Report

Executive summary
For those providing services on the front line of healthcare in Europe, change is accelerating—and there’s no turning back. Digital technologies, cost pressure and tighter protocols are transforming care delivery. Each of the main European markets is starting from a different position, but powerful forces are propelling the industry toward systemic change.
To better understand these dynamics, in 2016, Bain & Company fielded a multinational survey of 1,191 physicians across nine specialties and 167 hospital procurement administrators in four European countries, which are France, Germany, Italy and the UK. The European survey follows a 2015 Bain survey on the front line of US healthcare, and allows for selective comparison. (For a description of the methodology and survey questions, see the appendix.)
The surveys highlighted regional and national differences in healthcare systems in the US and Europe and across the four European countries we surveyed. Our findings underscore an urgent call to action for European healthcare organizations to move faster in renewing systems and processes to meet future demands. Big Data and real-world evidence can provide solutions to many healthcare challenges. Already they are changing the way organizations purchase and use drugs and devices, putting the focus on demonstrating value. But harnessing their full potential will require more integrated systems and a major shift in focus to patient outcomes.
In this chart digest, we present the results of our survey, focusing first on the general trend toward the systematization of healthcare and then on the implications of our survey results for medtech companies, pharmaceutical manufacturers and hospitals. We begin each chapter with our key findings and highlight the most significant survey responses with charts.
The financing and delivery of healthcare is becoming more systematized
Europe’s healthcare systems face daunting challenges: They are among the most expensive in the world, and their costs are steadily rising. European governments shoulder about 75% of total healthcare expenditure, compared with 47% for the US government, as private payers make up a large proportion of the US market. An increase in chronic diseases and aging populations already is straining Europe’s healthcare systems, and the burden is set to grow exponentially. Despite their different starting points, European governments agree they must find a way to lower costs while improving quality of care. To achieve those goals, healthcare organizations must become more flexible, more integrated and more focused on quality of care.
Our findings show Europe has started down the path of consolidating and professionalizing its care organizations. Change is visible along a number of dimensions. Physicians increasingly are using standardized treatment protocols and electronic medical records as well as more objective metrics for measuring clinical performance. Physicians’ perceptions of their own responsibility for cost are changing, and new payment models are putting providers at risk for outcomes. In order to measure these changes by country, we combined these dimensions into what we call a systematization index (see Figure 1).
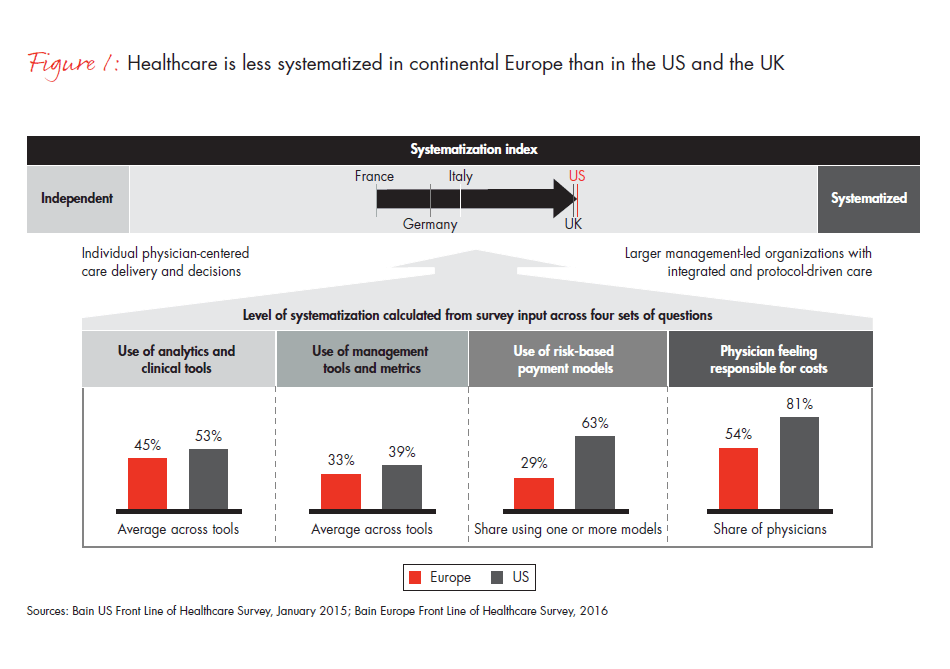
Clearly, the UK and the US have gone much further than continental Europe in developing larger, management-led healthcare organizations that rely on standard protocols for patient care. Most healthcare systems in continental Europe still allow physicians to decide independently on patient care. Their social insurance models encompass multiple payers and owners as well as direct access to specialists. The UK has likely been quicker to embrace a systematized model because it is predominantly a public healthcare model with a single payer.
Despite their slower start, we believe healthcare systems in continental Europe will become increasingly systematized over time as pressure grows to bring healthcare costs down and reorient payment systems toward patient outcomes. Already, care organizations are harnessing healthcare information technology and accelerating the proliferation of patient data and new data sources.
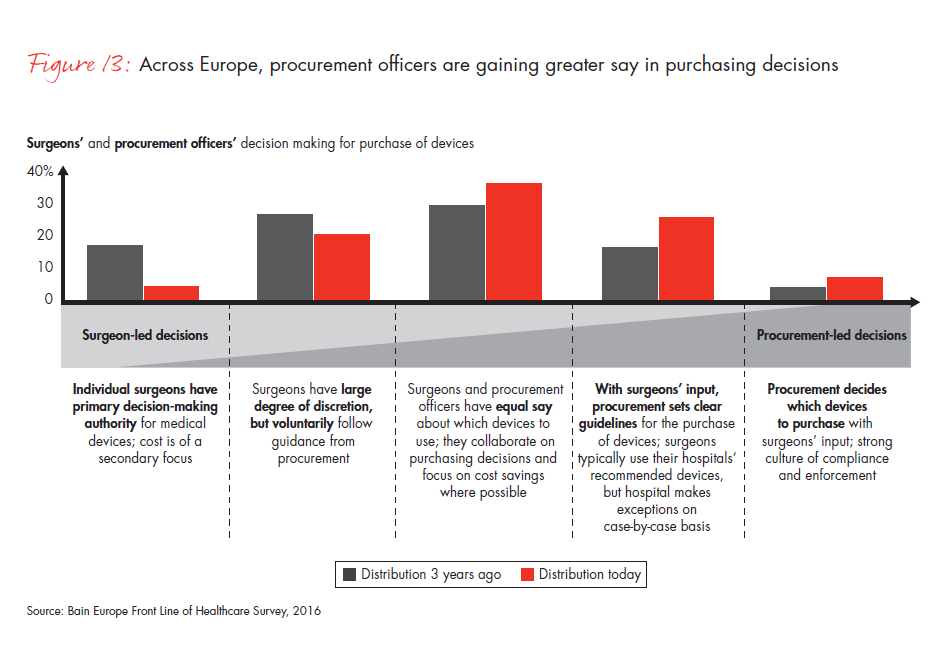
The systematization of healthcare in Europe will have a direct impact on pharma and medtech manufacturers as changes cascade down the value chain. Purchasing decisions in Europe already are becoming more focused on outcomes and economics. Procurement officers are gaining greater say in purchasing decisions, and surgeons and nonsurgical physicians are reporting a loss of autonomy in the decision-making process. The growing use of metrics in European healthcare systems, particularly in the UK, provides an opportunity for pharma and medtech manufacturers to support physicians and providers with products that demonstrate superior value.
As Europe’s national healthcare systems move at varying speeds to a more management-led model, the commercial landscape will become more complex. Providers will require different sales models and product types, adding to cost.
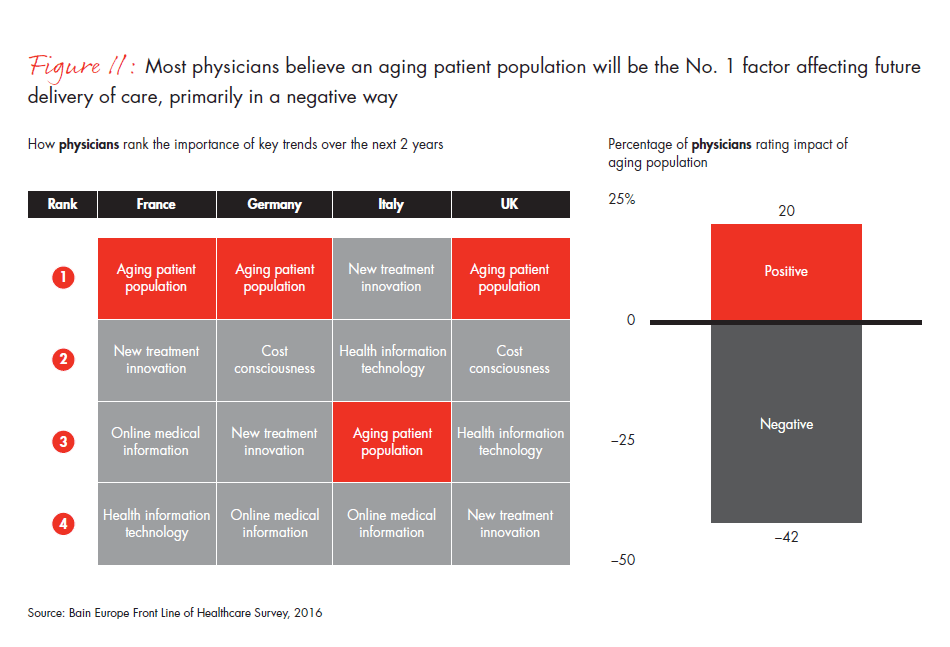
Although Europe’s healthcare systems have started down the path of change, they have a long way to go. A large percentage of European physicians consider their organizations and themselves to be ill prepared to address the changes ahead. More than 80% of survey respondents across Europe said they believe the aging population will have a major impact on the delivery of care going forward—and even more unsettling, 42% of those said that trend would have a negative impact on their ability to deliver high-quality care. The high level of skepticism among physicians about their organizations’ capability is a clear call to action for European provider organizations to accelerate change.
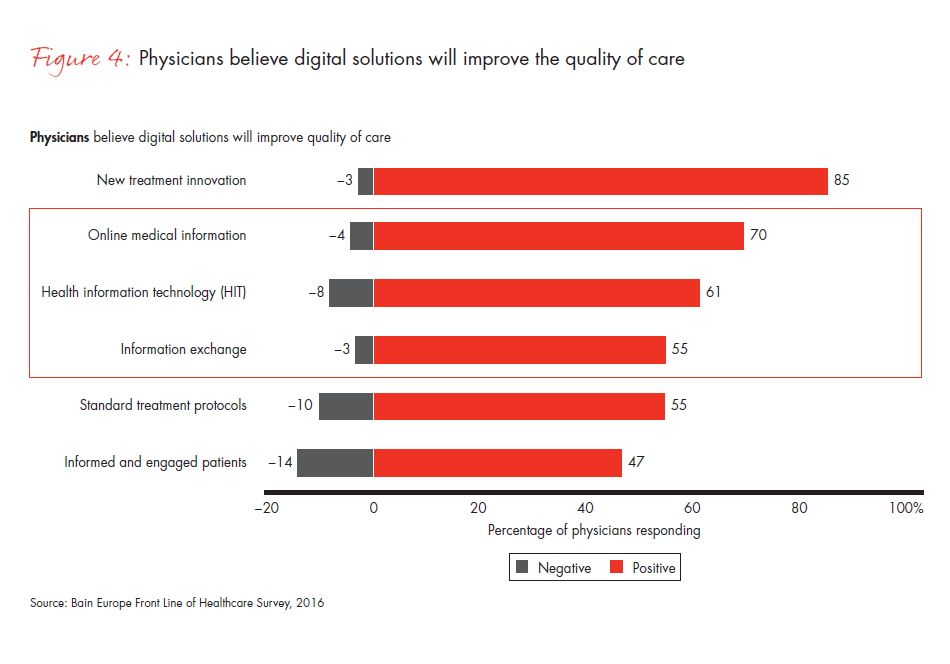
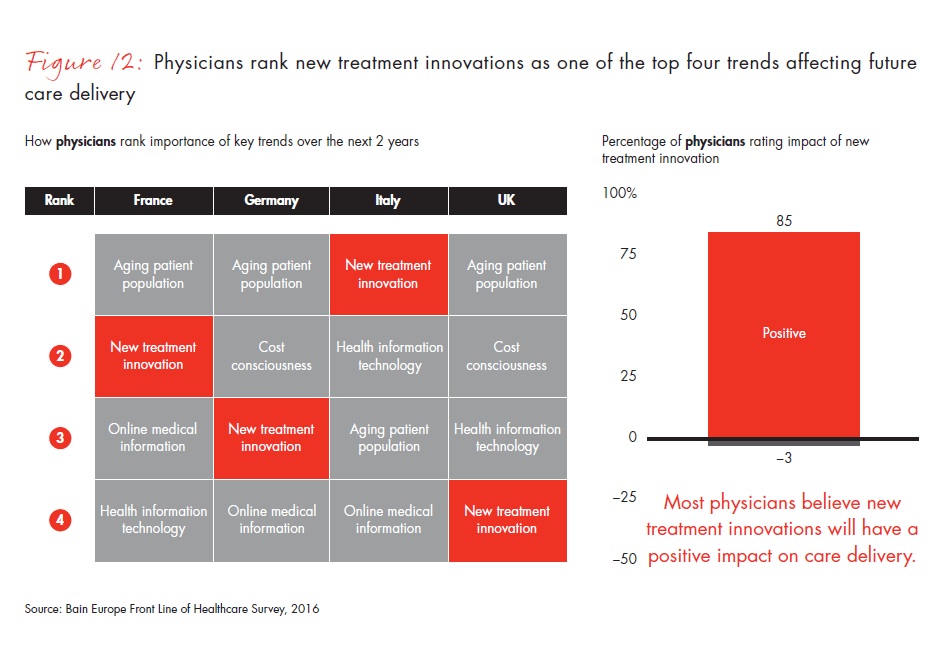
Balancing that concern, European physicians see new treatment innovations as the most positive force for change: 85% of physicians associate innovation with the ability to deliver high-quality care. The increasing use of metrics within healthcare systems in Europe creates an opportunity for pharmaceutical and medtech manufacturers to support physicians and providers in demonstrating superior value generation through their products.
Christian Rebhan, a partner with Bain's Healthcare practice, discusses recent trends in European healthcare and the need for transformation across the sector, from providers to pharma and medtech manufacturers.
What change means for medtech manufacturers
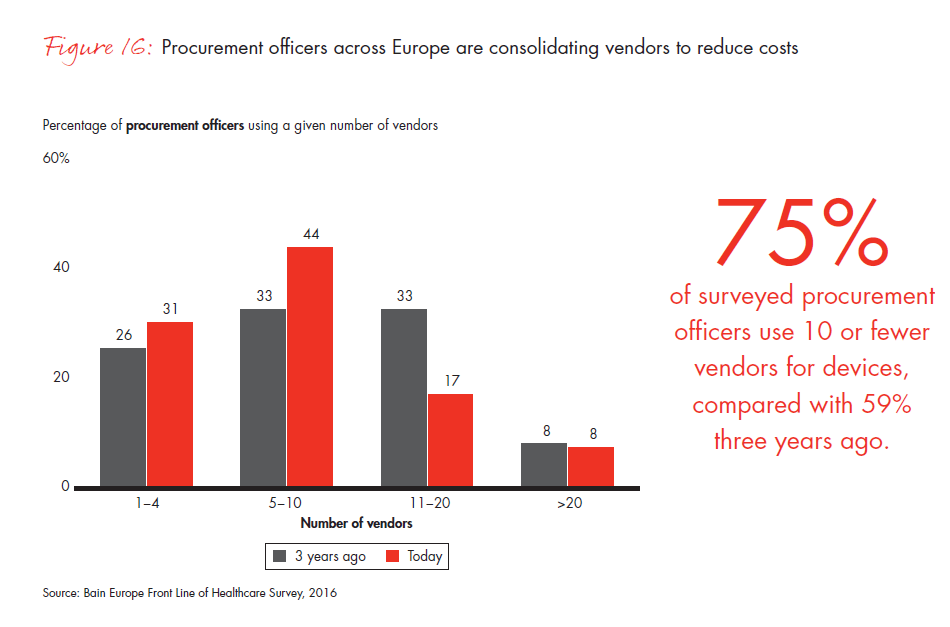
Europe’s shift to more centralized purchasing practices and its gradual move away from the physician-led model have a significant impact on medtech companies given their traditionally more physician-centered business model. As procurement officers gain influence, companies must cater to multiple decision makers with differing needs. The battle will be particularly fierce for companies that are not category leaders. As healthcare organizations consolidate the number of vendors and limit surgeons’ purchasing choices, they will tilt the playing field in favor of those with the greatest market share in a given category.
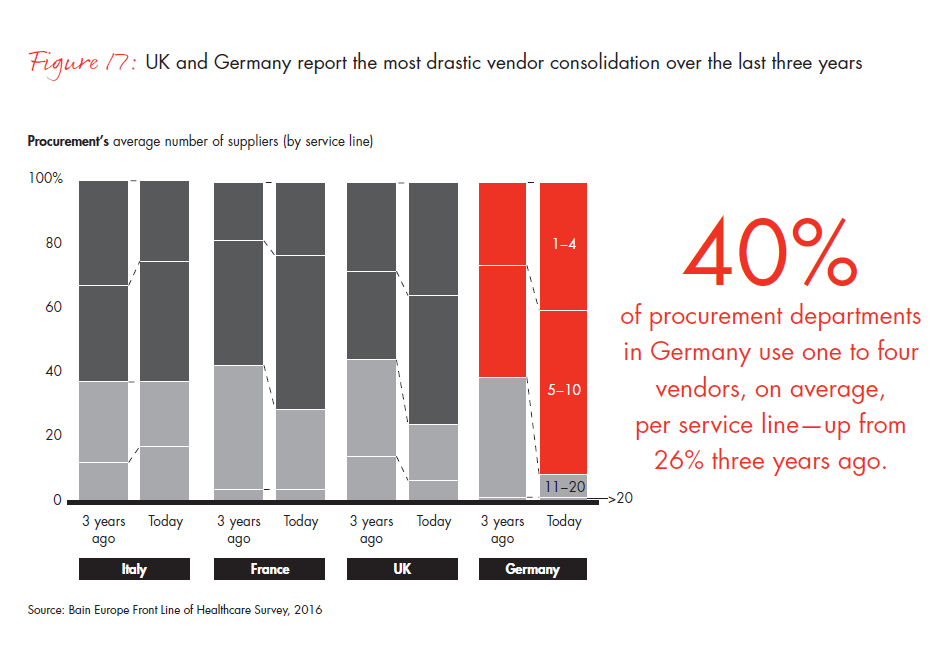
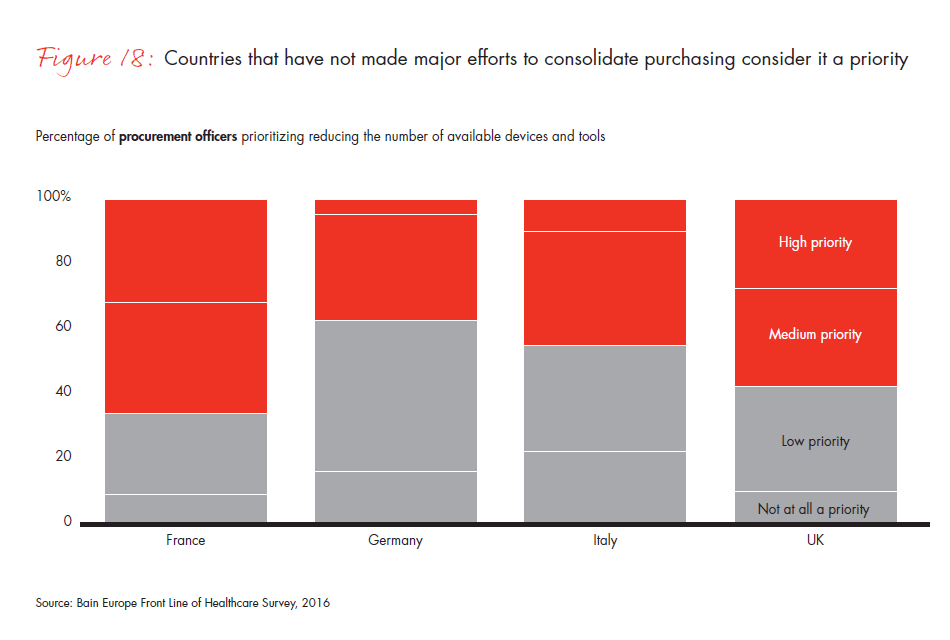
Germany is moving fastest to consolidate vendors: 91% of surveyed procurement officers in Germany use 10 or fewer vendors for devices today, compared with 60% three years ago. But countries that have made less-drastic consolidation efforts in the past, such as France, are likely to catch up. Two out of three procurement officers in France consider the reduction of available devices a medium or high priority for their purchasing departments.
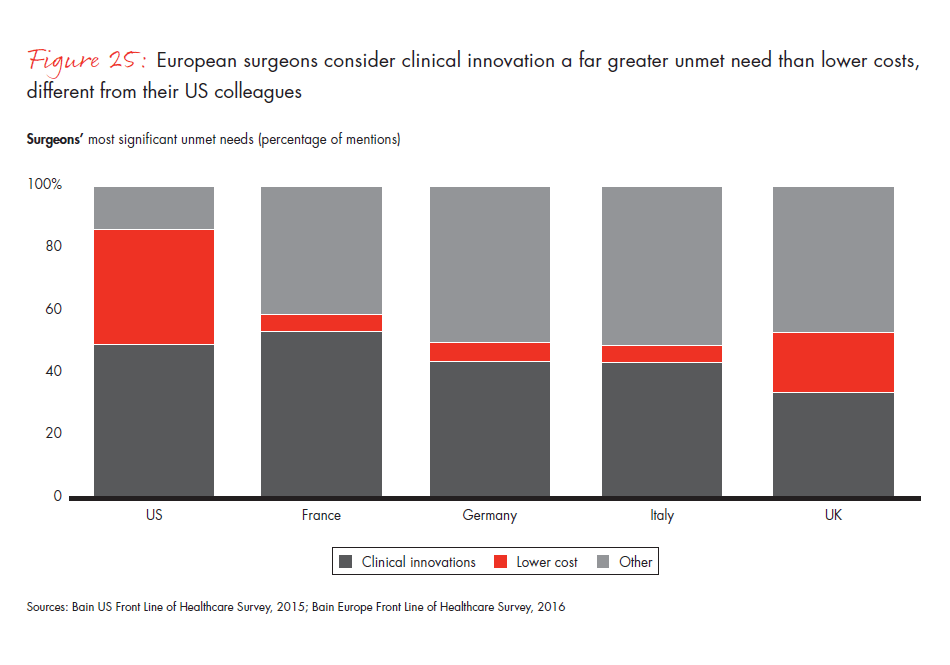
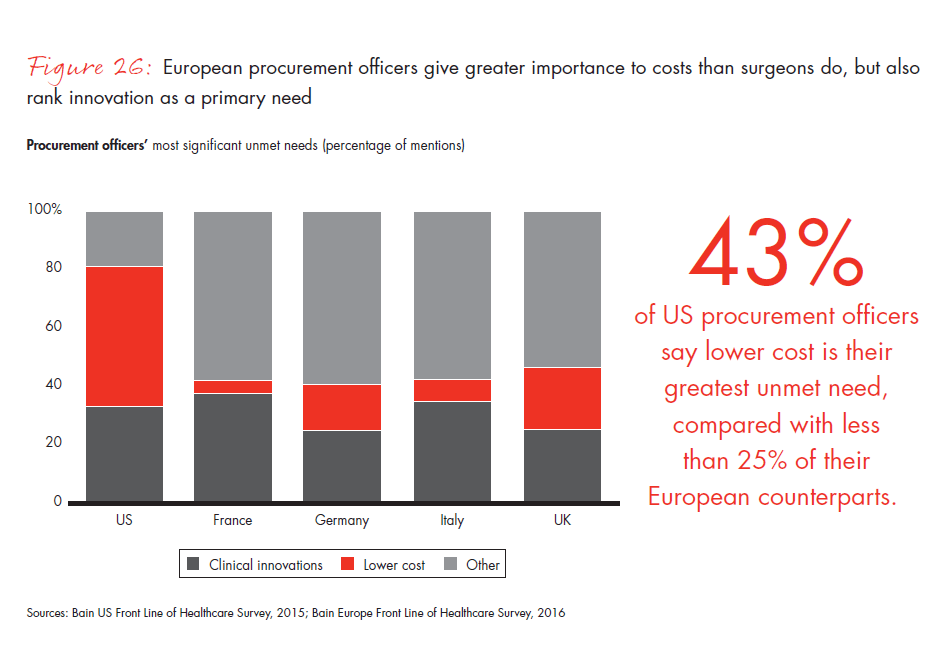
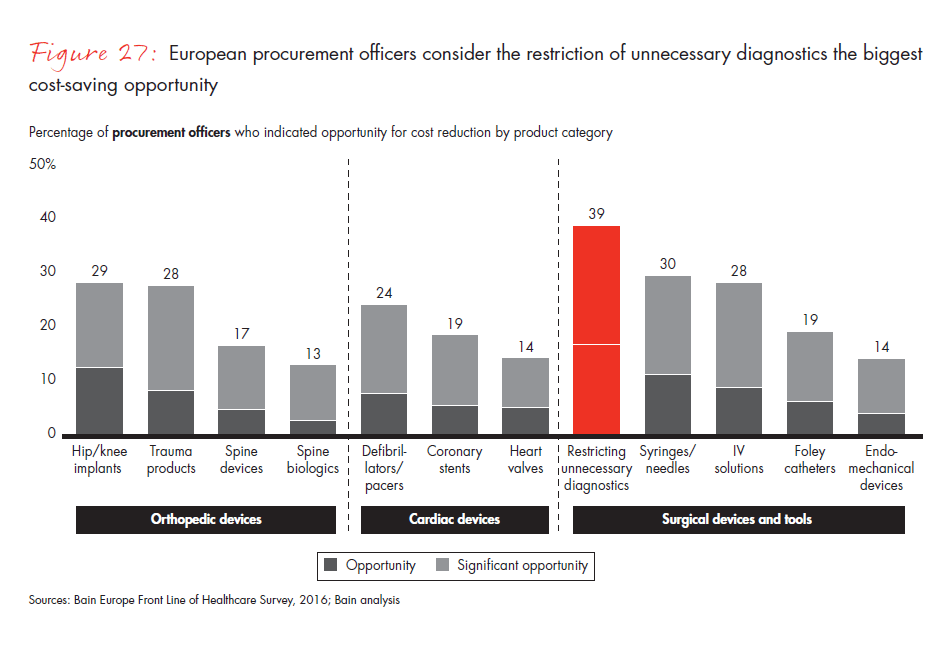
European surgeons and procurement officers say their greatest unmet need is clinical innovation. By contrast, their US counterparts ranked lower costs as their top priority. Accustomed to cost control by governments, European physicians want more clinical innovation and less cost innovation. When asked about the greatest opportunities for reducing costs, European procurement officers pointed to restricting unnecessary diagnostics.
Medical technology companies can adapt to this changing landscape by sharpening their focus on customers, categories and data. Those that develop the ability to aggregate data in support of efficacy claims will have a clear advantage as digital technologies transform healthcare delivery. Equally important, companies will need to deepen their understanding of the needs of physicians that use their products and build ties across all key stakeholder groups to gain privileged insights. The winners will build customer knowledge and the commercial clout to reshape one or two categories, introducing new value-added services and alternative pricing models.
Europe’s shift away from sales representatives is not yet as pronounced as it is in the US—in many cases, sales reps continue to provide invaluable input to the surgical teams utilizing their devices. Medtech companies selling in Europe can continue to capitalize on their traditional educator role while equipping their field forces to more effectively address the evolving needs of procurement officers and surgeons as they diversify their sources of information.

Healthcare in Europe: The Outlook for Medtech Companies
A look at how the European healthcare landscape is changing for medical device manufacturers.
What change means for pharmaceutical manufacturers
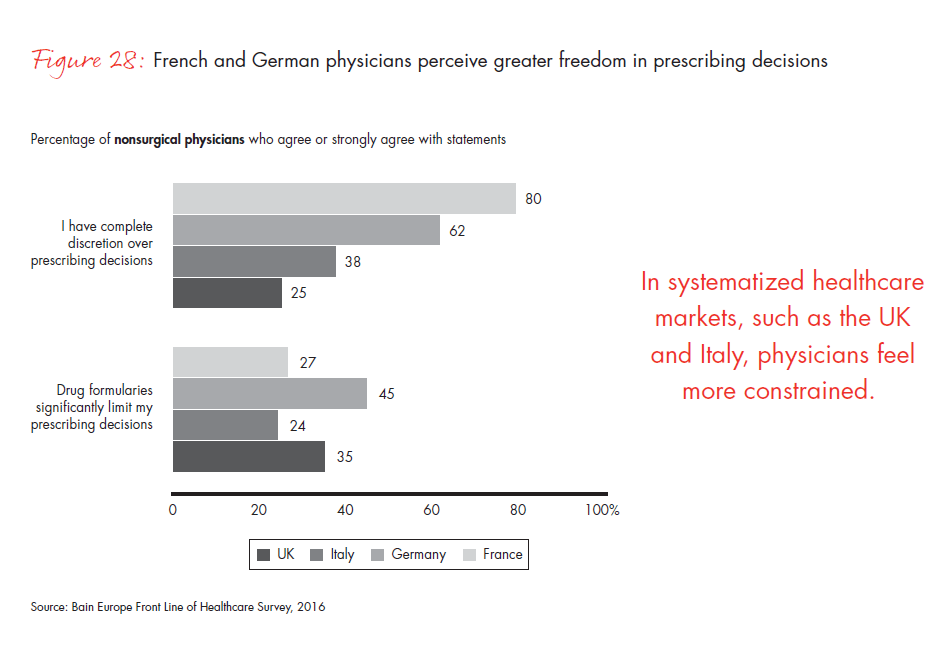
Growing pressure to lower costs and improve patient outcomes is prompting healthcare organizations to take a more systematic approach to prescription drug selection, but the pace of change varies widely across Europe. In France and Germany, where the physician-led model is still dominant, physicians report a high degree of freedom in prescribing drugs, despite limitations imposed by drug formularies. In markets with greater systematization, such as the UK and Italy, physicians feel more constrained. Over time, we believe systematization will continue to decrease European physicians’ discretion to prescribe independently.
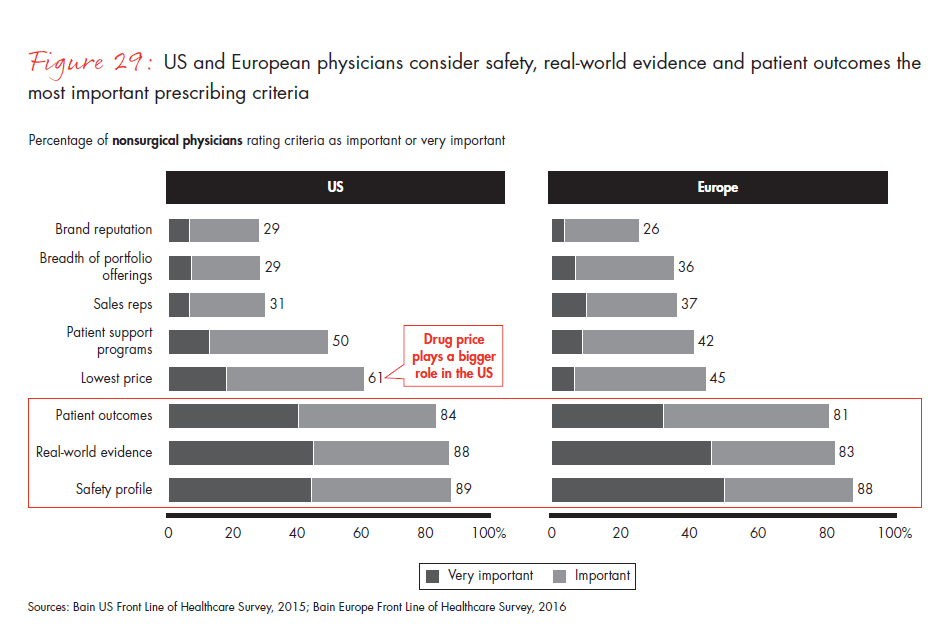
As procurement officers and other new stakeholders gain influence over prescribing decisions, pharma companies will face increasing demand for proof of incremental value. The winners will be those that can demonstrate new and meaningful sources of medical and economic value for their products. Already, European physicians rank safety, real-world evidence and patient outcomes data as the most important criteria when prescribing drugs, mirroring our US findings. A sharp rise in the use of digital devices, tools and metrics within the European healthcare systems (as described within this survey) will reinforce physicians’ growing focus on patient-generated data and real-world data.
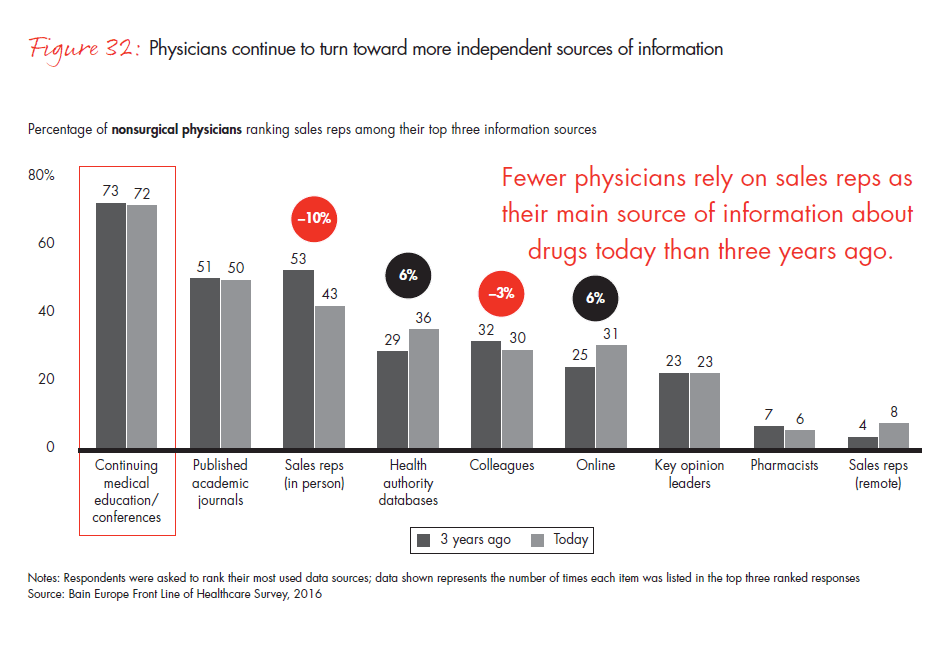
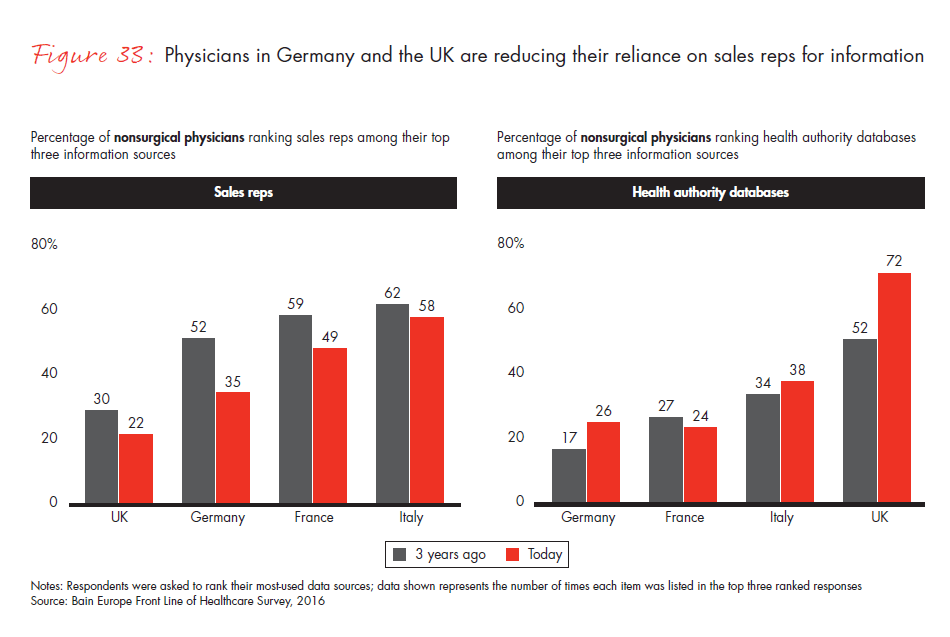
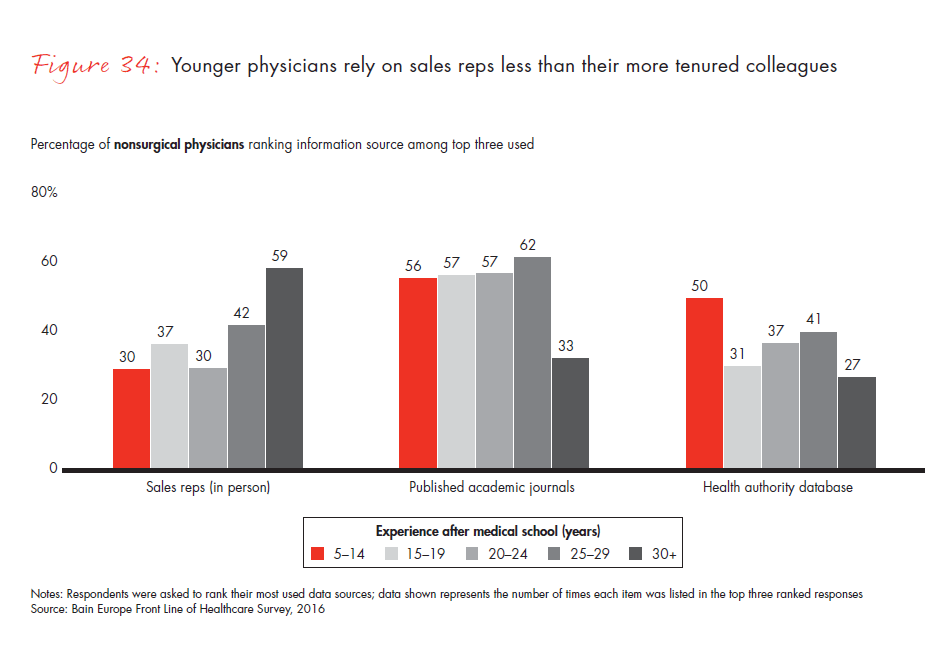
The percentage of European physicians who view sales reps as an important source of information is declining, following the trend in the US. Only 43% of nonsurgical physicians in our survey report that sales reps are one of their top three sources of information when learning about a drug, compared with 53% three years ago. The two most important sources were medical education/conferences and academic journals. As physicians diversify away from traditional information sources like sales reps and toward information sources perceived as more unbiased, pharma manufacturers will need to rethink their go-to-market model, particularly with younger physicians, who are far less inclined than longer-tenured colleagues to rely on sales reps as one of their top information sources.
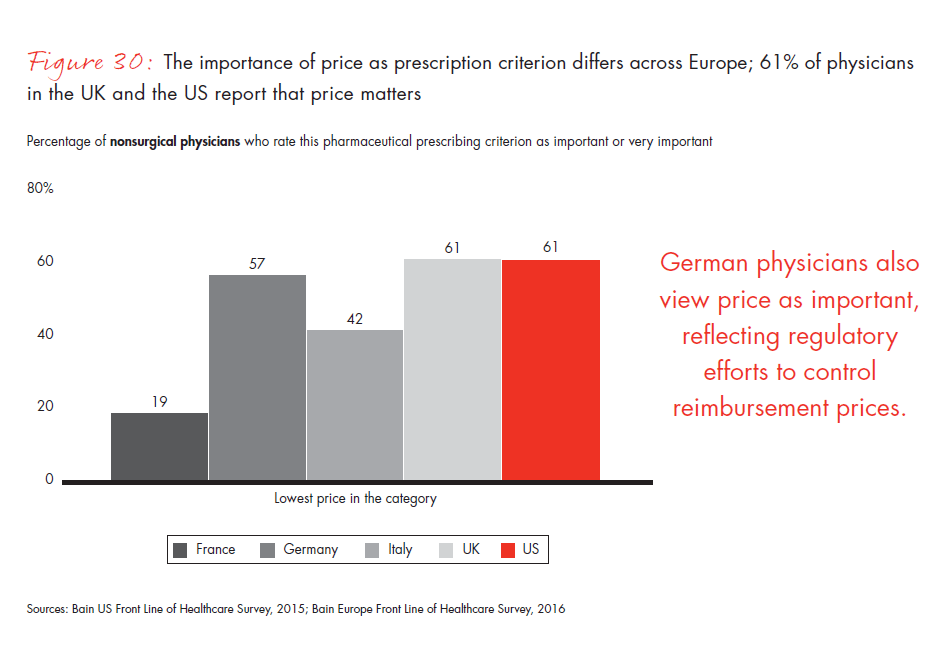
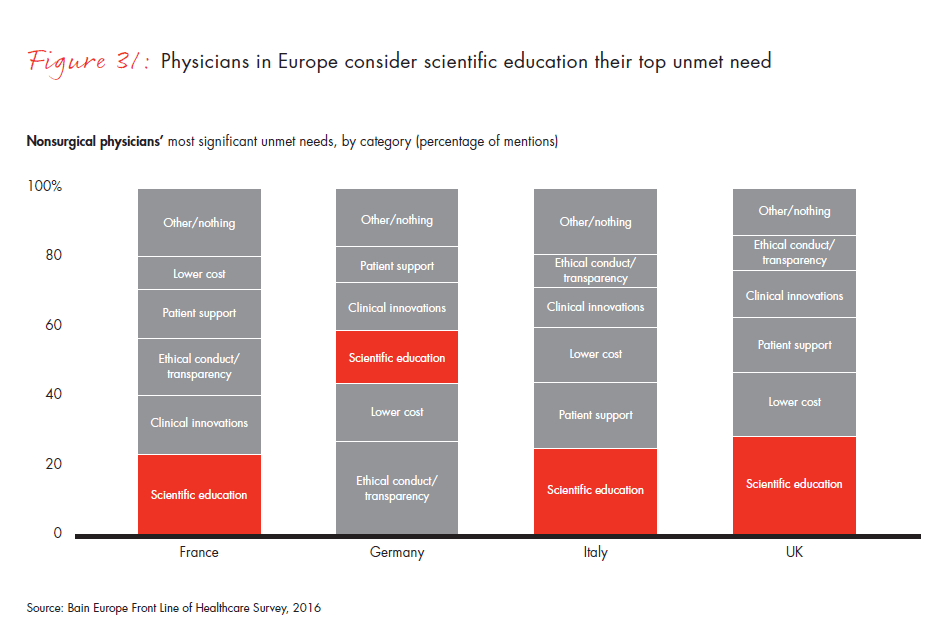
Underscoring that trend, European physicians rank scientific education as their most significant unmet need. Specifically, they want different data (comparative studies), more of the same data (real-world evidence) and more credible data (less marketing). By contrast, US physicians rated cost and clinical innovation as their most critical unmet needs, and were more concerned about prices than European colleagues. The importance of price varies significantly across Europe. The more systematized UK market and the German healthcare system require physicians to consider costs more thoroughly, whereas only one out of five physicians in France consider price as an important or very important prescribing criterion.
To compete effectively in a more systematized European healthcare market, where data is critical to demonstrating the value of products, pharma companies will need to generate unbiased medical information and create a credible omnichannel approach for disseminating it to multiple stakeholders. Both strategies require companies to embrace digital tools.
European hospital physicians report low satisfaction
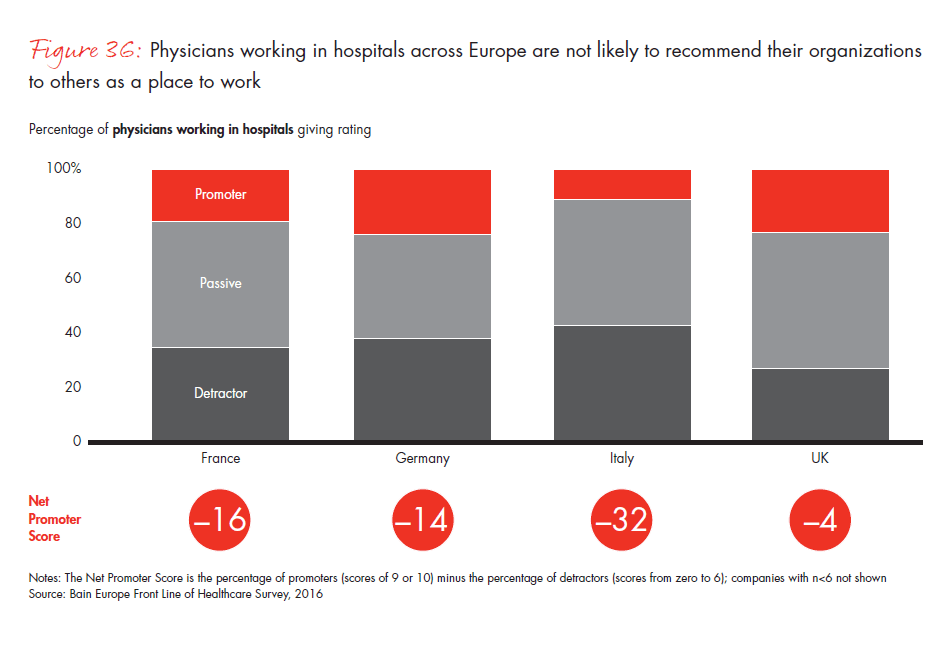
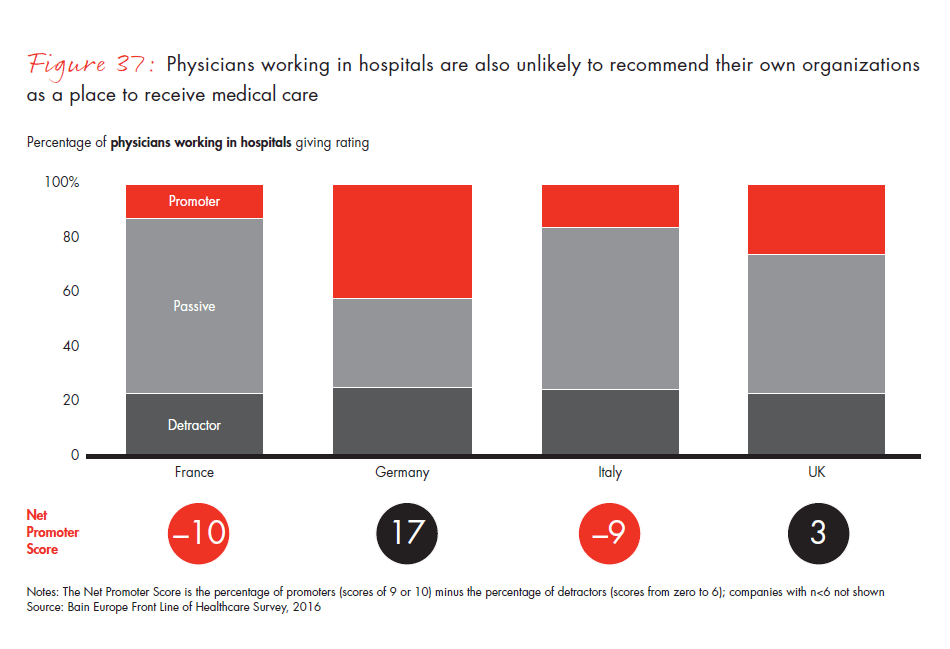
One of the most provocative findings of our survey is the low level of satisfaction among hospital physicians across Europe. We found that hospital physicians have a very low likelihood of recommending their organizations to others as a place to work, with specifically low advocacy ratings in Italy. Even more striking, a high share of hospital physicians refrain from recommending their organizations to friends or colleagues in need of medical services. Germany was a notable exception, where 42% of physicians are highly likely to recommend their organizations to friends or colleagues in need of medical care.
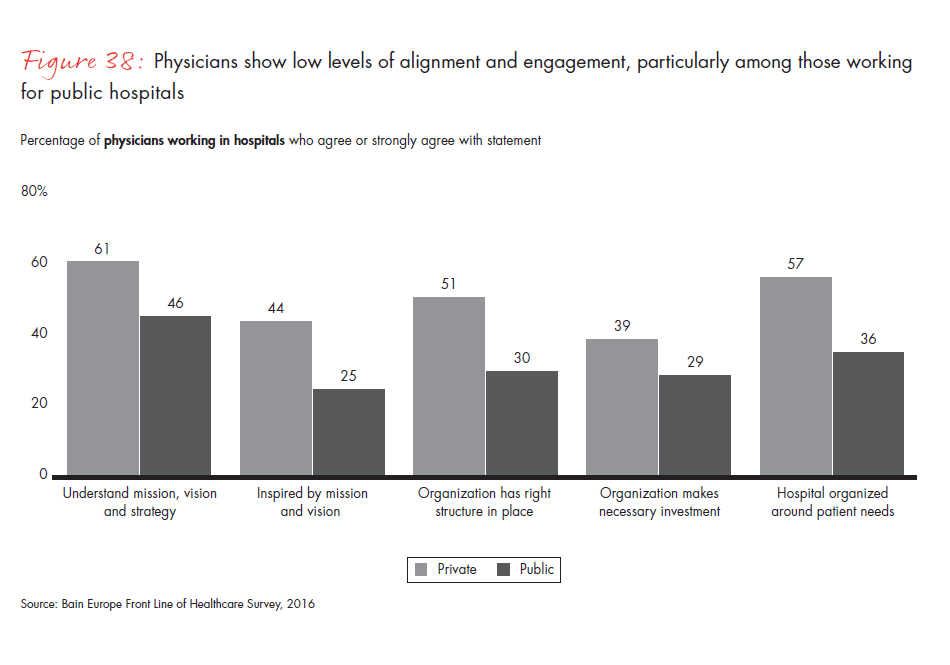
Overall, European hospital physicians are highly skeptical about their organizations’ ability to deal with future medical challenges. Only one-quarter of physicians working in public hospitals feel inspired by their employers’ mission and vision. Less than one-third believe that their organizations have the right structures in place and are making the investments required to achieve their mission.

Healthcare in Europe: The Outlook for Doctors and Hospitals
A look at how the European healthcare landscape is changing for doctors and hospitals.
These findings underscore an urgent need for European provider organizations to further professionalize their management, engage physicians more effectively and improve how they organize care delivery, as well as administer and manage scarce medical resources.
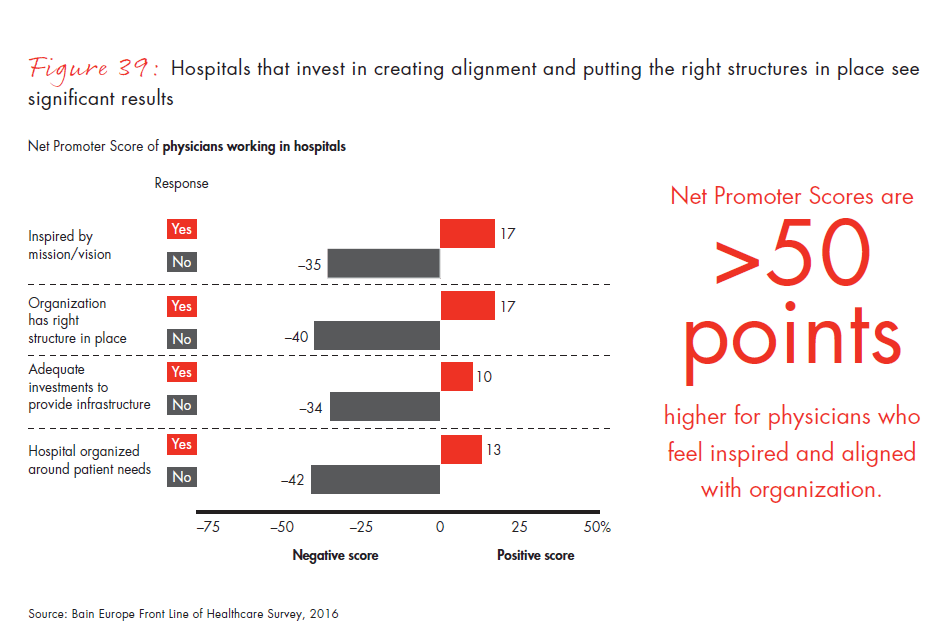
To address the gap in confidence, public and private provider organizations should engage physicians more effectively on processes, structures, capabilities and future direction. Hospitals that invest in creating alignment and putting the right structures in place see significant results. Our survey showed significantly higher satisfaction levels for physicians who feel aligned and engaged.
By the numbers: The shifting European healthcare landscape

1. Care delivery
- Increased cost pressure, tighter government regulation and digital technologies are transforming the delivery of healthcare, accelerating a global trend toward consolidation and professionalization. European countries are at different starting points and moving at different speeds, but all are becoming more systematized, particularly the UK.
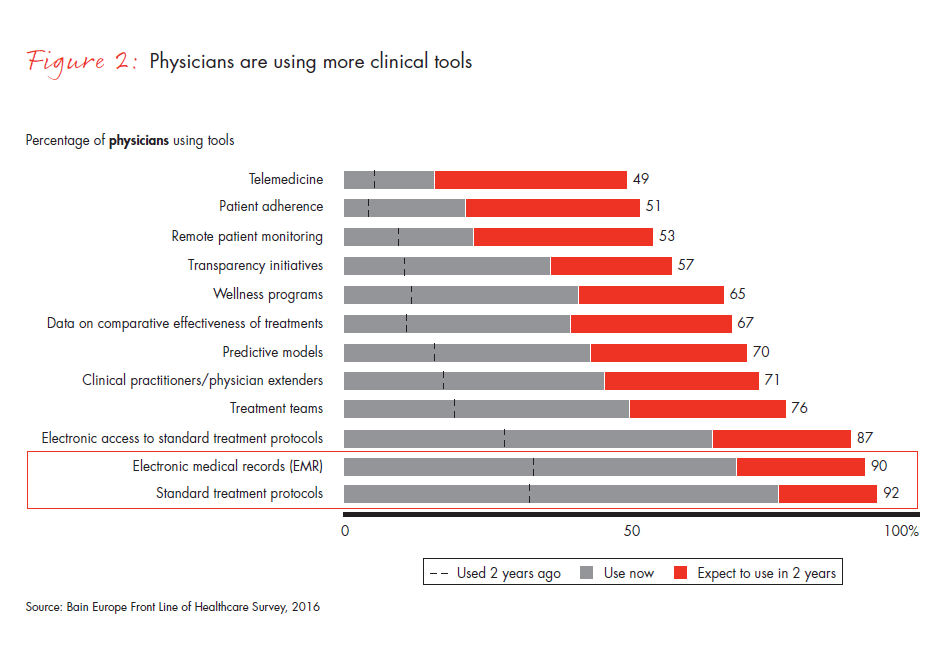
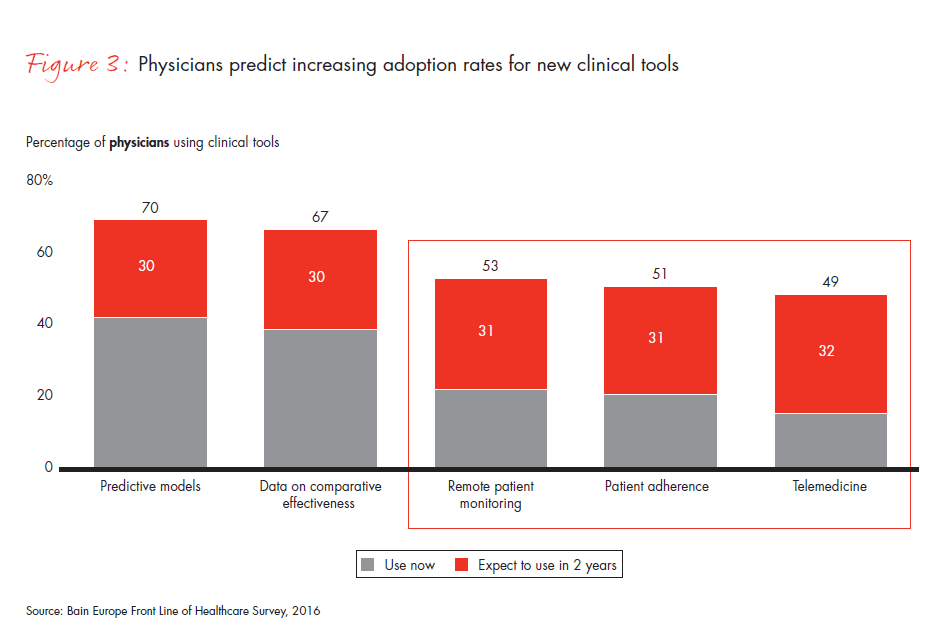
- Changes across several dimensions of care indicate systematization is likely to continue: The use of electronic medical records and standard treatment protocols more than doubled in the last two years, and physicians expect rapid increases in the use of telemedicine, remote patient monitoring and patient adherence programs.
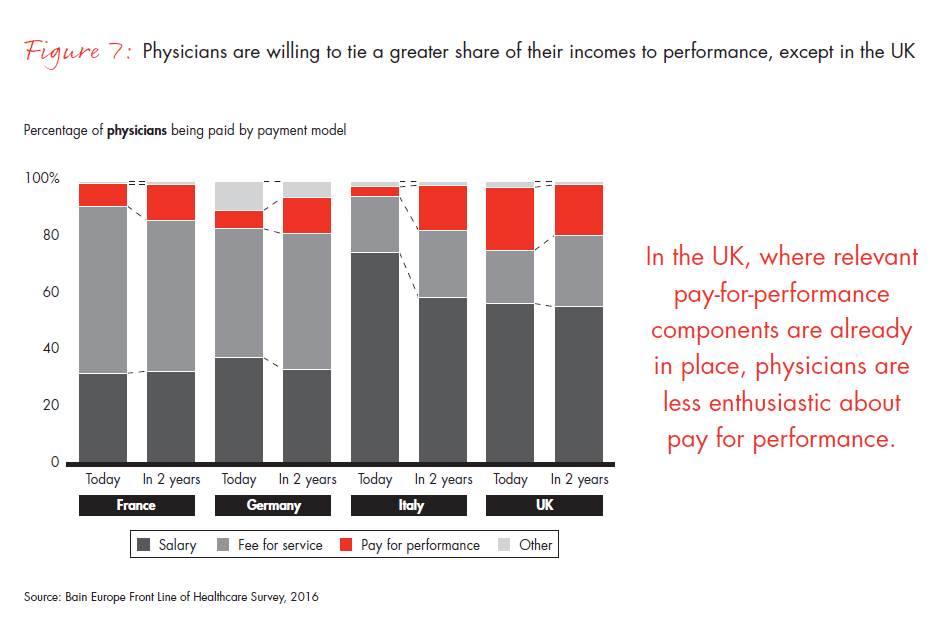
- While starting from low levels, physicians seem willing to tie a greater share of their incomes to performance. This is true for all the countries we surveyed except the UK, where relevant pay-for-performance components already exist and physicians have become more critical about the increased reliance on them.
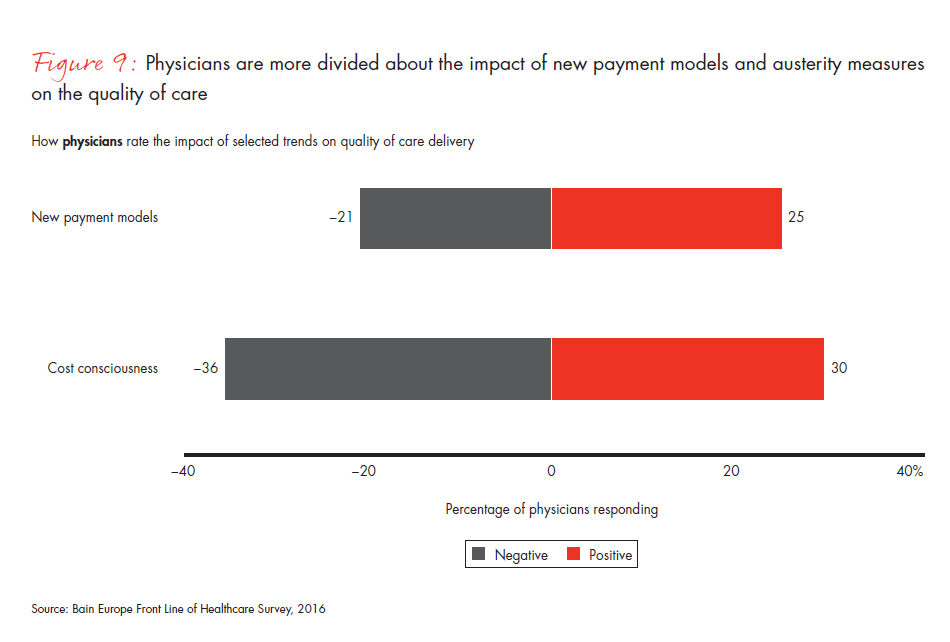
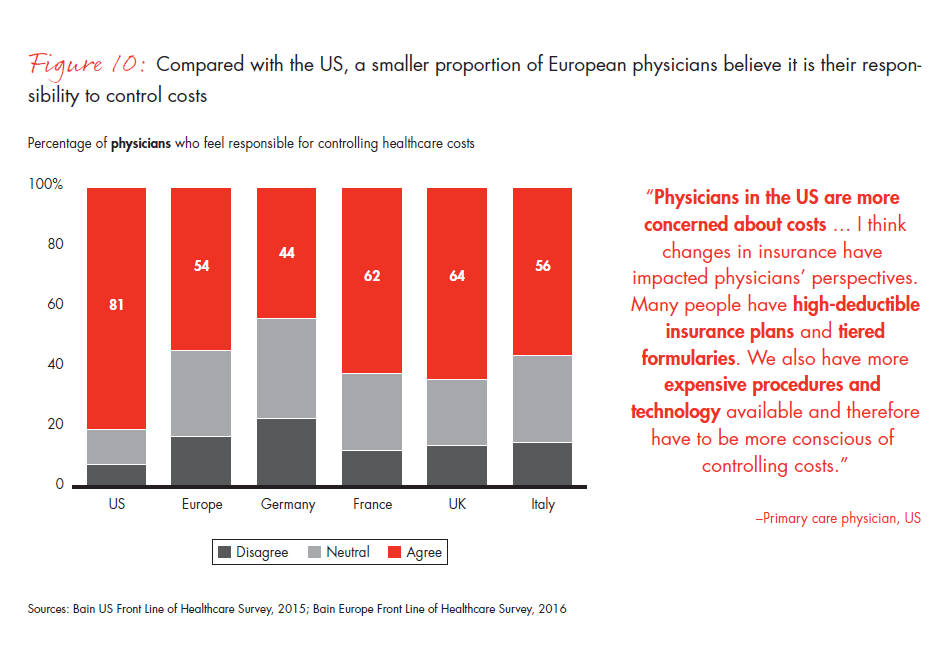
- European physicians have more negative views than their US counterparts about new payment models and austerity measures, with many saying they will have a negative impact on the quality of care. A far smaller percentage of European physicians report having a personal responsibility to control costs, compared with physicians in the US, with specifically low levels reported in Germany. The larger role of governments in European healthcare and smaller profit pools may be reasons for the divergence of views.
- A large share of European physicians say their healthcare systems are ill prepared to address the needs of an aging patient population, with 83% of survey respondents saying an aging population will be the biggest catalyst for change in European healthcare. Alarmingly, 42% of those think the aging population will have a negative effect on their ability to deliver high-quality care.
2. Medtech
- Bain’s survey of 167 procurement officers and 441 surgeons across four countries shows purchasing decisions for medical technology are becoming increasingly centralized. The percentage of surgeons reporting that their procurement departments set direction or even lead the decision making for the purchase of tools and devices has risen to 35%, up from 23% three years ago.
- Competition will become fierce as hospitals switch to preferred vendor programs, giving category leaders strong advantage. In Germany, 91% of surveyed procurement officers use 10 or fewer vendors for devices today, compared with 60% three years ago.
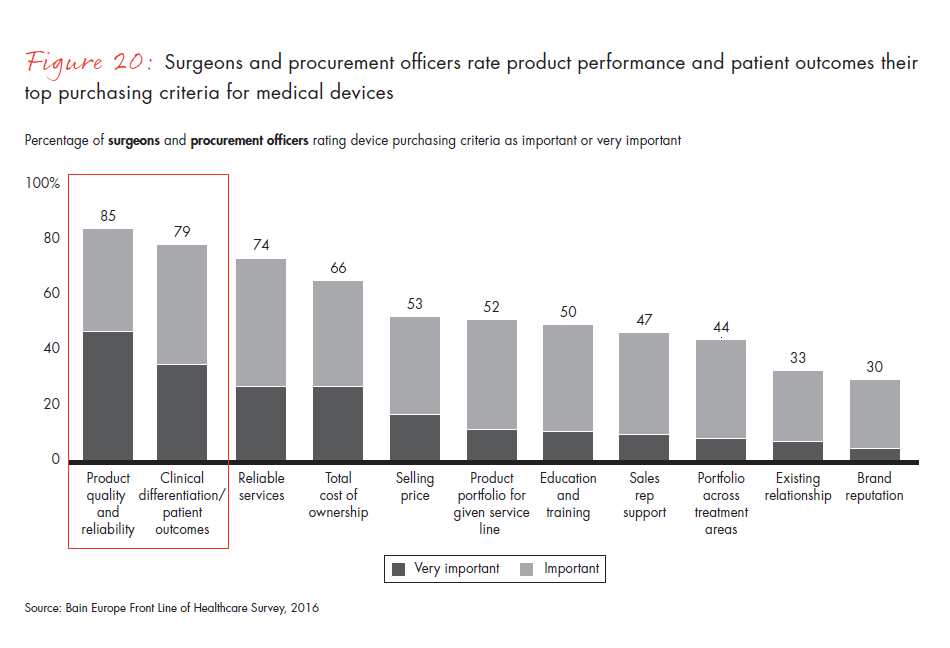
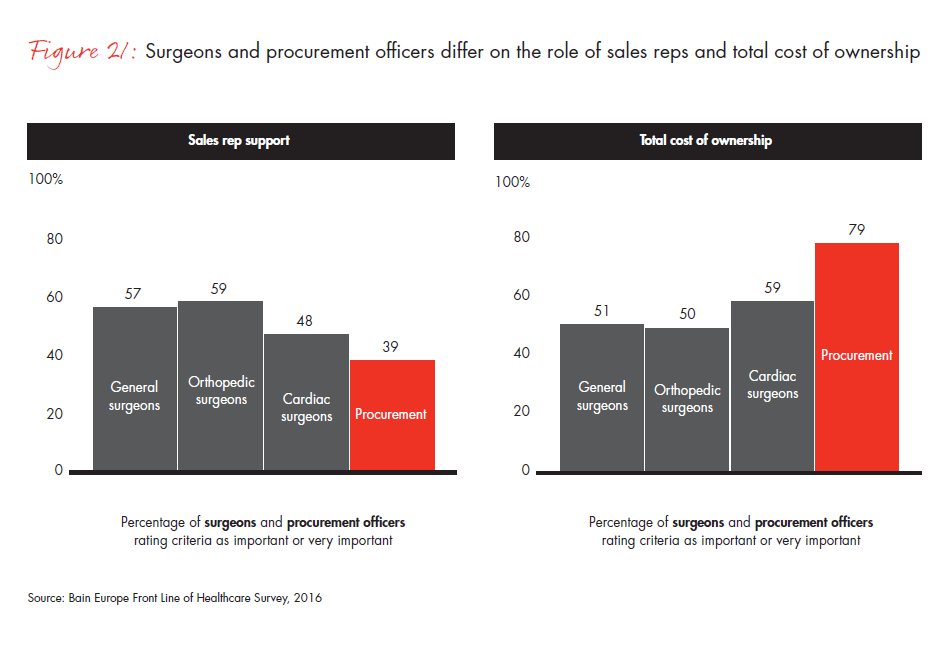
- The stakeholder landscape has become more complex, as surgeons and procurement officers express distinct and different preferences that inform their purchasing decisions. While surgeons and procurement officers agree that reliability and clinical outcomes are important purchasing criteria, they diverge on the importance of total cost of ownership.
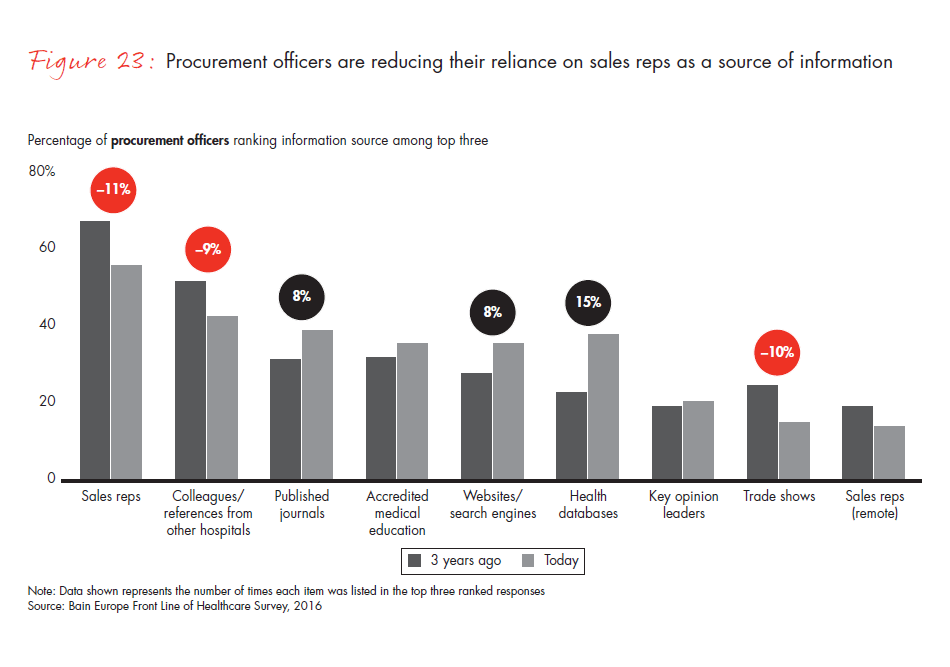
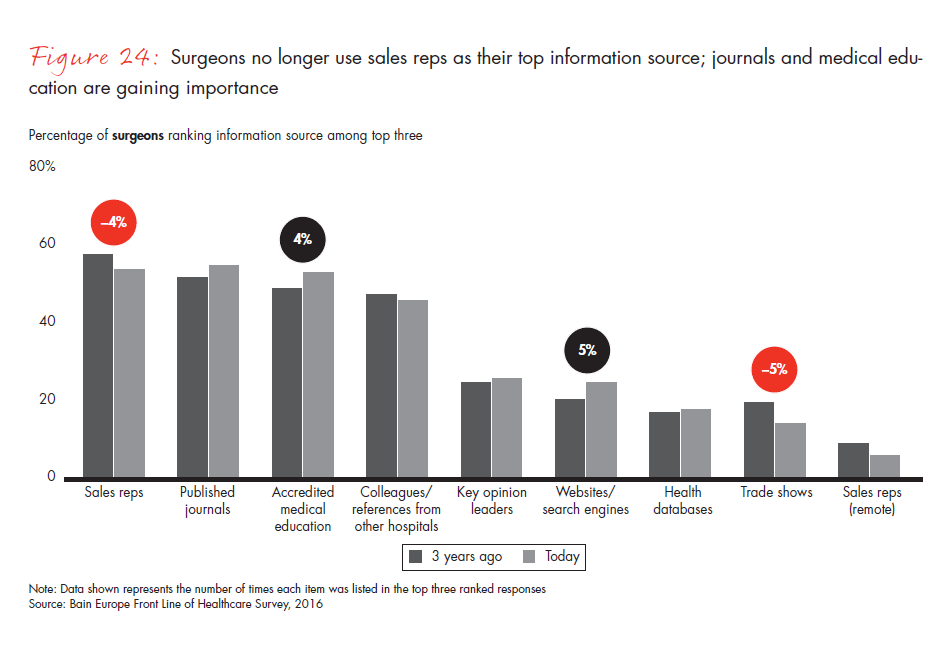
- Surgeons no longer see sales representatives as their top information source—journals and medical education are gaining importance. Procurement officers are also reducing their reliance on them. Medtech manufacturers should focus on the well-accepted educator role of sales reps.
- European surgeons and procurement officers rank clinical innovation as their greatest unmet need, while US colleagues put lower costs first. European procurement officers consider the restriction of unnecessary diagnostics as by far the biggest cost-saving opportunity.
- In this changing landscape, where stakeholders increasingly demand data to prove clinical and economic outcomes, medtech companies will need to enhance their ability to aggregate data to support claims of efficacy and efficiency. Sales reps will need more tools and training to address the total cost of ownership and enhance their role as educators.
3. Pharma
- Bain’s survey of 750 nonsurgical physicians across four countries and six specialties shows that European physicians still perceive a relatively high degree of independence in prescribing decisions, compared with physicians in the US. In France 80% feel empowered to decide which drug to prescribe.
- Safety, real-world evidence and patient outcome data remain the most important prescribing criteria for physicians in Europe and the US. Only 45% of European physicians consider price an important criterion, compared with 61% of US physicians. But the importance of price varies significantly across Europe.
- European physicians view scientific education as their greatest unmet need. They cite the need for different data (comparative studies), more of the same data (real-world evidence) and more credible data (less marketing). Their US counterparts ranked cost and clinical innovation as their most critical unmet needs.
- Physicians continue to turn away from sales representatives as a source of information and toward sources perceived as more unbiased. Only 43% of physicians cite sales reps as one of their top three sources of information about a drug, compared with 53% three years ago.
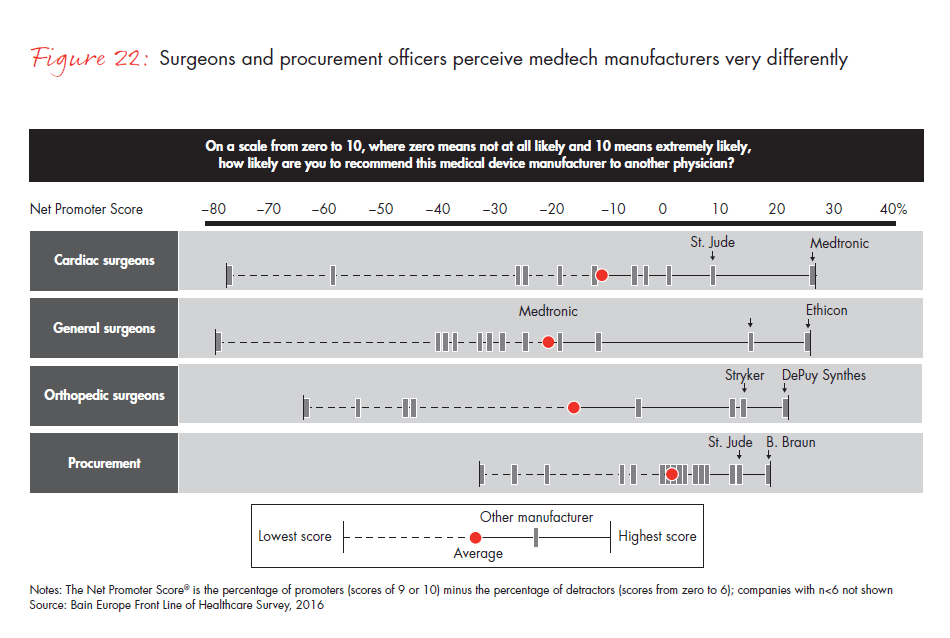
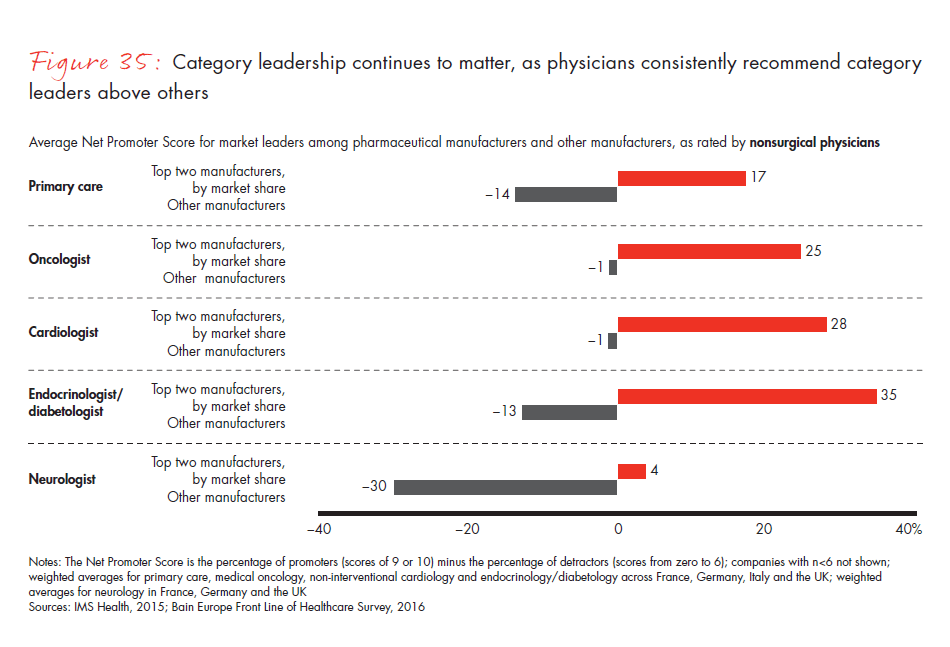
- Companies that are leaders in a given category within a country are the same companies that physicians recommend and view as innovative. They are better at providing a more positive customer experience to physicians than their competitors, underscoring the key advantage of category leadership in the pharmaceutical industry.
- To win, pharma manufacturers will need to refine their go-to-market model in the channels that matter most, demonstrate value, provide unbiased medical information and use a credible omnichannel approach to disseminate their data to stakeholders.
4. Hospitals
- Bain’s survey of 904 surgical and nonsurgical hospital physicians across four European countries and nine specialties examined their views on care delivery at their organizations. To measure satisfaction, we used a tested indicator of advocacy, the Net Promoter Score®, and assessed whether or not physicians would recommend their organizations to others as a place to work or to receive care.
- Hospital physicians across Europe report a worryingly low level of satisfaction. Not only are they unlikely to recommend their organizations to others as a place to work, but a high proportion would not recommend their organizations to friends or colleagues in need of medical services, except in Germany, where 42% of physicians are highly likely to recommend their organizations.
- Physicians question their organizations’ ability to deal with the medical challenges ahead. Fewer than one-third believe that their organizations have the right structures in place and are making the investments required to achieve their mission.
- Hospitals that invest in creating alignment and putting the right structures in place see significant results. The Net Promoter Score for physicians who truly feel inspired by their organizations’ mission and vision and who believe that their organizations actually have the right structures in place to effectively address the medical challenges ahead is some 50 points higher than for physicians who do not.
- Governments as well as public and private hospitals need to review and adjust the processes, infrastructure and capabilities required to provide high-quality care and professionalize hospital management. Hospital administrators should engage physicians more effectively and improve the way they organize care delivery and manage their scarce medical resources.
Appendix: Methodology
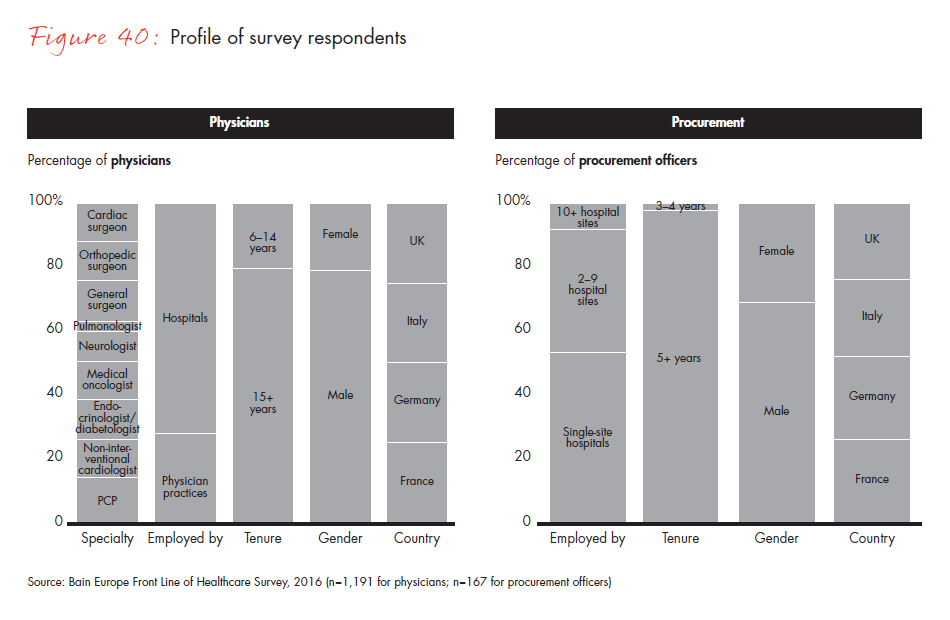
The Bain Europe Front Line of Healthcare survey was conducted in 2016 by the physician panel at SERMO, a leading global social network for physicians and healthcare market researcher. It included a total of 1,191 physicians and 167 procurement officers from Germany, France, Italy and the UK. The survey evenly sampled physicians across these countries: Sample size was between 295 and 302 physicians in each country, and within countries, no geographic region was overrepresented.
The survey focused on nine specialties: three surgical and six nonsurgical. The surgical specialties were general, cardiac and orthopedic surgery, and participants in these specialties provided input for the care delivery, medtech and hospital sections of this report. Nonsurgical specialties were primary care, medical oncology, non-interventional cardiology, endocrinology/diabetology and, in the UK, Germany and France, neurology; in Italy, we replaced neurology with pulmonology. Participants in these nonsurgical specialties provided input for the sections about care delivery, pharma and hospitals. The specialties were chosen based on their global and regional revenue bases and the degree of ongoing change in the shifting healthcare environment. We also surveyed procurement officers to capture purchasing trends for medical devices.
SERMO’s online panel of healthcare professionals conducted the survey in local languages. The company carried out strict quality checks to ensure maximum data integrity, such as consistency and straight-lining checks, speeding control and quality assessments of free text answers. The sample was weighted by specialty per country such that our results are nationally representative and internationally comparable for the specialties we selected. For overall European results, the sample was additionally weighted according to the number of physicians per country.
When measuring advocacy, we used the Net Promoter Score, which was developed by Bain & Company and is a tested indicator of advocacy. We asked two Net Promoter questions to assess physicians’ likelihood of recommending their organizations to friends or colleagues (a) as a place to work or (b) when in need of medical services. (A positive Net Promoter Score indicates physicians’ advocacy and support for their organizations, while a negative score shows the opposite.)
Survey questions
Figure 1: To show use of analytics and clinical tools, we calculated the percentage of physicians currently using a variety of tools. For risk-based payment models, we looked at the percentage currently using at least one of the following models: pay for performance, bundled payment, shared savings and capitation. For management tools use and physician cost consciousness, we based percentages on the number of physicians agreeing or strongly agreeing on a Likert scale to statements. For use of metrics, we calculated the percentage of physicians who said they are evaluated on three or more metrics.
Figure 2: “Please indicate if you have used the following tools or participated in the following programs (whether by your own choice or your organization’s or hospital’s choice).”
Figure 3: “Please indicate if you have used the following tools or participated in the following programs (whether by your own choice or your organization’s or hospital’s choice).”
Figure 4: “Please rate the impact of the trends below on your ability or the ability of your organization to deliver high-quality care to your patients.”
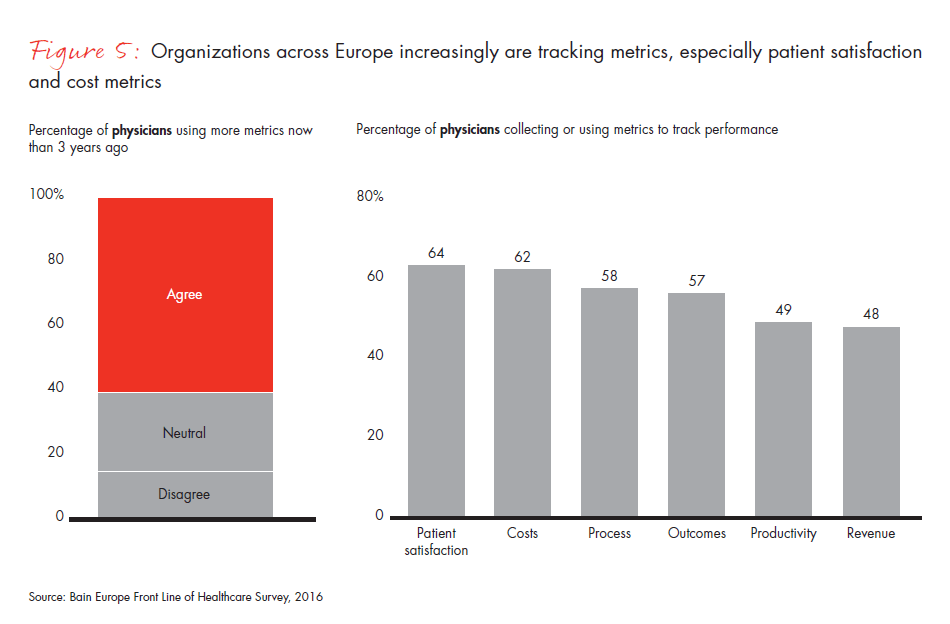
Figure 5: Left chart: “The healthcare environment in which I typically work is using more metrics now than three years ago.” Right chart: “Which of the following metrics are collected and monitored within the healthcare environment in which you typically work, and how are those metrics used?”
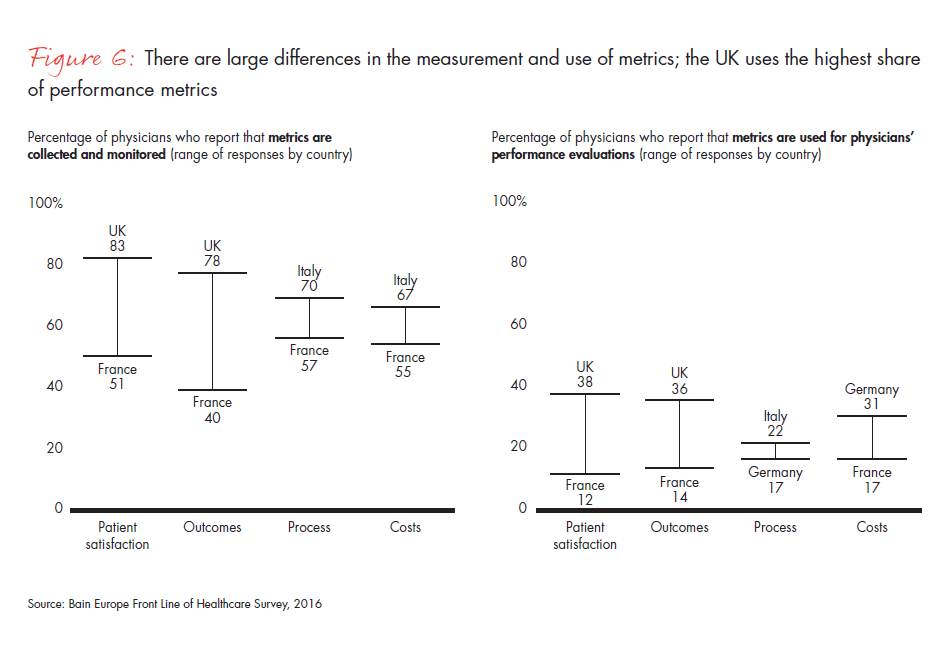
Figure 6: “Which of the following metrics are collected and monitored within the healthcare environment in which you typically work, and how are those metrics used?”
Figure 7: “During the last two years, how have you been paid for the care and the services you provided to your patients?” and “How would you like the share of your individual payment components to be in the future, to further improve today’s delivery of care?”
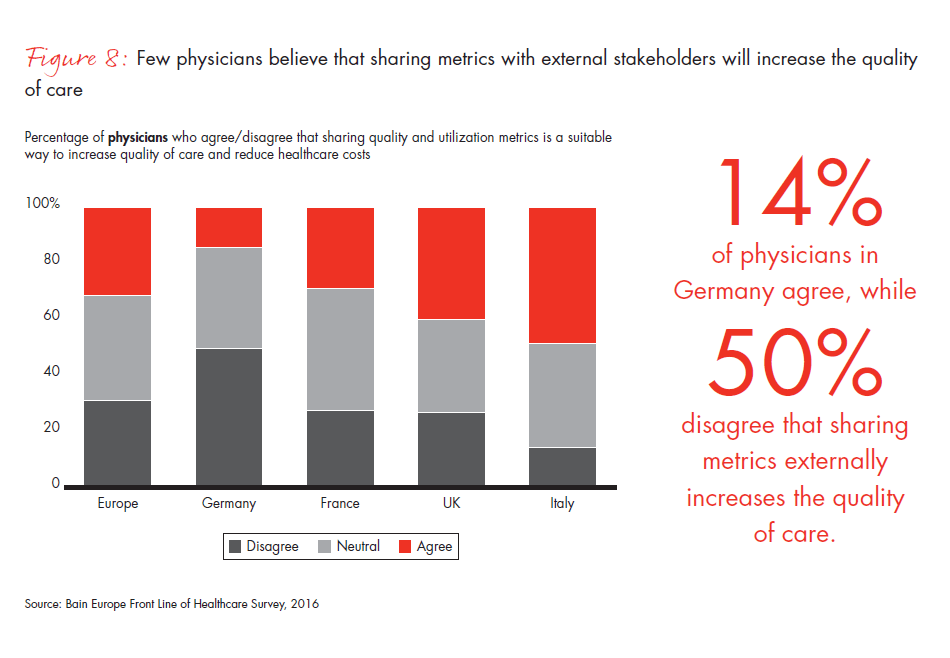
Figure 8: “Increased sharing of metrics with external stakeholders (e.g., patients) is a suitable way to reduce costs and improve the quality of care delivery.”
Figure 9: “Please rate the impact of the trends below on your ability or the ability of your organization to deliver high-quality care to your patients.”
Figure 10: “I feel it is part of my responsibility as a physician to help bring healthcare costs under control.”
Figure 11: Left chart: “How do you expect these trends to continue shaping your job in the near future, e.g., in the next two years?” Right chart: “Please rate the impact of the trends below on your ability or the ability of your organization to deliver high-quality care to your patients.”
Figure 12: Left chart: “How do you expect these trends to continue shaping your job in the near future, e.g., in the next two years?” Right chart: “Please rate the impact of the trends below on your ability or the ability of your organization to deliver high-quality care to your patients.”
Figure 13: “There are several purchasing methods that healthcare facilities use when purchasing medical devices. Please check the option that best describes the hospital or organization where you spend/spent the majority of your time today and three years ago.”
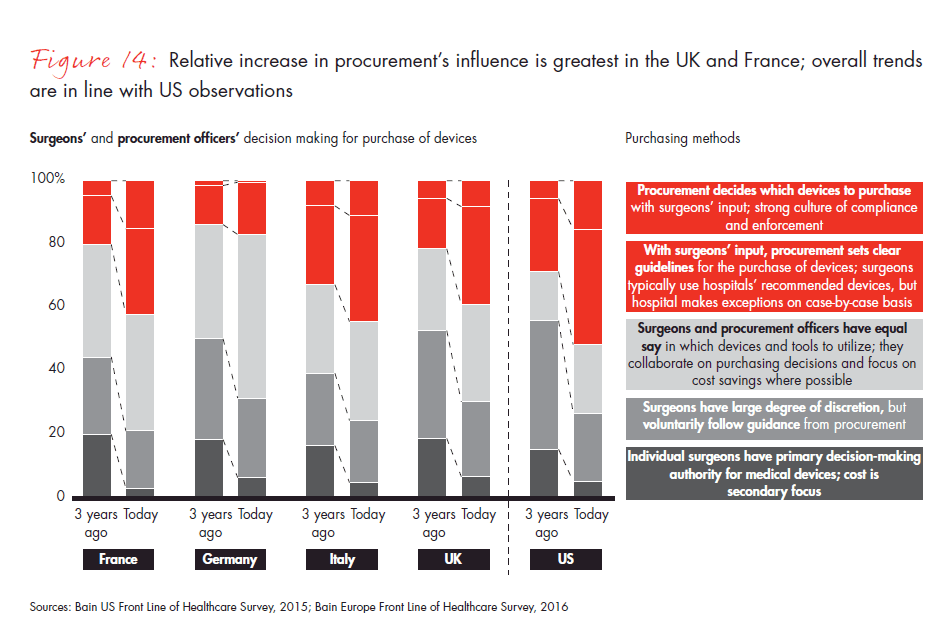
Figure 14: “There are several purchasing methods that healthcare facilities use when purchasing medical devices. Please check the option that best describes the hospital or organization where you spend/spent the majority of your time today and three years ago.”
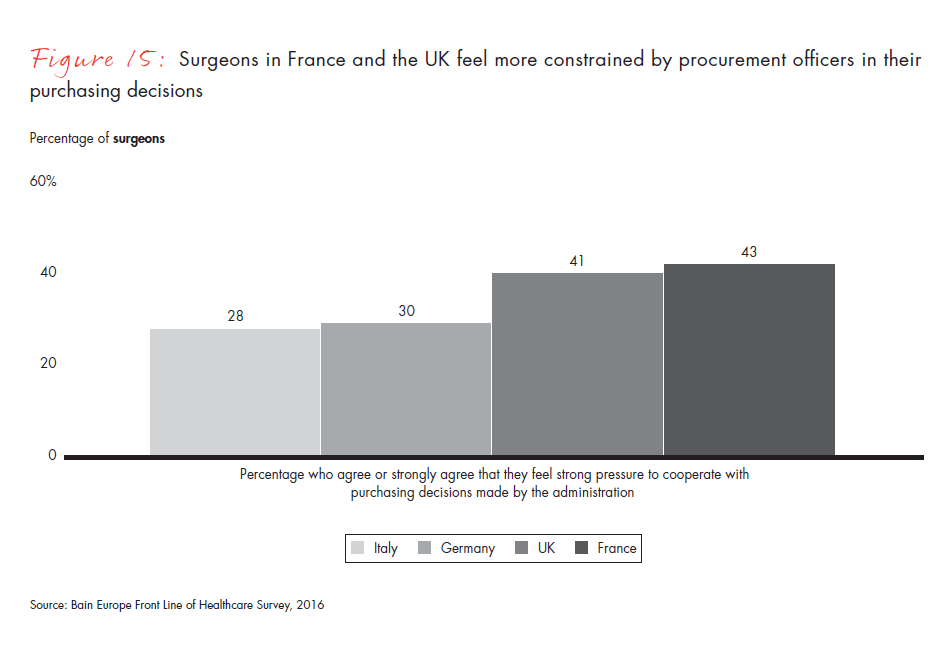
Figure 15: “To what extent do you agree or disagree with the following statements about medical devices?” Responses from surgeons only.
Figure 16: “For the questions below, think about the number of vendors you purchase(d) high-tech medical devices and tools from within a given service line now and three years ago.” Responses from procurement officers only.
Figure 17: “For the questions below, think about the number of vendors you purchase(d) high-tech medical devices and tools from within a given service line now and three years ago.” Responses from procurement officers only.
Figure 18: “To what extent are the following cost-saving initiatives a priority for your organization?” Responses from procurement officers only.
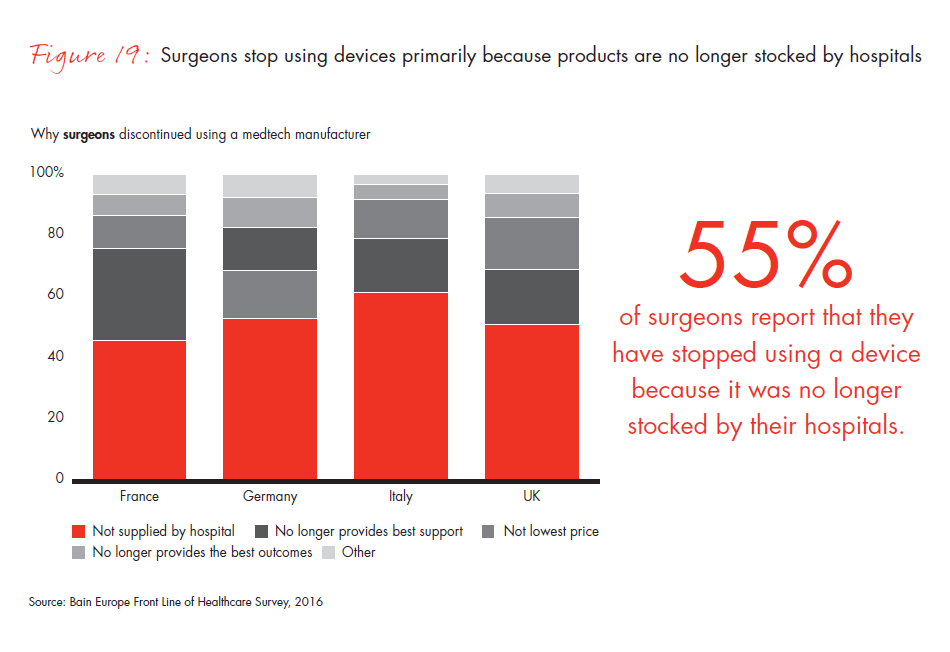
Figure 19: “Please select the reason that best describes why you discontinued using those devices and tools.” Responses from surgeons only.
Figure 20: “How important is each of the following criteria when deciding which manufacturer to use for your medical devices?”
Figure 21: “How important is each of the following criteria when deciding which manufacturer to use for your medical devices?”
Figure 22: “On a scale from zero to 10, where zero means not at all likely and 10 means extremely likely, how likely are you to recommend this manufacturer to another physician?”
Figure 23: “Today and three years ago, which of the following sources do/did you utilize most to get information about medical devices and tools? Please rank three to five sources, from most utilized to least utilized, with No. 1 as most utilized. Do not rank if you do not utilize.” Responses from procurement officers only.
Figure 24: “Today and three years ago, which of the following sources do/did you utilize most to get information about medical devices and tools? Please rank three to five sources, from most utilized to least utilized, with No. 1 as most utilized. Do not rank if you do not utilize.” Responses from surgeons only.
Figure 25: “Please list the most significant unmet need that could be addressed with medical technology, devices or tools.” Responses from surgeons only.
Figure 26: “Please list the most significant unmet need that could be addressed with medical technology, devices or tools.” Responses from procurement officers only.
Figure 27: “Where is there opportunity for your organization to achieve cost reduction(s)?” Responses from procurement officers only.
Figure 28: “To what extent do you agree or disagree with the following statements about your prescribing situation?” Responses from nonsurgical physicians only.
Figure 29: “How important are the following criteria when deciding which drug(s) to prescribe to a patient?” Responses from nonsurgical physicians only.
Figure 30: “How important are the following criteria when deciding which drug(s) to prescribe to a patient?” Responses from nonsurgical physicians only.
Figure 31: “Please list the most significant unmet need that a pharmaceutical company could address through its products and services, to improve the quality of care you deliver to your patients today.” Responses from non-surgical physicians only.
Figure 32: “Today, which of the following sources do you utilize most to get information about pharmaceutical products?” and “Three years ago, which of the following sources did you utilize most to get information about pharmaceutical products?” Responses from nonsurgical physicians only.
Figure 33: “Today, which of the following sources do you utilize most to get information about pharmaceutical products?” and “Three years ago, which of the following sources did you utilize most to get information about pharmaceutical products?” Responses from nonsurgical physicians only.
Figure 34: “Today, which of the following sources do you utilize most to get information about pharmaceutical products?” Responses from nonsurgical physicians only.
Figure 35: “On a scale from zero to 10, where zero means not at all likely and 10 means extremely likely, how likely are you to recommend this manufacturer to another physician?” Responses from nonsurgical physicians only.
Figure 36: “On a scale from zero to 10, where zero means not at all likely and 10 means extremely likely, how likely are you to recommend your practice or organization to a friend or colleague as a place to work?” Responses from physicians working in hospitals only.
Figure 37: “How likely are you to recommend your practice or organization to a friend or colleague in need of medical services?” Responses from physicians working in hospitals only.
Figure 38: “To what extent do you agree or disagree with the following statements about your employer?” Responses from physicians working in hospitals only.
Figure 39: “To what extend do you agree with the following statements about your employer?” and “On a scale of zero to 10, where zero means not at all likely and 10 means extremely likely, how likely are you to recommend your practice or organization to a friend or colleague as a place to work?” Responses from physicians working in hospitals only.
Authors
This report was prepared by Christian Rebhan, Michael Kunst, Nitin Chaturvedi, Loic Plantevin and Valerio Di Filippo, who are partners with Bain’s Healthcare practice. Christian Rebhan is a partner with Bain & Company based in Zurich. Nitin Chaturvedi is a partner based in London. Loic Plantevin is a partner based in Paris. Valerio Di Filippo is a partner based in Milan. Michael Kunst is a partner based in Munich, and he leads the firm’s Healthcare practice in Europe.
Acknowledgments
The authors wish to give special thanks to Nathalie Fetzer-Hoernig for her work on this report and to the physician panel at healthcare market researcher SERMO for conducting the Bain Europe Front Line of Healthcare Survey.
Net Promoter Score® is a trademark of Bain & Company, Inc., Fred Reichheld and Satmetrix Systems, Inc.








































