レポート

Executive summary
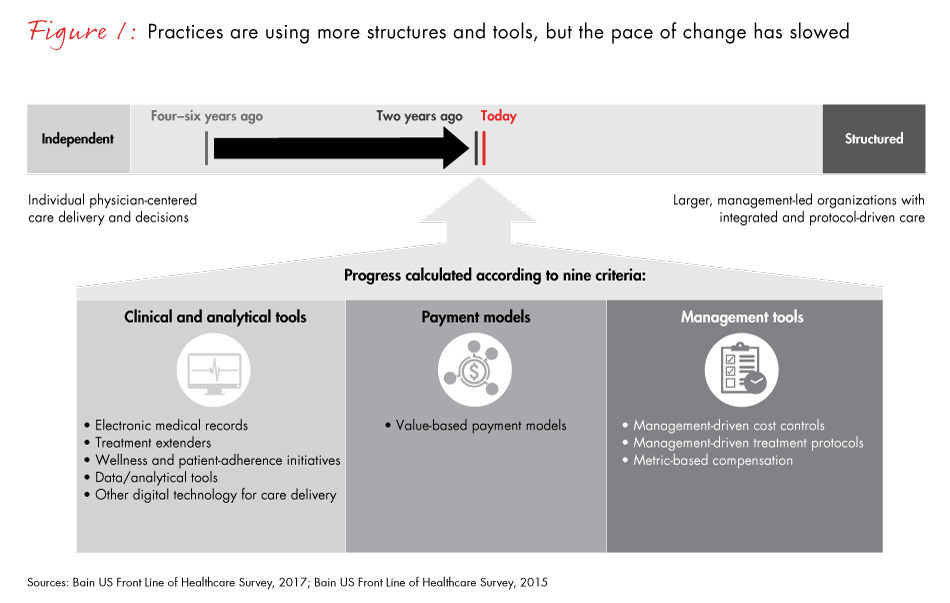
The US healthcare industry is still in search of a cure—a breakthrough model that can deliver high-quality care at lower cost. Over the past five years, hospitals, healthcare groups and medical practices have adopted new management structures and systems to curb spiraling costs. But none has proven to be a compelling way forward, and the pace of change since 2015 has slowed substantially.
Bain’s 2017 US Front Line of Healthcare Survey reflects an industry in the crosscurrents of change. No disruptive innovation has altered the rules of the game in healthcare the way online retail banking has transformed the financial services market or technology has upended other industries. Finding a better model in healthcare will take more time—and physicians want a hands-on role shaping it.
Steeped in a field that requires lifelong learning, many physicians are natural innovators and quick to test new systems and tools. But they staunchly resist new approaches that could put patient care at risk. That helps explain why management-led organizations that have not fully embraced physician input, for example, have run into resistance or have failed to make a greater impact. The US healthcare model remains firmly centered on physicians.
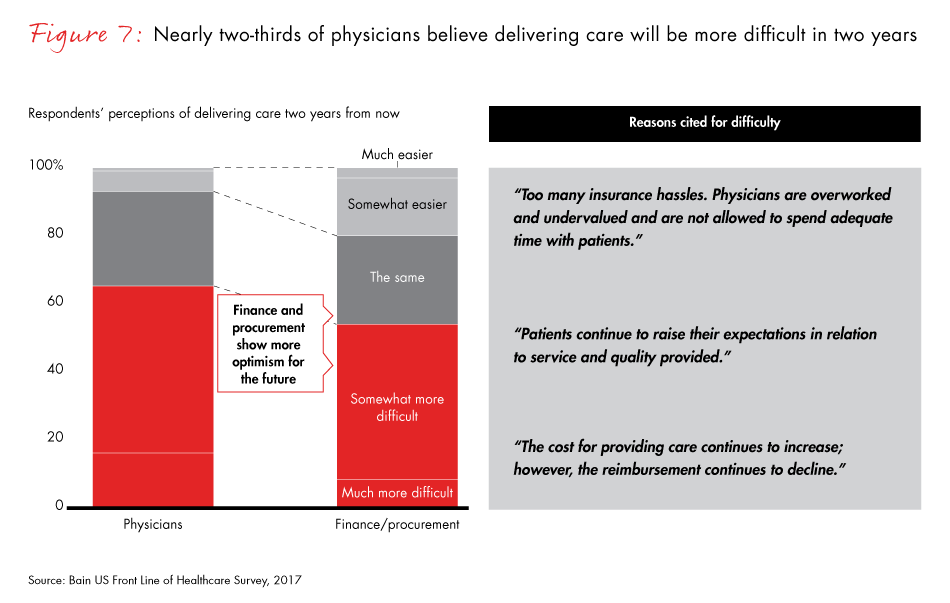
In fact, more than 60% of the physicians we surveyed believe it will become more difficult to deliver high-quality care in the next two years as they struggle to cope with a complex regulatory environment, increasing administrative burdens and a more difficult reimbursement landscape. After years of experimentation, physicians now want evidence that new models for care management, reimbursement, policy and patient engagement will actually improve clinical outcomes. Without it, they see little reason to alter the status quo and move toward wide-spread adoption.
Is there a way forward? Our survey findings indicate that bringing physicians back into the decision-making process helps create greater momentum for change. Physicians who are not aligned and engaged with their organizations have more reasons to resist new structures and systems, such as value-based payment models. By contrast, those who have a say in management decisions are much more satisfied with their working environment and more willing to lead change.
These are some of the key findings of our 2017 US Front Line of Healthcare Survey, which examines practitioners’ attitudes and concerns during a period of pivotal change for the industry. To better understand the evolving reality on the front line, we gathered input across the US from 980 physicians in eight specialties, 100 finance officers and 100 procurement officers (see appendix for methodology and survey questions).
We conducted the research for this report, our third US Front Line of Healthcare Survey, in a time of many open questions about the future of the Affordable Care Act, drug pricing and other regulations. However, the trends and business insights based on the data are likely to hold up under a broad range of policy outcomes. Our research focused not on how healthcare is funded, but on physicians’ and administrators’ priorities in care delivery—and the critical question of who has decision-making authority in the evolving healthcare system.

The US Healthcare Landscape by the Numbers
A look at the impact of the shifting healthcare landscape in the US on physicians, medtech, and pharma.
Why change has slowed
Physicians and healthcare organizations have become more cautious about adopting new structures, systems and tools for several reasons. With the first wave of change well under way, many practices already have implemented changes that are easy or required, and are reluctant to adopt more-complex systems and tools. Physicians are particularly hesitant to embrace new systems when the clinical implications and the return on investment are unproven and the administrative burden significant. As a result, many smaller physician-led practices may opt out, relying on a traditional approach to management and care.
Comparing our 2015 and 2017 survey findings, one notable slowdown has been in the adoption of value-based payment models. Many physicians anticipated a broad rollout of value-based care two years ago and a corresponding decline in practices using the traditional fee-for-service model. But few have been persuaded to switch, noting a lack of evidence that outcomes are the same or better using value-based care.
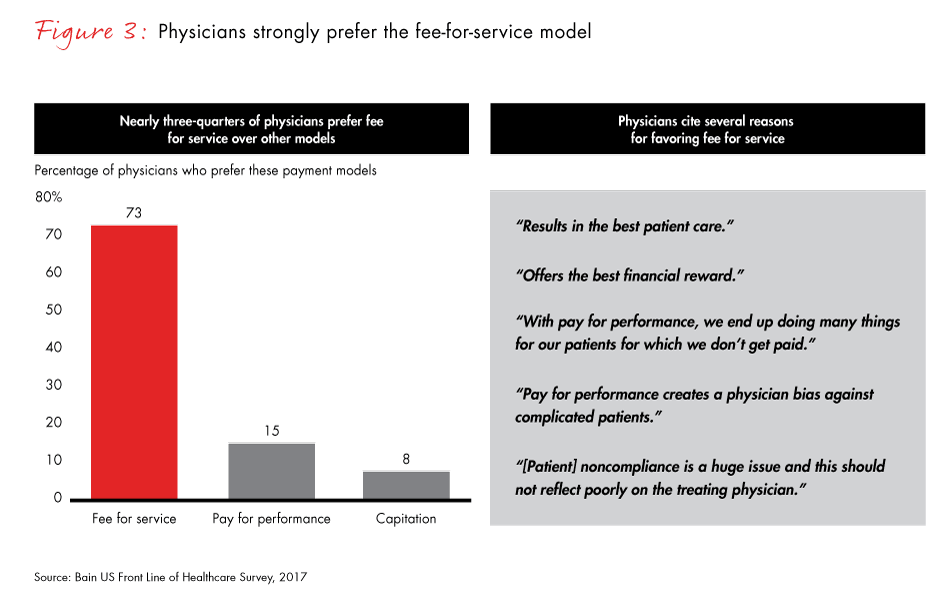
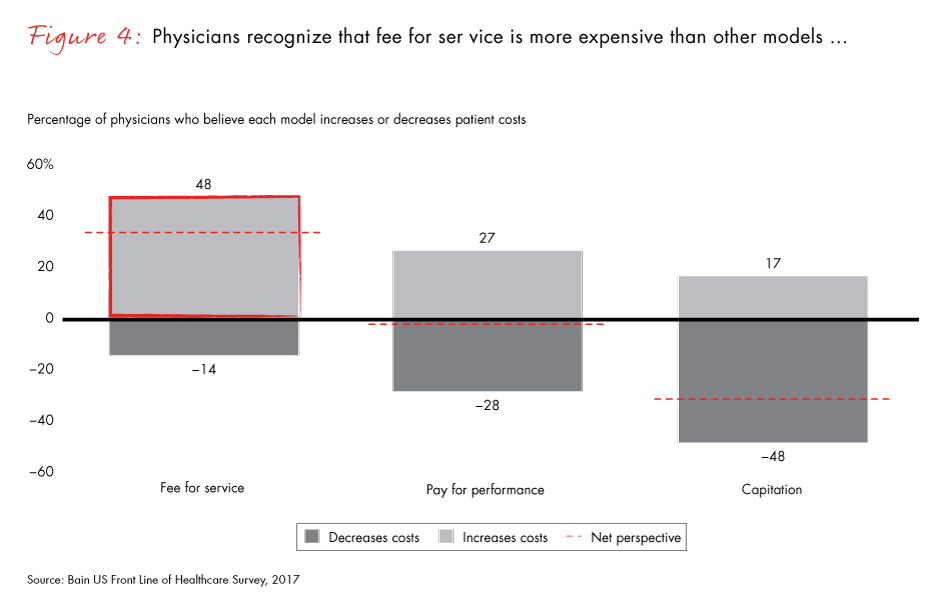
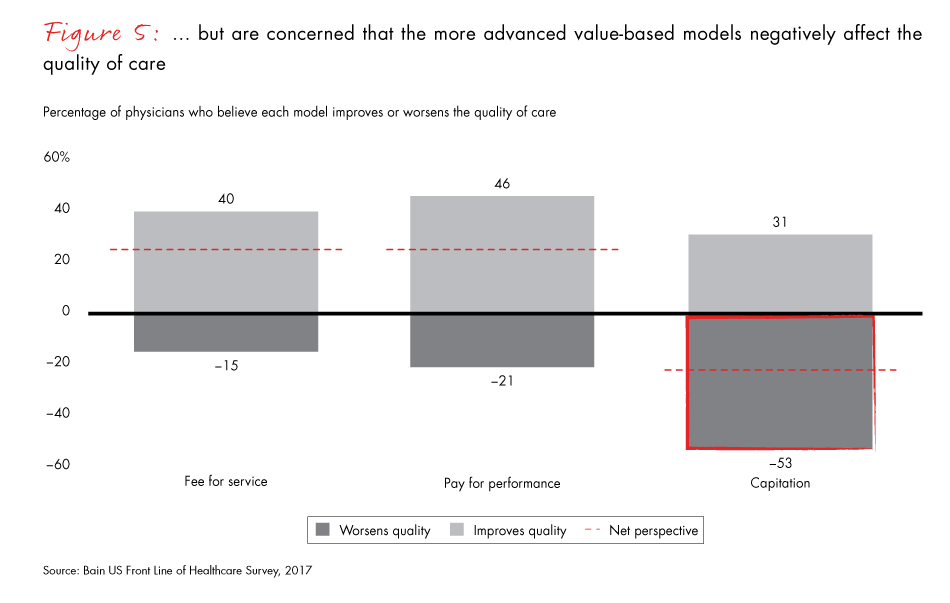
More than 70% of physicians prefer to use a fee-for-service model, citing concerns about the complexity and quality of care associated with value-based payment models. Fifty-three percent of physicians say that capitation reduces the quality of care, and most see little advantage from pay-for-performance models either. Further, many believe their organizations are not sufficiently prepared for the shift to value-based care.
Despite the reluctance to drop fee-for-service payment systems, many organizations continue to experiment with value-based care as part of a mix of payment models, recognizing the continual pull in the industry toward the value-based approach. Providers that want to move toward value-based payment models can generate greater support by working closely with their physicians to shape these models and addressing their concerns about outcomes, simplicity and fairness to all stakeholders.
Empowering physicians
Transformations are disruptive, and our 2017 survey reflects an industry in flux, but it also reveals signs of progress. Healthcare organizations on the forefront of change are moving to reempower physicians, recognizing their importance in managing costs and supporting the move toward value-based care. These organizations have realized that empowerment creates a virtuous circle: Physicians engaged in decision making are more likely to promote their organizations and to be aligned with their missions, likely leading to better care and outcomes.
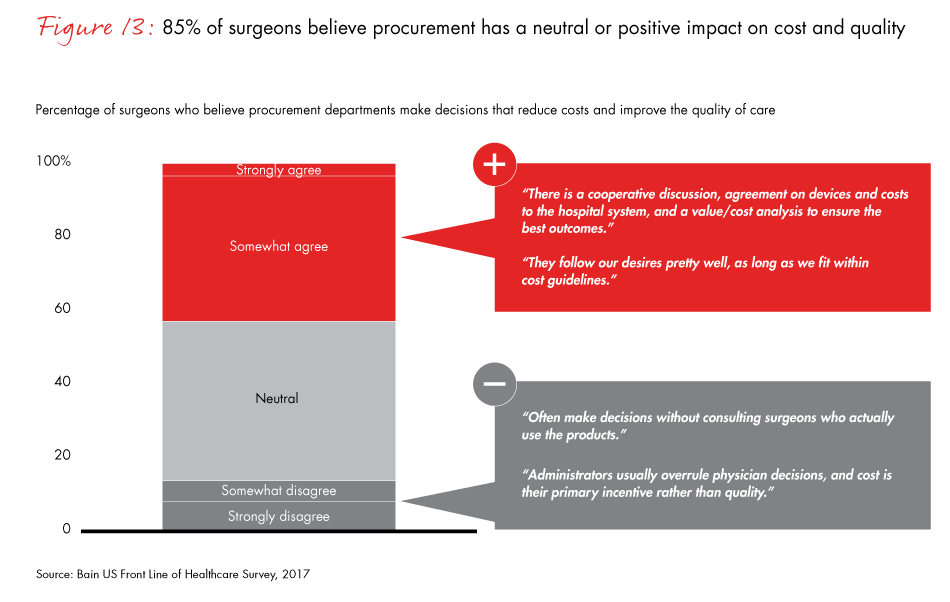
Medtech procurement is the best example of this alignment. More than 80% of surgeons and procurement officers say they work in collaborative partnerships to purchase medical equipment, weighing clinical and economic value together. Surgeons also express a more collaborative attitude about procurement than five years ago: 43% of surgeons now believe their procurement department improves costs and quality of care. “They keep costs reasonable while still allowing the majority of surgeons to use the instruments and implants they want,” one physician noted.
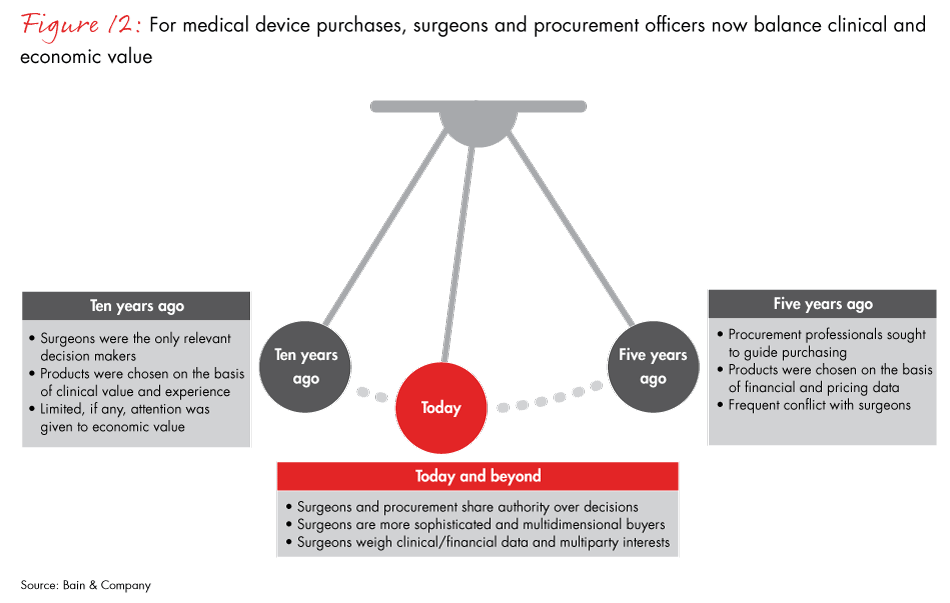
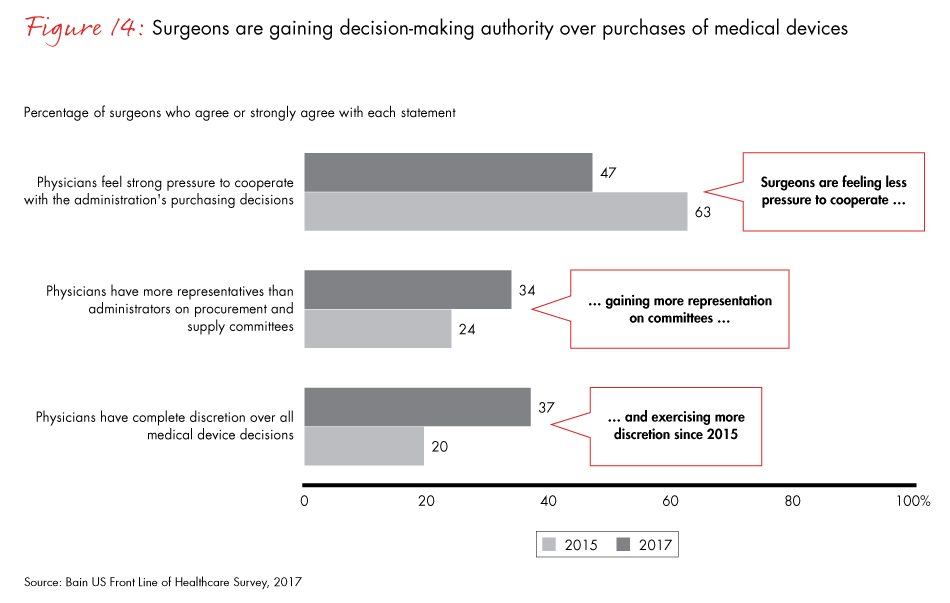
The move to reempower physicians reverses a 10-year trend that had shifted decision making away from doctors and toward procurement professionals who chose products mainly on the basis of price, often putting the two groups at odds. Our data shows that decision authority has started swinging back to surgeons, but with a new twist. Surgeons have become more sophisticated buyers, weighing clinical and financial data and considering multiparty interests when they select devices.

Front Line of US Healthcare: Giving Doctors a Say
Doctors that are involved in the decision-making process are more willing to lead change.
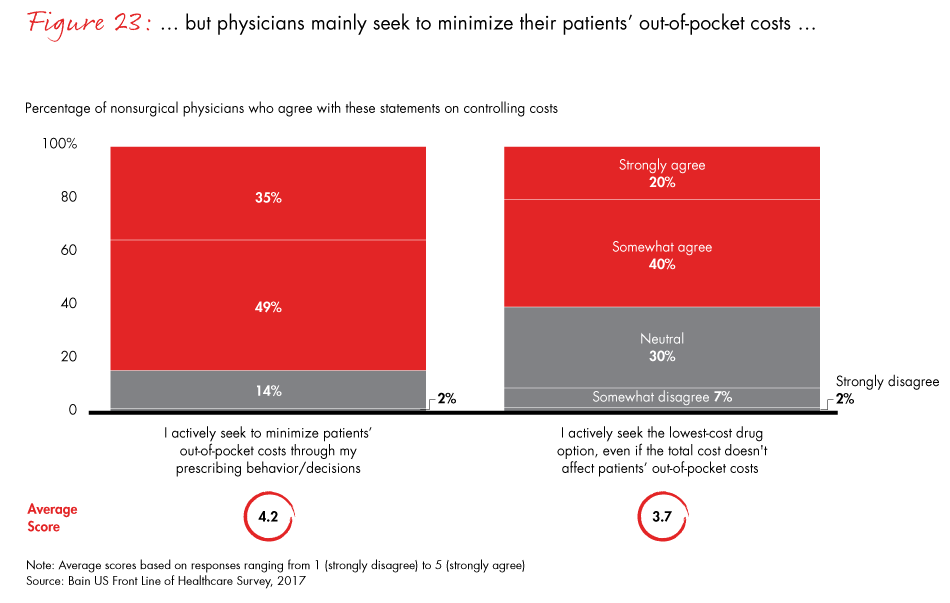
By contrast, nonsurgical physicians continue to feel their behavior constrained by payer restrictions, and they feel this most acutely in prescribing drugs, where most do not rely on pharmacy benefit managers (PBMs) to control costs or improve quality. Most physicians feel a responsibility to minimize costs, but they focus primarily on patients’ out-of-pocket expenses instead of overall costs to the healthcare system.
During the next two years, practitioners on the front line will continue to scrutinize the effectiveness of new systems and tools, both in terms of quality of care and cost. It will take time to develop clinical and economic evidence, which means the pace of change will remain slow. But it will also help the industry move toward better solutions.
As healthcare professionals grapple with new systems and approaches, all sectors of the industry are rethinking their strategies to meet evolving clinical and economic needs. In this report, we highlight how the changing environment for physicians will affect providers, medtech and pharma, and we examine some of the no-regrets moves each can take in a changing landscape.
Implications for providers
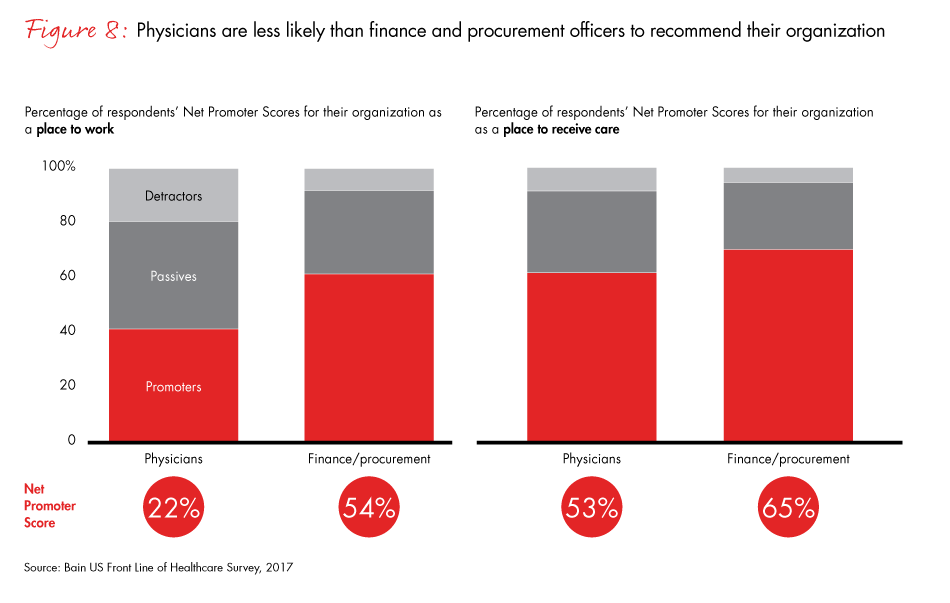
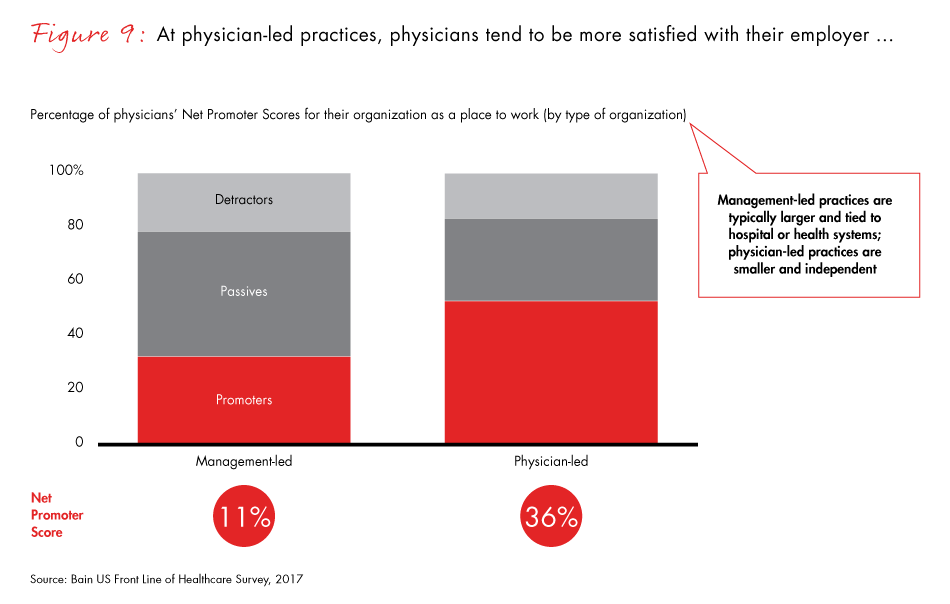
Healthcare providers that want to move toward value-based care can increase support for that shift by engaging their physicians and providing evidence that new initiatives deliver quality care at lower cost. Physicians in management-led organizations are less satisfied and less aligned with their organizations’ missions than those in physician-led organizations, the survey data shows. Management-led organizations received a Net Promoter Score® of 11% as a place to work, compared with 36% for physician-led practices. Overall, physicians give lower Net Promoter Scores to their organizations than finance and procurement officers do (see appendix for an explanation of Net Promoter Scores).
Our findings indicate management-led groups can increase physicians’ engagement by granting them greater autonomy and by adopting some of the best attributes of physician-led groups. Practices that offer a combination of efficiency and physician autonomy are likely to perform best.
Providers will have greater success at implementing change if they improve stakeholder alignment on cost-saving initiatives. Physicians need a clinical rationale for changing the way they deliver care—financial logic alone will not change long-established behaviors. Indeed, many have overlooked the role of the physician as system innovator. Physicians tell us that they are open to new cost-saving models, but need to be on the front line of change helping health systems identify which approaches create value for patients, and which don’t. For example, clinicians’ and administrators’ views differ on the importance of cost-saving initiatives. Physicians and finance officers rank care-management teams the top priority, while procurement officers say vendor consolidation and purchasing automation are most important.
Despite the slowing shift toward value-based care, healthcare organizations are aggregating at a rapid clip and continue to experiment with new governance models. Hospital systems within cities are growing by acquiring and partnering with other institutions and medical groups in the same area. The volume of hospital mergers and acquisitions increased 42% from 2010 to 2015, according to the American Hospital Association, which also says that the number of community hospitals affiliated with a healthcare system rose to 66% in 2015 from 51% in 1999. Finally, physicians continue to move away from solo practices: Only 14% were self-employed in 2017, down 6 points in two years, the Front Line survey found. This aggregation of systems and physicians could enable future change as fewer, larger organizations become the norm.
Implications for medtech
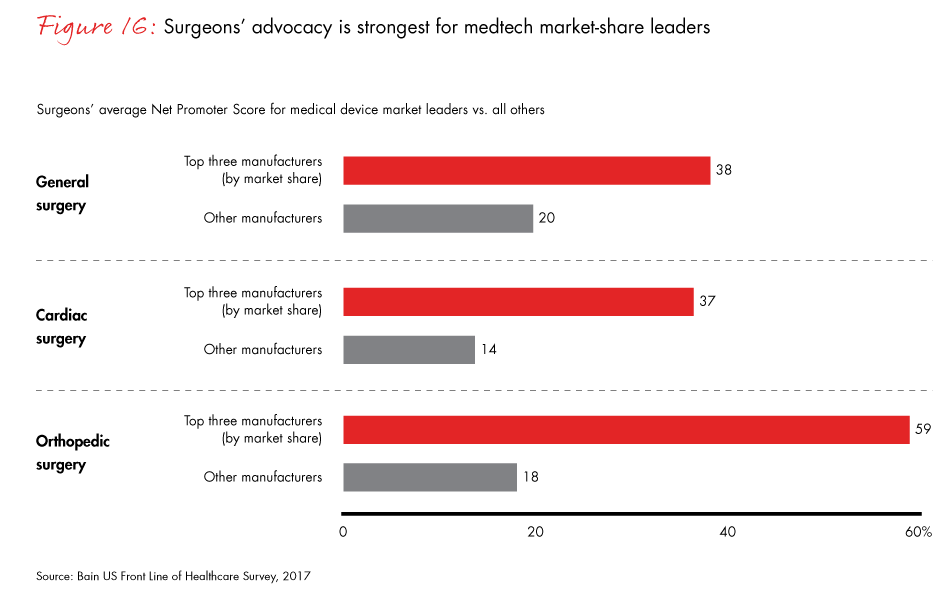
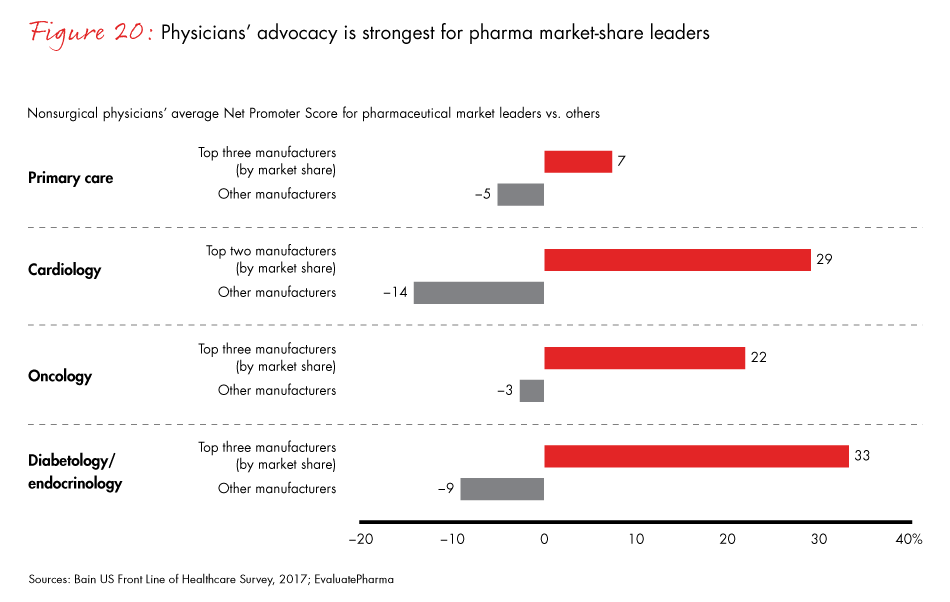
Building category leadership positions and offering value-added services can help medical device manufacturers stand out in a crowded field. More than 60% of surgeons rank “strongest existing relationship” with a manufacturer as a key purchasing criterion, up from 46% in 2015. Category leaders benefit from much stronger customer advocacy: Across general surgery, orthopedic surgery and cardiac surgery, market-share leaders, including all category leaders, receive much higher Net Promoter Scores than other manufacturers.
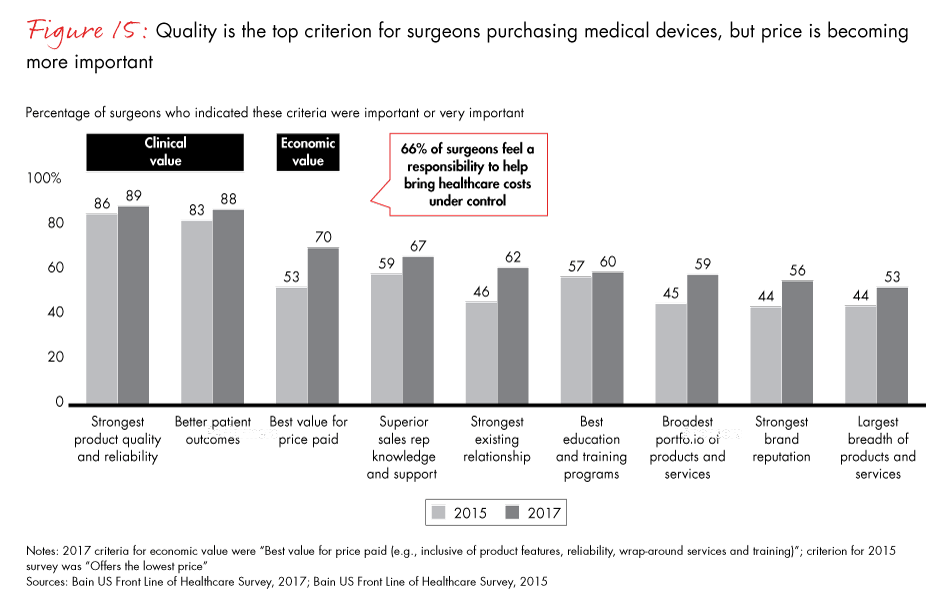
Healthcare providers continue to reward clinical innovation despite increasing pressure to control costs. Surgeons’ top criteria for medical equipment are product quality and patient outcomes. However, it’s important for medtech companies to demonstrate both the clinical and economic value of products. As surgeons regain purchasing authority, they have become more attuned to economic value and weigh financial data as part of the overall purchasing decision.

Front Line of US Healthcare 2017: The State of Medtech
Buying medical equipment has become more collaborative between surgeons and procurement.
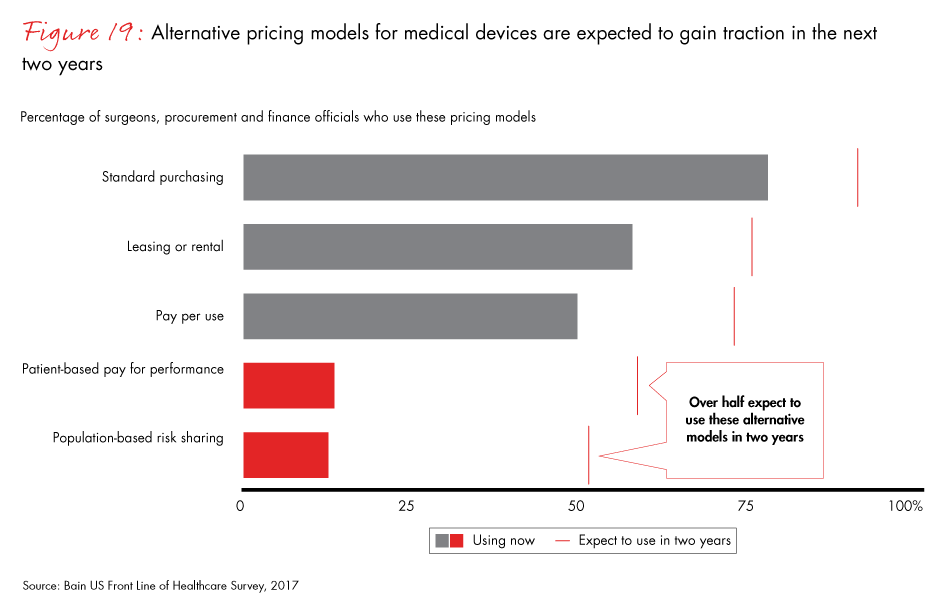
Healthcare professionals expect major increases in the use of innovative pricing models for medical devices over the next two years, including patient-based pay for performance and population-based risk sharing, to more than 50% of practices, from fewer than 15% today. Even though surgeons have overestimated the pace of adoption in the past, these models are likely to prevail in the long term. Medtech companies that get a head start now testing and refining alternative pricing models will be well positioned for an eventual uptick in their use.
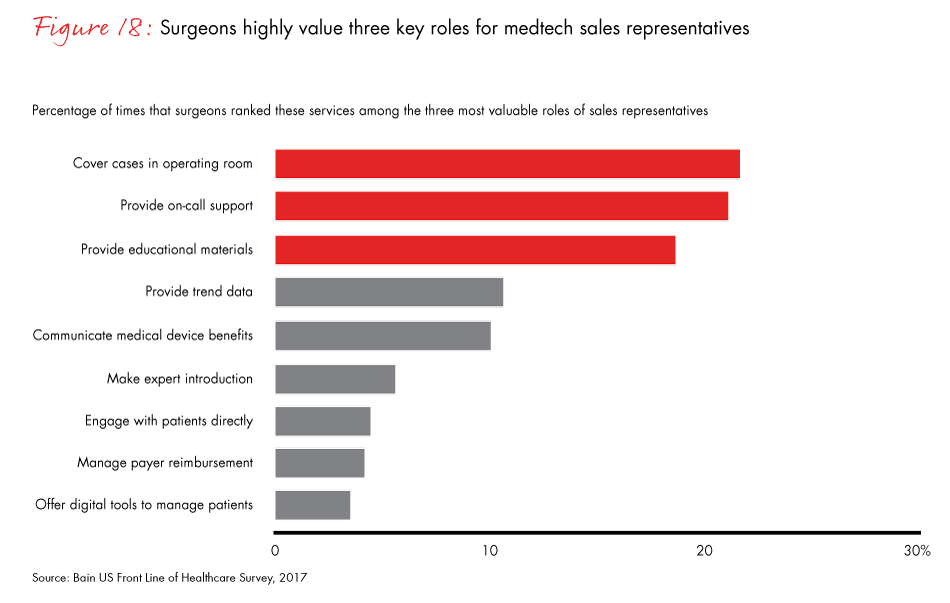
Sales representatives remain an important source of information for surgeons. Overall, the two most important roles a sales rep can play are covering cases in the operating room and providing on-call support, the survey found. But the relative importance of roles played by sales reps varies across specialties. Operating room coverage and on-call support were more important for orthopedic surgeons. General surgeons, on the other hand, value receiving educational materials more than cardiac surgeons and orthopedic surgeons do. Medtech companies can improve the effectiveness of sales reps by tailoring their role to surgeons’ needs.
Implications for pharma
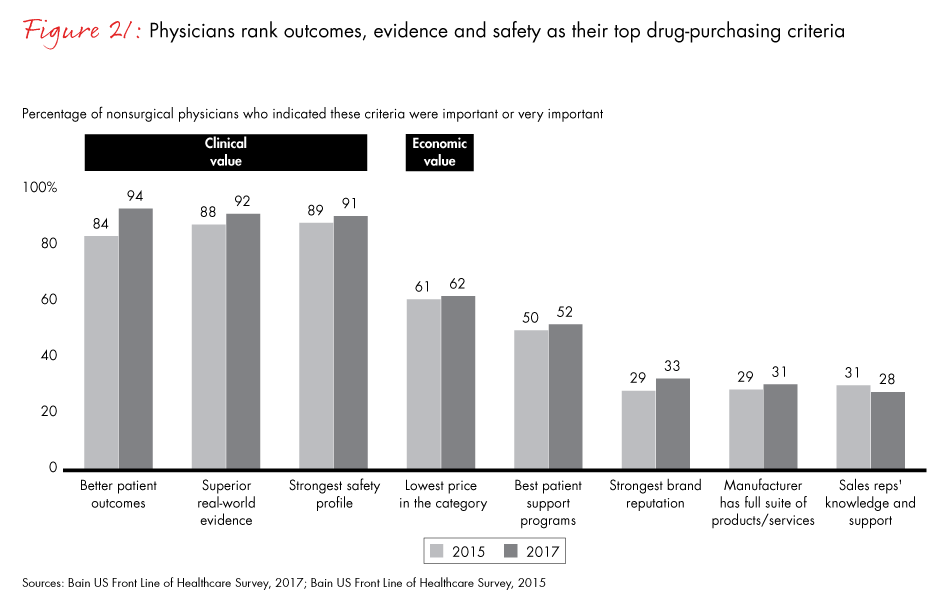
Nonsurgical physicians rank patient outcomes, real-world evidence and safety profiles as the most important factors influencing their prescribing decisions. The implications are clear: To demonstrate the clinical merits of their products, pharma companies must go far beyond the traditional clinical trial data for regulatory approval. Pharma companies that upgrade their medical affairs capabilities to generate real-world evidence underscoring the efficacy of new products will be best positioned to provide physicians the data they are seeking.
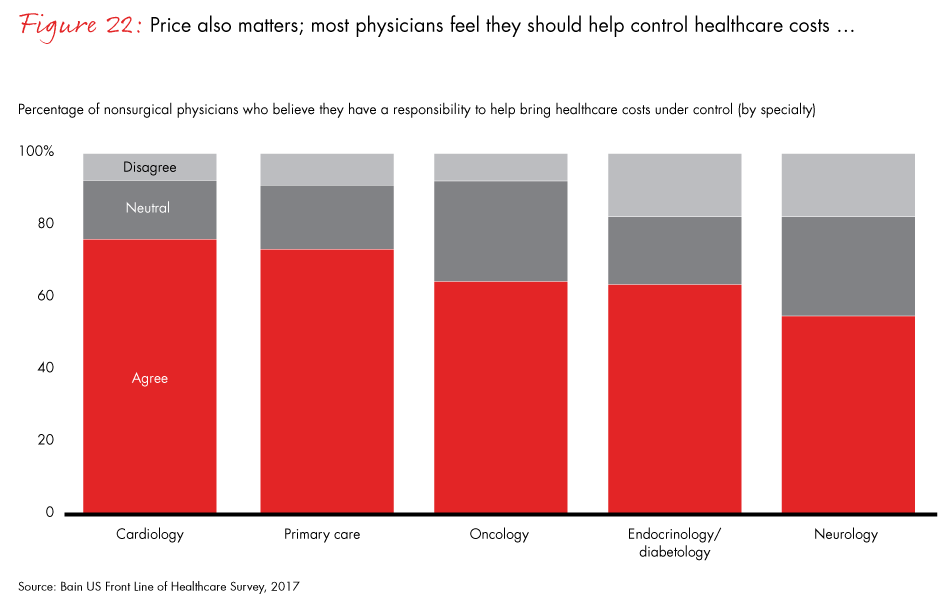
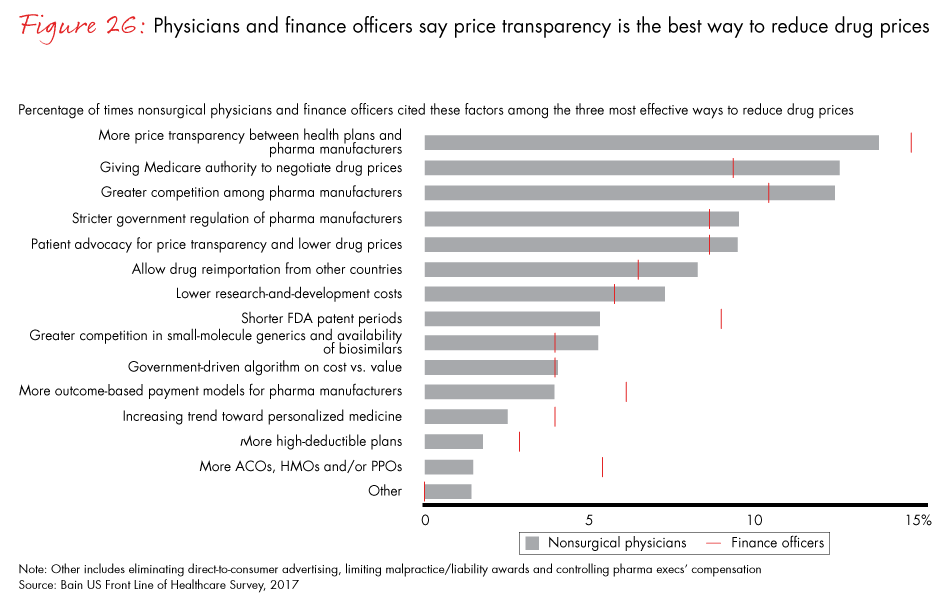
At the same time, however, physicians are increasingly concerned about the cost of drugs, at least to the extent that it affects their patients’ ability to afford therapy. Bringing drug prices down is a top priority for the healthcare industry and policy makers, but physicians say they are ill-equipped to manage total drug costs because they have limited visibility into, and limited control over, drug prices. As a result, the best they can do is to limit out-of-pocket drug costs for patients. When asked about the most effective approaches to reducing drug costs, physicians point to three key changes: price transparency between payers and pharmaceutical manufacturers, giving Medicare authority to negotiate drug prices and greater competition among manufacturers.
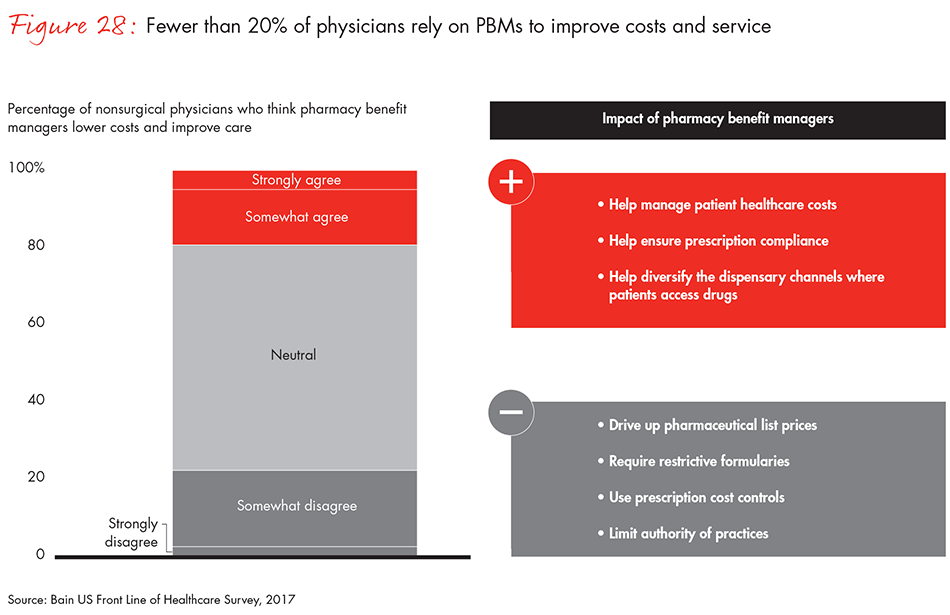
While physicians are concerned about drug pricing, they are critical of actions taken by PBMs and payers to control drug costs, particularly when these actions constrain their decision making. Only 19% of nonsurgical physicians believe PBMs improve costs and quality of care. That view contrasts sharply with surgeons’ more positive view of medtech procurement decisions, which they say help improve healthcare organizations’ bottom line without sacrificing the quality of patient care.
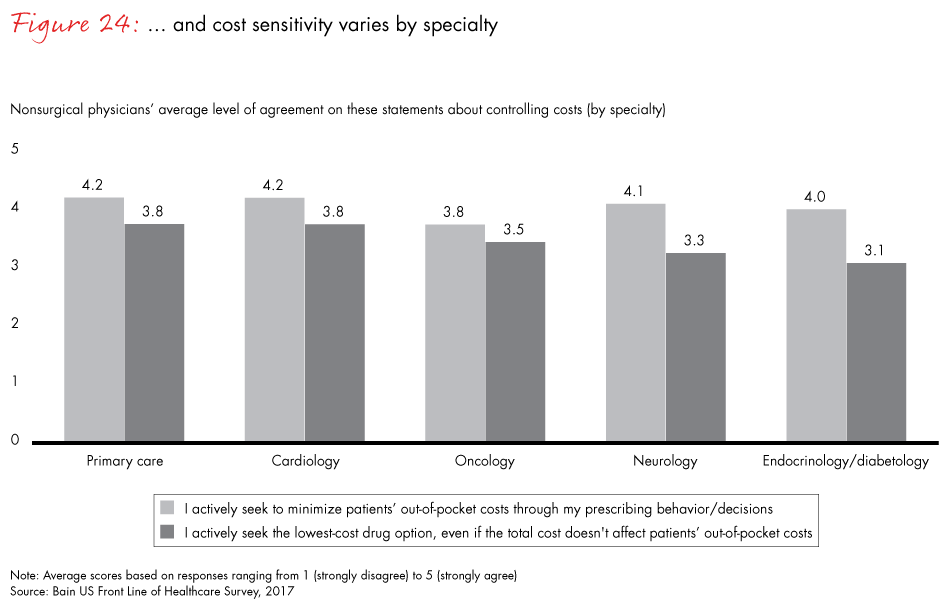
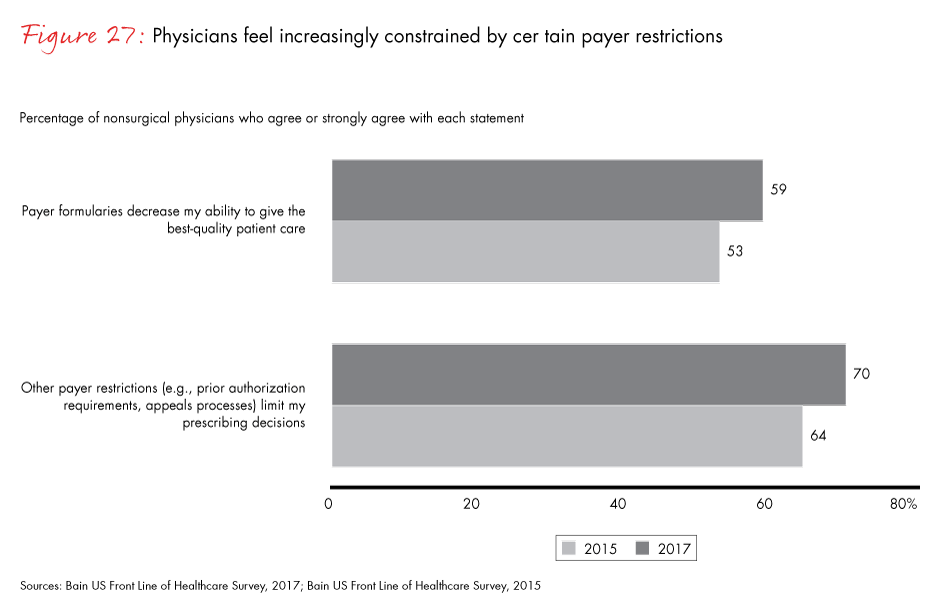
Seventy percent of nonsurgical physicians believe payer restrictions (prior authorization requirements, appeals process) limit their prescribing decisions, and 59% believe these restrictions decrease their ability to deliver high-quality care, both percentages up slightly from our survey in 2015. However, just how constrained physicians feel varies by specialty. Our survey showed medical oncologists feel notably less constrained by formularies and other payer restrictions, and are more likely than most other specialists to believe physicians have control or influence in pharmacy and therapeutics committees. Oncologists also weigh price less when making prescribing decisions.
However, the cost of treating cancer has been at the heart of the healthcare costs debate, and we expect oncologists to face growing payer restrictions in the coming years. Utilization management rates for oncology drugs rose to 50% in 2016, from 34% a year earlier. Competition will grow more intense: A flush of me-too products with minimal clinical differentiation are hitting the market, and payers are increasingly demanding real-world evidence of their relative efficacy.
That said, there is a contingent of physicians who indicate that they are actively seeking to manage total cost of care. Pharma companies can support physicians in that effort by providing evidence that their therapies are clinically differentiated and more cost-effective than other treatment options.
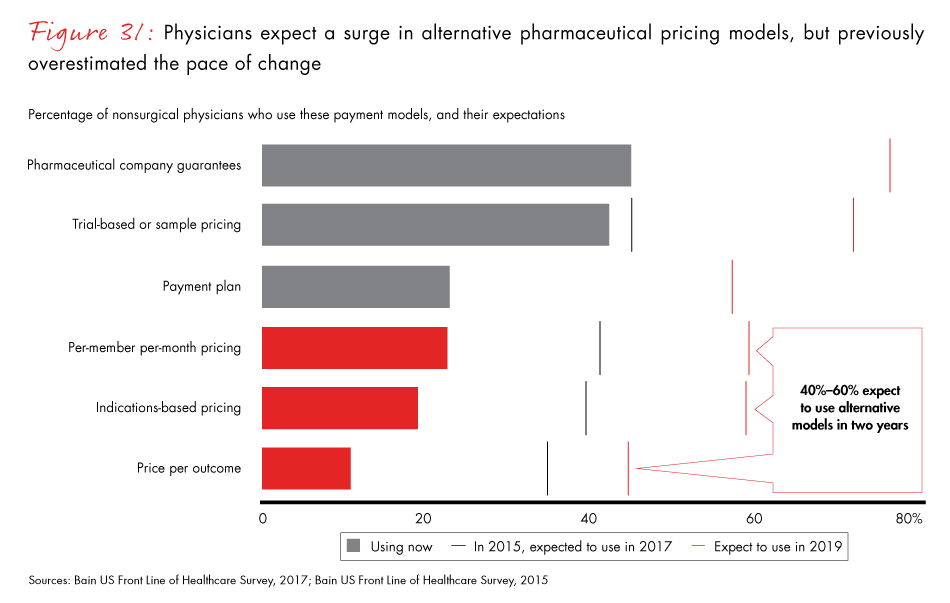
Pharma companies can prepare for an uptick in the use of alternative pricing models, where price is based on indications or outcomes, by testing and refining them with providers and payers. The physicians we surveyed expect the use of innovative pricing models for pharmaceuticals to more than triple over the next two years. In the past, however, the pace of adoption has been much slower than healthcare professionals anticipated.
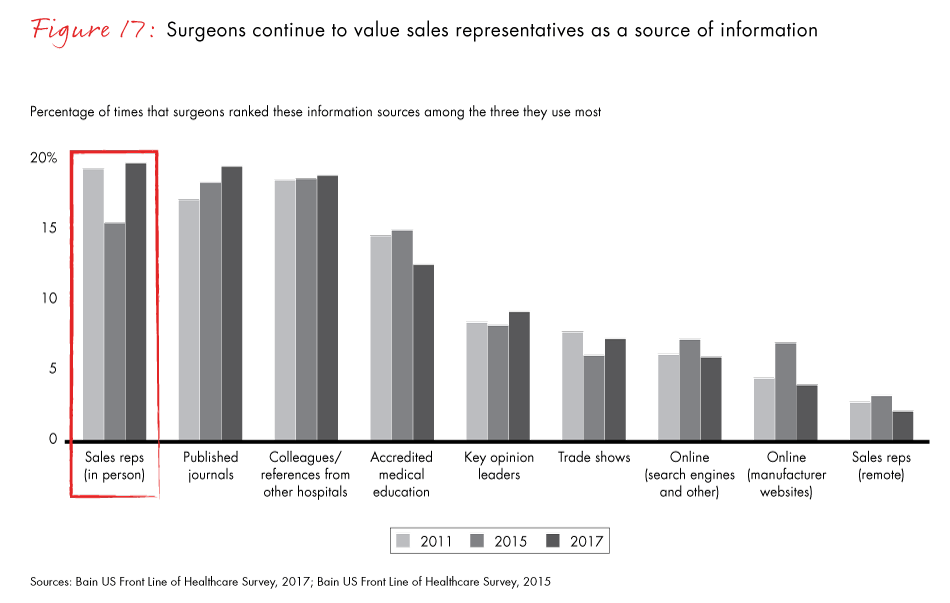
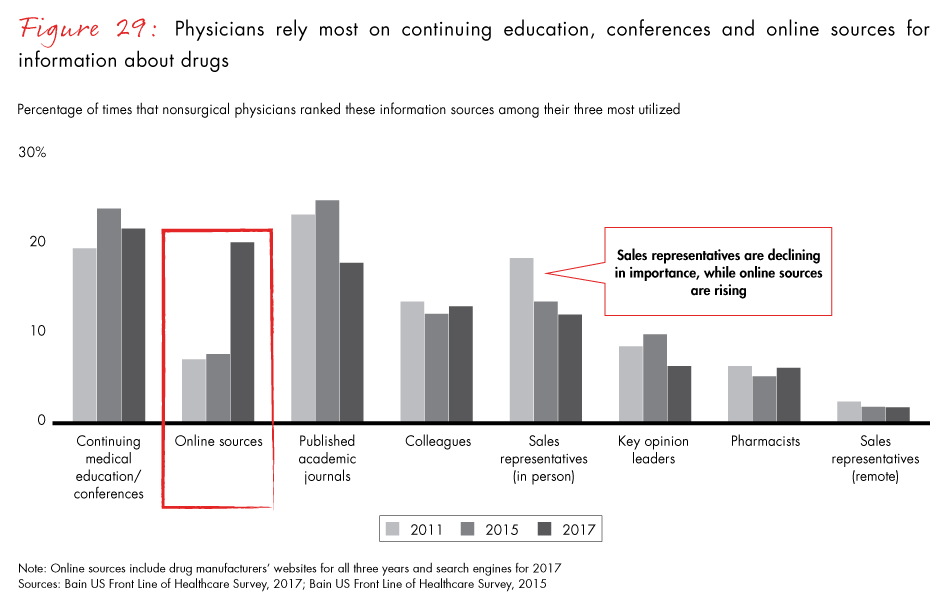
In a shifting landscape, an omnichannel approach to marketing is the most effective way to get drug information to nonsurgical physicians. Physicians rank continuing medical education (including conferences) as their most important source of information, relatively more important than published medical journals for the first time in this survey. Reliance on sales representatives declined over the last six years, moving from one of the top three information sources in 2011 to fifth place in 2017. Meanwhile, online sources, including drug websites and search engines, have greatly increased in importance. These trends are likely to continue since younger physicians are less interested in relying on sales reps as an information source and are more accustomed to going online for drug information.
The road ahead
After a decade of trying out new models, the US healthcare industry has yet to rally around an innovative approach that provides quality care at lower cost. In fact, a disruptive, technology-based solution like those that have transformed the telecom or retail industries may take much longer to develop for healthcare, although a comparable outcome seems inevitable. In the meantime, the industry will continue to innovate, with progress in fits and starts as different models gain traction in different places. Although the pace of change has been slower than predicted in recent years, as Microsoft cofounder Bill Gates once noted: “We always overestimate the change that will occur in the next two years and underestimate the change that will occur in the next ten.”
The key message of our 2017 survey is that future progress depends on physicians shaping and leading change. Healthcare organizations that engage and empower physicians are likely to lead the next wave of innovation. Proving the clinical and financial benefits of new systems and tools while reducing their complexity is essential to overcoming physician skepticism. Those efforts will take time, but they will help provide new momentum for change.
1. The changing landscape
- The adoption of new healthcare structures, value-based models and tools to curb spiraling costs and improve care has slowed and in some cases plateaued following five years of rapid experimentation and change.
- There is a growing divide among medical practices: Larger, management-led groups are more likely to adopt new structures and protocol-based care, while smaller, physician-led practices may be unlikely to make major investments in new systems and tools.
- One notable slowdown has been in the shift to value-based payment models, including pay-for-performance, shared savings, bundled payments and capitation or global payment models.
- More than 70% of physicians prefer a fee-for-service model even though they recognize that it is more expensive. Physicians are not convinced value-based models improve clinical outcomes. A higher proportion of finance and procurement officers prefer value-based models. The split highlights a lack of internal agreement on value-based care.
- Despite the slower pace of change, the healthcare industry continues to feel a steady pull toward value-based care. Medical practices continue to experiment with a mix of fee-for-service and value-based options.
- More than 60% of physicians say it will be more difficult to deliver high-quality care in the next two years, citing complex regulations, an increasing administrative burden and frustration associated with electronic medical records.
2. Providers
- Organizations that want to move toward value-based care will need to include their physicians to a much greater degree in decision making, empower them to innovate with the care-delivery model, and provide evidence that new systems and tools will deliver the same or better quality of care at lower cost—addressing physicians’ concerns about outcomes, simplicity and fairness.
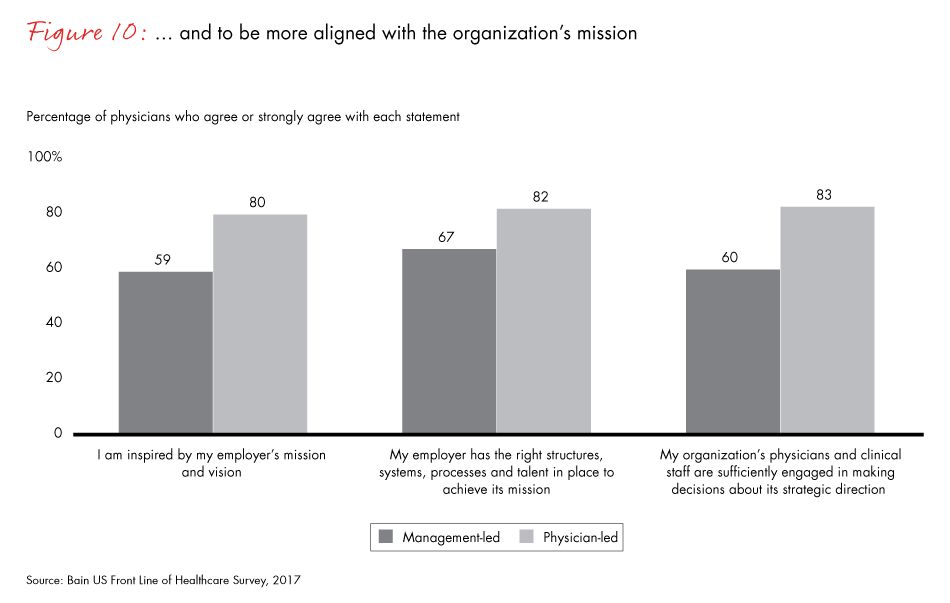
- Physician-led practices hold lessons for all providers: Their physicians give them a higher Net Promoter Score as a place to work (36%), feel inspired by the organization’s mission (80%) and feel sufficiently engaged in decisions about strategic direction (83%). Physicians in management-led organizations on average are less inspired, less aligned and less likely than peers in physician-led practices to believe that they are sufficiently engaged in making important decisions about strategic direction and operations.
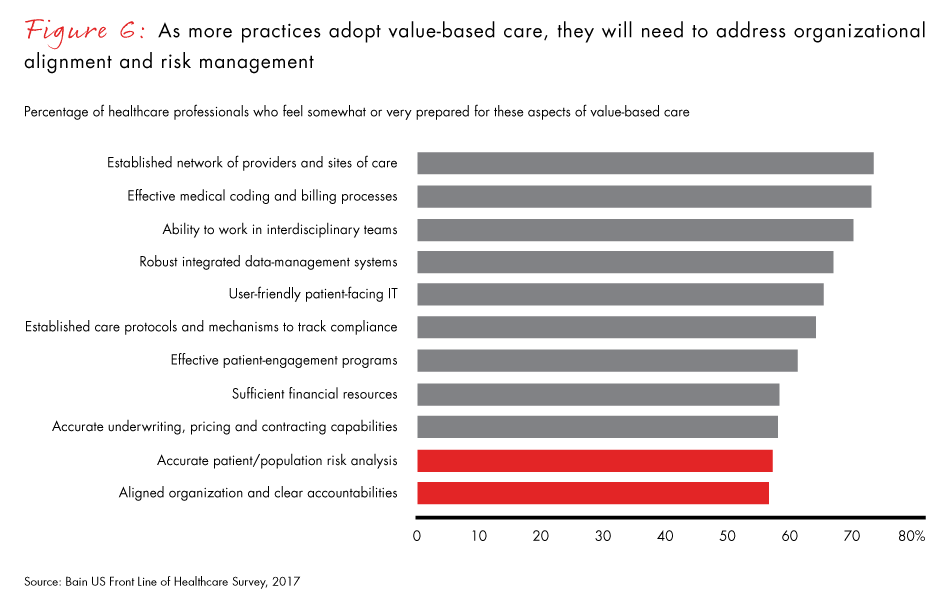
- Delivering value-based care requires an aligned organization with clear accountabilities—and healthcare professionals cite the lack of alignment and clear accountability as reasons their organizations are not prepared for a shift to value-based care.
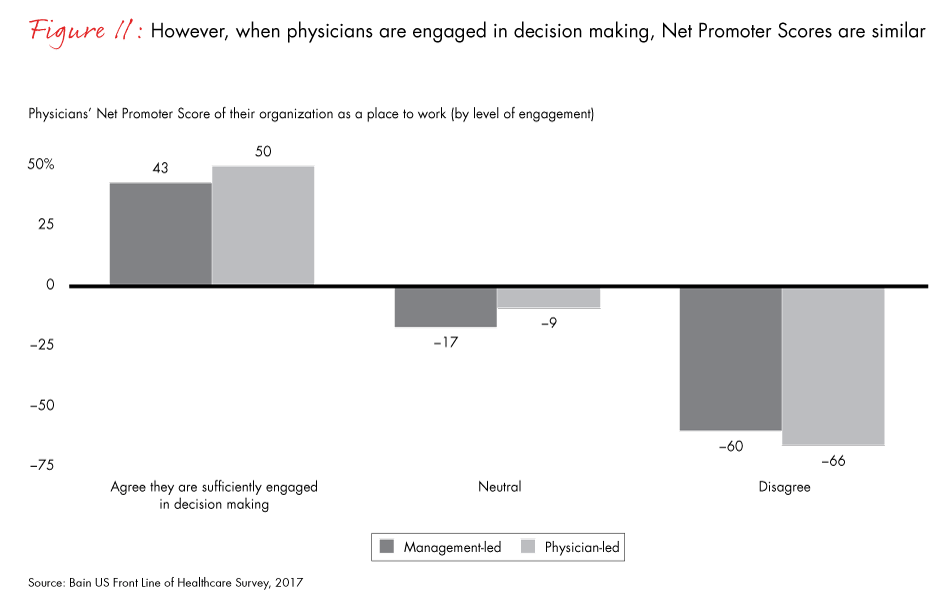
- Physicians who are engaged have a much higher employer Net Promoter Score (47%) than those who are neutral (-14%) or disengaged (-61%). This is true for physicians in both physician-led and management-led organizations. In fact, physicians in management-led organizations who feel engaged in decision making have a higher Net Promoter Score than those in physician-led organizations who do not.
3. Medtech
- Bain’s survey of 261 surgeons across three specialties shows medtech companies can improve their competitive standing by building category leadership positions and offering value-added services. Surgeons rate “strongest existing relationship” with medtech suppliers as a key purchasing criterion, and they rank ongoing product training support as the most valuable add-on service.
- Product quality and patient outcomes continue to rank as the top criteria in medtech purchasing decisions. Despite rising pressure on costs, the industry still values and rewards true clinical innovation. But successful companies demonstrate both the clinical and economic value of their products. Seventy percent of surgeons believe “best value for price paid” is an important purchasing criterion, a significant increase over two years ago.
- The decision-making authority for purchasing medical equipment has become more collaborative, with surgeons and procurement weighing purchases jointly. That reverses a 10-year trend that shifted the authority to procurement and finance officers. Now surgeons have become more sophisticated, multidimensional buyers, weighing clinical and financial data and the interests of both the patient and the hospital.
- More than 80% of practices said surgeons and procurement make decisions jointly, and surgeons are increasingly supportive of this arrangement. Surgeons who indicated high alignment with their practices’ mission are more likely to work in environments using a partnership purchasing model.
- Healthcare professionals expect major increases in alternative pricing models for medical devices over the next two years. A caveat: Healthcare professionals' previous expectations have proven overly optimistic. The use of alternative pricing models is unlikely to accelerate significantly until there is compelling clinical data that supports the transition.
4. Pharma
- Bain’s survey of 719 nonsurgical physicians across five specialties shows patient outcomes and superior real-world evidence are the most important criteria in prescribing decisions along with safety profile. Successful pharma companies can keep pace with the growing demand for scientific evidence by augmenting their medical affairs capabilities.
- Physicians are taking a more active role in trying to reduce drug costs. The majority of physicians seek to minimize patients’ out-of-pocket costs through their prescribing decisions.
- Physicians say the most effective approaches to lowering drug prices would be to improve price transparency between health plans and pharma manufacturers, give Medicare authority to negotiate drug prices and increase competition among pharma manufacturers.
- A key role of pharmacy benefits managers is controlling drug costs, but fewer than 20% of physicians rely on them to lower costs and improve quality of care.
- Seventy percent of nonsurgical physicians believe payer restrictions limit their prescribing decisions, and 59% believe these restrictions decrease their ability to deliver high-quality care—both up slightly since 2015.
- Category leadership continues to be a key determinant of success. Market-share leaders in each specialty have stronger customer advocacy than other manufacturers.
- Pharma companies that invest in an omnichannel approach to convey drug information to nonsurgical physicians will be the best positioned to adapt to changing preferences. Doctors rank continuing medical education and conferences as the most important information source. Reliance on sales representatives continues to decline and now ranks No. 5 in importance, down from No. 3 in 2011.
Appendix: Methodology and survey questions
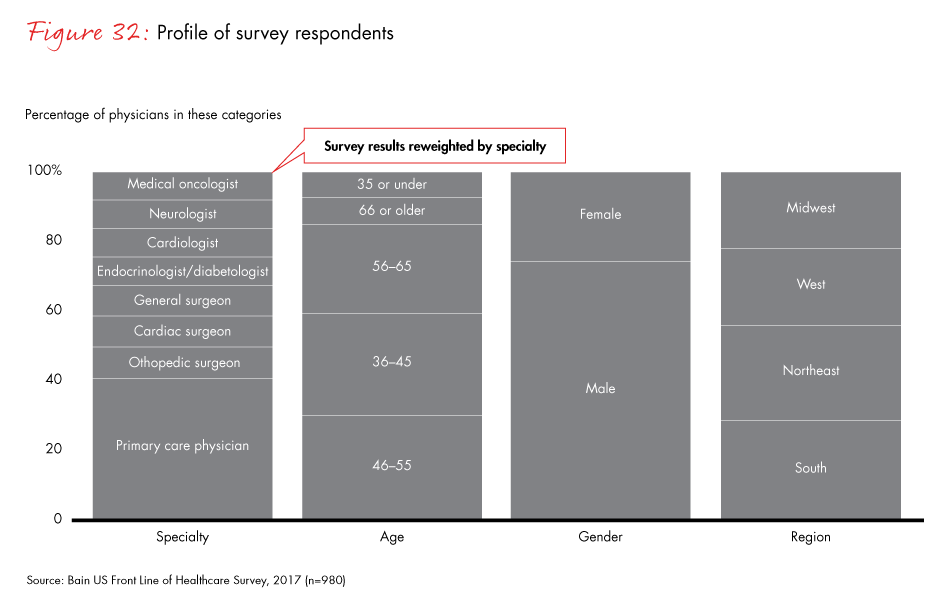
The Bain US Front Line of Healthcare Survey, conducted in 2017, included a total of 980 physicians, 100 procurement officers and 100 finance officers from the US. The survey sampled respondents across all 50 states and the District of Columbia, and the sample was representative of the Northeast, Midwest, South and West regions of the US.
The survey focused on eight physician specialties—three surgical and five nonsurgical. The surgical specialties were general, cardiac and orthopedic surgery, and participants in these specialties provided input for “The changing landscape,” “Providers” and “Medtech” sections of this report.
Nonsurgical specialties were primary care, medical oncology, noninterventional cardiology, endocrinology/ diabetology and neurology. Participants in these nonsurgical specialties provided input for “The changing landscape,” “Providers” and “Pharma” sections. The specialties were chosen based on the distribution of physicians by specialty across the US, global revenues associated with each specialty, and longitudinal consistency with the US Front Line of Healthcare Report 2015 and the Europe Front Line of Healthcare Report 2016.
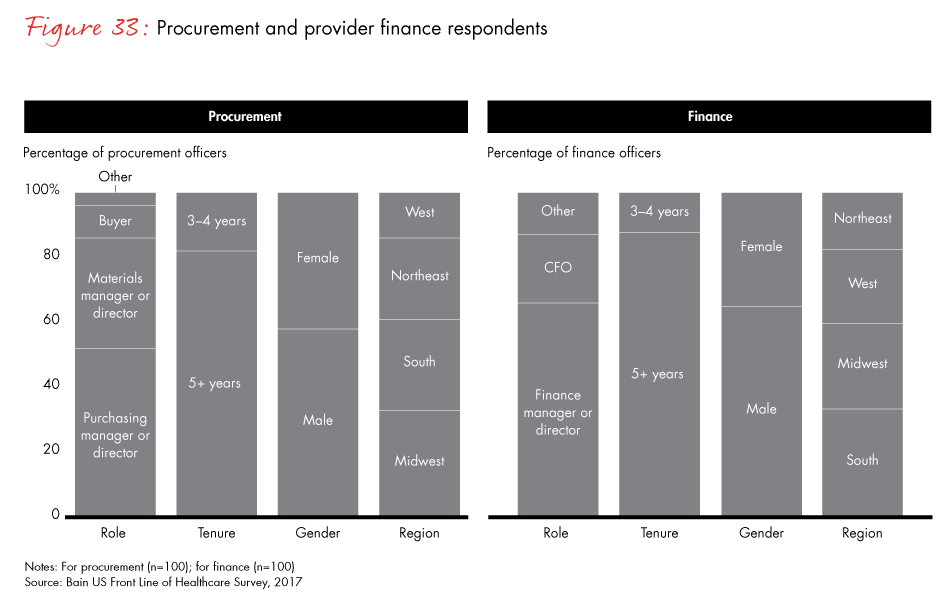
We also surveyed procurement and finance officers to capture their perspectives on key trends, including payment models, purchasing and pricing. Procurement and finance officers provided input into all four sections of the report. We did not survey physician views regarding group purchasing organizations, which for acute care medical technology contracting serve a role in the value chain similar to that of PBMs in prescription drugs.
The physician sample was weighted by specialty to ensure our results would be representative of the distribution of specialties across the US. For example, primary care physicians make up about 75% of the national population of physicians among the eight specialties we included, and were therefore given corresponding weight in the survey. To calculate weights, we used the Association of American Medical Colleges’ 2016 Physician Specialty Data Report. In addition, we also tracked physician demographics, including age, gender and region, to ensure general representativeness of the sample; the survey sample very closely aligns with the demographics of US physicians in these eight specialties.
For this survey, we engaged Research Now’s online panel of healthcare professionals. Survey responses underwent strict quality checks to ensure maximum data integrity; we tracked straight-lining behaviors (e.g., a respondent always selecting option c), speed, illogical responses and quality of free-text answers.
When comparing results with the past, we used Bain’s 2015 Front Line of Healthcare Report, Bain's 2013 Integrated Care for Pharma and Medtech Report, and Bain's 2011 Physician Attitude Report as sources of 2015, 2013 and 2011 data. When incorporating these surveys, we maintained the weighting given to specialties in these reports to ensure data integrity was preserved.
When measuring advocacy, we used the Net Promoter Score, which was developed by Bain & Company and is a tested indicator of advocacy. We asked Net Promoter® questions to assess, on a scale of zero to 10, physicians’ likelihood of recommending their organizations to friends or colleagues (a) as a place to work and (b) when in need of medical services. We also asked for Net Promoter Scores of medical device and pharmaceutical manufacturers. Ratings of zero to 6 signify detractors, 7 to 8 signify passives, and 9 to 10 signify promoters. The Net Promoter Score is calculated by subtracting the percentage of detractors from the percentage of promoters. A positive score indicates advocacy and support, while a negative score shows the opposite.
Regarding payment models, we used the following definitions:
Fee-for-service models reimburse healthcare providers for each service or test performed.
Pay-for-performance (P4P) models compensate providers if they meet certain metrics for quality and efficiency. In our survey, P4P includes bundled payment models in which providers receive a set payment for a specific episode of care, and shared savings models in which providers receive incentives for reducing costs for a defined patient population.
Capitation models pay providers a per-member-per-month fee for each patient covered under a health maintenance organization or managed care organization, regardless of the number of visits or treatments the patient receives.
Survey questions and notes
Figure 1: The definitions for our nine criteria measuring the use of structures, models and tools are:
Electronic medical records: Use of such records
Treatment extenders: Case managers, care coordinators and other patient management staff
Wellness initiatives: Health education and patient-adherence programs
Data/analytical tools: Analytics to identify at-risk patients or compare data on treatments
Other digital technology: Telemedicine, remote patient monitoring and electronic access to protocols
Value-based payment models: Models that link a payer’s contract to patient health outcomes
Management-driven cost controls: Management uses controls and incentives to lower costs
Management-driven treatment protocols: Management requires or provides incentives for standard treatment protocols
Metric-based compensation: Metrics used in performance reviews and to determine compensation
The time range of longitudinal data is two, four or six years ago, depending on the question. We calculated the overall systems score as an average of scores across nine criteria. We excluded physician cost consciousness from the criteria, given its attitudinal and subjective nature and the variability across organizations.
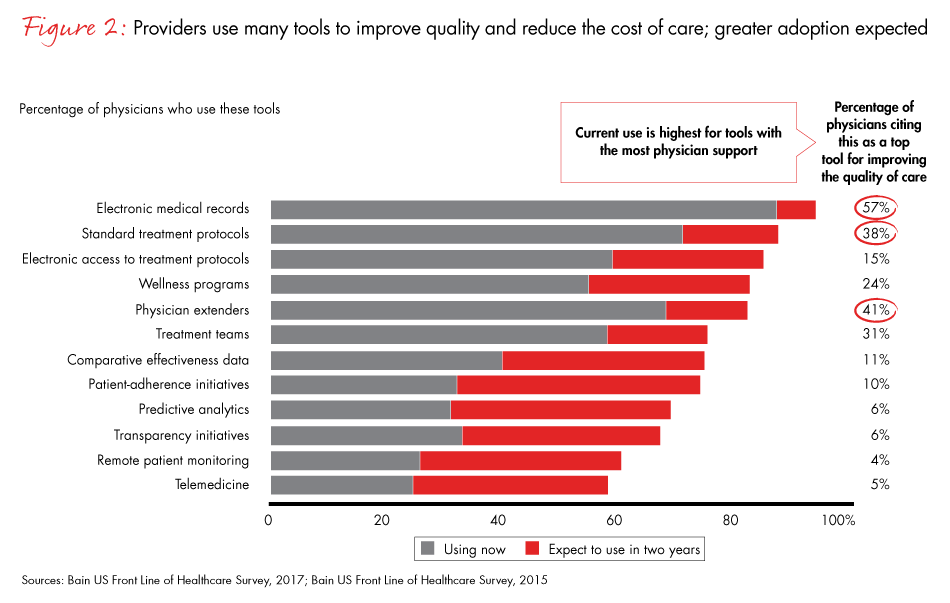
Figure 2: For the bar chart: “Please indicate if you have used the following tools or participated in the following programs.” For percentages in the right-hand column: “Currently, which tools or programs have the most positive impact on the quality of care delivered where you work? Rank three tools.” Denotes the percentage of times each tool or program was ranked in top three, with equal weight given to 1, 2 and 3. Surgical and nonsurgical physicians.
Figure 3: “Which payment models would you prefer for the majority of patients at your practice?” Excludes “other.” Surgical and nonsurgical physicians.
Figure 4: “To what degree do you think these payment models affect your patients’ costs?” Excludes respondents who were neutral. Surgical and nonsurgical physicians.
Figure 5: “To what degree do you think these payment models affect patients’ quality of care?” Excludes respondents who were neutral. Surgical and nonsurgical physicians.
Figure 6: “As practices move toward pay-for-performance and value-based models, how prepared do you think your practice is along the following dimensions?” Excludes “I don’t know.” Surgical and nonsurgical physicians, procurement and finance officers.
Figure 7: “Do you think it will be more difficult, the same or easier for your practice to deliver high-quality care to patients in two years?” Surgical and nonsurgical physicians.
Figure 8: For the left-hand side: “On a scale of zero to 10, where zero means ‘not at all likely’ and 10 means ‘extremely likely,’ how likely are you to recommend your current organization to a friend or colleague as a place to work?” For the right-hand side: “On a scale of zero to 10, where zero means ‘not at all likely’ and 10 means ‘extremely likely,’ how likely are you to recommend your current organization to a friend or colleague in need of medical services?” Surgical and nonsurgical physicians.
Figure 9: “On a scale of zero to 10, where zero means ‘not at all likely’ and 10 means ‘extremely likely,’ how likely are you to recommend your current organization to a friend or colleague as a place to work?” Surgical and nonsurgical physicians.
Figure 10: “To what extent do you agree or disagree with the following statements about your employer?” Surgical and nonsurgical physicians.
Figure 11: “On a scale of zero to 10, where zero means ‘not at all likely’ and 10 means ‘extremely likely,’ how likely are you to recommend your current organization to a friend or colleague as a place to work?” Surgical and nonsurgical physicians.
Figure 13: “To what extent do you agree with the following statement: My practice’s procurement department is helping us make decisions that improve costs and quality of care.”
Figure 14: “To what extent do you agree or disagree with the following statements about medical devices at your organization?”
Figure 15: “How important are the following criteria to you when deciding which manufacturer to use for your medical devices?”
Figure 16: “On a scale of zero to 10, where zero means ‘not at all likely’ and 10 means ‘extremely likely,’ how likely are you to recommend this manufacturer to a colleague?” The top three manufacturers include all companies with a category leadership position (relative market share >0.75).
Figure 17: “Today, which of the following sources do you use most to get information about medical devices? Please rank three sources in order from most used to least used, with 1 as most used. Do not rank if you do not use.”
Figure 18: “What are the three most valuable roles a medical device sales representative can play?” Excludes “other.”
Figure 19: “Which of the medtech payment models below are being used by your organization?” Excludes “I don’t know” and “other.”
Figure 20: “On a scale of zero to 10, where zero means ‘not at all likely’ and 10 means ‘extremely likely,’ how likely are you to recommend this manufacturer to another physician?” The top manufacturers include all companies with a category leadership position (relative market share >0.75). Excludes neurology.
Figure 21: “How important are the following criteria when deciding which drug(s) to prescribe to a patient?”
Figure 22: “Please indicate the extent to which you agree or disagree with the following statement about your clinical decisions: Part of my responsibility as a physician is to help bring healthcare costs under control.” “Agree” includes those who strongly and somewhat agree; “disagree” includes those who strongly and somewhat disagree.
Figure 23: “To what extent do you agree with the following statements?”
Figure 24: “To what extent do you agree with the following statements?”
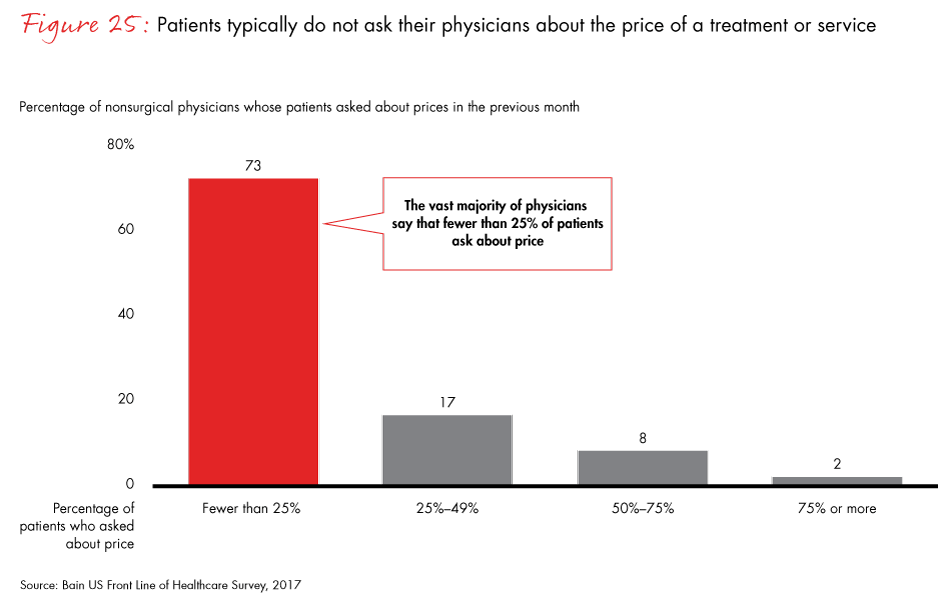
Figure 25: “In the last month, what percentage of patients at your hospital or practice requested price information about a treatment or service from you?”
Figure 26: “Which actions do you think would be most effective at reducing pharmaceutical prices? Please choose the top three.”
Figure 27: “How often do the following statements apply to your prescribing decisions at your organization?”
Figure 28: “Which of the following statements represents your perspective on pharmacy benefit managers? (a) PBMs are significantly improving costs and quality of care at my practice. (b) PBMs are improving costs and quality of care at my practice. (c) PBMs are having a neutral effect on costs and quality of care at my practice. (d) PBMs are worsening costs and quality of care at my practice. (e) PBMs are significantly worsening costs and quality of care at my practice.”
Figure 29: “Today, which of the following sources do you use most to get information about pharmaceutical products? Please rank three sources in order from most used to least used, with 1 as most used. Do not rank if you do not use.”
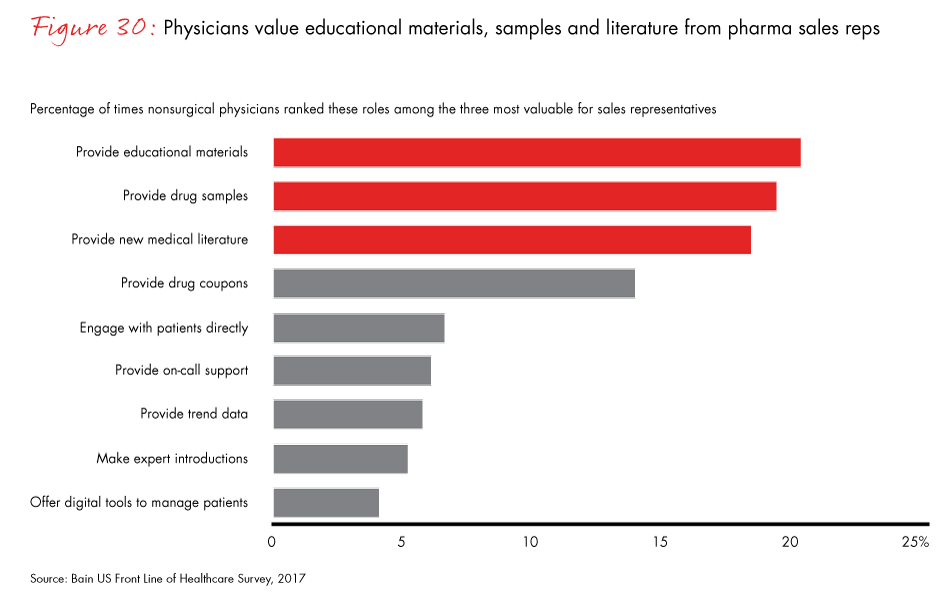
Figure 30: “What are the three most valuable roles a pharma/biotech sales representative can play?” Excludes “other.”
Figure 31: “Which of the pharmaceutical pricing models below are used by your patients’ insurance providers?” Excludes “I don’t know” and “other.” 2015 data for “pharmaceutical company guarantees” and “payment plan” are not available.
Authors
This report was prepared by Tim van Biesen, Josh Weisbrod, Michael Brookshire, Julie Coffman and Andy Pasternak, who are partners in Bain’s Healthcare practice. Tim van Biesen leads the firm’s Americas Healthcare practice and is based in New York. Josh Weisbrod also is based in New York, Michael Brookshire is in Bain’s Dallas office, and Julie Coffman and Andy Pasternak are in the firm’s Chicago office.
Acknowledgments
The authors wish to give special thanks to Prilla Schenck, Nyssa Liebermann, Emilia Sibley and David Joseph for their contributions to this report. Additional thanks to Gail Edmondson for her editorial support, and to Research Now for programming and hosting the survey and for supplying its online panel of healthcare professionals.
Net Promoter Score® and Net Promoter® are trademarks of Bain & Company, Inc., Fred Reichheld and Satmetrix Systems, Inc.
































