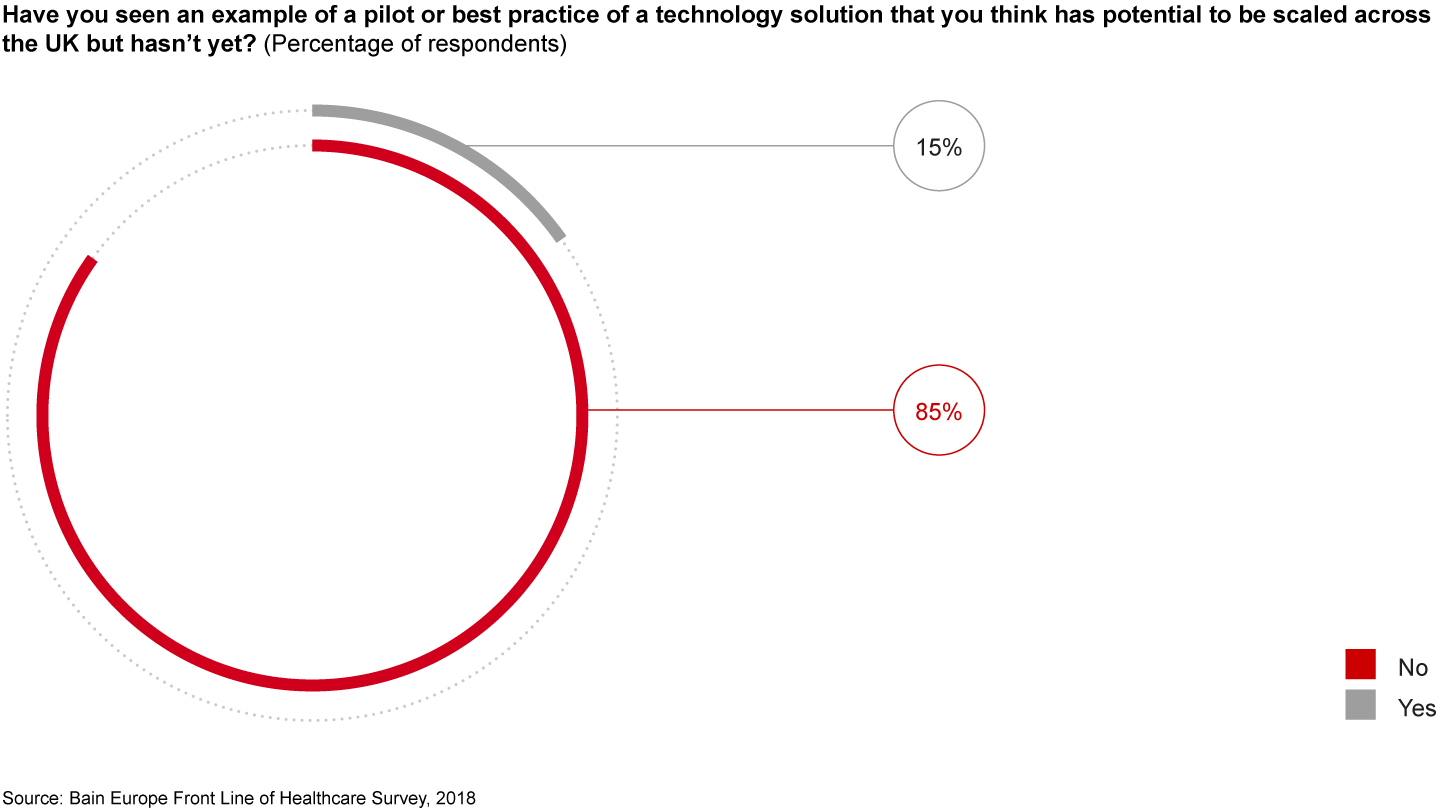

Historically, the NHS has been slow to adopt these technologies due to a lack of understanding of the use case, applicability, limited scaling across sites and not collaborating with the right external partners.
Looking forward, Secretary of State for Health and Social Care Matt Hancock recently announced a £500 million package to help jump-start the rollout of innovative technology across the NHS. The majority is earmarked for new technology in hospitals to improve access and safety.
Factor No. 5: Pay freezes. Despite growing its workforce over the past five years, the NHS continues to experience a chronic shortage of physicians across most areas of medicine. The British Medical Association reported that nearly three-quarters of all medical specialties had unfilled training posts, and dozens of specialties must make do with annual recruitment shortfalls. Fewer trainees are moving directly into specialty training; instead, they are choosing to take a career break. This, coupled with the chronic GP shortage, suggests that it is unlikely that the NHS will recruit the required number of physicians to meet demand effectively.
Pay freezes have certainly not helped the situation. For seven years, frontline providers have endured frozen wages, followed by salary increases capped at 1%, as part of the government’s austerity programme. Such measures amounted to an effective pay cut, as these restrictions do not allow salaries to keep pace with the rising cost of living. Combined, these factors have resulted in the front line inching closer to the breaking point.
The recent announcement regarding salary increases for NHS staff is no doubt welcome, but only time will tell if it will yield results.
Five priorities for investment
Increased funding will bring much-needed relief to a system that is struggling to satisfy demands. To make the most of its investment, the government should focus the majority of its funding on innovation in care quality. Our survey found five key areas in which to deploy the funding for best use.
Priority No. 1: Create an enterprising vision for NHS trusts. The NHS needs to set a bolder ambition for its trusts. This should start with a three- to five-year vision and a strategy for world-class care provision. By getting this right within the trusts, the vision can become a catalyst for system-wide integration.
Even though widespread integration between primary and secondary care will face some challenges in the short to medium term, an opportunity for integration and service redesign within secondary care itself could materialise. Spending on secondary care constitutes the majority of the NHS’s budget, making it paramount that secondary care services are efficiently designed to avoid compromising patient outcomes.
In addition, the NHS should employ a wider system service-line review to ensure the highest quality of service while realising economies of scale. Although it is increasingly common for trusts to deliver some secondary care services jointly, further integration and formation of CoEs would expedite reform. These CoEs could define global standards in outcomes and productivity, together with leading research and developing international expertise.
Moreover, our survey suggests that creating CoEs would have the backing of the healthcare front line. The majority of physicians support the formation of CoEs, and nearly two in three physicians expect the formation of CoEs to improve patient care as well as cost effectiveness (see Figure 10).
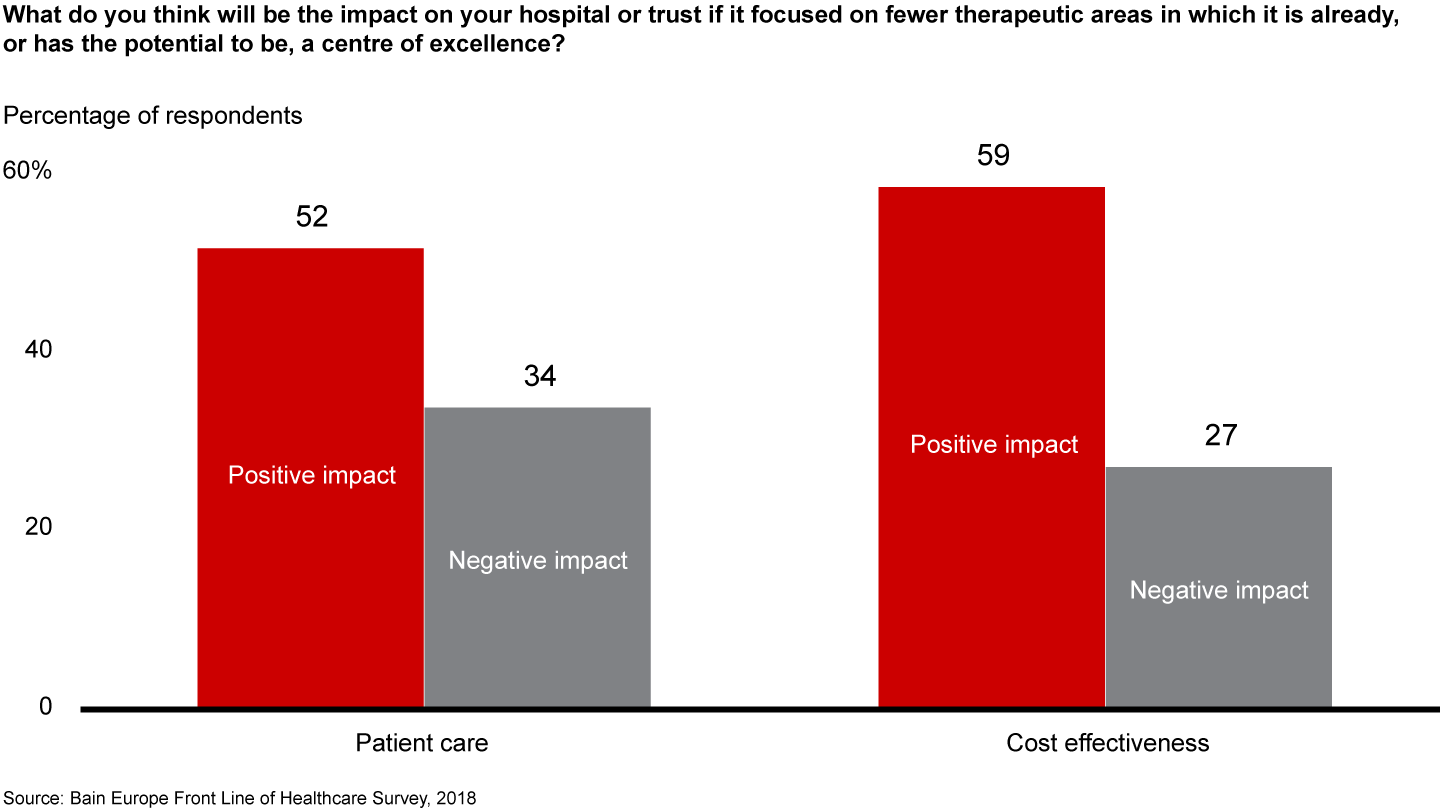

Priority No. 2: Incentivise plans that help trusts reach their full potential. The NHS can support individual trusts in achieving their full potential by looking holistically at all potential productivity strategies rather than focusing on cost containment alone. We base our preferred approach to individual trust productivity improvement on three key building blocks:
- multiyear operational improvements across sites;
- revenue enhancement; and
- asset optimisation.
Enabling trusts to achieve their full potential will also serve as a catalyst for, and accelerator of, broader system reform by ensuring that individual trusts focus on long-term self-sustainability.
Following a full-potential initiative and service redesign, selected and essential services from individual trusts or hospitals that are unable to achieve financial stability and meet minimum clinical safety metrics should be transferred to nearby thriving facilities. The insufficient facilities can then function as step-down, routine care or other alternative uses.
Priority No. 3: Empower and enable clinicians to lead transformation efforts. Transformation will only be sustainable if clinicians are empowered and enabled to take the lead. It’s not simply a matter of gaining buy-in on an already defined strategy; the Care Quality Commission found that that the most successful NHS cultures had a high level of clinical engagement and involvement in planning and delivery.
For their part, clinicians have expressed a willingness to participate in improvement programmes. Nearly 40% of doctors are already involved in improvement programmes within their hospitals, and another 40% wish to get more involved (see Figure 11).
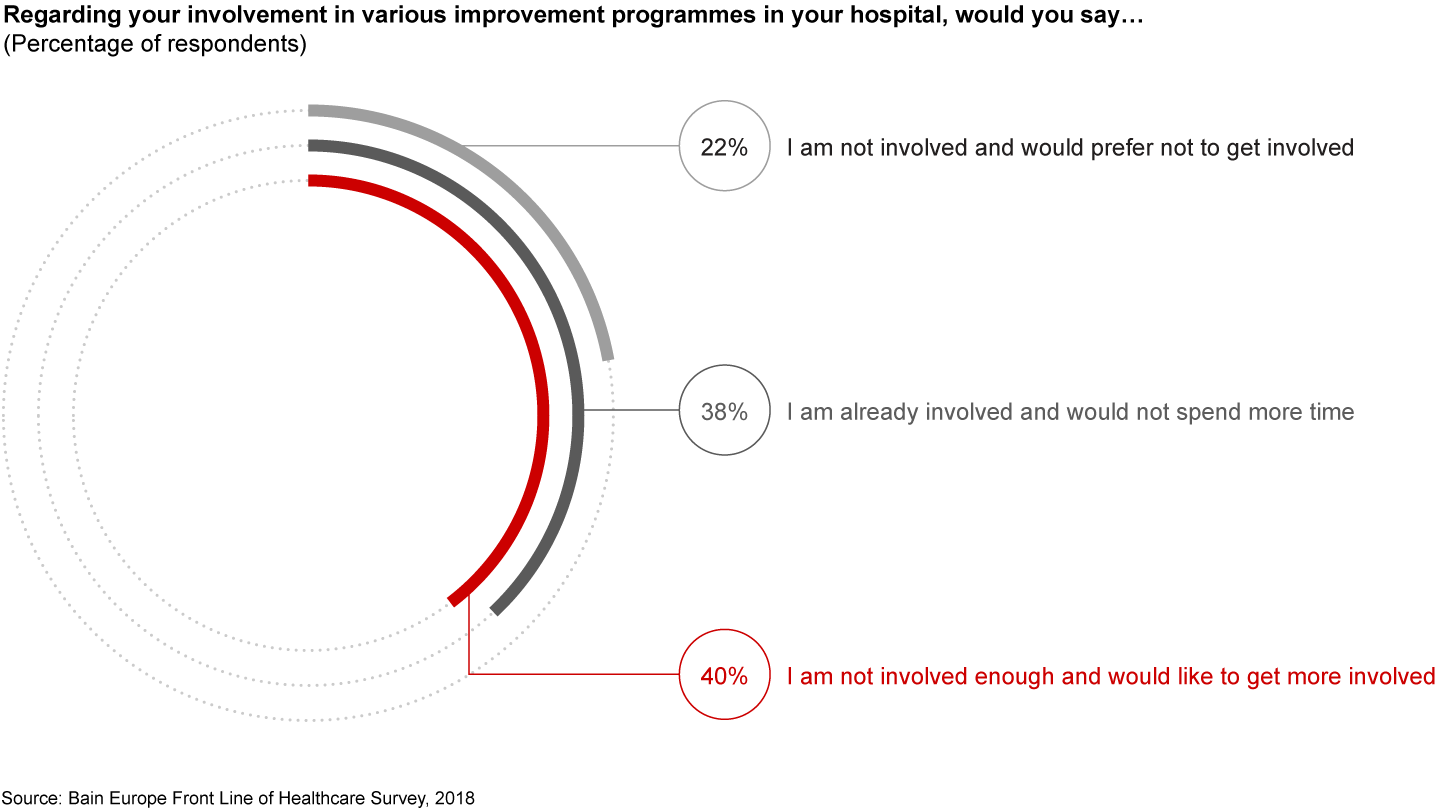

This will require a different mindset at the top. If we look at a recent example such as the rollout of the STPs, there are some key lessons to note. First, the time frames for the STPs’ development were too short, resulting in limited clinical engagement. Second, communication channels and systems were not always available to ensure that clinicians were informed of appropriate decisions or were able to consult on critical matters before the finalisation of STPs.
With the right structures in place, clinical involvement in service redesign and change delivery should be achievable.
Priority No. 4: Overhaul the NHS leadership programmes. The NHS should relentlessly overhaul its talent management programmes in two key areas: the NHS leadership programmes and training programmes for doctors that relate specifically to management and leadership skills.
An overhaul of the NHS leadership programmes should focus specifically on CEO recruitment, training and retention practices. There is a demonstrable relationship between the quality of management and the quality of clinical services in hospitals. As such, ensuring a stable and capable management team is of utmost importance.
The NHS Leadership Academy was set up to train senior NHS management staff and support their development. This, however, has not translated into a more stable hospital management team. According to The King’s Fund, the average tenure for a hospital CEO is just less than three years. This has raised concerns that trusts and foundation trusts are encountering substantial challenges in CEO-level recruitment. Tackling this issue will require a complete overhaul in the way that CEOs are recruited, trained, supported/mentored and evaluated in the short term.
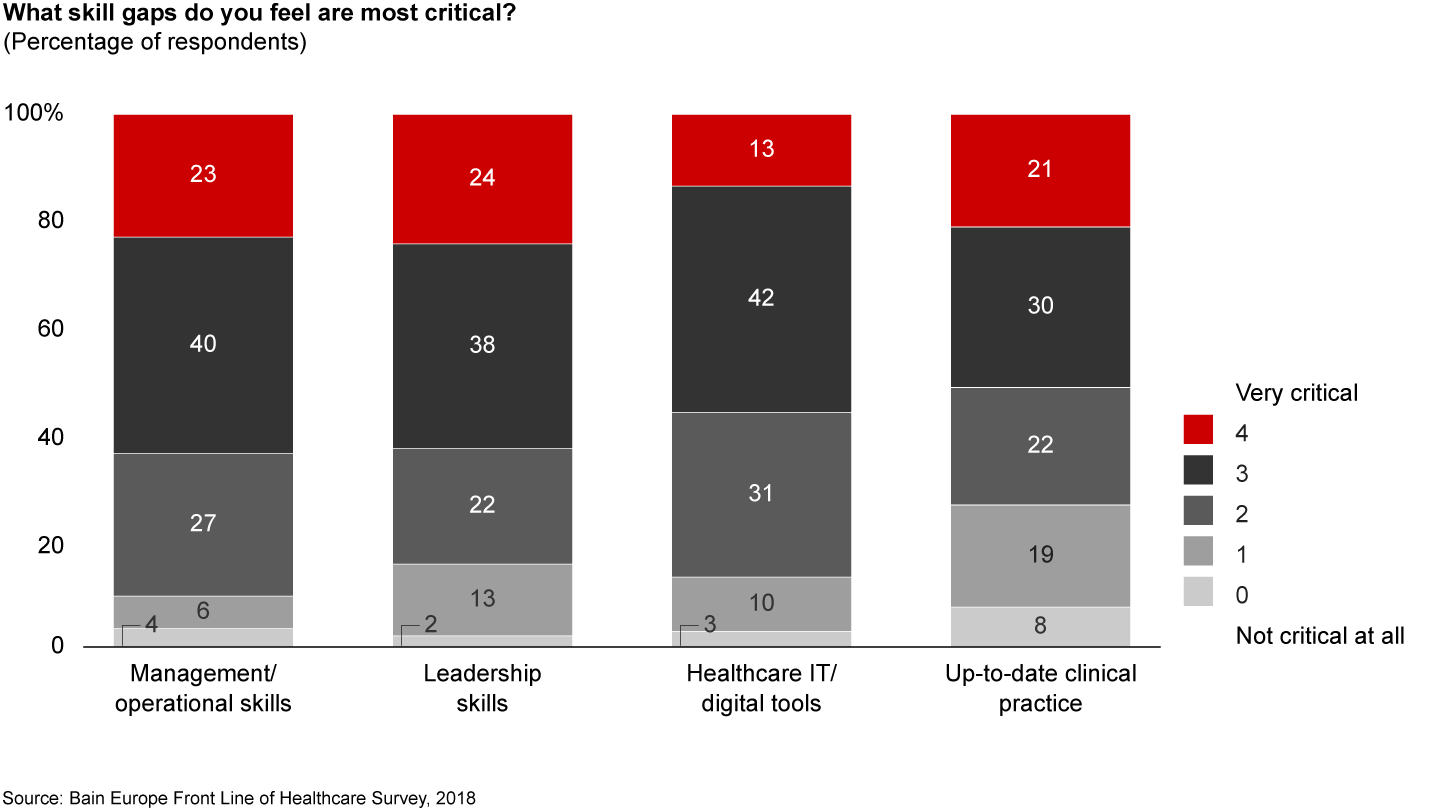
In addition, physicians need additional training in leadership, management skills and technology. Not only is this necessary to contend with the overly stretched clinical workforce, but there are also significant skill gaps that must be closed in order to enable transformation. These gaps pose potential risks to patient outcomes—a point with which most frontline physicians agree. More than 90% of physicians believe that skill gaps will have some level of impact on patient safety and outcomes, with more than 60% expecting this impact to be moderate to major (see Figure 12). Physicians highlight management and leadership skills as the most critical skill gaps (see Figure 13).
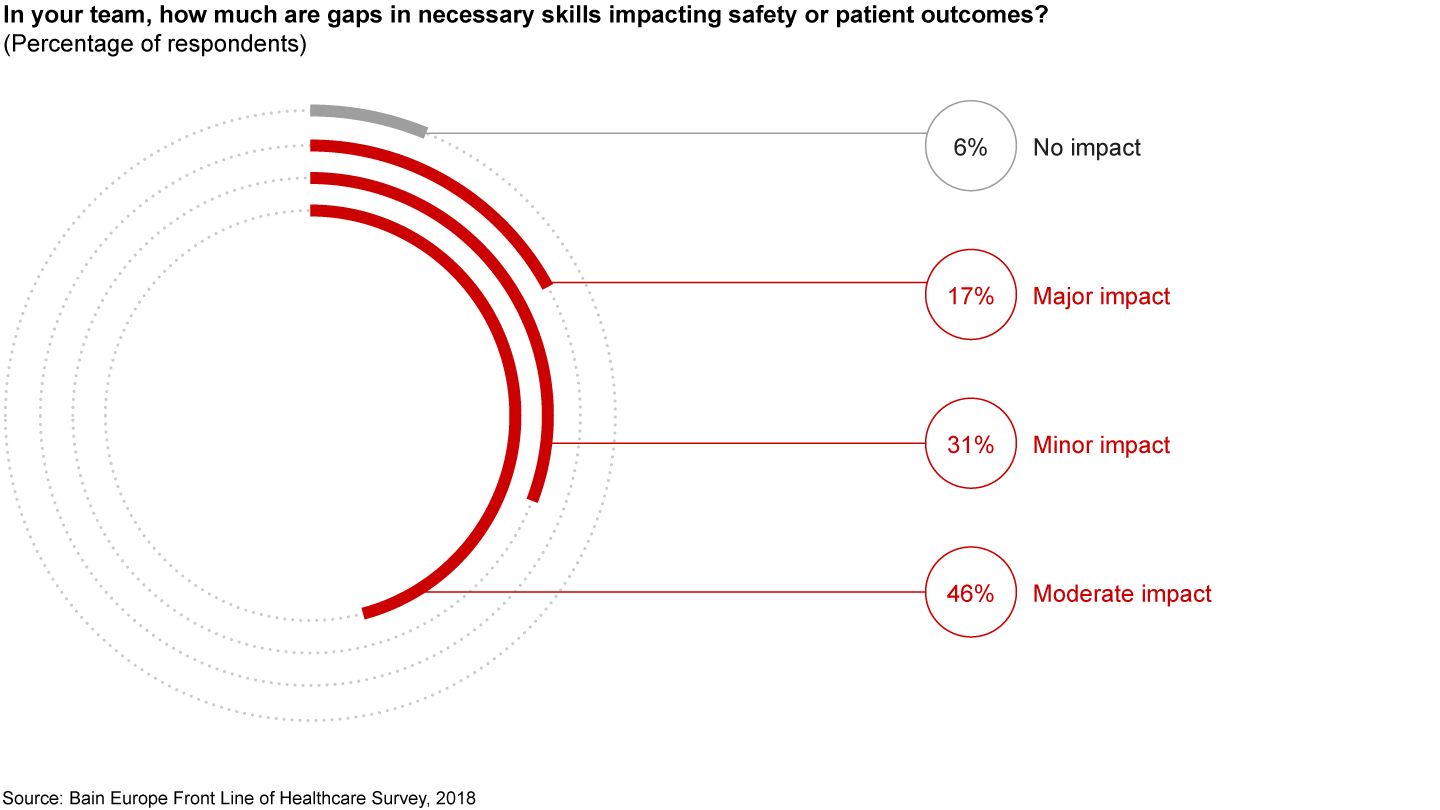


Priority No. 5: Use targeted investments to accelerate the adoption of technology. No one doubts how important technology will be in healthcare in the coming years. The additional funding must be invested in technology that demonstrably meets at least one of four objectives: improve clinical outcomes, increase productivity, engage the workforce or reduce demand through better education of the broader population. Such an initiative would require a combination of bold top-down measures with a deep understanding of patients’ and clinicians’ use cases.
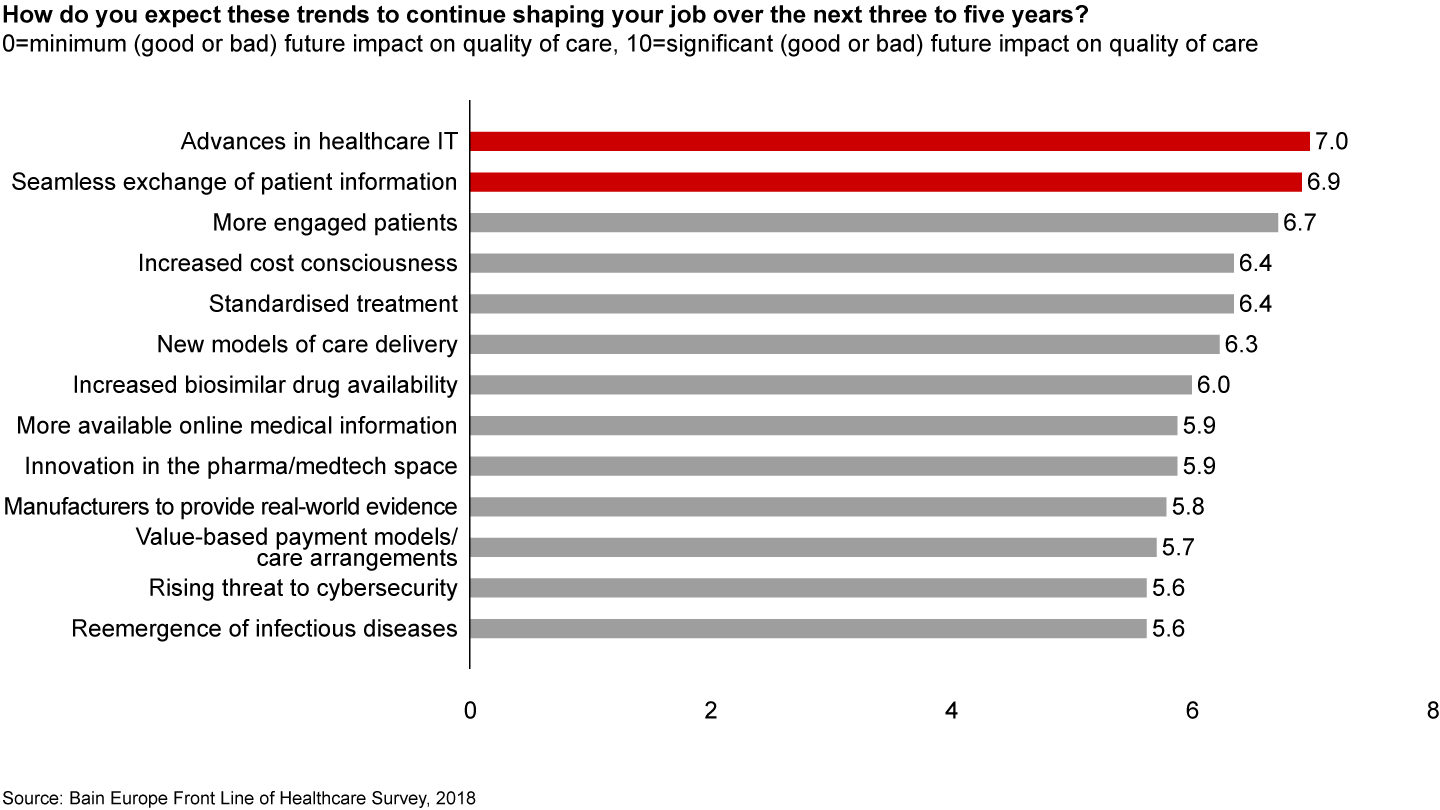
Advances in healthcare IT and the seamless, digitally enabled exchange of patient information among providers have been identified as the key trends that will shape clinicians’ work (see Figure 14).

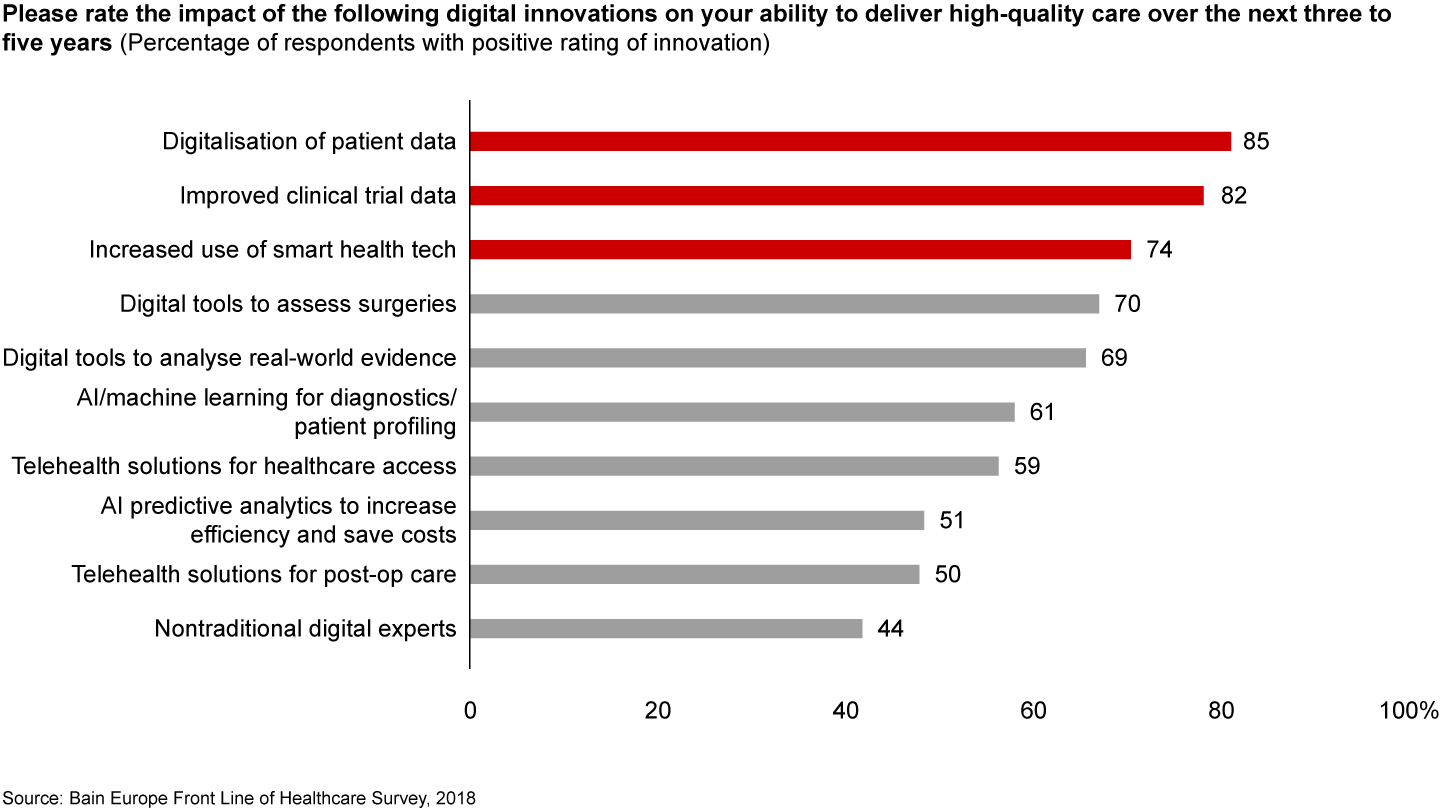
Physicians report that investments in the following three categories can lead to the greatest improvement in efficiencies and quality of care (see Figure 15):
- digitisation of patient-related data;
- data quality from clinical trials through Big Data and digital; and
- increased use of mobile wellness apps, wearable sensors and digitally enabled smart devices for disease management, such as blood glucose monitoring, compliance apps and smart asthma inhalers.

As with all of our recommendations, clinical engagement will be essential. Digital solutions need to address specific use cases, target important clinician and patient episodes, and address the optimal channel in order be scalable. Furthermore, new digital solutions will require the adoption of new processes, which clinicians should help shape to ensure that quality care remains the top priority. Frontline buy-in can be further encouraged by developing a test-and-learn micro environment preceding a wide-scale rollout.
Implications for the future
With the government’s NHS funding commitment comes new opportunities to build on past successes and confront current challenges with clear-eyed pragmatism. Not least of this will be building support for funding mechanisms. Regardless of the source of funding, the NHS must transform to become a better receptacle for renewed funding.
To do so, it is critical that a sizeable portion of the additional funding be invested in innovations that will deliver long-term efficiencies and support greater productivity. In this sense, the NHS can speak to its investments in modernisation efforts that will enable it to do more with less while improving access to care and the quality of care delivery.
The success of this effort will hinge on inspiring frontline providers to engage (or reengage, in some cases) in transformational efforts. This will require not just a well-overdue increase in pay; it will also necessitate applicable frameworks to help physicians make meaningful contributions to, and take ownership of, change efforts. By ensuring that physicians feel more valued, the NHS will add more value as it reorients its model for the 21st century. Making this change won’t be easy, but it will go far in positioning the health system for favourable outcomes over the next 70 years.

Front Line of Healthcare Report 2018
Rising physician dissatisfaction in Europe signals an urgent need for change.
Appendix: Methodology
The Bain Europe Front Line of Healthcare Survey was conducted in 2018 by the physician panel at SERMO, a leading global social network for physicians and healthcare market researcher. It canvassed 1,156 physicians and 154 procurement officers from Germany, France, Italy and the UK, including 324 physicians in the UK.
The survey focused on eight specialties in the UK: three surgical and five nonsurgical. The surgical specialties were general, cardiac and orthopaedic surgery. Nonsurgical specialties were primary care, medical oncology, noninterventional cardiology, endocrinology and neurology.
SERMO’s panel carried out strict quality checks to ensure maximum data integrity, such as consistency and straight lining checks, speeding control, and quality assessments of free-text answers.
Nitin Chaturvedi is a partner with Bain & Company in London, and Dr. Akshay Agarwal is a principal with Bain & Company in London. Nitin leads Bain’s Healthcare practice in the UK, of which Akshay is a core member.
Net Promoter®, Net Promoter System®, Net Promoter Score® and NPS® are registered trademarks of Bain & Company, Inc., Fred Reichheld and Satmetrix Systems, Inc.